Abstract
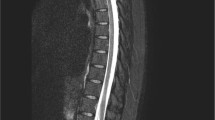
Neurological syndromes occur in around 40–70% of HIV-infected people. Direct central nervous system involvement by the virus usually manifests as HIV encephalitis, HIV leucoencephalopathy, vacuolar leucoencephalopathy or vacuolar myelopathy. Indirect involvement is usually associated with neurotropic opportunistic infections which include tuberculosis, toxoplasmosis, cryptococcosis and viral encephalitis such as herpes simplex, varicella-zoster, cytomegalovirus and Human polyomavirus 2. We report a case of transverse myelitis in a recently diagnosed HIV patient who was otherwise asymptomatic initially and developed paraparesis after 1 month of initiation of antiretroviral therapy. After ruling out opportunistic infections and other causes of compressive and non-compressive myelopathy, development of transverse myelitis was attributed to immune reconstitution inflammatory syndrome in view of baseline low CD4 count and their improvement after HAART initiation. Prompt treatment with corticosteroids successfully reversed the symptoms.

Similar content being viewed by others
References
Aboulafia DM, Taylor L (2002) Vacuolar myelopathy and vacuolar cerebellar leukoencephalopathy: a late complication of AIDS after highly active antiretroviral therapy-induced immune reconstitution. AIDS Patient Care STDs 16:579–584
Andrade P, Figueiredo C, Carvalho C, Santos L, Sarmento A (2014) Transverse myelitis and acute HIV infection: a case report. BMC Infect Dis 14:149. https://doi.org/10.1186/1471-2334-14-149
Bahr N, Boulware DR, Marais S, Scriven J, Wilkinson RJ, Meintjes G (2013) Central nervous system immune reconstitution inflammatory syndrome. Curr Infect Dis Reports 15:583–593. https://doi.org/10.1007/s11908-013-0378-5
Bowen L, Nath A, Smith B (2018) CNS immune reconstitution inflammatory syndrome. Handb Clin Neurol 152:167–176. https://doi.org/10.1016/B978-0-444-63849-6.00013-X
Manabe YC, Campbell JD, Sydnor E, Moore RD (2007) Immune reconstitution inflammatory syndrome: risk factors and treatment implications. J Acquir Immune Defic Syndr 46:456–462. https://doi.org/10.1097/QAI.0b013e3181594c8c
Mathew T, Avati A, D’Souza D, Therambil M, Baptist AA, Shaji A, Nadig R, Rockey SM, Parry G (2019) HIV infection associated neuromyelitis optica spectrum disorder: clinical features, imaging findings, management and outcomes. Mult Scler Relat Disord 27:289–293. https://doi.org/10.1016/j.msard.2018.11.014
McCarthy M, Nath A (2010) Neurologic consequences of the immune reconstitution inflammatory syndrome (IRIS). Curr Neurol Neurosci Rep 10:467–475. https://doi.org/10.1007/s11910-010-0138-y
Niu MT, Stein DS, Schnittman SM (1993) Primary human immunodeficiency virus type 1 infection: review of pathogenesis and early treatment interventions in humans and animal retrovirus infections. J Infect Dis 14:1490–1501. https://doi.org/10.1093/infdis/168.6.1490
Rasul S, Delapenha R, Farhat F, Gajjala J, Zahra SM (2011) Graves’ disease as a manifestation of immune reconstitution in HIV-infected individuals after initiation of highly active antiretroviral therapy. AIDS Res Treat 2011:743597–743594. https://doi.org/10.1155/2011/743597
Author information
Authors and Affiliations
Contributions
All the authors have provided substantial contributions in the clinical management of the case and literature review on the topic in question. Dr. Preeti Dalal and Dr. Karuna Anot have drafted the manuscript, and Dr. Monica Gupta and Dr. Sanjay D’Cruz have revised it critically for important intellectual content. All the authors have read the final version and approved it. All the authors agree to be accountable for all aspects of the work in ensuring that questions related to the accuracy or integrity of any part of the work are appropriately investigated and resolved.
Corresponding author
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dalal, P., Anot, K., Monica, G. et al. Acute paraparesis in HIV-infected patient after initiation of highly active antiretroviral therapy. J. Neurovirol. 26, 793–796 (2020). https://doi.org/10.1007/s13365-020-00879-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13365-020-00879-4