Summary
Background
Cerebrospinal fluid (CSF) shunting is a highly effective treatment for idiopathic normal pressure hydrocephalus (iNPH). However, secondary deterioration can occur at a later time. Thus, the current study aimed to evaluate the incidence rate and causes of secondary deterioration.
Methods
A retrospective analysis was conducted on all patients with iNPH who were treated with implantation of a CSF shunt since 1993. A meticulous shunt workup was recommended to all patients who presented to our department with secondary deterioration during their follow-up visits. Data about the proportion of patients with such deterioration and its causes, subsequent treatment, and clinical outcome were obtained.
Results
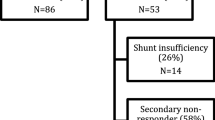
A total of 169 patients were included, and the mean follow-up time was 69.2 months. In total, 119 (70.4%) patients presented with a total of 153 secondary deteriorations. In 9 cases (5.9%), the deterioration was caused by delayed subdural hematoma and in 27 (22.1%) cases, by shunt dysfunction. Invasive shunt testing was commonly required to validate shunt failure. Moreover, 19 of 27 patients experienced a satisfactory improvement after revision surgery. In total, 86 deteriorations were attributed to nonsurgical causes, and the valve pressure was decreased in 79 patients, with only 16.5% presenting with a satisfactory improvement after lowering of valve pressure.
Conclusions
Most patients with shunted iNPH presented with deterioration in the later course of the disease. Shunt dysfunction was considered a cause of secondary deterioration. Moreover, shunt revision surgery was a highly effective treatment, and patients with deterioration should undergo screening procedures for shunt dysfunction, including invasive shunt testing.



Similar content being viewed by others
References
Akiba C, Nakajima M, Miyajima M, Ogino I, Motoi Y, Kawamura K, Adachi S, Kondo A, Sugano H, Tokuda T, Irie K (2018) Change of amyloid-β 1-42 toxic conformer ratio after cerebrospinal fluid diversion predicts long-term cognitive outcome in patients with idiopathic normal pressure hydrocephalus. JAD 63(3):989–1002
Allali G, Laidet M, Armand S, Momjian S, Marques B, Saj A, Assal F (2017) A combined cognitive and gait quantification to identify normal pressure hydrocephalus from its mimics: The Geneva’s protocol. Clin Neurol Neurosurg 160:5–11
Andren K, Wikkelso C, Tisell M, Hellstrom P (2014) Natural course of idiopathic normal pressure hydrocephalus. J Neurol Neurosurg Psychiatry 85(7):806–810
Andrén K, Wikkelsö C, Sundström N, Agerskov S, Israelsson H, Laurell K, Hellström P, Tullberg M (2018) Long-term effects of complications and vascular comorbidity in idiopathic normal pressure hydrocephalus: a quality registry study. J Neurol 265(1):178–186
Aoki Y, Kazui H, Tanaka T, Ishii R, Wada T, Ikeda S, Hata M, Canuet L, Katsimichas T, Musha T, Matsuzaki H (2015) Noninvasive prediction of shunt operation outcome in idiopathic normal pressure hydrocephalus. Sci Rep 5(1):7775
Benveniste RJ, Sur S (2018) Delayed symptom progression after ventriculoperitoneal shunt placement for normal pressure hydrocephalus. J Neurol Sci 393:105–109
Birkeland P, Lauritsen J, Poulsen FR (2015) Aspirin is associated with an increased risk of subdural hematoma in normal-pressure hydrocephalus patients following shunt implantation. JNS 123(2):423–426
Bozhkov Y, Roessler K, Hore N, Buchfelder M, Brandner S (2017) Neurological outcome and frequency of overdrainage in normal pressure hydrocephalus directly correlates with implanted ventriculo-peritoneal shunt valve type. Neurol Res 39(7):601–605
Eide P, Pripp A (2014) Increased prevalence of cardiovascular disease in idiopathic normal pressure hydrocephalus patients compared to a population-based cohort from the HUNT3 survey. Fluids Barriers CNS 11(1):19
Golomb J, Wisloff J, Miller DC, Boksay I, Kluger A, Weiner H, Salton J, Graves W (2000) Alzheimer’s disease comorbidity in normal pressure hydrocephalus: prevalence and shunt response. J Neurol Neurosurg Psychiatry 68(6):778–781
Hoya K, Tanaka Y, Uchida T, Takano I, Nagaishi M, Kowata K, Hyodo A (2012) Treatment of traumatic acute subdural hematoma in adult hydrocephalus patients with cerebrospinal fluid shunt. Clin Neurol Neurosurg 114(3):211–216
Israelsson H, Carlberg B, Wikkelsö C, Laurell K, Kahlon B, Leijon G, Eklund A, Malm J (2017) Vascular risk factors in INPH: A prospective case-control study (the INPH-CRasH study). Neurology 88(6):577–585
Jang H, Park SB, Kim Y, Kim KW, Lee JI, Kim ST, Lee KH, Kang ES, Choe YS, Seo SW, Kim HJ (2018) Prognostic value of amyloid PET scan in normal pressure hydrocephalus. J Neurol 265(1):63–73
Jaraj D, Rabiei K, Marlow T, Jensen C, Skoog I, Wikkelso C (2014) Prevalence of idiopathic normal-pressure hydrocephalus. Neurology 82(16):1449–1454
Jaraj D, Agerskov S, Rabiei K, Marlow T, Jensen C, Guo X, Kern S, Wikkelsø C, Skoog I (2016) Vascular factors in suspected normal pressure hydrocephalus: A population-based study. Neurology 86(7):592–599
Kiefer M, Meier U, Eymann R (2010) Does idiopathic normal pressure hydrocephalus always mean a poor prognosis? In: Czernicki Z, Baethmann A, Ito U, Katayama Y, Kuroiwa T, Mendelow D (eds) Brain Edema XIV. Springer Vienna, Vienna, pp 101–106
Kim B-J, Park K-J, Park D-H, Lim D-J, Kwon T-H, Chung Y-G, Kang S-H (2014) Risk factors of delayed surgical evacuation for initially nonoperative acute subdural hematomas following mild head injury. Acta Neurochir 156(8):1605–1613
Klinge P, Marmarou A, Bergsneider M, Relkin N, Black PML (2005) Outcome of shunting in idiopathic normal-pressure hydrocephalus and the value of outcome assessment in shunted patients. Neurosurgery 57(suppl_3):S2-40–S2-52
Kuriyama N, Miyajima M, Nakajima M, Kurosawa M, Fukushima W, Watanabe Y, Ozaki E, Hirota Y, Tamakoshi A, Mori E, Kato T (2017) Nationwide hospital-based survey of idiopathic normal pressure hydrocephalus in Japan: Epidemiological and clinical characteristics. Brain Behav 7(3):e00635
Lemcke J, Meier U, Muller C, Fritsch MJ, Kehler U, Langer N, Kiefer M, Eymann R, Schuhmann MU, Speil A, Weber F (2013) Safety and efficacy of gravitational shunt valves in patients with idiopathic normal pressure hydrocephalus: a pragmatic, randomised, open label, multicentre trial (SVASONA). J Neurol Neurosurg Psychiatry 84(8):850–857
Marmarou A, Black P, Bergsneider M, Klinge P, Relkin N, International NPH Consultant Group (2005) Guidelines for management of idiopathic normal pressure hydrocephalus: progress to date. In: Poon WS, Chan MTV, Goh KYC et al (eds) Intracranial Pressure and Brain Monitoring XII. Springer-Verlag, Vienna, pp 237–240
Meier U, Mutze S (2004) Correlation between decreased ventricular size and positive clinical outcome following shunt placement in patients with normal-pressure hydrocephalus. J Neurosurg 100(6):1036–1040
Meier U, Paris S, Graewe A, Stockheim D, Hajdukova A, Mutze S (2003) Is there a correlation between operative results and change in ventricular volume after shunt placement? A study of 60 cases of idiopathic normal-pressure hydrocephalus. Neuroradiology 45(6):377–380
Mirzayan MJ, Luetjens G, Borremans JJ, Regel JP, Krauss JK (2010) Extended long-term (> 5 years) outcome of cerebrospinal fluid shunting in idiopathic normal pressure hydrocephalus. Neurosurgery 67(2):295–301
Mocco J, Tomey MI, Komotar RJ, Mack WJ, Frucht SJ, Goodman RR, McKhann GM (2006) Ventriculoperitoneal Shunting of idiopathic normal pressure hydrocephalus increases midbrain size: a potential mechanism for gait improvement. Neurosurgery 59(4):847–851
Petersen J, Hellström P, Wikkelsø C, Lundgren-Nilsson Å (2014) Improvement in social function and health-related quality of life after shunt surgery for idiopathic normal-pressure hydrocephalus. JNS 121(4):776–784
Starr BW, Hagen MC, Espay AJ (2014) Hydrocephalic Parkinsonism: lessons from normal pressure hydrocephalus mimics. J Clin Mov Disord 1(1):2
Toma AK, Stapleton S, Papadopoulos MC, Kitchen ND, Watkins LD (2011) Natural history of idiopathic normal-pressure hydrocephalus. Neurosurg Rev 34(4):433–439
Wallenstein MB, McKhann GM (2010) Salomón Hakim and the discovery of normal-pressure hydrocephalus. Neurosurgery 67(1):155–159
Funding
No funding was received for this research.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study concept and design. Material preparation, data collection, and analysis were performed by Stefanie Kaestner, Rhea Behrend, and Christian Roth. The first draft of the manuscript was written by Stefanie Kaestner. Review and editing were performed by Katharina Graf and Wolfgang Deinsberger. All authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (name of institute/committee) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Consent
Formal informed consent was not required for this type of study.
Additional information
Comments
The authors present a retrospective study of secondary deterioration in a large cohort of patients with idiopathic normal pressure hydrocephalus.169 patients are followed up for a mean of 69.2 months. Patients were selected for shunting by a tap test. Secondary deterioration occurred in 70%, at a mean of 37.8 months. At the time of secondary deterioration, patients underwent a CT scan and shunt radiography, and, if normal, had the opening pressure of their valve reduced. If there was no improvement, as was often the case, shunt function was investigated with injection of contrast medium, fluoroscopy and test aspiration of 30 mLs of CSF. 27 from 153 episodes of secondary deterioration were related to shunt malfunction; clinical improvement was evident after shunt revision in 19 episodes. The authors conclude that on long-term follow-up secondary deterioration is very common. More importantly, as about a fourth of these episodes were associated with shunt malfunction, investigation of the shunt, rather than assuming a nonsurgical cause, often results in improvement with shunt revision.This is an important study, as secondary deterioration in NPH is often attributed to progressive vascular or neurodegenerative causes. The study underlines the value of formal shunt investigation within a large cohort followed up for a reasonably long time.
Kristian Aquilina,
London, UK
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on CSF Circulation
Rights and permissions
About this article
Cite this article
Kaestner, S., Behrends, R., Roth, C. et al. Treatment for secondary deterioration in idiopathic normal pressure hydrocephalus in the later course of the disease: a retrospective analysis. Acta Neurochir 162, 2431–2439 (2020). https://doi.org/10.1007/s00701-020-04475-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00701-020-04475-7