Abstract
Purpose
Primary spinal cord glioblastoma (GBM) is a rare and devastating disease. Little attention was ever paid to this rare disease. As a result, the standard treatment protocol and prognostic factors of primary spinal cord GBM were not well established. The aim of this study was to determine the predictors associated with survival in patients with primary spinal cord GBM.
Methods
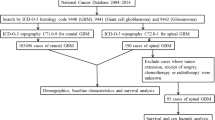
A total of 122 patients with primary spinal cord GBM from Surveillance, Epidemiology, and End Results database and our institution were included in this retrospective analysis. Information about age, sex, race, tumor invasion, extent of resection, radiation, chemotherapy and year of diagnosis was collected. Univariate and multivariate accelerated failure time (AFT) regression model was performed to identify prognostic factors.
Results
Of the 122 patients, 102 (83.6%) expired at the time of data collection. Overall survival at 1 year, 2 years, 3 years and 5 years was 48.4%, 22.8%, 17.1% and 8.4%, respectively, and median survival time was 12 months. Only radiation was found to be associated with survival in the AFT regression model (time ratio 1.94, 95% CI 1.01–3.72, p < 0.05). Radiotherapy could improve survival slightly; patients who received RT survived approximately two times as long as patients who did not receive RT, but the advantage was short term.
Conclusion
The survival of primary spinal cord GBM is poor in the current treatment strategy. Radiotherapy was associated with better survival, but the advantage was short term.




Similar content being viewed by others
Abbreviations
- AIC:
-
Akaike’s information criterion
- AFT:
-
Accelerated failure time model
- CSF:
-
Cerebrospinal fluid
- IQR:
-
Interquartile range
- GBM:
-
Glioblastoma
- GTR:
-
Gross total resection
- PH:
-
Proportional hazards assumption
- RT:
-
Radiotherapy
- S/PR:
-
Subtotal/partial resection
- TMZ:
-
Temozolomide
- 95% CI:
-
95% Confidence interval
References
Helseth A, Mork SJ (1989) Primary intraspinal neoplasms in Norway, 1955 to 1986. A population-based survey of 467 patients. J Neurosurg 71:842–845. https://doi.org/10.3171/jns.1989.71.6.0842
Santi M, Mena H, Wong K, Koeller K, Olsen C, Rushing EJ (2003) Spinal cord malignant astrocytomas. Clinicopathologic features in 36 cases. Cancer 98:554–561. https://doi.org/10.1002/cncr.11514
McGirt MJ, Goldstein IM, Chaichana KL, Tobias ME, Kothbauer KF, Jallo GI (2008) Extent of surgical resection of malignant astrocytomas of the spinal cord: outcome analysis of 35 patients. Neurosurgery 63(55–60):60–61. https://doi.org/10.1227/01.NEU.0000335070.37943.09
Stupp R, Brada M, van den Bent MJ, Tonn JC, Pentheroudakis G (2014) High-grade glioma: ESMO clinical practice guidelines for diagnosis, treatment and follow-up. Ann Oncol 25:i93–i101. https://doi.org/10.1093/annonc/mdu050
Hernández-Durán S, Bregy A, Shah AH, Hanft S, Komotar RJ, Manzano GR (2015) Primary spinal cord glioblastoma multiforme treated with temozolomide. J Clin Neurosci 22:1877–1882. https://doi.org/10.1016/j.jocn.2015.04.017
Shen C, Wu J, Zhao W, Cai Z, Cai R, Chen C (2017) Primary spinal glioblastoma multiforme: a case report and review of the literature. Medicine 96:e6634. https://doi.org/10.1097/MD.0000000000006634
Tomeczkowski J, Lange A, Güntert A, Thilakarathne P, Diels J, Xiu L, De Porre P, Tapprich C (2015) Converging or crossing curves: Untie the gordian knot or cut it? Appropriate statistics for non-proportional hazards in decitabine DACO-016 study (AML). Adv Ther 32:854–862. https://doi.org/10.1007/s12325-015-0238-9
Georgiadou M, Lilja J, Jacquemet G, Guzmán C, Rafaeva M, Alibert C, Yan Y, Sahgal P, Lerche M, Manneville J, Mäkelä TP, Ivaska J (2017) AMPK negatively regulates tensin-dependent integrin activity. J Cell Biol 216:1107–1121. https://doi.org/10.1083/jcb.201609066
Ostrom QT, Cioffi G, Gittleman H, Patil N, Waite K, Kruchko C, Barnholtz-Sloan JS (2019) CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2012–2016. Neuro-Oncol 21:v1–v100. https://doi.org/10.1093/neuonc/noz150
Konar SK, Maiti TK, Bir SC, Kalakoti P, Bollam P, Nanda A (2016) Predictive factors determining the overall outcome of primary spinal glioblastoma multiforme: an integrative survival analysis. World Neurosurg 86:341–348. https://doi.org/10.1016/j.wneu.2015.08.078
Cheng X, Lou S, Huang S, Chen H, Liu J (2017) Primary spinal cord glioblastoma multiforme: a retrospective study of patients at a single institution. World Neurosurg 106:113–119. https://doi.org/10.1016/j.wneu.2017.03.120
Adams H, Avendano J, Raza SM, Gokaslan ZL, Jallo GI, Quinones-Hinojosa A (2012) Prognostic factors and survival in primary malignant astrocytomas of the spinal cord: a population-based analysis from 1973 to 2007. Spine 37:E727–E735. https://doi.org/10.1097/BRS.0b013e31824584c0
Nakamura M, Chiba K, Ishii K, Ogawa Y, Takaishi H, Matsumoto M, Toyama Y (2006) Surgical outcomes of spinal cord astrocytomas. Spinal Cord 44:740–745. https://doi.org/10.1038/sj.sc.3101932
Ciappetta P, Salvati M, Capoccia G, Artico M, Raco A, Fortuna A (1991) Spinal glioblastomas: report of seven cases and review of the literature. Neurosurgery 28:302–306. https://doi.org/10.1097/00006123-199102000-00022
Raco A, Piccirilli M, Landi A, Lenzi J, Delfini R, Cantore G (2010) High-grade intramedullary astrocytomas: 30 years’ experience at the neurosurgery department of the University of Rome “Sapienza”. J Neurosurg Spine 12:144–153. https://doi.org/10.3171/2009.6.SPINE08910
Minehan KJ, Brown PD, Scheithauer BW, Krauss WE, Wright MP (2009) Prognosis and treatment of spinal cord astrocytoma. Int J Radiat Oncol Biol Phys 73:727–733. https://doi.org/10.1016/j.ijrobp.2008.04.060
Fakhreddine MH, Mahajan A, Penas-Prado M, Weinberg J, McCutcheon IE, Puduvalli V, Brown PD (2013) Treatment, prognostic factors, and outcomes in spinal cord astrocytomas. Neuro-Oncol 15:406–412. https://doi.org/10.1093/neuonc/nos309
Lam S, Lin Y, Melkonian S (2013) Analysis of risk factors and survival in pediatric high-grade spinal cord astrocytoma: a population-based study. Pediatr Neurosurg 48:299–305. https://doi.org/10.1159/000353135
Diaz-Aguilar D, ReFaey K, Clifton W, Durcanova B, Chen SG, Deen HG, Bydon M, Trifiletti DM, Pichelmann MA, Quiñones-Hinojosa A (2019) Prognostic factors and survival in low grade gliomas of the spinal cord: a population-based analysis from 2006 to 2012. J Clin Neurosci 61:14–21. https://doi.org/10.1016/j.jocn.2018.11.025
Luksik AS, Garzon-Muvdi T, Yang W, Huang J, Jallo GI (2017) Pediatric spinal cord astrocytomas: a retrospective study of 348 patients from the SEER database. J Neurosurg Pediatr 19:711–719. https://doi.org/10.3171/2017.1.PEDS16528
Zou Y, Sun J, Zhou Y, Bai HX, Huang X, Babu R, Landi A, Foong KS, Zhang Z, Woo JH, Tao Y, Li X, Tang X, Xiao B, Zhang PJ, Yang L (2018) Prognostic factors and treatment of spinal astrocytomas: a multi-institutional cohort analysis. Spine 43:E565–E573. https://doi.org/10.1097/BRS.0000000000002485
Benes RV, Barsa P, Benes JV, Suchomel P (2009) Prognostic factors in intramedullary astrocytomas: a literature review. Eur Spine J 18:1397–1422. https://doi.org/10.1007/s00586-009-1076-8
Ardeshiri A, Chen B, Hütter B, Oezkan N, Wanke I, Sure U, Sandalcioglu IE (2013) Intramedullary spinal cord astrocytomas: the influence of localization and tumor extension on resectability and functional outcome. Acta Neurochir 155:1203–1207. https://doi.org/10.1007/s00701-013-1762-5
Chanchotisatien A, Xiong J, Yu J, Chu S (2019) Exophytic primary intramedullary spinal cord glioblastoma: case report and critical review of literature. World Neurosurg 122:573–576. https://doi.org/10.1016/j.wneu.2018.11.113
Cabrera-Aldana EE, De la Garza RR, Pichardo-Bahena R (2017) Multicentric spinal cord glioblastoma. World Neurosurg 100:707–711. https://doi.org/10.1016/j.wneu.2017.01.006
Beyer S, von Bueren AO, Klautke G, Guckenberger M, Kortmann RD, Pietschmann S, Muller K (2016) A systematic review on the characteristics, treatments and outcomes of the patients with primary spinal glioblastomas or gliosarcomas reported in literature until March 2015. PLoS ONE 11:e148312. https://doi.org/10.1371/journal.pone.0148312
Seki T, Hida K, Yano S, Aoyama T, Koyanagi I, Sasamori T, Hamauch S, Houkin K (2016) Clinical factors for prognosis and treatment guidance of spinal cord astrocytoma. Asian Spine J 10:748–754. https://doi.org/10.4184/asj.2016.10.4.748
Liu A, Sankey EW, Bettegowda C, Burger PC, Jallo GI, Groves ML (2015) Poor prognosis despite aggressive treatment in adults with intramedullary spinal cord glioblastoma. J Clin Neurosci 22:1628–1631. https://doi.org/10.1016/j.jocn.2015.05.008
Yazici G, Yazici G, Zorlu F, Zorlu F, Cengiz M, Cengiz M, Ozyigit G, Ozyigit G, Eren G, Eren G, Yüce D, Yüce D, Varan A, Varan A, Akyuz C, Akyuz C, Akalan N, Akalan N, Gurkaynak M, Gurkaynak M (2016) High-grade glioma in children and adolescents: a single-center experience. Child’s Nerv Syst 32:291–297. https://doi.org/10.1007/s00381-015-2980-3
Ewelt C, Stummer W, Klink B, Felsberg J, Steiger H, Sabel M (2010) Cordectomy as final treatment option for diffuse intramedullary malignant glioma using 5-ALA fluorescence-guided resection. Clin Neurol Neurosurg 112:357–361. https://doi.org/10.1016/j.clineuro.2009.12.013
Viljoen S, Hitchon PW, Ahmed R, Kirby PA (2014) Cordectomy for intramedullary spinal cord glioblastoma with a 12-year survival. Surg Neurol Int 5:101. https://doi.org/10.4103/2152-7806.135305
Allen JC, Aviner S, Yates AJ, Boyett JM, Cherlow JM, Turski PA, Epstein F, Finlay JL (1998) Treatment of high-grade spinal cord astrocytoma of childhood with “8-in-1” chemotherapy and radiotherapy: a pilot study of CCG-945. Children’s Cancer Group. J Neurosurg 88:215–220. https://doi.org/10.3171/jns.1998.88.2.0215
Mayer RR, Warmouth GM, Troxell M, Adesina AM, Kass JS (2012) Glioblastoma multiforme of the conus medullaris in a 28-year-old female: a case report and review of the literature. Clin Neurol Neurosurg 114:275–277. https://doi.org/10.1016/j.clineuro.2011.10.017
Ryu SJ, Kim JY, Kim KH, Park JY, Kuh SU, Chin DK, Kim KS, Cho YE, Kim SH (2016) A retrospective observational study on the treatment outcomes of 26 patients with spinal cord astrocytoma including two cases of malignant transformation. Eur Spine J 25:4067–4079. https://doi.org/10.1007/s00586-016-4475-7
Chamberlain MC, Tredway TL (2011) Adult primary intradural spinal cord tumors: a review. Curr Neurol Neurosci 11:320–328. https://doi.org/10.1007/s11910-011-0190-2*10.1007/s11910-011-0190-2
Kim WH, Yoon SH, Kim CY, Kim KJ, Lee MM, Choe G, Kim IA, Kim JH, Kim YJ, Kim HJ (2011) Temozolomide for malignant primary spinal cord glioma: an experience of six cases and a literature review. J Neurooncol 101:247–254. https://doi.org/10.1007/s11060-010-0249-y
Chamberlain MC (2008) Temozolomide for recurrent low-grade spinal cord gliomas in adults. Cancer 113:1019–1024. https://doi.org/10.1002/cncr.23677
Kaley TJ, Mondesire-Crump I, Gavrilovic IT (2012) Temozolomide or bevacizumab for spinal cord high-grade gliomas. J Neuro-Oncol 109:385–389. https://doi.org/10.1007/s11060-012-0905-5
Chamberlain MC, Johnston SK (2011) Recurrent spinal cord glioblastoma: salvage therapy with bevacizumab. J Neurooncol 102:427–432. https://doi.org/10.1007/s11060-010-0330-6
Shankar GM, Lelic N, Gill CM, Thorner AR, Van Hummelen P, Wisoff JH, Loeffler JS, Brastianos PK, Shin JH, Borges LF, Butler WE, Zagzag D, Brody RI, Duhaime AC, Taylor MD, Hawkins CE, Louis DN, Cahill DP, Curry WT, Meyerson M (2016) BRAF alteration status and the histone H3F3A gene K27M mutation segregate spinal cord astrocytoma histology. Acta Neuropathol 131:147–150. https://doi.org/10.1007/s00401-015-1492-2
Sloan EA, Cooney T, Oberheim Bush NA, Buerki R, Taylor J, Clarke JL, Torkildson J, Kline C, Reddy A, Mueller S, Banerjee A, Butowski N, Chang S, Mummaneni PV, Chou D, Tan L, Theodosopoulos P, McDermott M, Berger M, Raffel C, Gupta N, Sun PP, Li Y, Shah V, Cha S, Braunstein S, Raleigh DR, Samuel D, Scharnhorst D, Fata C, Guo H, Moes G, Kim JYH, Koschmann C, Van Ziffle J, Onodera C, Devine P, Grenert JP, Lee JC, Pekmezci M, Phillips JJ, Tihan T, Bollen AW, Perry A, Solomon DA (2019) Recurrent non-canonical histone H3 mutations in spinal cord diffuse gliomas. Acta Neuropathol 138:877–881. https://doi.org/10.1007/s00401-019-02072-2
Gessi M, Gielen GH, Dreschmann V, Waha A, Pietsch T (2015) High frequency of H3F3A K27M mutations characterizes pediatric and adult high-grade gliomas of the spinal cord. Acta Neuropathol 130:435–437. https://doi.org/10.1007/s00401-015-1463-7
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The study was approved by the ethical board of Xuanwu Hospital.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Cheng, L., Yao, Q., Ma, L. et al. Predictors of mortality in patients with primary spinal cord glioblastoma. Eur Spine J 29, 3203–3213 (2020). https://doi.org/10.1007/s00586-020-06515-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06515-3