Abstract
Purpose
Many studies reported mid-term clinical and radiological outcomes after cervical disc arthroplasty. Only a few studies analysed the long-term results. The aim of the study was to evaluate the clinical and radiological outcomes in patients treated with single-level Bryan cervical disc arthroplasty after 18 years of follow-up.
Methods
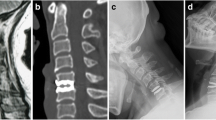
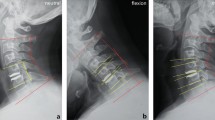
This study was a retrospective analysis of institutional databases concerning patients treated with Bryan cervical disc arthroplasty. SF36 PCS, NDI and VAS were used to evaluate clinical and functional outcomes. Standard, flexion–extension X-ray and MRI were used to evaluate the radiological results.
Results
Fifty-seven patients treated with single-level Bryan cervical disc arthroplasty completed the 18-year follow-up. At the final follow-up, a residual movement was observed in 32 patients (56%). The treated level range of motion decreased from 10.1° pre-operatively to 6.1° at the last follow-up (p = 0.0021). The range of motion of the adjacent segments and of the cervical spine had no significant change. Disc degeneration of the adjacent segment after 18-year follow-up was observed in 77.1% of treated patients.
Conclusion
The clinical and radiographic outcomes 18 years after surgery are acceptable. The treated level range of motion reduction and the adjacent segment degeneration seems not to affect the clinical results after 18 years of follow-up.




Similar content being viewed by others
References
Badhiwala JH, Wilson JR (2018) The natural history of degenerative cervical myelopathy. Neurosurg Clin N Am 29:21–32. https://doi.org/10.1177/2192568217700396
Burkhardt BW, Brielmaier M, Schwerdtfeger K, Oertel JM (2018) Clinical outcome following anterior cervical discectomy and fusion with and without anterior cervical plating for the treatment of cervical disc herniation-a 25-year follow-up study. Neurosurg Rev 41:473–482. https://doi.org/10.1007/s10143-017-0872-6
Liu N, Lu T, Wang Y, Sun Z, Li J, He X (2019) Effects of new cage profiles on the improvement in biomechanical performance of multilevel anterior cervical Corpectomy and fusion: a finite element analysis. World Neurosurg 129:e87–e96. https://doi.org/10.1016/j.wneu.2019.05.037
Sasso WR, Smucker JD, Sasso MP, Sasso RC (2017) Long-term clinical outcomes of cervical disc Arthroplasty: a prospective, randomized, controlled trial. Spine (Phila Pa 1976) 42:209–216. https://doi.org/10.1097/BRS.0000000000001746
Goffin JL, Casey A, Kehr P, Liebig K, Lind B, Logroscino C, Pointillart V, Van Calenbergh F, van Loon J (2002) Preliminary clinical experience with the Bryan cervical disc prosthesis. Neurosurgery 51:840–845. https://doi.org/10.1227/00006123-200209000-00048
Miller J, Sasso R, Anderson P, Riew KD, McPhilamy A, Gianaris T (2018) Adjacent level degeneration: bryan total disc arthroplasty versus anterior cervical discectomy and fusion. Clin Spine Surg 31:E98–E101. https://doi.org/10.1097/BSD.0000000000000598
Song Q, He D, Han XL, Zhang N, Wang J, Tian W (2018) Clinical and radiological outcomes of cervical disc arthroplasty: ten year follow-up study. Int Orthop 42:2389–2396. https://doi.org/10.1007/s00264-018-3947-2(Epub 2018 Apr 21)
Mehren C, Suchomel P, Grochulla F, Barsa P, Sourkova P, Hradil J, Korge A, Mayer HM (2006) Heterotopic ossification in total cervical artificial disc replacement. Spine (Phila Pa 1976) 31:2802–2806. https://doi.org/10.1097/01.brs.0000245852.70594.d5
Pfirrmann CW, Metzdorf A, Zanetti M, Hodler J, Boos N (2001) Magnetic resonance classification of lumbar intervertebral disc degeneration. Spine (Phila Pa 1976) 26:1873–1878
Lee JH, Park WM, Kim YH, Jahng TA (2016) A biomechanical analysis of an artificial disc with a shock-absorbing core property by using whole-cervical spine finite element analysis. Spine 41:E893–E901. https://doi.org/10.1097/brs.0000000000001468
Tian W, Yan K, Han X, Yu J, Jin P, Han X (2017) Comparison of the clinical and radiographic results between cervical artificial disk replacement and anterior cervical fusion: a 6-year prospective nonrandomized comparative study. Clin Spine Surg 30:E578–E586. https://doi.org/10.1097/bsd.0000000000000206
Han X, He D, Zhang N, Song Q, Wang J, Tian W (2019) Comparison of 10-year outcomes of bryan cervical disc arthroplasty for myelopathy and radiculopathy. Orthop Surg 11:1127–1134. https://doi.org/10.1111/os.12565
Zhao Y, Zhang Y, Sun Y, Pan S, Zhou F, Liu Z (2016) Application of cervical arthroplasty with Bryan cervical disc: 10-year follow-up results in China. Spine 41:111–115. https://doi.org/10.1097/brs.0000000000001145
Dejaegher J, Walraevens J, van Loon J, Van Calenbergh F, Demaerel P, Goffin J (2017) 10-year follow-up after implantation of the Bryan cervical disc prosthesis. Eur Spine J 26:1191–1198. https://doi.org/10.1007/s00586-016-4897-2
Wu JC, Huang WC, Tu TH, Tsai HW, Ko CC, Wu CL, Cheng H (2012) Differences between soft-disc herniation and spondylosis in cervical arthroplasty: CT-documented heterotopic ossification with minimum 2 years of follow-up. J Neurosurg Spine 16:163–171. https://doi.org/10.3171/2011.10.SPINE11497
Leung C, Casey AT, Goffin J, Kehr P, Liebig K, Lind B, Logroscino C, Pointillart V (2005) Clinical significance of heterotopic ossification in cervical disc replacement: a prospective multicenter clinical trial. Neurosurgery 57:759–763
De Vitis R, Passiatore M, Cilli V, Maffeis J, Milano G, Taccardo G (2020) Intramedullary nailing for treatment of forearm non-union: is it useful?—a case series. J Orthop 10(20):97–104. https://doi.org/10.1016/j.jor.2020.01.011
De Vitis R, Passiatore M, Perna A, Tulli A, Pagliei A, Taccardo G (2019) Modified Matti-Russe technique using a “butterfly bone graft” for treatment of scaphoid non-union. J Orthop 27(19):63–66. https://doi.org/10.1016/j.jor.2019.11.030
Proietti L, Scaramuzzo L, Schirò GR, Sessa S, Tamburrelli FC, Cerulli G (2015) Degenerative facet joint changes in lumbar percutaneous pedicle screw fixation without fusion. Orthop Traumatol Surg Res 101:375–379. https://doi.org/10.1016/j.otsr.2015.01.013
Song KJ, Choi BW, Jeon TS, Lee KB, Chang H (2011) Adjacent segment degenerative disease: is it due to disease progression or a fusion-associated phenomenon? Comparison between segments adjacent to the fused and non-fused segments. Eur Spine J 20:1940–1945. https://doi.org/10.1007/s00586-011-1864-9
Ricciardi L, Stifano V, Proietti L, Perna A, Della Pepa GM, La Rocca G, Olivi A, Polli FM (2018) Intraoperative and postoperative segmental lordosis mismatch: analysis of 3 fusion techniques. World Neurosurg 115:e659–e663. https://doi.org/10.1016/j.wneu.2018.04.126
Proietti L, Schirò GR, Sessa S, Scaramuzzo L (2014) The impact of sagittal balance on low back pain in patients treated with zygoapophysial facet joint injection. Eur Spine J 6:628–633. https://doi.org/10.1007/s00586-014-3559-5
Fong SY, DuPlessis SJ, Casha S, Hurlbert RJ (2006) Design limitations of Bryan disc arthroplasty. Spine J 6:233–241. https://doi.org/10.1016/j.spinee.2006.01.007
Goffin J, van Loon J, Van Calenbergh F, Lipscomb B (2010) A clinical analysis of 4- and 6-year follow-up results after cervical disc replacement surgery using the bryan cervical disc prosthesis. J Neurosurg Spine 12:261–269. https://doi.org/10.3171/2009.9.SPINE09129
Wenger M, Pv Hoonacker, Zachee B, Lange R, Markwalder TM (2009) Bryan cervical disc prostheses: preservation of function over time. J Clin Neurosci 16:220–225. https://doi.org/10.1016/j.jocn.2008.01.021
Acknowledgements
None.
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors declare that they have no conflict of interest.
Ethical approval
All procedures performed were in accordance with the 1964 Helsinki declaration. This research has been approved by the IRB of the authors’ affiliated institutions.
Informed consent
Written informed consent for scientific purposes and clinical data collection was obtained according to institutional protocol.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Genitiempo, M., Perna, A., Santagada, D.A. et al. Single-level Bryan cervical disc arthroplasty: evaluation of radiological and clinical outcomes after 18 years of follow-up. Eur Spine J 29, 2823–2830 (2020). https://doi.org/10.1007/s00586-020-06486-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06486-5