Abstract
Background
Acute kidney injury (AKI) often occurs in pediatric patients who received allogeneic hematopoietic cell transplantation (HCT). We evaluated the risk and effect of HCT-related AKI in pediatric patients.
Methods
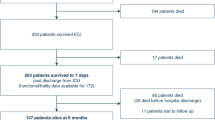
We retrospectively studied the survival and renal outcome of 69 children 100 days and 1-year posttransplant in our institution in 2004–2016. Stage-3 AKI developed in 34 patients (49%) until 100 days posttransplant.
Results
The 100-day overall survival (OS) rates of patients with stage-3 AKI were lower than those without it (76.5% vs. 94.3%, P = 0.035). The 1-year OS rates did not differ markedly between 21 post-100-day survivors with stage-3 AKI and 29 without it (80.8% vs. 87.9%, P = 0.444). The causes of 19 deaths included the relapse of underlying disease or graft failure (n = 11), treatment-related events (4), and second HCT-related events (4). Underlying disease of malignancy (crude hazard ratio (HR) 5.7; 95% confidence interval (CI), 2.20 to 14.96), > 1000 ng/mL ferritinemia (crude HR 4.29; 95% CI, 2.11 to 8.71), stem cell source of peripheral (crude HR 2.96; 95% CI, 1.22 to 7.20) or cord blood (crude HR 2.29; 95% CI, 1.03 to 5.06), and myeloablative regimen (crude HR 2.56; 95% CI, 1.24 to 5.26), were identified as risk factors for stage-3 AKI until 100 days posttransplant. Hyperferritinemia alone was significant (adjusted HR 5.52; 95% CI, 2.21 to 13.76) on multivariable analyses.
Conclusions
Hyperferritinemia was associated with stage-3 AKI and early mortality posttransplant. Pretransplant iron control may protect the kidney of pediatric HCT survivors.


Similar content being viewed by others
Abbreviations
- AKI:
-
Acute kidney injury
- HCT:
-
Hematopoietic cell transplantation
- OS:
-
Overall survival
- HR:
-
Hazard ratio
- CI:
-
Confidence interval
- HLA:
-
Human leukocyte antigen
- TBI:
-
Total body irradiation
- VOD:
-
Veno-occlusive disease
- GVHD:
-
Graft-versus-host disease
- CMV:
-
Cytomegalovirus
- SOS:
-
Sinusoidal obstruction syndrome
References
D’Souza A, Fretham C (2018) Current uses and outcomes of hematopoietic cell transplantation (HCT): CIBMTR summary slides. https://www.cibmtr.org. Accessed 01 November 2019
Niederwieser D, Baldomero H, Szer J, Gratwohl M, Aljurf M, Atsuta Y, Bouzas LF, Confer D, Greinix H, Horowitz M, Iida M, Lipton J, Mohty M, Novitzky N, Nunez J, Passweg J, Pasquini MC, Kodera Y, Apperley J, Seber A, Gratwohl A (2016) Hematopoietic stem cell transplantation activity worldwide in 2012 and a SWOT analysis of the worldwide network for blood and marrow transplantation group including the global survey. Bone Marrow Transplant 51:778–785
Koh KN, Sunkara A, Kang G, Sooter A, Mulrooney DA, Triplett B, Onder AM, Bissler J, Cunningham LC (2018) Acute kidney injury in pediatric patients receiving allogeneic hematopoietic cell transplantation: incidence, risk factors, and outcomes. Biol Blood Marrow Transplant 24:758–764
Ileri T, Ertem M, Ozcakar ZB, Ince EU, Biyikli Z, Uysal Z, Ekim M, Yalcinkaya F (2010) Prospective evaluation of acute and chronic renal function in children following matched related donor hematopoietic stem cell transplantation. Pediatr Transplant 14:138–144
Hazar V, Gungor O, Guven AG, Aydin F, Akbas H, Gungor F, Tezcan G, Akman S, Yesilipek A (2009) Renal function after hematopoietic stem cell transplantation in children. Pediatr Blood Cancer 53:197–202
Kist-van Holthe JE, Goedvolk CA, Brand R, van Weel MH, Bredius RG, van Oostayen JA, Vossen JM, van der Heijden BJ (2002) Prospective study of renal insufficiency after bone marrow transplantation. Pediatr Nephrol 17:1032–1037
Kist-van Holthe JE, van Zwet JM, Brand R, van Weel MH, Vossen JM, van der Heijden AJ (1998) Bone marrow transplantation in children: consequences for renal function shortly after and 1 year post-BMT. Bone Marrow Transplant 22:559–564
Esiashvili N, Chiang KY, Hasselle MD, Bryant C, Riffenburgh RH, Paulino AC (2009) Renal toxicity in children undergoing total body irradiation for bone marrow transplant. Radiother Oncol 90:242–246
Bao YS, Xie RJ, Wang M, Feng SZ, Han MZ (2011) An evaluation of the RIFLE criteria for acute kidney injury after myeloablative allogeneic haematopoietic stem cell transplantation. Swiss Med Wkly 141:w13225
Armand P, Kim HT, Cutler CS, Ho VT, Koreth J, Alyea EP, Soiffer RJ, Antin JH (2007) Prognostic impact of elevated pretransplantation serum ferritin in patients undergoing myeloablative stem cell transplantation. Blood 109:4586–4588
Pullarkat V, Blanchard S, Tegtmeier B, Dagis A, Patane K, Ito J, Forman SJ (2008) Iron overload adversely affects outcome of allogeneic hematopoietic cell transplantation. Bone Marrow Transplant 42:799–805
Kataoka K, Nannya Y, Hangaishi A, Imai Y, Chiba S, Takahashi T, Kurokawa M (2009) Influence of pretransplantation serum ferritin on nonrelapse mortality after myeloablative and nonmyeloablative allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 15:195–204
Martines AM, Masereeuw R, Tjalsma H, Hoenderop JG, Wetzels JF, Swinkels DW (2013) Iron metabolism in the pathogenesis of iron-induced kidney injury. Nat Rev Nephrol 9:385–398
Raina R, Herrera N, Krishnappa V, Sethi SK, Deep A, Kao WM, Bunchman T, Abu-Arja R (2017) Hematopoietic stem cell transplantation and acute kidney injury in children: a comprehensive review. Pediatr Transplant 21:e12935. https://doi.org/10.1111/petr.12935
Didsbury MS, Mackie FE, Kennedy SE (2015) A systematic review of acute kidney injury in pediatric allogeneic hematopoietic stem cell recipients. Pediatr Transplant 19:460–470
Michael M, Kuehnle I, Goldstein SL (2004) Fluid overload and acute renal failure in pediatric stem cell transplant patients. Pediatr Nephrol 19:91–95
Uemura O, Nagai T, Ishikura K, Ito S, Hataya H, Gotoh Y, Fujita N, Akioka Y, Kaneko T, Honda M (2014) Creatinine-based equation to estimate the glomerular filtration rate in Japanese children and adolescents with chronic kidney disease. Clin Exp Nephrol 18:626–633
Mehta RL, Kellum JA, Shah SV, Molitoris BA, Ronco C, Warnock DG, Levin A (2007) Acute kidney injury network: report of an initiative to improve outcomes in acute kidney injury. Crit Care 11:R31
Gyurkocza B, Sandmaier BM (2014) Conditioning regimens for hematopoietic cell transplantation: one size does not fit all. Blood 124:344–353
Przepiorka D, Weisdorf D, Martin P, Klingemann HG, Beatty P, Hows J, Thomas ED (1995) 1994 consensus conference on acute GVHD grading. Bone Marrow Transplant 15:825–828
Ishida H, Kato M, Kudo K, Taga T, Tomizawa D, Miyamura T, Goto H, Inagaki J, Koh K, Terui K, Ogawa A, Kawano Y, Inoue M, Sawada A, Kato K, Atsuta Y, Yamashita T, Adachi S (2015) Comparison of outcomes for pediatric patients with acute myeloid leukemia in remission and undergoing allogeneic hematopoietic cell transplantation with myeloablative conditioning regimens based on either intravenous busulfan or total body irradiation: a report from the Japanese Society for Hematopoietic Cell Transplantation. Biol Blood Marrow Transplant 12:2141–2147
Gupta A, Fu P, Hashem H, Vatsayan A, Shein S, Dalal J (2017) Outcomes and healthcare utilization in children and young adults with aplastic anemia: a multiinstitutional analysis. Pediatr Blood Cancer 12:10
Vichinsky E, Butensky E, Fung E, Hudes M, Theil E, Ferrell L, Williams R, Louie L, Lee PD, Harmatz P (2005) Comparison of organ dysfunction in transfused patients with SCD or beta thalassemia. Am J Hematol 80:70–74
Meloni A, Puliyel M, Pepe A, Berdoukas V, Coates TD, Wood JC (2014) Cardiac iron overload in sickle-cell disease. Am J Hematol 89:678–683
Aldudak B, Karabay Bayazit A, Noyan A, Ozel A, Anarat A, Sasmaz I, Kilinç Y, Gali E, Anarat R, Dikmen N (2000) Renal function in pediatric patients with beta-thalassemia major. Pediatr Nephrol 15:109–112
Ozkurt S, Acikalin MF, Temiz G, Akay OM, Soydan M (2014) Renal hemosiderosis and rapidly progressive glomerulonephritis associated with primary hemochromatosis. Ren Fail 36:814–816
Gardenghi S, Marongiu MF, Ramos P, Guy E, Breda L, Chadburn A, Liu Y, Amariglio N, Rechavi G, Rachmilewitz EA, Breuer W, Cabantchik ZI, Wrighting DM, Andrews NC, de Sousa M, Giardina PJ, Grady RW, Rivella S (2007) Ineffective erythropoiesis in beta-thalassemia is characterized by increased iron absorption mediated by down-regulation of hepcidin and up-regulation of ferroportin. Blood 109:5027–5035
Nakamura T, Naguro I, Ichijo H (2019) Iron homeostasis and iron-regulated ROS in cell death, senescence and human diseases. Biochim Biophys Acta Gen Subj 1863:1398–1409
Dixon SJ, Lemberg KM, Lamprecht MR, Skouta R, Zaitsev EM, Gleason CE, Patel DN, Bauer AJ, Cantley AM, Yang WS, Morrison B 3rd, Stockwell BR (2012) Ferroptosis: an iron-dependent form of nonapoptotic cell death. Cell 149:1060–1072
Linkermann A, Bräsen JH, Darding M, Jin MK, Sanz AB, Heller JO, De Zen F, Weinlich R, Ortiz A, Walczak H, Weinberg JM, Green DR, Kunzendorf U, Krautwald S (2013) Two independent pathways of regulated necrosis mediate ischemia-reperfusion injury. Proc Natl Acad Sci U S A 110:12024–12029
Sheerin NS, Sacks SH, Fogazzi GB (1999) In vitro erythrophagocytosis by renal tubular cells and tubular toxicity by haemoglobin and iron. Nephrol Dial Transplant 14:1391–1397
Walker PD, Shah SV (1991) Hydrogen peroxide cytotoxicity in LLC-PK1 cells: a role for iron. Kidney Int 40:891–898
Sánchez-González PD, López-Hernandez FJ, Morales AI, Macías-Nuñez JF, López-Novoa JM (2011) Effects of deferasirox on renal function and renal epithelial cell death. Toxicol Lett 203:154–161
Scindia Y, Dey P, Thirunagari A, Liping H, Rosin DL, Floris M, Okusa MD, Swaminathan S (2015) Hepcidin mitigates renal ischemia-reperfusion injury by modulating systemic Iron homeostasis. J Am Soc Nephrol 26:2800–2814
Mishra J, Ma Q, Prada A, Mitsnefes M, Zahedi K, Yang J, Barasch J, Devarajan P (2003) Identification of neutrophil gelatinase-associated lipocalin as a novel early urinary biomarker for ischemic renal injury. J Am Soc Nephrol 14:2534–2543
Acknowledgements
We thank Emeritus Prof. Toshiro Hara, Prof. Akinobu Matsuzaki, Dr. Takeshi Inamitsu, Dr. Aiko Suminoe, and Prof. Hidetoshi Takada (belonged to Department of Pediatrics, Kyushu University Hospital), along with all of the staff who treated the patients in Kyushu University Hospital.
Author information
Authors and Affiliations
Contributions
MK, KN, YK, and SO were the principal investigators, taking primary responsibility for the paper. KE, TI, UO, AS, and MI performed the clinical management with helpful discussion regarding the completion of the work. HN and NK conducted critical care. SH gave advice on the statistical analyses.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kurokawa, M., Nishiyama, K., Koga, Y. et al. Hyperferritinemia and acute kidney injury in pediatric patients receiving allogeneic hematopoietic cell transplantation. Pediatr Nephrol 35, 1977–1984 (2020). https://doi.org/10.1007/s00467-020-04619-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-020-04619-y