Abstract
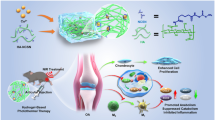
Osteoarthritis (OA), in which inflammation plays a crucial role, is the most common joint disease characterized by cartilage degradation. Neferine (Nef), a dibenzyl isoquinoline alkaloid, has shown its anti-inflammatory effects on other inflammatory diseases. Therefore, we hypothesized that Nef might also have an anti-inflammatory effect on OA and explored its effect on IL-1β-treated rat chondrocytes. Sprague Dawley (SD) rat chondrocytes were stimulated with IL-1β (10 ng/ml) and Nef (1, 5, and 10 μM) or IL-1β (10 ng/ml) alone for 24 h. Expression of inducible nitric oxide synthase (iNOS), cyclooxygenase 2 (COX-2), matrix metalloproteinases (MMPs), and thrombospondin motifs-5 (ADAMTS5) was determined by quantitative real-time PCR and Western blotting. Expression of collagen II and aggrecan was examined by Western blotting, immunofluorescence, and safranin O staining. In addition, activation of MAPK and NF-κB signaling pathway was examined by Western blotting, and p65 nuclear translocation was evaluated by immunofluorescence. Nef reduced expression of inflammatory regulators (iNOS and COX-2) in IL-1β-treated chondrocytes. Expression of IL-1β-induced major catabolic enzymes (MMP3, MMP13, and ADAMTS5) was inhibited by Nef. Meanwhile, downregulation of collagen II and aggrecan expression was also ameliorated. Furthermore, Nef dampened abnormal activation of MAPK and NF-κB signaling pathway triggered by IL-1β. Overall, the results above showed that Nef inhibited IL-1β-induced excess production of inflammatory and catabolic factors in rat chondrocytes via inhibiting the MAPK and NF-κB pathways, suggesting a promising pharmacotherapy for OA.







Similar content being viewed by others
Change history
19 October 2022
A Correction to this paper has been published: https://doi.org/10.1007/s10753-022-01760-8
References
Mandl, L.A. 2019. Osteoarthritis year in review 2018: Clinical. Osteoarthritis and Cartilage 27 (3): 359–364. https://doi.org/10.1016/j.joca.2018.11.001.
Chen, Di, Jie Shen, Weiwei Zhao, Tingyu Wang, Han Lin, John L. Hamilton, and Hee-Jeong Im. 2017. Osteoarthritis: Toward a comprehensive understanding of pathological mechanism. Bone Res 5: 16044. https://doi.org/10.1038/boneres.2016.44.
Vina, E.R., and C.K. Kwoh. 2018. Epidemiology of osteoarthritis: Literature update. Current Opinion in Rheumatology 30 (2): 160–167. https://doi.org/10.1097/BOR.0000000000000479.
Kye, Su-Yeon, and Keeho Park. 2017. Suicidal ideation and suicidal attempts among adults with chronic diseases: A cross-sectional study. Comprehensive Psychiatry 73: 160–167. https://doi.org/10.1016/j.comppsych.2016.12.001.
Veronese, Nicola, Brendon Stubbs, Marco Solmi, Toby O. Smith, Marianna Noale, Cyrus Cooper, and Stefania Maggi. 2017. Association between lower limb osteoarthritis and incidence of depressive symptoms: Data from the osteoarthritis initiative. Age and Ageing 46 (3): 470–476. https://doi.org/10.1093/ageing/afw216.
Pelletier, J.P., J. Martel-Pelletier, and S.B. Abramson. 2001. Osteoarthritis, an inflammatory disease: Potential implication for the selection of new therapeutic targets. Arthritis and Rheumatism 44 (6): 1237–1247. https://doi.org/10.1002/1529-0131(200106)44:6<1237::Aid-art214>3.0.Co;2-f.
Kapoor, M., J. Martel-Pelletier, D. Lajeunesse, J.P. Pelletier, and H. Fahmi. 2011. Role of proinflammatory cytokines in the pathophysiology of osteoarthritis. Nature Reviews Rheumatology 7 (1): 33–42. https://doi.org/10.1038/nrrheum.2010.196.
Appleton, C.T. 2018. Osteoarthritis year in review 2017: Biology. Osteoarthritis and Cartilage 26 (3): 296–303. https://doi.org/10.1016/j.joca.2017.10.008.
Malemud, C.J. 2015. Biologic basis of osteoarthritis: State of the evidence. Current Opinion in Rheumatology 27 (3): 289–294. https://doi.org/10.1097/bor.0000000000000162.
Panina, Svetlana B., Igor V. Krolevets, Natalia P. Milyutina, Alexander B. Sagakyants, Igor V. Kornienko, Anzhelika A. Ananyan, Mikhail A. Zabrodin, Andrey A. Plotnikov, and Valeriy V. Vnukov. 2017. Circulating levels of proinflammatory mediators as potential biomarkers of post-traumatic knee osteoarthritis development. Journal of Orthopaedics and Traumatology 18 (4): 349–357. https://doi.org/10.1007/s10195-017-0473-8.
Loeser, R.F. 2006. Molecular mechanisms of cartilage destruction: Mechanics, inflammatory mediators, and aging collide. Arthritis and Rheumatism 54 (5): 1357–1360. https://doi.org/10.1002/art.21813.
Mueller, M.B., and R.S. Tuan. 2011. Anabolic/catabolic balance in pathogenesis of osteoarthritis: Identifying molecular targets. PM & R : The Journal of Injury, Function, and Rehabilitation 3 (6 Suppl 1): S3–S11. https://doi.org/10.1016/j.pmrj.2011.05.009.
Furukawa, H. 1965. On the alkaloids of Nelumbo Nucifera Gaertn. IX. Alkaloids of loti embryo. (2). Structure of neferine, a new biscoclaurine alkaloid. Yakugaku Zasshi 85: 335–338.
Wu, X., Y. Guo, X. Min, L. Pei, and X. Chen. 2018. Neferine, a bisbenzylisoquinoline alkaloid, ameliorates dextran sulfate sodium-induced ulcerative colitis. The American Journal of Chinese Medicine 46 (6): 1263–1279. https://doi.org/10.1142/S0192415X18500660.
Wu, C., J. Chen, R. Yang, F. Duan, S. Li, and X. Chen. 2019. Mitochondrial protective effect of neferine through the modulation of nuclear factor erythroid 2-related factor 2 signalling in ischaemic stroke. British Journal of Pharmacology 176 (3): 400–415. https://doi.org/10.1111/bph.14537.
Tang, Y.S., Y.H. Zhao, Y. Zhong, X.Z. Li, J.X. Pu, Y.C. Luo, and Q.L. Zhou. 2019. Neferine inhibits LPS-ATP-induced endothelial cell pyroptosis via regulation of ROS/NLRP3/Caspase-1 signaling pathway. Inflammation Research 68: 727–738. https://doi.org/10.1007/s00011-019-01256-6.
Kadioglu, O., B.Y.K. Law, S.W.F. Mok, S.W. Xu, T. Efferth, and V.K.W. Wong. 2017. Mode of action analyses of neferine, a bisbenzylisoquinoline alkaloid of Lotus (Nelumbo nucifera) against multidrug-resistant tumor cells. Frontiers in Pharmacology 8: 238. https://doi.org/10.3389/fphar.2017.00238.
Wong, V.K., A.G. Wu, J.R. Wang, L. Liu, and B.Y. Law. 2015. Neferine attenuates the protein level and toxicity of mutant huntingtin in PC-12 cells via induction of autophagy. Molecules 20 (3): 3496–3514. https://doi.org/10.3390/molecules20033496.
Pham, D.C., Y.C. Chang, S.R. Lin, Y.M. Fuh, M.J. Tsai, and C.F. Weng. 2018. FAK and S6K1 inhibitor, neferine, dually induces autophagy and apoptosis in human neuroblastoma cells. Molecules 23 (12). https://doi.org/10.3390/molecules23123110.
Priya, L.B., R. Baskaran, C.Y. Huang, and V.V. Padma. 2017. Neferine ameliorates cardiomyoblast apoptosis induced by doxorubicin: Possible role in modulating NADPH oxidase/ROS-mediated NFkappaB redox signaling cascade. Scientific Reports 7 (1): 12283. https://doi.org/10.1038/s41598-017-12060-9.
Chen, S., B. Chu, Y. Chen, X. Cheng, D. Guo, L. Chen, J. Wang, Z. Li, Z. Hong, and D. Hong. 2019. Neferine suppresses osteoclast differentiation through suppressing NF-kappaB signal pathway but not MAPKs and promote osteogenesis. Journal of Cellular Physiology. https://doi.org/10.1002/jcp.28857.
Dubreuil, Maureen, Qiong Louie-Gao, Christine E. Peloquin, Hyon K. Choi, Yuqing Zhang, and Tuhina Neogi. 2018. Risk of myocardial infarction with use of selected non-steroidal anti-inflammatory drugs in patients with spondyloarthritis and osteoarthritis. Annals of the Rheumatic Diseases 77 (8): 1137–1143. https://doi.org/10.1136/annrheumdis-2018-213089.
Cooper, Cyrus, Roland Chapurlat, Nasser Al-Daghri, Gabriel Herrero-Beaumont, Olivier Bruyere, Francois Rannou, Roland Roth, Daniel Uebelhart, and Jean-Yves Reginster. 2019. Safety of oral non-selective non-steroidal anti-inflammatory drugs in osteoarthritis: What does the literature say? Drugs & Aging 36: 15–24. https://doi.org/10.1007/s40266-019-00660-1.
Lu, W., J. Shi, J. Zhang, Z. Lv, F. Guo, H. Huang, W. Zhu, and A. Chen. 2016. CXCL12/CXCR4 axis regulates aggrecanase activation and cartilage degradation in a post-traumatic osteoarthritis rat model. International Journal of Molecular Sciences 17 (10). https://doi.org/10.3390/ijms17101522.
Shepard, N., and N. Mitchell. 1976. Simultaneous localization of proteoglycan by light and electron microscopy using toluidine blue OA study of epiphyseal cartilage. Journal of Histochemistry & Cytochemistry 24 (5):621–629. https://doi.org/10.1177/24.5.132503.
Schmitz, N., S. Laverty, V.B. Kraus, and T. Aigner. 2010. Basic methods in histopathology of joint tissues. Osteoarthritis and Cartilage 18 (Suppl 3): S113–S116. https://doi.org/10.1016/j.joca.2010.05.026.
Huang, W., C. Cheng, W.S. Shan, Z.F. Ding, F.E. Liu, W. Lu, W. He, J.G. Xu, and Z.S. Yin. 2019. Knockdown of SGK1 alleviates the IL-1beta-induced chondrocyte anabolic and catabolic imbalance by activating FoxO1-mediated autophagy in human chondrocytes. The FEBS Journal. https://doi.org/10.1111/febs.15009.
Bos, P.K., G.J. van Osch, D.A. Frenz, J.A. Verhaar, and H.L. Verwoerd-Verhoef. 2001. Growth factor expression in cartilage wound healing: Temporal and spatial immunolocalization in a rabbit auricular cartilage wound model. Osteoarthritis and Cartilage 9 (4): 382–389. https://doi.org/10.1053/joca.2000.0399.
Huang, X., Y. Xi, Q. Pan, Z. Mao, R. Zhang, X. Ma, and H. You. 2018. Caffeic acid protects against IL-1beta-induced inflammatory responses and cartilage degradation in articular chondrocytes. Biomedicine & Pharmacotherapy 107: 433–439. https://doi.org/10.1016/j.biopha.2018.07.161.
Mao, Z., P. Wang, Q. Pan, X. Huang, R. Zhang, X. Shang, X. Ma, and H. You. 2018. Pravastatin alleviates interleukin 1beta-induced cartilage degradation by restoring impaired autophagy associated with MAPK pathway inhibition. International Immunopharmacology 64: 308–318. https://doi.org/10.1016/j.intimp.2018.09.018.
Oda, Akinori, Ryota Takamiya, Rin Kaneko, Haruna Yoshida, Yuta Yanagita, Hatsumi Sekiguchi, Yoshihito Nobe, and Kazuaki Muramatsu. 2019. Utility of a rotation/revolution-type agitator for chondrocyte isolation during preparation of engineered cartilage. Journal of Bioscience and Bioengineering 128 (1): 117–122. https://doi.org/10.1016/j.jbiosc.2018.12.010.
Liacini, A., J. Sylvester, W.Q. Li, and M. Zafarullah. 2002. Inhibition of interleukin-1-stimulated MAP kinases, activating protein-1 (AP-1) and nuclear factor kappa B (NF-kappa B) transcription factors down-regulates matrix metalloproteinase gene expression in articular chondrocytes. Matrix Biology 21 (3): 251–262. https://doi.org/10.1016/s0945-053x(02)00007-0.
Pettipher, E.R., G.A. Higgs, and B. Henderson. 1986. Interleukin-1 induces leukocyte infiltration and cartilage proteoglycan degradation in the synovial joint. Proceedings of the National Academy of Sciences of the United States of America 83 (22): 8749–8753. https://doi.org/10.1073/pnas.83.22.8749.
Needleman, P., and P.T. Manning. 1999. Interactions between the inducible cyclooxygenase (COX-2) and nitric oxide synthase (iNOS) pathways: Implications for therapeutic intervention in osteoarthritis. Osteoarthritis and Cartilage 7 (4): 367–370. https://doi.org/10.1053/joca.1998.0237.
Pelletier, J.P., J.C. Fernandes, G. Tardif, V. Lascau-Coman, M. Dupuis, and J. Martel-Pelletier. 1998. Direct in vivo transfer of the IL-1Ra gene in osteoarthritic rabbit knee joints: Prevention of the disease progression. Arthritis and Rheumatism 41 (9): S342–S342.
Simkin, Peter A. 2009. Rethinking the physiology of articular cartilage. Journal of clinical Rheumatology 15 (5): 260–263. https://doi.org/10.1097/RHU.0b013e3181b1d873.
Stanton, H., F.M. Rogerson, C.J. East, S.B. Golub, K.E. Lawlor, C.T. Meeker, C.B. Little, K. Last, P.J. Farmer, I.K. Campbell, A.M. Fourie, and A.J. Fosang. 2005. ADAMTS5 is the major aggrecanase in mouse cartilage in vivo and in vitro. Nature 434 (7033): 648–652. https://doi.org/10.1038/nature03417.
Song, Ruo-Hua, Micky D. Tortorella, Anne-Marie Malfait, James T. Alston, Zhiyong Yang, Elizabeth C. Arner, and David W. Griggs. 2007. Aggrecan degradation in human articular cartilage explants is mediated by both ADAMTS-4 and ADAMTS-5. Arthritis and Rheumatism 56 (2): 575–585. https://doi.org/10.1002/art.22334.
Neuhold, L.A., L. Killar, W.G. Zhao, M.L.A. Sung, L. Warner, J. Kulik, J. Turner, et al. 2001. Postnatal expression in hyaline cartilage of constitutively active human collagenase-3 (MMP-13) induces osteoarthritis in mice. Journal of Clinical Investigation 107 (1): 35–44. https://doi.org/10.1172/jci10564.
Little, C.B., A. Barai, D. Burkhardt, S.M. Smith, A.J. Fosang, Z. Werb, M. Shah, and E.W. Thompson. 2009. Matrix metalloproteinase 13-deficient mice are resistant to osteoarthritic cartilage erosion but not chondrocyte hypertrophy or osteophyte development. Arthritis and Rheumatism 60 (12): 3723–3733. https://doi.org/10.1002/art.25002.
Fan, Z.Y., B. Bau, H.Q. Yang, and T. Aigner. 2004. IL-1 beta induction of IL-6 and LIF in normal articular human chondrocytes involves the ERK, p38 and NF kappa B signaling pathways. Cytokine 28 (1): 17–24. https://doi.org/10.1016/j.cyto.2004.06.003.
Saklatvala, J. 2007. Inflammatory signaling in cartilage: MAPK and NF-kappa B pathways in chondrocytes and the use of inhibitors for research into pathogenesis and therapy of osteoarthritis. Current Drug Targets 8 (2): 305–313. https://doi.org/10.2174/138945007779940115.
Herrero-Beaumont, Gabriel, Sandra Perez-Baos, Olga Sanchez-Pernaute, Jorge A. Roman-Blas, Ana Lamuedra, and Raquel Largo. 2019. Targeting chronic innate inflammatory pathways, the main road to prevention of osteoarthritis progression. Biochemical Pharmacology 165: 24–32. https://doi.org/10.1016/j.bcp.2019.02.030.
Yang, Da-Wei, Gui-Bin Qian, Ming-Jiu Jiang, Peng Wang, and Kun-Zheng Wang. 2019. Inhibition of microRNA-495 suppresses chondrocyte apoptosis through activation of the NF-kappaB signaling pathway by regulating CCL4 in osteoarthritis. Gene Therapy 26 (6): 217–229. https://doi.org/10.1038/s41434-019-0068-5.
Abramson, S.B. 2008. Osteoarthritis and nitric oxide. Osteoarthritis and Cartilage 16 (Suppl 2): S15–S20. https://doi.org/10.1016/s1063-4584(08)60008-4.
Schaefer, J.F., M.L. Millham, B. de Crombrugghe, and L. Buckbinder. 2003. FGF signaling antagonizes cytokine-mediated repression of Sox9 in SW1353 chondrosarcoma cells. Osteoarthritis and Cartilage 11 (4): 233–241.
Gebauer, M., J. Saas, F. Sohler, J. Haag, S. Soder, M. Pieper, E. Bartnik, J. Beninga, R. Zimmer, and T. Aigner. 2005. Comparison of the chondrosarcoma cell line SW1353 with primary human adult articular chondrocytes with regard to their gene expression profile and reactivity to IL-1beta. Osteoarthritis and Cartilage 13 (8): 697–708. https://doi.org/10.1016/j.joca.2005.04.004.
Funding
National Natural Science Foundation of China (Grant No. 81772390) and the Fundamental Research Funds for the Central Universities (Grant No. 2017KFYXJJ104) funded this research study.
Author information
Authors and Affiliations
Contributions
HY and BN conceived the experiments and wrote the manuscript. BN, XH, and YX carried out the cell experiments. ZM and XC purchased animals and isolated primary rat chondrocytes. RZ and XM analyzed the data and made charts and graphs. HY financed the study.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no competing interests.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Ni, B., Huang, X., Xi, Y. et al. Neferine Inhibits Expression of Inflammatory Mediators and Matrix Degrading Enzymes in IL-1β-Treated Rat Chondrocytes via Suppressing MAPK and NF-κB Signaling Pathways. Inflammation 43, 1209–1221 (2020). https://doi.org/10.1007/s10753-019-01143-6
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-019-01143-6