Abstract
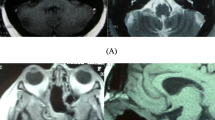
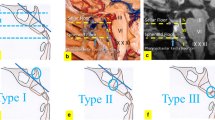
Chordoma is a rare slow-growing neoplastic bone lesion. However, they show an invasive local growth and high recurrence rate, leading to an overall survival rate of 65% at 5 years and 35% at 10 years. We conducted a pooled and meta-analysis comparing recurrence rate, post-operative-complications, and survival in patients undergoing either microsurgical (MA) or endoscopic approaches (EA). Search of literature was conducted in accordance with the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) guidelines to identify surgical series of clivus chordomas published between January 1990 and March 2018 on Pubmed, Scopus, and Cochrane. Two different statistical analyses have been performed: a pooled analysis and a single-arm meta-analysis of overall recurrence rate and subgroup meta-analysis of complications in the subgroups open surgery and endoscopic surgery. After full-text screening, a total of 58 articles were included in the pooled analysis and 27 studies were included for the study-level meta-analysis. Pooled analysis—the extent of resection was the only association that remained significant (subtotal: HR = 2.18, p = 0.004; partial: HR = 4.40, p < 0.001). Recurrence was more prevalent among the surgical patients (45.5%) compared to endoscopic ones (23.7%). Meta-analysis—results of the cumulative meta-analysis showed an overall rate of recurrence of 25.6%. MA recurrence rate was 31.8% (99% CI 14-52.8), EA recurrence rate was 19.4% (5.4-39.2). CSF leak rate for the endoscopic group was 10.3% (99%CI 5-17.3) and 9.5% (99%CI 1.2-24.6) for the open surgery group. The partial removal versus total removal has an influence on recurrence rate (p < 0.001). MA recurrence rate was 31.8%; EA recurrence rate was 19.4%. The extent of resection is confirmed as a statistically significant factor affecting the risk for recurrence both with the pooled analysis and with the meta-analysis. Meta-analysis demonstrated that older patients tend to recur more than young patients, especially in surgical group.




Similar content being viewed by others
References
Smoll NR, Gautschi OP, Radovanovic I, Schaller K, Weber DC (2013) Incidence and relative survival of chordomas: the standardized mortality ratio and the impact of chordomas on a population. Cancer 119(11):2029–2037. https://doi.org/10.1002/cncr.28032
McMaster ML, Goldstein AM, Bromley CM, Ishibe N, Parry DM (2001) Chordoma: incidence and survival patterns in the United States, 1973-1995. Cancer Causes Control 12(1):1–11. https://doi.org/10.1023/a:1008947301735
Chambers KJ, Lin DT, Meier J, Remenschneider A, Herr M, Gray ST (2014) Incidence and survival patterns of cranial chordoma in the United States. Laryngoscope 124(5):1097–1102. https://doi.org/10.1002/lary.24420
Labidi M, Watanabe K, Bouazza S, Bresson D, Bernat AL, George B, Froelich S (2016) Clivus chordomas: a systematic review and meta-analysis of contemporary surgical management. J Neurosurg Sci 60(4):476–484
Mukherjee D, Chaichana KL, Gokaslan ZL, Aaronson O, Cheng JS, McGirt MJ (2011) Survival of patients with malignant primary osseous spinal neoplasms: results from the surveillance, epidemiology, and end results (SEER) database from 1973 to 2003. J Neurosurg Spine 14(2):143–150. https://doi.org/10.3171/2010.10.SPINE10189
Stacchiotti S (2015) Sommer J; Chordoma Global Consensus Group. Building a global consensus approach to chordoma: a position paper from the medical and patient community. Lancet Oncol 16(2):e71–e83. https://doi.org/10.1016/S1470-2045(14)71190-8
Jägersberg M, El Rahal A, Dammann P, Merkler D, Weber DC, Schaller K (2017) Clival chordoma: a single-centre outcome analysis. Acta Neurochir 159(10):1815–1823. https://doi.org/10.1007/s00701-017-3163-7
Rousseau M, Evans J (2017) Key statistical assumptions and methods in one-arm metaanalyses with binary endpoints and low event rates, including a real-life example in the area of endoscopic colonic stenting. Cogent Med 4(1):1334318
Di Maio P, Iocca O, De Virgilio A et al (2018) Role of palatine tonsillectomy in the diagnostic workup of head and neck squamous cell carcinoma of unknown primary origin: a systematic review and meta-analysis. Head Neck 41:1–10. https://doi.org/10.1002/hed.25522
Higgins JPT, Green S (eds) (2011) Cochrane Handbook for Systematic Reviews of Interventions Version 5.1.0 [updated March 2011]. Cochrane Collab
Sekhar LN, Jannetta PJ, Burkhart LE, Janosky JE (1990) Meningiomas involving the clivus: a six-year experience with 41 patients. Neurosurgery 27(5):764–781
Fernandez-Miranda JC, Gardner PA, Snyderman CH, Devaney KO, Mendenhall WM, Suárez C, Rinaldo A, Ferlito A (2014) Clival chordomas: a pathological, surgical, and radiotherapeutic review. Head Neck 36(6):892–906. https://doi.org/10.1002/hed.23415
George B, Bresson D, Herman P, Froelich S (2015) Chordomas: a review. Neurosurg Clin N Am 26(3):437–452. https://doi.org/10.1016/j.nec.2015.03.012
Zoli M, Milanese L, Bonfatti R, Faustini-Fustini M, Marucci G, Tallini G, Zenesini C, Sturiale C, Frank G, Pasquini E, Mazzatenta D (2018) Clival chordomas: considerations after 16 years of endoscopic endonasal surgery. J Neurosurg 128(2):329–338. https://doi.org/10.3171/2016.11.JNS162082
Frank G, Sciarretta V, Calbucci F, Farneti G, Mazzatenta D, Pasquini E (2006) The endoscopic transnasal transsphenoidal approach for the treatment of cranial base chordomas and chondrosarcomas. Neurosurgery 59(1 Suppl 1):ONS50–ONS57. https://doi.org/10.1227/01.NEU.0000219914.17221.55
Cho YH, Kim JH, Khang SK, Lee JK, Kim CJ (2008) Chordomas and chondrosarcomas of the skull base: comparative analysis of clinical results in 30 patients. Neurosurg Rev 31:35–43
Colli BO, Al-Mefty O (2001) Chordomas of the skull base: followup review and prognostic factors. Neurosurg Focus 10:3E1
Crockard HA, Steel T, Plowman N, Singh A, Crossman J, Revesz T (2001) A multidisciplinary team approach to skull base chordomas. J Neurosurg 95:175–183
Jahangiri A, Chin AT, Wagner JR, Kunwar S, Ames C, Chou D, Barani I, Parsa AT, McDermott MW, Benet A, El-Sayed IH, Aghi MK (2015) Factors predicting recurrence after resection of clival chordoma using variable surgical approaches and radiation modalities. Neurosurgery 76(2):179–185; discussion 185-6. https://doi.org/10.1227/NEU.0000000000000611
Zou Y, Neale N, Sun J, Yang M, Bai HX, Tang L, Zhang Z, Landi A, Wang Y, Huang RY, Zhang PJ, Li X, Xiao B, Yang L (2018 Oct) Prognostic factors in clival chordomas: an integrated analysis of 347 patients. World Neurosurg 118:e375–e387. https://doi.org/10.1016/j.wneu.2018.06.194
Shkarubo AN, Koval KV, Kadashev BA, Andreev DN, Chernov IV (2018) Extended endoscopic endonasal posterior (transclival) approach to tumors of the clival region and ventral posterior cranial fossa. Part 3. Analysis of surgical treatment outcomes in 127 patients. Zh Vopr Neirokhir Im N N Burdenko 82(3):15–28. https://doi.org/10.17116/neiro201882315
Sekhar LN, Pranatartiharan R, Chanda A, Wright DC (2001) Chordomas and chondrosarcomas of the skull base: results and complications of surgical management. Neurosurg Focus 10:E2
Conger A, Zhao F, Wang X, Eisenberg A, Griffiths C, Esposito F, Carrau RL, Barkhoudarian G, Kelly DF (2018) Evolution of the graded repair of CSF leaks and skull base defects in endonasal endoscopic tumor surgery: trends in repair failure and meningitis rates in 509 patients. J Neurosurg 130(3):861–875. https://doi.org/10.3171/2017.11.JNS172141
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee (include name of committee + reference number) and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Cannizzaro, D., Tropeano, M.P., Milani, D. et al. Microsurgical versus endoscopic trans-sphenoidal approaches for clivus chordoma: a pooled and meta-analysis. Neurosurg Rev 44, 1217–1225 (2021). https://doi.org/10.1007/s10143-020-01318-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10143-020-01318-y