Abstract
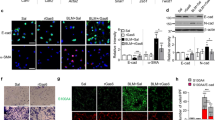
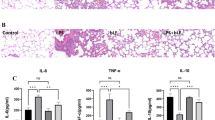
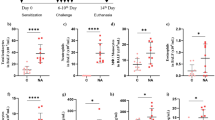
Angiotensin-II (Ang-II) receptor plays a role in allergic airway inflammation; however, the underlying mechanism and role of macrophages need better understanding. In the present study, angiotensin-II infusion (1 μg/kg/min) in ovalbumin-induced airway inflammation mice model significantly decreased immune cell infiltration, goblet cell hyperplasia, and eosinophil numbers in lungs. Ang-II infusion increased M1 and decreased M2 macrophage population in bronchoalveolar lavage fluid and respective macrophage markers in lung macrophages. Similarly, in vitro Ang-II treatment in murine bone marrow-derived macrophages (BMDMs) induced M1 and reduced M2 macrophage phenotype with enhanced bactericidal activity. Mechanistically, Ang-II inhibits Let-7c and miR-99a expression in BMDMs and in vivo as well. Lentiviral overexpression of Let-7c and miR-99a miRNAs in BMDMs abrogated Ang-II-induced M1 phenotype activation and promoted M2 phenotype, which is governed by targeting TNFα by miR-99a. In lung macrophages, ovalbumin-induced TNFα inhibition was rescued after Ang-II treatment. In BMDMs, knockdown of TNFα abrogated Ang-II-induced M2 to M1 macrophage phenotype switch and associated bactericidal activity. Ang-II affects mature miRNA formation by enhancing Lin28B levels in macrophages in vivo and in vitro. Furthermore, Lin28B knockdown prevented Ang-II-mediated inhibition of mature Let-7c/miR-99a miRNA formation, M2 to M1 macrophage phenotype switch, and increased bactericidal activity. Therefore, present study suggests a role of Lin28B in Ang-II-induced Let-7c/miR-99a miRNA formation that consequently affects TNFα production, M1 phenotype activation, and allergic airway inflammation.

Ovalbumin inhibits LIN28B expression thereby fails to inhibit premature to mature Let-7c/miR-99a miRNA formation. Mature miR-99a miRNA that inhibits TNFα consequently promotes M2 polarization and allergic airway inflammation.
While Ang-II induces Lin28B, which inhibits Let-7c/miR-99a miRNA processing and mature miRNA formation, this results in increased TNFα levels that lead to M1 polarization and allergic airway inflammation inhibition.








Similar content being viewed by others
Abbreviations
- AAI:
-
allergic airway inflammation
- BALF:
-
bronchoalveolar lavage fluid
- Angiotensin-II:
-
Ang-II
- MCSF:
-
macrophage colony stimulating factor
- BMDMs:
-
bone marrow-derived macrophages
- TNF:
-
tumor necrosis factor
- PPARγ:
-
peroxisome proliferator-activated receptor gamma
- 3’UTR:
-
3′untranslated region
- TU/ml:
-
transduction units per ml
- PFU:
-
plaque-forming unit
- CFU:
-
colony-forming unit
- hr.:
-
hour
- shTNF:
-
TNF-shRNA
- Chr:
-
chromosome
- H&E:
-
hematoxylin and eosin
- PAS:
-
periodic acid-Schiff
References
Martinez, F.D., and D. Vercelli. Asthma. Lancet 382 (9901): 1360–1372.
Locksley, R.M. 2010. Asthma and allergic inflammation. Cell 140 (6): 777–783.
Finkelman, F.D., S.P. Hogan, G.K. Hershey, M.E. Rothenberg, and M. Wills-Karp. 2010. Importance of cytokines in murine allergic airway disease and human asthma. Journal of Immunology 184 (4): 1663–1674.
Haworth, O., and B.D. Levy. 2007. Endogenous lipid mediators in the resolution of airway inflammation. The European Respiratory Journal 30 (5): 980–992.
Remuzzi, G., N. Perico, M. Macia, and P. Ruggenenti. 2005. The role of renin-angiotensin-aldosterone system in the progression of chronic kidney disease. Kidney International. Supplement 99: S57–S65. https://doi.org/10.1111/j.1523-1755.2005.09911.x.
Khan, B.V., D.G. Harrison, M.T. Olbrych, R.W. Alexander, and R.M. Medford. 1996. Nitric oxide regulates vascular cell adhesion molecule 1 gene expression and redox-sensitive transcriptional events in human vascular endothelial cells. Proceedings of the National Academy of Sciences of the United States of America 93 (17): 9114–9119.
Barnes, P.J., and M. Karin. 1997. Nuclear factor-kappaB: A pivotal transcription factor in chronic inflammatory diseases. The New England Journal of Medicine 336 (15): 1066–1071. https://doi.org/10.1056/NEJM199704103361506.
Dandona, P., V. Kumar, A. Aljada, H. Ghanim, T. Syed, D. Hofmayer, P. Mohanty, D. Tripathy, and R. Garg. 2003. Angiotensin II receptor blocker valsartan suppresses reactive oxygen species generation in leukocytes, nuclear factor-kappa B, in mononuclear cells of normal subjects: Evidence of an antiinflammatory action. The Journal of Clinical Endocrinology and Metabolism 88 (9): 4496–4501. https://doi.org/10.1210/jc.2002-021836.
Diep, Q.N., F. Amiri, R.M. Touyz, J.S. Cohn, D. Endemann, M.F. Neves, and E.L. Schiffrin. 2002. PPARalpha activator effects on Ang II-induced vascular oxidative stress and inflammation. Hypertension 40 (6): 866–871.
Diep, Q.N., M. El Mabrouk, J.S. Cohn, D. Endemann, F. Amiri, A. Virdis, M.F. Neves, and E.L. Schiffrin. 2002. Structure, endothelial function, cell growth, and inflammation in blood vessels of angiotensin II-infused rats: Role of peroxisome proliferator-activated receptor-gamma. Circulation 105 (19): 2296–2302.
Michel, M.C., H.R. Brunner, C. Foster, and Y. Huo. 2016. Angiotensin II type 1 receptor antagonists in animal models of vascular, cardiac, metabolic and renal disease. Pharmacology & Therapeutics 164: 1–81.
Coop, C.A., R.S. Schapira, and T.M. Freeman. 2017. Are ACE inhibitors and beta-blockers dangerous in patients at risk for anaphylaxis? The Journal of Allergy and Clinical Immunology. In Practice 5 (5): 1207–1211.
Ohwada, K., K. Watanabe, K. Okuyama, Y. Ohkawara, T. Sugaya, M. Takayanagi, and I. Ohno. 2007. The involvement of type 1a angiotensin II receptors in the regulation of airway inflammation in a murine model of allergic asthma. Clinical and Experimental Allergy 37 (11): 1720–1727.
Gordon, S., and P.R. Taylor. 2005. Monocyte and macrophage heterogeneity. Nature Reviews. Immunology 5 (12): 953–964. https://doi.org/10.1038/nri1733.
Biswas, S.K., and A. Mantovani. 2010. Macrophage plasticity and interaction with lymphocyte subsets: Cancer as a paradigm. Nature Immunology 11 (10): 889–896. https://doi.org/10.1038/ni.1937.
Mosser, D.M., and J.P. Edwards. 2008. Exploring the full spectrum of macrophage activation. Nature Reviews. Immunology 8 (12): 958–969. https://doi.org/10.1038/nri2448.
Karp, C.L., and P.J. Murray. 2012. Non-canonical alternatives: What a macrophage is 4. The Journal of Experimental Medicine 209 (3): 427–431.
Murray, P.J., and T.A. Wynn. 2011. Protective and pathogenic functions of macrophage subsets. Nature Reviews. Immunology 11 (11): 723–737. https://doi.org/10.1038/nri3073.
Nabe, T., H. Wakamori, C. Yano, A. Nishiguchi, R. Yuasa, H. Kido, Y. Tomiyama, A. Tomoda, H. Kida, A. Takiguchi, M. Matsuda, K. Ishihara, S. Akiba, S. Ohya, H. Fukui, N. Mizutani, and S. Yoshino. 2015. Production of interleukin (IL)-33 in the lungs during multiple antigen challenge-induced airway inflammation in mice, and its modulation by a glucocorticoid. European Journal of Pharmacology 757: 34–41. https://doi.org/10.1016/j.ejphar.2015.03.015.
Tiemessen, M.M., A.L. Jagger, H.G. Evans, M.J. van Herwijnen, S. John, and L.S. Taams. 2007. CD4+CD25+Foxp3+ regulatory T cells induce alternative activation of human monocytes/macrophages. Proceedings of the National Academy of Sciences of the United States of America 104 (49): 19446–19451. https://doi.org/10.1073/pnas.0706832104.
Wu, D., A.B. Molofsky, H.E. Liang, R.R. Ricardo-Gonzalez, H.A. Jouihan, J.K. Bando, A. Chawla, and R.M. Locksley. 2011. Eosinophils sustain adipose alternatively activated macrophages associated with glucose homeostasis. Science 332 (6026): 243–247. https://doi.org/10.1126/science.1201475.
Molofsky, A.B., J.C. Nussbaum, H.E. Liang, S.J. Van Dyken, L.E. Cheng, A. Mohapatra, A. Chawla, and R.M. Locksley. 2013. Innate lymphoid type 2 cells sustain visceral adipose tissue eosinophils and alternatively activated macrophages. The Journal of Experimental Medicine 210 (3): 535–549. https://doi.org/10.1084/jem.20121964.
Song, X., S. Xie, K. Lu, and C. Wang. 2015. Mesenchymal stem cells alleviate experimental asthma by inducing polarization of alveolar macrophages. Inflammation 38 (2): 485–492. https://doi.org/10.1007/s10753-014-9954-6.
Girodet, P.O., D. Nguyen, J.D. Mancini, M. Hundal, X. Zhou, E. Israel, and M. Cernadas. 2016. Alternative macrophage activation is increased in asthma. American Journal of Respiratory Cell and Molecular Biology 55 (4): 467–475. https://doi.org/10.1165/rcmb.2015-0295OC.
Moreira, A.P., K.A. Cavassani, R. Hullinger, R.S. Rosada, D.J. Fong, L. Murray, D.P. Hesson, and C.M. Hogaboam. 2010. Serum amyloid P attenuates M2 macrophage activation and protects against fungal spore-induced allergic airway disease. The Journal of Allergy and Clinical Immunology 126 (4): 712–721 e717. https://doi.org/10.1016/j.jaci.2010.06.010.
O'Neill, L.A., F.J. Sheedy, and C.E. McCoy. 2011. MicroRNAs: The fine-tuners of toll-like receptor signalling. Nature Reviews. Immunology 11 (3): 163–175.
Pua, H.H., D.F. Steiner, S. Patel, J.R. Gonzalez, J.F. Ortiz-Carpena, R. Kageyama, N.T. Chiou, A. Gallman, D. de Kouchkovsky, L.T. Jeker, M.T. McManus, D.J. Erle, and K.M. Ansel. 2016. MicroRNAs 24 and 27 suppress allergic inflammation and target a network of regulators of T helper 2 cell-associated cytokine production. Immunity 44 (4): 821–832.
Johansson, K., C. Malmhall, P. Ramos-Ramirez, and M. Radinger. 2017. MicroRNA-155 is a critical regulator of type 2 innate lymphoid cells and IL-33 signaling in experimental models of allergic airway inflammation. The Journal of Allergy and Clinical Immunology 139 (3): 1007–1016 e1009.
Lu, T.X., A. Munitz, and M.E. Rothenberg. 2009. MicroRNA-21 is up-regulated in allergic airway inflammation and regulates IL-12p35 expression. Journal of Immunology 182 (8): 4994–5002. https://doi.org/10.4049/jimmunol.0803560.
Sharma, A., M. Kumar, T. Ahmad, U. Mabalirajan, J. Aich, A. Agrawal, and B. Ghosh. 2012. Antagonism of mmu-mir-106a attenuates asthma features in allergic murine model. Journal of Applied Physiology (Bethesda, MD: 1985) 113 (3): 459–464.
Banerjee, S., N. Xie, H. Cui, Z. Tan, S. Yang, M. Icyuz, E. Abraham, and G. Liu. 2013. MicroRNA let-7c regulates macrophage polarization. Journal of Immunology 190 (12): 6542–6549. https://doi.org/10.4049/jimmunol.1202496.
Jaiswal, A., S. S. Reddy, M. Maurya, P. Maurya, and M. K. Barthwal. 2018. MicroRNA-99a mimics inhibit M1 macrophage phenotype and adipose tissue inflammation by targeting TNFalpha. Cellular & Molecular Immunology.
Liao, B., X. Bao, L. Liu, S. Feng, A. Zovoilis, W. Liu, Y. Xue, J. Cai, X. Guo, B. Qin, R. Zhang, J. Wu, L. Lai, M. Teng, L. Niu, B. Zhang, M.A. Esteban, and D. Pei. 2011. MicroRNA cluster 302-367 enhances somatic cell reprogramming by accelerating a mesenchymal-to-epithelial transition. The Journal of Biological Chemistry 286 (19): 17359–17364.
Sun, D., Y.S. Lee, A. Malhotra, H.K. Kim, M. Matecic, C. Evans, R.V. Jensen, C.A. Moskaluk, and A. Dutta. 2011. miR-99 family of MicroRNAs suppresses the expression of prostate-specific antigen and prostate cancer cell proliferation. Cancer Research 71 (4): 1313–1324.
Li, Q., J. Xie, B. Wang, R. Li, J. Bai, L. Ding, R. Gu, L. Wang, and B. Xu. 2016. Overexpression of microRNA-99a attenuates cardiac hypertrophy. PLoS One 11 (2): e0148480.
Newman, M.A., J.M. Thomson, and S.M. Hammond. 2008. Lin-28 interaction with the Let-7 precursor loop mediates regulated microRNA processing. Rna 14 (8): 1539–1549.
Gomolak, J.R., and S.P. Didion. 2014. Angiotensin II-induced endothelial dysfunction is temporally linked with increases in interleukin-6 and vascular macrophage accumulation. Frontiers in Physiology 5: 396. https://doi.org/10.3389/fphys.2014.00396.
Inada, Y., T. Nakane, and S. Chiba. 2002. Binding of KRH-594, an antagonist of the angiotensin II type 1 receptor, to cloned human and rat angiotensin II receptors. Fundamental & Clinical Pharmacology 16 (4): 317–323. https://doi.org/10.1046/j.1472-8206.2002.00076.x.
Georgsson, J., C. Skold, B. Plouffe, G. Lindeberg, M. Botros, M. Larhed, F. Nyberg, et al. 2005. Angiotensin II pseudopeptides containing 1,3,5-trisubstituted benzene scaffolds with high AT2 receptor affinity. Journal of Medicinal Chemistry 48 (21): 6620–6631. https://doi.org/10.1021/jm050280z.
Chandrasekaran, K., D.S. Karolina, S. Sepramaniam, A. Armugam, E.M. Wintour, J.F. Bertram, and K. Jeyaseelan. 2012. Role of microRNAs in kidney homeostasis and disease. Kidney International 81 (7): 617–627. https://doi.org/10.1038/ki.2011.448.
Plank, M.W., S. Maltby, H.L. Tay, J. Stewart, F. Eyers, P.M. Hansbro, and P.S. Foster. 2015. MicroRNA expression is altered in an ovalbumin-induced asthma model and targeting miR-155 with antagomirs reveals cellular specificity. PLoS One 10 (12): e0144810.
Cheng, Z., L.L. Dai, X. Wang, L.Q. Jia, X.G. Jing, P.F. Li, M. Liu, H. Wang, and L. An. 2017. MicroRNA-145 down-regulates mucin 5AC to alleviate airway remodeling and targets EGFR to inhibit cytokine expression. Oncotarget 8 (28): 46312–46325.
Han, H., and S.F. Ziegler. 2013. Bronchoalveolar lavage and lung tissue digestion. Bio Protoc 3 (16).
Tang, C., M.D. Inman, N. van Rooijen, P. Yang, H. Shen, K. Matsumoto, and P.M. O'Byrne. 2001. Th type 1-stimulating activity of lung macrophages inhibits Th2-mediated allergic airway inflammation by an IFN-gamma-dependent mechanism. Journal of Immunology 166 (3): 1471–1481.
Acknowledgments
The authors of this manuscript acknowledge the technical help provided by Mr. C.P. Pandey and Mr. A.L. Vishwakarma. UGC, New Delhi, supports A.J. and M.M., and CSIR, New Delhi, supports P.M. This manuscript has CSIR-CDRI Communication number: 10054.
Funding
This work was supported by the Council of Scientific and Industrial Research (CSIR) and CSIR-CDRI.
Author information
Authors and Affiliations
Contributions
A.J. performed major experiments and wrote the manuscript. M.M. performed staining and some in vivo experiments, P.M. helped in in vivo experiments, and M.K.B. conceptualized and supervised this study and manuscript writing.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 1767 kb)
Rights and permissions
About this article
Cite this article
Jaiswal, A., Maurya, M., Maurya, P. et al. Lin28B Regulates Angiotensin II-Mediated Let-7c/miR-99a MicroRNA Formation Consequently Affecting Macrophage Polarization and Allergic Inflammation. Inflammation 43, 1846–1861 (2020). https://doi.org/10.1007/s10753-020-01258-1
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-020-01258-1