Abstract
Background
Kidney dysfunction is a common complication in adults with Duchenne muscular dystrophy (DMD); however, little attention has been paid to kidney function in pediatric patients.
Methods
Medical records of patients with DMD who were followed up for ≥ 12 months were retrospectively reviewed. Inclusion criteria were (i) aged 5–18 years, (ii) proven mutations in the dystrophin gene, and (iii) absence of structural anomalies of the kidney and urinary tract. Serum creatine kinase (CK) was used as an indirect marker of muscle destruction.
Results
Forty-four patients (mean age, 10.9 ± 3.3 years) were included. Blood pressure was evaluated by 24-h ambulatory blood pressure monitoring in 28 patients. Hypertension was found in 9 (32.1%), eight of whom were using steroids. Mild proteinuria, hypercalciuria, hypocalciuria, and hyperphosphaturia in 24-h urine collection (n = 36) were detected in 3 (8.3%), 5 (13.9%), 7 (19.7%), and 6 (16.7%) patients, respectively. Twenty-one (58.3%) demonstrated hyperuricosuria, associated with hyperuricemia in 4. Logarithmic cystatin C (CysC) had a positive correlation to creatinine (Cr) (p = 0.001, r = 0.54), CK (p = 0.048, r = 0.30), and parathormone (PTH) (p = 0.001, r = 0.49). Moreover, the patients were divided into two groups according to median CysC value: group 1 (n = 20, CysC ≤ 0.76 mg/l) and group 2 (n = 24, CysC > 0.76 mg/l). Mean CK, PTH, and Cr levels were significantly elevated in group 2 compared with group 1 (p = 0.010, 0.033, and 0.023, respectively).
Conclusions
Long-term exposure to the excessive burden of intracellular components released from damaged muscles may be associated with an increased risk over time of chronic kidney impairment in pediatric DMD patients.

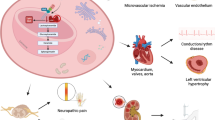
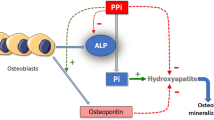
Graphical abstract

Similar content being viewed by others
References
Braat E, Hoste L, De Waele L, Gheysens O, Vermeersch P, Goffin K, Pottel H, Goemans N, Levtchenko E (2015) Renal function in children and adolescents with Duchenne muscular dystrophy. Neuromuscul Disord 25:381–387
Matsumura T, Saito T, Fujimura H, Sakoda S (2012) Renal dysfunction is a frequent complication in patients with advanced stage of Duchenne muscular dystrophy. Rinsho Shinkeigaku 52:211–217
Matsumura T, Saito T, Fujimura H, Shinno S, Sakoda S (2011) A longitudinal cause-of-death analysis of patients with Duchenne muscular dystrophy. Rinsho Shinkeigaku 51:743–750
Motoki T, Shimizu-Motohashi Y, Saito I, Komaki H, Ishiyama A, Aibara K, Jogamoto T, Tezuka Y, Kawabe M, Makino A, Nagatani K, Tatara K, Kuwabara K, Kikuchi C, Fukuda M, Ishii E, Eguchi M (2020) Renal dysfunction can occur in advanced-stage Duchenne muscular dystrophy. Muscle Nerve 61:192–197
Gauld LM, Kappers J, Carlin JB, Robertson CF (2004) Height prediction from ulna length. Dev Med Child Neurol 46:475–480
Polinsky MS, Kaiser BA, Baluarte HJ (1987) Urolithiasis in childhood. Pediatr Clin N Am 34:683–710
De Santo NG, Di Iorio B, Capasso G, Paduano C, Stamler R, Langman CB, Stamler J (1992) Population based data on urinary excretion of calcium, magnesium, oxalate, phosphate and uric acid in children from Cimitile (southern Italy). Pediatr Nephrol 6:149–157
Lurbe E, Agabiti-Rosei E, Cruickshank JK, Dominiczak A, Erdine S, Hirth A, Invitti C, Litwin M, Mancia G, Pall D, Rascher W, Redon J, Schaefer F, Seeman T, Sinha M, Stabouli S, Webb NJ, Wühl E, Zanchetti A (2016) 2016 European Society of Hypertension guidelines for the management of high blood pressure in children and adolescents. J Hypertens 34:1887–1920
Viollet L, Gailey S, Thornton DJ, Friedman NR, Flanigan KM, Mahan JD, Mendell JR (2009) Utility of cystatin C to monitor renal function in Duchenne muscular dystrophy. Muscle Nerve 40:438–442
Zaffanello M, Franchini M, Fanos V (2007) Is serum Cystatin-C a suitable marker of renal function in children? Ann Clin Lab Sci 37:233–240
Lappalainen H, Tiula E, Uotila L, Mänttäri M (2002) Elimination kinetics of myoglobin and creatine kinase in rhabdomyolysis: implications for follow-up. Crit Care Med 30:2212–2215
Rodríguez E, Soler MJ, Rap O, Barrios C, Orfila MA, Pascual J (2013) Risk factors for acute kidney injury in severe rhabdomyolysis. PLoS One 8:e82992
Bosch X, Poch E, Grau JM (2009) Rhabdomyolysis and acute kidney injury. N Engl J Med 361:62–72
Bertorini TE, Palmieri GM, Airozo D, Edwards NL, Fox IH (1981) Increased adenine nucleotide turnover in duchenne muscular dystrophy. Pediatr Res 15:1478–1482
Mallat SG, Al Kattar S, Tanios BY, Jurjus A (2016) Hyperuricemia, hypertension, and chronic kidney disease: an emerging association. Curr Hypertens Rep 18:74
Johnson RJ, Nakagawa T, Jalal D, Sánchez-Lozada LG, Kang DH, Ritz E (2013) Uric acid and chronic kidney disease: which is chasing which? Nephrol Dial Transplant 28:2221–2228
Ricotti V, Ridout DA, Scott E, Quinlivan R, Robb SA, Manzur AY, Muntoni F (2013) Long-term benefits and adverse effects of intermittent versus daily glucocorticoids in boys with Duchenne muscular dystrophy. J Neurol Neurosurg Psychiatry 84:698–705
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(PPTX 68 kb).
Rights and permissions
About this article
Cite this article
Kutluk, M.G., Doğan, Ç.S. Kidney involvement and associated risk factors in children with Duchenne muscular dystrophy. Pediatr Nephrol 35, 1953–1958 (2020). https://doi.org/10.1007/s00467-020-04587-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00467-020-04587-3