Abstract
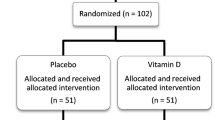
Current pharmacological approaches have failed to provide complete remission for patients with Attention-Deficit/Hyperactivity Disorder (ADHD). This study aimed to evaluate the efficacy and tolerability of resveratrol (that have been shown to have antioxidative, anti-inflammatory, and anti-apoptotic effects) as an adjunct to methylphenidate in pharmacologic treatment of ADHD. This 8-week, double-blinded, placebo-controlled trial randomized 66 participants to receive either 500 mg/day resveratrol or matched placebo in addition to methylphenidate. ADHD symptoms were evaluated in the patients using the Parent and Teacher versions of ADHD-Rating Scale (ADHD-RS) at three measurement points with time intervals of 4 weeks. Furthermore, the tolerability of the treatment strategies was systematically compared. Repeated measures analysis demonstrated a significant effect for time–treatment interaction on all three subscales of the Parent ADHD-RS during the trial period (total: p = 0.015; inattention: p = 0.032; hyperactivity/impulsivity: p = 0.036). Nevertheless, the effect for time–treatment interaction was not significant for the Teacher version of ADHD-RS (total: F = 0.81, df = 1.33, p = 0.401; inattention: F = 0.57, df = 1.37, p = 0.507; hyperactivity/impulsivity: F = 0.65, df = 1.34, p = 0.466). The frequencies of complications in the treatment groups were similar. Resveratrol administration for a duration of 8 weeks improved characteristic symptoms in patients with ADHD according to their parents. Further investigations containing larger sample sizes, longer supplementation periods, and dose–response evaluations are required to replicate these findings in ADHD children more confidently.



Similar content being viewed by others
References
Dehbozorghi S, Bagheri S, Moradi K, Shokraee K, Mohammadi MR, Akhondzadeh S (2019) Efficacy and safety of tipepidine as adjunctive therapy in children with attention-deficit/hyperactivity disorder: randomized, double-blind, placebo-controlled clinical trial. Psychiatry Clin Neurosci 73:690–696. https://doi.org/10.1111/pcn.12913
Rowland AS, Skipper BJ, Umbach DM, Rabiner DL, Campbell RA, Naftel AJ, Sandler DP (2015) The prevalence of ADHD in a population-based sample. J Atten Disord 19:741–754. https://doi.org/10.1177/1087054713513799
Castells X, Blanco-Silvente L, Cunill R (2018) Amphetamines for attention deficit hyperactivity disorder (ADHD) in adults. Cochrane Database Syst Rev 8:Cd007813. https://doi.org/10.1002/14651858.CD007813.pub3
Curatolo P, Paloscia C, D'Agati E, Moavero R, Pasini A (2009) The neurobiology of attention deficit/hyperactivity disorder. Eur J Paediatr Neurol 13:299–304. https://doi.org/10.1016/j.ejpn.2008.06.003
Sharma A, Couture J (2014) A review of the pathophysiology, etiology, and treatment of attention-deficit hyperactivity disorder (ADHD). Ann Pharmacother 48:209–225. https://doi.org/10.1177/1060028013510699
Steele M, Jensen PS, Quinn DM (2006) Remission versus response as the goal of therapy in ADHD: a new standard for the field? Clin Ther 28:1892–1908. https://doi.org/10.1016/j.clinthera.2006.11.006
Ghajar A, Aghajan-Nashtaei F, Afarideh M, Mohammadi MR, Akhondzadeh S (2018) l-Carnosine as adjunctive therapy in children and adolescents with attention-deficit/hyperactivity disorder: a randomized, double-blind, placebo-controlled clinical trial. J Child Adolesc Psychopharmacol 28:331–338. https://doi.org/10.1089/cap.2017.0157
Liu DY, Shen XM, Yuan FF, Guo OY, Zhong Y, Chen JG, Zhu LQ, Wu J (2015) The physiology of BDNF and its relationship with ADHD. Mol Neurobiol 52:1467–1476. https://doi.org/10.1007/s12035-014-8956-6
Lopresti AL (2015) Oxidative and nitrosative stress in ADHD: possible causes and the potential of antioxidant-targeted therapies. Atten Defic Hyperact Disord 7:237–247. https://doi.org/10.1007/s12402-015-0170-5
Ikonomidou C, Kaindl AM (2011) Neuronal death and oxidative stress in the developing brain. Antioxid Redox Signal 14:1535–1550. https://doi.org/10.1089/ars.2010.3581
Salehi B, Mishra AP, Nigam M, Sener B, Kilic M, Sharifi-Rad M, Fokou PVT, Martins N, Sharifi-Rad J (2018) Resveratrol: a double-edged sword in health benefits. Biomedicines 6:91. https://doi.org/10.3390/biomedicines6030091
Kanthasamy K, Gordon R, Jin H, Anantharam V, Ali S, Kanthasamy AG, Kanthasamy A (2011) Neuroprotective effect of resveratrol against methamphetamine-induced dopaminergic apoptotic cell death in a cell culture model of neurotoxicity. Curr Neuropharmacol 9:49–53. https://doi.org/10.2174/157015911795017353
Pacheco M, Frozza R, Bernardi A (2018) Anti-inflammatory effects of resveratrol: mechanistic insights. Int J Mol Sci 2018:19
Bastianetto S, Ménard C, Quirion R (2015) Neuroprotective action of resveratrol. Biochim Biophys Acta (BBA) Mol Basis Dis 1852:1195–1201. https://doi.org/10.1016/j.bbadis.2014.09.011
Pasinetti GM, Wang J, Ho L, Zhao W, Dubner L (2015) Roles of resveratrol and other grape-derived polyphenols in Alzheimer's disease prevention and treatment. Biochem Biophys Acta 1852:1202–1208. https://doi.org/10.1016/j.bbadis.2014.10.006
Rege SD, Kumar S, Wilson DN, Tamura L, Geetha T, Mathews ST, Huggins KW, Broderick TL, Babu JR (2013) Resveratrol protects the brain of obese mice from oxidative damage. Oxid Med Cell Longev 2013:419092. https://doi.org/10.1155/2013/419092
Pasinetti GM, Wang J, Ho L, Zhao W, Dubner L (2015) Roles of resveratrol and other grape-derived polyphenols in Alzheimer's disease prevention and treatment. Biochim Biophys Acta 1852:1202–1208. https://doi.org/10.1016/j.bbadis.2014.10.006
Moore A, Beidler J, Hong MY (2018) Resveratrol and depression in animal models: a systematic review of the biological mechanisms. Molecules. https://doi.org/10.3390/molecules23092197
Wightman EL, Haskell-Ramsay CF, Reay JL, Williamson G, Dew T, Zhang W, Kennedy DO (2015) The effects of chronic trans-resveratrol supplementation on aspects of cognitive function, mood, sleep, health and cerebral blood flow in healthy, young humans. Br J Nutr 114:1427–1437. https://doi.org/10.1017/s0007114515003037
Ge JF, Xu YY, Qin G, Cheng JQ, Chen FH (2016) Resveratrol ameliorates the anxiety- and depression-like behavior of subclinical hypothyroidism rat: possible involvement of the HPT axis, HPA axis, and Wnt/beta-catenin pathway. Front Endocrinol (Lausanne) 7:44. https://doi.org/10.3389/fendo.2016.00044
Ghanizadeh A, Mohammadi MR, Yazdanshenas A (2006) Psychometric properties of the Farsi translation of the kiddie schedule for affective disorders and schizophrenia-present and lifetime version. BMC Psychiatry 6:10. https://doi.org/10.1186/1471-244x-6-10
Akhondzadeh S, Mohammadi MR, Khademi M (2004) Zinc sulfate as an adjunct to methylphenidate for the treatment of attention deficit hyperactivity disorder in children: a double blind and randomized trial [ISRCTN64132371]. BMC Psychiatry 4:9. https://doi.org/10.1186/1471-244x-4-9
Farokhnia M, Shafiee Sabet M, Iranpour N, Gougol A, Yekehtaz H, Alimardani R, Farsad F, Kamalipour M, Akhondzadeh S (2014) Comparing the efficacy and safety of Crocus sativus L. with memantine in patients with moderate to severe Alzheimer's disease: a double-blind randomized clinical trial. Hum Psychopharmacol 29(4):351–359. https://doi.org/10.1002/hup.2412
Kashani L, Omidvar T, Farazmand B, Modabbernia A, Ramzanzadeh F, Tehraninejad ES, Ashrafi M, Tabrizi M, Akhondzadeh S (2013) Does pioglitazone improve depression through insulin-sensitization? Results of a randomized double-blind metformin-controlled trial in patients with polycystic ovarian syndrome and comorbid depression. Psychoneuroendocrinology 38(6):767–776. https://doi.org/10.1016/j.psyneuen.2012.08.010
Malek M, Ashraf-Ganjouei A, Moradi K, Bagheri S, Mohammadi M-R, Akhondzadeh S (2020) Prednisolone as adjunctive treatment to risperidone in children with regressive type of autism spectrum disorder: a randomized, placebo-controlled trial. Clin Neuropharmacol 43:39–45
Seidman LJ, Valera EM, Makris N (2005) Structural brain imaging of attention-deficit/hyperactivity disorder. Biol Psychiat 57:1263–1272
Castle L, Aubert RE, Verbrugge RR, Khalid M, Epstein RS (2007) Trends in medication treatment for ADHD. J Attent Disord 10:335–342
Huang Y-S, Tsai M-H (2011) Long-term outcomes with medications for attention-deficit hyperactivity disorder. CNS Drugs 25:539–554
Santosh PJ, Sattar S, Canagaratnam M (2011) Efficacy and tolerability of pharmacotherapies for attention-deficit hyperactivity disorder in adults. CNS Drugs 25:737–763
Palta P, Samuel LJ, Miller ER III, Szanton SL (2014) Depression and oxidative stress: results from a meta-analysis of observational studies. Psychosom Med 76:12
Brown NC, Andreazza AC, Young LT (2014) An updated meta-analysis of oxidative stress markers in bipolar disorder. Psychiatry Res 218:61–68
Joseph N, Zhang-James Y, Perl A, Faraone SV (2015) Oxidative stress and ADHD: a meta-analysis. J Attent Disord 19:915–924
Hawkey E, Nigg JT (2014) Omega-3 fatty acid and ADHD: Blood level analysis and meta-analytic extension of supplementation trials. Clin Psychol Rev 34:496–505
Frémont L (2000) Biological effects of resveratrol. Life Sci 66:663–673
Dasgupta B, Milbrandt J (2007) Resveratrol stimulates AMP kinase activity in neurons. Proc Natl Acad Sci 104:7217–7222
Chung S, Yao H, Caito S, Hwang J-w, Arunachalam G, Rahman I (2010) Regulation of SIRT1 in cellular functions: role of polyphenols. Arch Biochem Biophys 501:79–90
Pasinetti GM, Wang J, Ho L, Zhao W, Dubner L (2015) Roles of resveratrol and other grape-derived polyphenols in Alzheimer's disease prevention and treatment. Biochim Biophys Acta (BBA)-Mol Basis Dis 1852:1202–1208
Turner RS, Thomas RG, Craft S, van Dyck CH, Mintzer J, Reynolds BA, Brewer JB, Rissman RA, Raman R, Aisen PS (2015) A randomized, double-blind, placebo-controlled trial of resveratrol for Alzheimer disease. Neurology 85:1383–1391
Kou X, Chen N (2017) Resveratrol as a natural autophagy regulator for prevention and treatment of Alzheimer’s disease. Nutrients 9:927
Leal G, Afonso PM, Salazar IL, Duarte CB (2015) Regulation of hippocampal synaptic plasticity by BDNF. Brain Res 1621:82–101
Jain S, Banerjee BD, Ahmed RS, Arora VK, Mediratta PK (2013) Possible role of oxidative stress and brain derived neurotrophic factor in triazophos induced cognitive impairment in rats. Neurochem Res 38:2136–2147
Wang X, Xie Y, Zhang T, Bo S, Bai X, Liu H, Li T, Liu S, Zhou Y, Cong X (2016) Resveratrol reverses chronic restraint stress-induced depression-like behaviour: involvement of BDNF level, ERK phosphorylation and expression of Bcl-2 and Bax in rats. Brain Res Bull 125:134–143
Swanson JM, Flodman P, Kennedy J, Spence MA, Moyzis R, Schuck S, Murias M, Moriarity J, Barr C, Smith M (2000) Dopamine genes and ADHD. Neurosci Biobehav Rev 24:21–25
Avshalumov MV, Chen BT, Koós T, Tepper JM, Rice ME (2005) Endogenous hydrogen peroxide regulates the excitability of midbrain dopamine neurons via ATP-sensitive potassium channels. J Neurosci 25:4222–4231
Tsang AH, Chung KK (2009) Oxidative and nitrosative stress in Parkinson's disease. Biochim Biophysica Acta (BBA)-Mol Basis Dis 1792:643–650
Sankhwar ML, Yadav RS, Shukla RK, Singh D, Ansari RW, Pant AB, Parmar D, Khanna VK (2016) Monocrotophos induced oxidative stress and alterations in brain dopamine and serotonin receptors in young rats. Toxicol Ind Health 32:422–436
Acknowledgements
This study was the postgraduate thesis of Dr Maryam Rafeiy-Torghabeh under the supervision of Prof. Shahin Akhondzadeh for the Iranian Board of Psychiatry. This study was supported by a grant from Tehran University of Medical Sciences to Prof. Shahin Akhondzadeh (Grant no. 38897). The funding organization had no role in the design and conduct of the study; in the collection, analysis, and interpretation of the data; or in the preparation, review, or approval of the article and the decision to submit the article for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflict of interest to disclose.
Rights and permissions
About this article
Cite this article
Rafeiy-Torghabeh, M., Ashraf-Ganjouei, A., Moradi, K. et al. Resveratrol adjunct to methylphenidate improves symptoms of attention-deficit/hyperactivity disorder: a randomized, double-blinded, placebo-controlled clinical trial. Eur Child Adolesc Psychiatry 30, 799–807 (2021). https://doi.org/10.1007/s00787-020-01562-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00787-020-01562-z