Abstract
Background
We evaluated the diagnostic performance of HbA1c in diabetes and prediabetes and compared its efficiency in a model where HbA1c is used as a screening test.
Material and method
Records of 945 patients who had undergone simultaneous OGTT and HbA1c were evaluated. American Diabetes Association (ADA) criteria were used for diagnosis. Agreement between OGTT and HbA1c was evaluated. Using OGTT as the gold standard, the diagnostic performance of HbA1c was evaluated with ROC analysis and optimum cutoffs were determined. Then, the group was rearranged as if HbA1c was performed first as a screening test with new cutoffs and if OGTT was performed for diagnosis among suspected individuals.
Results
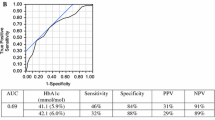
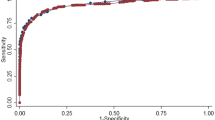
According to OGTT, 53 (5.6%) patients were diabetic and 247 were prediabetic; 18 of diabetics (34%) and 94 of prediabetics (38%) were diagnosed by HbA1c with present ADA cutoffs. The kappa coefficient for agreement between OGTT and HbA1c was 0.756 for diabetes and 0.336 for prediabetes. In ROC analysis, optimal HbA1c cutoff points were 38 mmol/mol (AUC 0.953) for diabetes and 35.5 mmol/mol (AUC 0.673) for prediabetes. In a new model after initial screening with HbA1c, 398 patients with HbA1c > 35.5 mmol/mol were taken for further OGTT. Fifty-three of diabetics (100%) and 199 of prediabetics (81%) were diagnosed. Prediabetic 48 patients (19%) were missed.
Conclusion
HbA1c showed poor performance in diagnosis of diabetes and prediabetes. Instead, using HbA1c as a screening test with well-defined cutoff may offer practical and economical advantages greatly reducing the number of OGTTs required.




Similar content being viewed by others
References
International ExpertCommittee. International Expert Committee report on the role of the A1C assay in thediagnosis of diabetes. Diabetes Care. 2009;32:1327–34. https://doi.org/10.2337/dc09-9033.
American Diabetes Association. Standards of medical care in diabetes-2010. Diabetes Care. 2010;33(Suppl 1):S11–61. https://doi.org/10.2337/dc10-S011.
American Diabetes Association. 2. Classification and diagnosis of diabetes: standards of medical care in diabetes-2018. DiabetesCare. 2018;41(suppl.1):s13–27. https://doi.org/10.2337/dc18-S002.
Monnier L, Colette C. Postprandial and basal hyperglycaemia in type 2 diabetes: contributions to overall glucose exposure and diabetic complications. Diabetes Metab. 2015;41(6 Suppl 1):6S9–15. https://doi.org/10.1016/S1262-3636(16)30003-9.
Yang L, Shen X, Yan S, Xu F, Wu P. The effectiveness of age on HbA1c as a criterion for the diagnosis of diabetes in Chinese different age subjects. Clin Endocrinol. 2015;82(2):205–12. https://doi.org/10.1111/cen.12494.
Chan CL, Pyle L, Newnes L, Nadeau KJ, Zeitler PS, Kelsey MM. Continuous glucose monitoring and its relationship to hemoglobin A1c and oral glucose tolerance testing in obese and prediabetic youth. J Clin Endocrinol Metab. 2015;100(3):902–10. https://doi.org/10.1210/jc.2014-3612.
Libman IM, Barinas-Mitchell E, Bartucci A, Robertson R, Arslanian S. Reproducibility of the oral glucose tolerance test in overweight children. J Clin Endocrinol Metab. 2008;93(11):4231–7. https://doi.org/10.1210/jc.2008-0801.
Gillett MJ. International Expert Committee report on the role of the A1c assay in the diagnosis of diabetes. Diabetes Care. 2009;32:1327–34.
Van’tRiet E, Alssema M, Rijkelijkhuizen JM, Kostense PJ, Nijpels G, et al. The relationship between HbA1c and glucose levels in the general Dutch population: the new Hoorn study. Diabetes Care. 2010;33(1):61–6. https://doi.org/10.2337/dc09-0677.
Rohlfing CL, Little RR, Wiedmeyer HM, England JD, Madsen R, et al. Use of GHb (HbA1c) in screening for undiagnosed diabetes in the U.S. population. Diabetes Care. 2000 Feb;23(2):187–91. https://doi.org/10.2337/diacare.23.2.187.
Bao Y, Ma X, Li H, Zhou M, Hu C, et al. Glycated haemoglobin A1c for diagnosing diabetes in Chinese population: crosssectional epidemiological survey. BMJ. 2010;340:c2249. https://doi.org/10.1136/bmj.c2249.
Burtis CA, Ashwood ER, Burns DE. Tietz fundementals of clinical chemistry. 6th ed. St. Louis: Elsevier Saunders; 2008. p. 384.
Cowie CC, Rust KF, Byrd-Holt DD, et al. Prevalence of diabetesandhigh risk fordiabetesusing A1C criteria in the U.S. population in 1988–2006. DiabetesCare. 2010;33:562–8. https://doi.org/10.2337/dc09-1524.
Bennett CM, Guo M, Dharmage SC. HbA(1c) as a screeningtoolfordetection of type 2 diabetes: a systematicreview. DiabetMed. 2007;24:333–43. https://doi.org/10.1111/j.1464-5491.2007.02106.
Herman WH, Cohen RM. Racial and ethnic differences in the relationship between HbA1c and blood glucose: implications for the diagnosis of diabetes. J Clin Endocrinol Metab. 2012;97:1067–72. https://doi.org/10.1210/jc.2011-1894.
Colagiuri S, Hussain Z, Zimmet P, Cameron A, Shaw J. Screening for type 2 diabetes and impaired glucose metabolism: the Australian experience. Diabetes Care. 2004;27:367–71. https://doi.org/10.2337/diacare.27.2.367.
Giniş Z, Öztürk G, Sırmalı R, Yalçındağ A, Dülderoğlu Y, et al. The role of HbA1c as a screening and diagnostic test for diabetes mellitus in Ankara. Turk J MedSci. 2012;42(Sup.2):1430–6.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors declare that they have no conflict of interest.
Research involving human participants
Since this is a retrospective data analysis without using individual patient characteristic, a particular consent could not be obtained for the study. But permission was taken from our ethical committee and number was given.
Statement on consent for participation
The study was approved by the Ethics Review Committee of the Dr Lütfi KırdarKartal Research and Training Hospital (permission number and date: 2018/514/130/6 29.05.18).
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hürmeydan, Ö., Madenci, Ö.Ç., Yildiz, Z. et al. Diagnostic performance of HbA1c for detecting prediabetes and diabetes in Turkish adults. Int J Diabetes Dev Ctries 40, 585–590 (2020). https://doi.org/10.1007/s13410-020-00807-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13410-020-00807-6