Abstract
Background
Each stroke subtype is associated with specific risk factors, and stroke prevention depends solely on the control of the underlying risk factors for each stroke subtype. Obstructive sleep apnea has been established as a major risk factor for stroke and cardiovascular disease. However, information on the stroke subtype linked to obstructive sleep apnea is scarce.
Methods
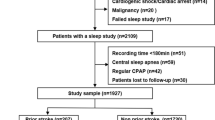
This was a single-center, observational case series study conducted on patients who were admitted with acute ischemic stroke to King Khalid University Hospital. The TOAST criteria were used to determine the stroke subtype in each of these patients. The Berlin questionnaire was utilized to assess the presence of obstructive sleep apnea. The proportion of each stroke subtype was then calculated and compared between the group with associated obstructive sleep apnea and the group without associated obstructive sleep apnea.
Results
A total of 170 consecutive patients with acute ischemic stroke were admitted between January 2018 and September 2018. Eighty-seven (51%) patients were found to have obstructive sleep apnea. The proportion of small artery disease was significantly greater in the obstructive sleep apnea group (44% vs. 26%, P = 0.02). There was no difference in the distribution of the other stroke subtypes between the two groups. Univariate analysis revealed that small artery disease was associated with body mass index, hypertension, and obstructive sleep apnea. However, in a multivariate logistic analysis, only hypertension was found to be independently associated with small artery disease.
Conclusion
Small artery disease is the most common stroke subtype associated with obstructive sleep apnea. Clinicians must vigilantly assess the presence of obstructive sleep apnea in ischemic stroke patients, especially in patients whose stroke is attributed to small artery disease.

Similar content being viewed by others
References
Albers GW, Marks MP, Kemp S, Christensen S, Tsai JP, Ortega-Gutierrez S, McTaggart R, Torbey MT, Kim-Tenser M, Leslie-Mazwi T, Sarraj A, Kasner SE, Ansari SA, Yeatts SD, Hamilton S, Mlynash M, Heit JJ, Zaharchuk G, Kim S, Carrozzella J, Palesch YY, Demchuk AM, Bammer R, Lavori PW, Broderick JP, Lansberg MG, DEFUSE 3 Investigators (2018) Thrombectomy for stroke at 6 to 16 hours with selection by perfusion imaging. N Engl J Med 378(8):708–718
Nogueira RG, Jadhay AP, Haussen DC, Bonafe A et al (2018) Thrombectomy 6 to 24 hours after stroke with a mismatch between deficit and infarct. N Engl J Med 378(1):11–21
Hacke W, Kaste M, Bluhmki E, Brozman M, Dávalos A, Guidetti D, Larrue V, Lees KR, Medeghri Z, Machnig T, Schneider D, von Kummer R, Wahlgren N, Toni D (2008) Thrombolysis with alteplase 3 to 4.5 hours after acute ischemic stroke. N Engl J Med 359:1317–1329
Goyal M, Menon BK, van Zwam WH, Dippel DW et al (2016) Endovascular thrombectomy after large-vessel ischemic stroke: a meta-analysis of individual patient data from five randomized trials. Lancet. 387:1723–1731
Rothwell PM, Coull AJ, Silver LE, Fairhead JF, Giles MF, Lovelock CE, Redgrave JNE, Bull LM, Welch SJV, Cuthbertson FC, Binney LE, Gutnikov SA, Anslow P, Banning AP, Mant D, Mehta Z (2005) Population-based study of event-rate, incidence, case fatality, and mortality for all acute vascular events in all arterial territories (Oxford vascular study). Lancet. 366:1773–1783
Johnston SC, Mendis S, Mathers CD (2009) Global variation in stroke burden and mortality: estimates from monitoring, surveillance, and modeling. Lancet Neurol 8:345–354
Bamford J, Sandercock P, Dennis M, Burn J, Warlow C (1991) Classification and natural history of clinical subtypes of cerebral infarction. Lancet. 337:1521–1526
Kernan WN, Ovbiagele B, Black HR, Bravata DM, Chimowitz MI, Ezekowitz MD, Fang MC, Fisher M, Furie KL, Heck DV, Johnston SC, Kasner SE, Kittner SJ, Mitchell PH, Rich MW, Richardson D, Schwamm LH, Wilson JA, American Heart Association Stroke Council, Council on Cardiovascular and Stroke Nursing, Council on Clinical Cardiology, and Council on Peripheral Vascular Disease (2014 Jul) Guidelines for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 45(7):2160–2236
Peppard PE, Young T, Barnet JH, Palta M, Hagen EW, Hla KM (2013) Increased prevalence of sleep-disordered breathing in adults. Am J Epidemiol 177(9):1006–1014. https://doi.org/10.1093/aje/kws342
Dong R, Dong Z, Liu H, Shi F, Du J (2018 Jun) Prevalence, risk factors, outcomes, and treatment of obstructive sleep apnea in patients with cerebrovascular disease: a systematic review. J Stroke Cerebrovasc Dis 27(6):1471–1480. https://doi.org/10.1016/j.jstrokecerebrovasdis.2017.12.048
Johnson KG, Johnson DC (2010) Frequency of sleep apnea in stroke and TIA patients: a meta-analysis. J Clin Sleep Med 6:131–137
Durgan DJ, Bryan RM Jr (2012 Aug) Cerebrovascular consequences of obstructive sleep apnea. J Am Heart Assoc 1(4):e000091
Igelstrom H, Asenlof P, Emtner M, Lindberg E (2018 Sep) Improvement in obstructive sleep apnea after a tailored behavioral sleep medicine intervention targeting healthy eating and physical activity: a randomized controlled trial. Sleep Breath 22(3):653–661
Peppard PE, Young T, Palta M, Dempsey J, Skatrud J (2000) Longitudinal study of moderate weight change and sleep-disordered breathing. JAMA. 284(23):3015–3021
Giles TL, Lasserson TJ, Smith BH, White J et al (2006) Continuous positive airways pressure for obstructive sleep apnoea adults. Cochrane Database Syst Rev 3:CD001106
Marin JM, Carrizo SJ, Vicente E, Agusti G (2005) Long-term cardiovascular outcomes in men with obstructive sleep apnoea-hypopnoea with or without treatment with continuous positive airway pressure: an observational study. Lancet 365(9464):1046–1053
Poli M, Philip P, Taillard J, Debruxelles S, Renou P, Orgogozo JM, Rouanet F, Sibon I (2017) Atrial fibrillation is a major cause of stroke in apneic patients: a prospective study. Sleep Med 30:251–254. https://doi.org/10.1016/j.sleep.2015.07.031
Lipford MC, Flemming, Calvin AD, Mandrekar J, Brown RD, Somers VK, Caples SM (2015) Associations between cardioembolic stroke and obstructive sleep apnea. Sleep. 38(11):1699–1705
Berlin questionnaire (2000) Sleep Breath 4(2):99. https://doi.org/10.1007/BF03045031
Netzer NC, Stoohs RA, Netzer CM, Clark K et al (1999) Using the Berlin questionnaire to identify patients at risk for the sleep apnea syndrome. Ann Intern Med 31(7):485–491
Andrechuk CRS, Netzer N, Zancanella E, Almeida AR, Ceolim MF (2019) Cultural adaptation and evaluation of the measurement properties of the Berlin questionnaire for Brazil. Sleep Med 60:182–187. https://doi.org/10.1016/j.sleep.2019.03.022
Senaratna CV, Perret JL, Matheson MC, Lodge CJ, Lowe AJ, Cassim R, Russell MA, Burgess JA, Hamilton GS, Dharmage SC (2017) Validity of the Berlin questionnaire in detecting obstructive sleep apnea: a systematic review and meta-analysis. Sleep Med Rev 36:116–124. https://doi.org/10.1016/j.smrv.2017.04.001
Adams HP Jr, Bendixen BH, Kappelle LJ, Biller J, Love BB, Gordon DL, Marsh EE III (1993) Classification of subtype of acute ischemic stroke. Definitions for use in a multicenter clinical trial. TOAST. Trial of org 10172 in acute stroke treatment. Stroke 24(1):35–41
Fure B, Wyller TB, Thommessen B (2005 Oct) TOAST criteria applied in acute ischemic stroke. Acta Neurol Scand 112(4):254–258
Kolominsky-Rabas PL, Weber M, Gefeller O, Neundoerfer B, Heuschmann PU (2001) Epidemiology of ischemic stroke subtypes according to TOAST criteria. Stroke. 32:2735–2740
Petty GW, Brown RD, Whisnant JP, Sicks JD, O’Fallon WM, Wiebers DO (1999) Ischemic stroke subtypes: a population-based study of incidence and risk factors. Stroke. 30:2513–2516
Bejot Y, Caillier M, Ben Salem D, Couvreur G, Rouaud O, Osseby GV, Durier J, Marie C, Moreau TM (2008 Dec) Ischemic stroke subtypes and associated risk factors: a French population based study. J Neurol Neurosurg Psychiatry 79(12):1344–1348
Zafar A, Al-Khamis FA, Al-Bakr AI, Alsulaiman AA, Msmar AH (2016 Jul) Risk factors and subtypes of acute ischemic stroke: a study at king Fahd hospital of the university. Neurosciences. 21(3):246–251
Pantoni L (2010 Jul) Cerebral small vessel disease: from pathogenesis and clinical characteristics to therapeutic challenges. Lancet Neurol 9(7):689–701
Cuadrado-Godia E, Dwivedi P, Sharma S, Ois Santiago A, Roquer Gonzalez J, Balcells M, Laird J, Turk M, Suri HS, Nicolaides A, Saba L, Khanna NN, Suri JS (2018) Cerebral small vessel disease: a review focusing on pathophysiology, biomarkers, and machine learning strategy. J Stroke 20(3):302–320
Park H, Jo J, Cheong J, Chang H, Lee H, Lee S, Suk S (2014) Prevalence and risk factors of cerebral white matter changes and silent infarcts on brain computed tomography scans among community-dwelling healthy adults: the present project. Neurology Asia 19(4):351–356
Goldstein LB, Bushnell CD, Adams RJ, Appel LJ (2011) Guidelines for the primary prevention of stroke: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 42(2):517–584
Marin JM, Agusti A, Villar I, Forner M, Nieto D, Carrizo SJ, Barbe F, Vicente E, Wei Y, Nieto FJ, Jelic S (2012) Association between treated and untreated obstructive sleep apnea and risk of hypertension. JAMA. 307(20):2169–2176
Walia HK, Li H, Rueschman M, Bhatt DL, Patel SR, Quan SF, Gottlieb DJ, Punjabi NM, Redline S, Mehra R (2014 Aug 15) Association of severe obstructive sleep apnea and elevated blood pressure despite antihypertensive medication use. J Clin Sleep Med 10(8):835–843
Ip MS, Tse HF, Lam B, Tsang KW, Lam WK (2004) Endothelial function in obstructive sleep apnea and response to treatment. Am J Respir Crit Care Med 169(3):348–353
Nieto FJ, Herrington DM, Redline S, Benjamin EJ, Robbins JA (2004) Sleep apnea and markers of vascular endothelial function in a large community sample of older adults. Am J Respir Crit Care Med 169(3):354–360
Davignon J, Ganz P (2004) Role of endothelial dysfunction in atherosclerosis. Circulation. 109(23 Suppl 1):III27–III32
Budhiraja R, Parthasarathy S, Quan SF (2007) Endothelial dysfunction in obstructive sleep apnea. J Clin Sleep Med 3(4):409–415
Kushida CA, Littner MR, Morgenthaler T, Alessi CA, Bailey D, Coleman J Jr, Friedman L, Hirshkowitz M, Kapen S, Kramer M, Lee-Chiong T, Loube DL, Owens J, Pancer JP, Wise M (2005 Apr) Practice parameters for the indications for polysomnography and related procedures: an update for 2005. Sleep. 28(4):499–521
Wolf ME, Sauer T, Alonso A, Hennerici MG (2012) Comparison of the new ASCO classification with the TOAST classification in a population with acute ischemic stroke. J Neurol 259(7):1284–1289
Deacon NL, Jen R, Li Y, Malhotra A (2016) Treatment of obstructive sleep apnea. Prospects for personalized combined modality therapy. Ann Am Thorac Soc 13(1):101–108
Funding
The authors extend their appreciation to the Deanship of Scientific Research at King Saud University for funding this work through research group no. (RGP-1438-008).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
Approval was obtained from the ethics committee of King Khalid University Hospital. The procedures used in this study adhere to the tenets of the Declaration of Helsinki.
Consent to participate
Verbal informed consent was obtained prior to the interview.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Al-Hussain, F., Mohammad, Y. Lacune is the stroke subtype linked to obstructive sleep apnea. Neurol Sci 41, 3301–3306 (2020). https://doi.org/10.1007/s10072-020-04437-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-020-04437-y