Abstract
Background
Older adults with type 2 diabetes mellitus (DM) have high incidence of falls. The aim of this study was to compare sensorimotor functions, balance, mobility, fear of falling, and fall history in older people with DM (with and without neuropathy) and non-diabetic healthy controls.
Methods
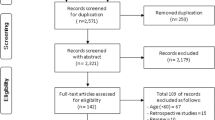
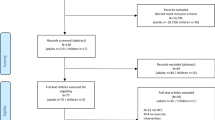
We enrolled 153 participants aged 50–70 years: 51 people with diabetic peripheral neuropathy (D-PN), 52 with diabetes without neuropathy (D-noPN), and 50 healthy controls (HC). Participants completed a fear of falling assessment and detailed test battery comprising sensorimotor functions, lower limb strength, contrast vision, reaction time, balance, and mobility from which a composite physiological fall risk score (PFRS) was derived. In addition, a fall history of the past 3 months was recorded.
Results
Post hoc comparisons of ANOVA test revealed the D-PN had significant deficits than the other two groups in tests of lower limb sensation, knee extension strength, reaction time, postural sway, one leg standing, sit-to-stand and the timed up and go test. The D-PN had the highest fear of falling (30.18 ± 6.75) and the highest PFRS (1.68 ± 1.13). PFRS for the D-noPN (0.74 ± 0.80) was intermediate between HC (0.49 ± 0.96) and DP-N groups. Thirty-four D-PN participants (66.7%), 19 D-noPN participants (36.5%), and 7 HC (14.0%) reported one or more falls in the past 3 months (Chi2 test for trend = 28.1, df = 2, p < 0.001).
Conclusions
Older people with diabetic neuropathy have impaired sensorimotor function, balance, mobility, and associated increased fear of falling and fall rates. This population may benefit from fall risk assessments involving the above measures, and subsequent interventions targeted to deficits amenable to correction.

Similar content being viewed by others
References
World Health Organization. Diabetes fact sheet. 2019. https://www.who.int/news-room/fact-sheets/detail/diabetes. Accessed 15 May 2019.
Sánchez Martínez M, Blanco A, Castell MV, Gutiérrez Misis A, González Montalvo JI, Zunzunegui MV, et al. Diabetes in older people: prevalence, incidence and its association with medium- and long-term mortality from all causes. Aten Primaria. 2014;46(7):376–84.
International Diabetes Federation, Diabetes atlas: the global burden. 5th ed. 2011. https://www.idf.org/e-library/epidemiology-research/diabetes-atlas/20-atlas-5th-edition.html. Accessed 11 May 2019.
Katulanda P, Sheriff MH, Matthews DR. The diabetes epidemic in Sri Lanka - a growing problem. Ceylon Med J. 2006;51(1):26–8.
Wijewardene K, Mohideen MR, Mendis S, Fernando DS, Kulathilaka T, Weerasekara D, et al. Prevalence of hypertension, diabetes and obesity: baseline findings of a population based survey in four provinces in Sri Lanka. Ceylon Med J. 2005;50(2):62–70.
Katulanda P, Constantine GR, Mahesh JG, Sheriff R, Seneviratne RD, Wijeratne S, et al. Prevalence and projections of diabetes and pre-diabetes in adults in Sri Lanka--Sri Lanka Diabetes, Cardiovascular Study (SLDCS). Diabet Med. 2008;25(9):1062–9.
Deli G, Bosnyak E, Pusch G, Komoly S, Feher G. Diabetic neuropathies: diagnosis and management. Neuroendocrinology. 2013;98(4):267–80.
Tesfaye S, Selvarajah D. Advances in the epidemiology, pathogenesis and management of diabetic peripheral neuropathy. Diabetes Metab Res Rev. 2012;28(Suppl 1):8–14.
Kaur S, Pandhi P, Dutta P. Painful diabetic neuropathy: an update. Ann Neurosci. 2011;18(4):168–75.
Katulanda P, Ranasinghe P, Jayawardena R, Constantine GR, Sheriff MH, Matthews DR. The prevalence, patterns and predictors of diabetic peripheral neuropathy in a developing country. Diabetol Metab Syndr. 2012;4(1):21.
Ites KI, Anderson EJ, Cahill ML, Kearney JA, Post EC, Gilchrist LS. Balance interventions for diabetic peripheral neuropathy: a systematic review. J Geriatr Phys Ther. 2011;34(3):109–16.
Richardson JK, Ching C, Hurvitz EA. The relationship between electromyographically documented peripheral neuropathy and falls. J Am Geriatr Soc. 1992;40(10):1008–12.
Richardson JK, Hurvitz EA. Peripheral neuropathy: a true risk factor for falls. J Gerontol A Biol Sci Med Sci. 1995;50(4):M211–5.
Dingwell JB, Ulbrecht JS, Boch J, Becker MB, O’Gorman JT, Cavanagh PR. Neuropathic gait shows only trends towards increased variability of sagittal plane kinematics during treadmill locomotion. Gait Posture. 1999;10(1):21–9.
Bokan-Mirković V, Škarić-Karanikić Ž, Nejkov S, Vuković M, Ćirović D. Diabetic polyneuropathy and risk of falls: fear of falling and other factors. Acta Clin Croat. 2017;56(4):721–7.
Macgilchrist C, Paul L, Ellis BM, Howe TE, Kennon B, Godwin J. Lower-limb risk factors for falls in people with diabetes mellitus. Diabet Med. 2010;27(2):162–8.
Dixit S, Maiya A, Shasthry BA, Kumaran DS, Guddattu V. Postural sway in diabetic peripheral neuropathy among Indian elderly. Indian J Med Res. 2015;142(6):713–20.
Mustapa A, Justine M, Mustafah NM, Jamil N, Manaf H. Postural control and gait performance in the diabetic peripheral neuropathy: a systematic review. Biomed Res Int. 2016;14.
Alvarenga PP, Pereira DS, Anjos DM. Functional mobility and executive function in elderly diabetics and non-diabetics. Rev Bras Fisioter. 2010;14(6):491–6.
Henderson EJ, Lord SR, Bordie MA, Gaut DM, Lawrence AD, Close TCT, et al. Rivastigmine for gait stability in patients with Parkinson's disease (ReSPonD): a randomised, double-blind, placebo-controlled, phase 2 trial. Lancet Neurol. 2016;15(3):249–58.
Mythili A, Kumar KD, Subrahmanyam KA, Venkateswarlu K, Butchi RG. A comparative study of examination scores and quantitative sensory testing in diagnosis of diabetic polyneuropathy. Int J Diabetes Dev Ctries. 2010;30(1):43–8.
Lord SR, Menz HB, Tiedemann A. A physiological profile approach to falls risk assessment and prevention. Phys Ther. 2003;83(3):237–52.
Makizako H, Shimada H, Doi T, Tsutsumimoto K, Nakakubo S, Hotta R, et al. Predictive cutoff values of the five-times sit-to-stand test and the timed "up & go" test for disability incidence in older people dwelling in the community. Phys Ther. 2017;97(4):417–24.
Allet L, Kim H, Ashton-Miller J, De Mott T, Richardson JK. Frontal plane hip and ankle sensorimotor function, not age, predicts unipedal stance time. Muscle Nerve. 2012;45(4):578–85.
Barry E, Galvin R, Keogh C, Horgan F, Fahey T. Is the timed up and go test a useful predictor of risk of falls in community dwelling older adults: a systematic review and meta-analysis. BMC Geriatr. 2014;14:14.
Lord SR, Ward JA. Age-associated differences in sensori-motor function and balance in community dwelling women. Age Ageing. 1994;23(6):452–60.
Lamb SE, Jørstad-Stein EC, Hauer K, Becker C. Development of a common outcome data set for fall injury prevention trials: the Prevention of Falls Network Europe consensus. J Am Geriatr Soc. 2005;53(9):1618–22.
Toosizadeh N, Mohler J, Armstrong DG, Talal TK, Najafi B. The influence of diabetic peripheral neuropathy on local postural muscle and central sensory feedback balance control. PLoS One. 2015;10(8):e0135255.
Kars HJ, Hijmans JM, Geertzen JH, Zijlstra W. The effect of reduced somatosensation on standing balance: a systematic review. J Diabetes Sci Technol. 2009;3(4):931–43.
Lafond D, Corriveau H, Prince F. Postural control mechanisms during quiet standing in patients with diabetic sensory neuropathy. Diabetes Care. 2004;27(1):173–8.
Kim TN, Park MS, Yang SJ, Yoo HJ, Kang HJ, Song W, et al. Prevalence and determinant factors of sarcopenia in patients with type 2 diabetes. The Korean Sarcopenic Obesity Study (KSOS). 2010;33(7):1497–9.
Wang T, Feng X, Zhou J, Gong H, Xia S, Wei Q, et al. Type 2 diabetes mellitus is associated with increased risks of sarcopenia and pre-sarcopenia in Chinese elderly. Sci Rep. 2016;6:38937.
Park SW, Goodpaster BH, Strotmeyer ES, de Rekeneire N, Harris TB, Schwartz AV, et al. Decreased muscle strength and quality in older adults with type 2 diabetes: the health, aging, and body composition study. Diabetes. 2006;55(6):1813–8.
Vaz MM, Costa GC, Reis JG, Junior WM, Albuquerque de Paula FJ, Abreu DC. Postural control and functional strength in patients with type 2 diabetes mellitus with and without peripheral neuropathy. Arch Phys Med Rehabil. 2013;94(12):2465–70.
Uccioli L, Giacomini PG, Monticone G, Magrini A, Durola L, Bruno E, et al. Body sway in diabetic neuropathy. Diabetes Care. 1995;18(3):339–44.
Boucher P, Teasdale N, Courtemanche R, Bard C, Fleury M. Postural stability in diabetic polyneuropathy. Diabetes Care. 1995;18(5):638–45.
Turcot K, Allet L, Golay A, Hoffmeyer P, Armand S. Postural strategies in diabetes patients with peripheral neuropathy determined using cross-correlation functions. Diabetes Technol Ther. 2012;14(5):403–10.
Turcot K, Allet L, Golay A, Hoffmeyer P, Armand S. Investigation of standing balance in diabetic patients with and without peripheral neuropathy using accelerometers. Clin Biomech (Bristol, Avon). 2009;24(9):716–21.
Chau RM, Ng TK, Kwan RL, Choi CH, Cheing GL. Risk of fall for people with diabetes. Disabil Rehabil. 2013;35(23):1975–80.
Kwan MM, Lin SI, Chen CH, Close JC, Lord SR. Sensorimotor function, balance abilities and pain influence timed up and go performance in older community-living people. Aging Clin Exp Res. 2011;23(3):196–201.
DeMott TK, Richardson JK, Thies SB, Ashton-Miller JA. Falls and gait characteristics among older persons with peripheral neuropathy. Am J Phys Med Rehabil. 2007;86(2):125–32.
Lord SR, Delbaere K, Gandevia SC. Use of a physiological profile to document motor impairment in ageing and in clinical groups. J Physiol. 2016;594(16):4513–23.
Thanthrige RS, Dassanayake S, Dissanayake D. Relationship between increased risk of falling and cognitive impairment in residents of an elderly home in the Colombo district. Ceylon Med J. 2014;59(1):21–3.
Acknowledgments
We wish to thank the management of National Hospital Colombo, Sri Lanka, and Faculty of Medicine, University of Colombo, Sri Lanka, for ethics approval and facilities provided for this study to make this research successful.
Author contributors
All authors contributed equally in conceptualization of the study. Data collection was conducted by AHW under direct guidance and supervision of PK and DWND. AHW was trained for the methods of the study by PK, DWND, and SL. AHW prepared the manuscript under the guidance of DWND and SL. SL and DWND edited the manuscript. LA and PK contributed to the manuscript by editing and reviewing the manuscript. Final manuscript was reviewed and approved by all the authors for submission.
Funding
This work was supported by the Postgraduate research Scholarship (AP/3/2/2016/PG/05), University of Colombo, Sri Lanka.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
This study was approved by the Ethical Review Committee of the Faculty of Medicine, University of Colombo (EC-15-166) and the National Hospital of Sri Lanka, Research Ethics Committee (ETH/COM/2016). All participants signed informed consent prior to their participation.
Conflict of interest
The PPA (NeuRA FallScreen) is commercially available through Neuroscience Research Australia.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Wettasinghe, A.H., Dissanayake, D.W.N., Allet, L. et al. Sensorimotor impairments, postural instability, and risk of falling in older adults with diabetic peripheral neuropathy. Int J Diabetes Dev Ctries 40, 547–554 (2020). https://doi.org/10.1007/s13410-020-00827-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13410-020-00827-2