Abstract
Background and Purpose
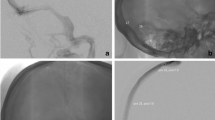
The aim of this study was to assess the safety and effectiveness of lateral sinus stenosis (LSS) stenting in patients with idiopathic intracranial hypertension (IIH) who are refractory to medical treatment, particularly focusing on visual outcomes including papilledema.
Material and Methods
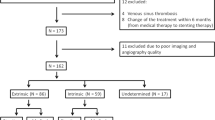
Retrospective study of consecutive patients with IIH refractory to medical treatment who underwent LSS stenting. Clinical features, visual fields and optical coherence tomography (OCT) retinal nerve fiber layer (RNFL) and ganglion cell layer (GCL) thicknesses were assessed before stenting, at 1 month poststenting and at last follow-up. Complications were also recorded.
Results
A total of 16 women were included, with a mean age of 39 ± 11 years. All patients had papilledema while 15/16 (94%) had headaches. Mean visual acuity was 0.036 logMAR, range (+0.4 to +0.0 logMAR). The mean RNFL thickness prior to stenting was 121.7 µm (±34.7 µm) and mean GCL thickness was 80.2 µm (±8.9 µm). Mean follow-up was 19.7 months (±11.8 months). After stenting, acetazolamide was discontinued in 15/16 (94%) patients. Papilledema improved in 14/16 (88%) of patients. The mean RNFL thickness was significantly decreased 1 month after stenting (96.3 ± 15.6 µm; p < 0.001) and at last visit (93.4 ± 15.3 µm; p < 0.001). The GCL thickness after LSS stenting was moderately decreased at the last visit examination: 80.2 ± 8.9 µm vs. 78.0 ± 10.7 µm; (p < 0.01). No stent-related complication occurred, while there was one case of restenosis.
Conclusion
Improvement of papilledema appears to occur relatively rapidly after the LSS stenting. The results further support the role of LSS stenting in the treatment of IIH, especially with respect to visual symptoms.


Similar content being viewed by others
References
Raoof N, Sharrack B, Pepper IM, Hickman SJ. The incidence and prevalence of idiopathic intracranial hypertension in Sheffield, UK. Eur J Neurol. 2011;18:1266–8.
Farb RI, Vanek I, Scott JN, Mikulis DJ, Willinsky RA, Tomlinson G, terBrugge KG. Idiopathic intracranial hypertension: the prevalence and morphology of sinovenous stenosis. Neurology. 2003;60:1418–24.
Lenck S, Radovanovic I, Nicholson P, Hodaie M, Krings T, Mendes-Pereira V. Idiopathic intracranial hypertension: the veno glymphatic connections. Neurology. 2018;91:515–22.
Digre KB, Bruce BB, McDermott MP, Galetta KM, Balcer LJ, Wall M; NORDIC Idiopathic Intracranial Hypertension Study Group. Quality of life in idiopathic intracranial hypertension at diagnosis. Neurology. 2015;84:2449–56.
Mulla Y, Markey KA, Woolley RL, Patel S, Mollan SP, Sinclair AJ. Headache determines quality of life in idiopathic intracranial hypertension. J Headache Pain. 2015;16:521.
OCT Sub-Study Committee for NORDIC Idiopathic Intracranial Hypertension Study Group, Auinger P, Durbin M, Feldon S, Garvin M, Kardon R, Keltner J, Kupersmith MJ, Sibony P, Plumb K, Wang JK, Werner JS. Baseline OCT measurements in the idiopathic intracranial hypertension treatment trial, part II: correlations and relationship to clinical features. Invest Ophthalmol Vis Sci. 2014;55:8173–9.
Thambisetty M, Lavin PJ, Newman NJ, Biousse V. Fulminant idiopathic intracranial hypertension. Neurology. 2007;68:229–32.
Bailey IL, Lovie-Kitchin JE. Visual acuity testing. From the laboratory to the clinic. Vision Res. 2013;90:2–9.
Mwanza JC, Budenz DL. New developments in optical coherence tomography imaging for glaucoma. Curr Opin Ophthalmol. 2018;29:121–9.
Bruce BB, Kedar S, Van Stavern GP, Monaghan D, Acierno MD, Braswell RA, Preechawat P, Corbett JJ, Newman NJ, Biousse V. Idiopathic intracranial hypertension in men. Neurology. 2009;72:304–9.
Lenck S, Vallée F, Labeyrie MA, Touitou V, Saint-Maurice JP, Guillonnet A, Tantot A, Crassard I, Bernat AL, Houdart E. Stenting of the lateral sinus in idiopathic intracranial hypertension according to the type of stenosis. Neurosurgery. 2017;80:393–400.
Higgins JN, Owler BK, Cousins C, Pickard JD. Venous sinus stenting for refractory benign intracranial hypertension. Lancet. 2002;359:228–30.
Aguilar-Pérez M, Martinez-Moreno R, Kurre W, Wendl C, Bäzner H, Ganslandt O, Unsöld R, Henkes H. Endovascular treatment of idiopathic intracranial hypertension: retrospective analysis of immediate and long-term results in 51 patients. Neuroradiology. 2017;59:277–87.
Kumpe DA, Seinfeld J, Huang X, Mei Q, Case DE, Roark CD, Subramanian PS, Lind KE, Pelak VS, Bennett JL. Dural sinus stenting for idiopathic intracranial hypertension: factors associated with hemodynamic failure and management with extended stenting. J Neurointerv Surg. 2017;9:867–74.
Zhou D, Meng R, Zhang X, Guo L, Li S, Wu W, Duan J, Song H, Ding Y, Ji X. Intracranial hypertension induced by internal jugular vein stenosis can be resolved by stenting. Eur J Neurol. 2018;25:365–e13.
Starke RM, Wang T, Ding D, Durst CR, Crowley RW, Chalouhi N, Hasan DM, Dumont AS, Jabbour P, Liu KC. Endovascular treatment of venous sinus stenosis in idiopathic Intracranial hypertension: complications, neurological outcomes, and radiographic results. ScientificWorldJournal. 2015;2015:140408.
Dinkin MJ, Patsalides A. Venous sinus stenting in idiopathic intracranial hypertension: results of a prospective trial. J Neuroophthalmol. 2017;37:113–21.
Nicholson P, Brinjikji W, Radovanovic I, Hilditch CA, Tsang ACO, Krings T, Mendes Pereira V, Lenck S. Venous sinus stenting for idiopathic intracranial hypertension: a systematic review and meta-analysis. J Neurointerv Surg. 2019;11:380–5.
Liu KC, Starke RM, Durst CR, Wang TR, Ding D, Crowley RW, Newman SA. Venous sinus stenting for reduction of intracranial pressure in IIH: a prospective pilot study. J Neurosurg. 2017;127:1126–33.
Alessi G, Levrier O, Conrath J, Hoffart L, Donnet A, L’attention L, Metellus P, Giorgi R, Matonti F, Ridings B. Optical coherence tomography in following up papilledema in idiopathic intracranial hypertension treated with lateral sinus stent placement. J Fr Ophtalmol. 2010;33:637–48.
Shazly TA, Jadhav AP, Aghaebrahim A, Ducruet AF, Jankowitz BT, Jovin TG, Bonhomme GR. Venous sinus stenting shortens the duration of medical therapy for increased intracranial pressure secondary to venous sinus stenosis. J Neurointerv Surg. 2018;10:310–4.
Frisen L. Swelling of the optic nerve head: a staging scheme. J Neurol Neurosurg Psychiatry. 1982;45:13–8.
Fard MA, Ghahvechian H, Sahrayan A, Subramanian PS. Early macular vessel density loss in acute Ischemic optic neuropathy compared to papilledema: implications for pathogenesis. Transl Vis Sci Technol. 2018;7:10.
Albrecht P, Blasberg C, Ringelstein M, Müller AK, Finis D, Guthoff R, Kadas EM, Lagreze W, Aktas O, Hartung HP, Paul F, Brandt AU, Methner A. Optical coherence tomography for the diagnosis and monitoring of idiopathic intracranial hypertension. J Neurol. 2017;264:1370–80.
Wall M, George D. Idiopathic intracranial hypertension: a prospective study of 50 patients. Brain. 1991;114:155–80.
NORDIC Idiopathic Intracranial Hypertension Study Group Writing Committee, Wall M, McDermott MP, Kieburtz KD, Corbett JJ, Feldon SE, Friedman DI, Katz DM, Keltner JL, Schron EB, Kupersmith MJ. Effect of acetazolamide on visual function in patients with idiopathic intracranial hypertension and mild visual loss: the idiopathic intracranial hypertension treatment trial. JAMA. 2014;311:1641–51.
ten Hove MW, Friedman DI, Patel AD, Irrcher I, Wall M, McDermott MP; NORDIC Idiopathic Intracranial Hypertension Study Group. Safety and tolerability of acetazolamide in the idiopathic intracranial hypertension treatment trial. J Neuroophthalmol. 2016;36:13–9.
Satti SR, Leishangthem L, Chaudry MI. Meta-analysis of CSF diversion procedures and dural venous sinus stenting in the setting of medically refractory idiopathic intracranial hypertension. AJNR Am J Neuroradiol. 2015;36:1899–904.
Dinkin MJ, Patsalides A. Venous sinus stenting for idiopathic intracranial hypertension: where are we now? Neurol Clin. 2017;35:59–81.
Smith KA, Peterson JC, Arnold PM, Camarata PJ, Whittaker TJ, Abraham MG. A case series of dural venous sinus stenting in idiopathic intracranial hypertension: association of outcomes with optical coherence tomography. Int J Neurosci. 2017;127:145–53.
Author information
Authors and Affiliations
Contributions
All authors read and approved the submitted manuscript; the manuscript has not been submitted elsewhere nor published elsewhere in whole or in part. All authors contributed to the study conception and design. Data collection was performed by Romain Touzé, Sophie Bonnin and Stéphanie Lenck. Data analysis was performed by Romain Touzé and Sophie Bonnin. The first draft of the manuscript was written by Romain Touzé, Sophie Bonnin and Stéphanie Lenck, and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
R. Touzé, S. Bonnin, E. Houdart, P. Nicholson, B. Bodaghi, E. Shotar, S. Lenck, V. Touitou declare that they have no competing interests. F. Clarençon: Unrelated: Medtronic, Guerbet, Balt Extrusion (payment for readings), and Codman Neurovascular (core laboratory).
Ethical standards
This study has been approved by the local ethics committee (IRB 00008855). Because this study used data obtained as part of standard of care, the requirement for informed consent was waived.
Additional information
Availability of data and material
The authors declare that all data concerning this study are available on request.
Rights and permissions
About this article
Cite this article
Touzé, R., Bonnin, S., Houdart, E. et al. Long-term Kinetic Papilledema Improvement After Venous Sinus Stenting in Idiopathic Intracranial Hypertension. Clin Neuroradiol 31, 483–490 (2021). https://doi.org/10.1007/s00062-020-00908-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00062-020-00908-z