Abstract
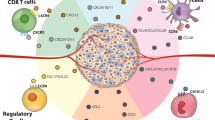
Immunotherapeutic treatment strategies greatly extend patient survival following malignant disease across a wide range of tumor types, including even those with metastatic disease. While diverse in approach, adoptive cell therapy, introduction of T cells that express chimeric antigen receptors, and checkpoint inhibitors all aim to re-invigorate the immune system to promote tumor cell identification and elimination. This review will focus on immune cell infiltration into tumors as well as a cellular organization within the tumor microenvironment as directed by the cell-specific expression patterns of chemokines and chemokine receptors. Through better understanding the chemokine network within tumors, we can uncover mechanisms to promote beneficial immune cell infiltration that can be combined with checkpoint inhibition. Conversely, chemokine expression is not limited to cells of the immune system, and it is understood that tumor cells also express chemokines and chemokine receptors. Tumor cells can hijack the chemokine networks to promote immune suppression and metastatic tumor cell trafficking. We will discuss the ways in which the chemokine network lies at the crossroad of immune evasion and tumor regression. Overall, this review will summarize key publications in the field of immune cell recruitment to tumors, highlight the dichotomous nature of chemokine interventions into cancer, and aims to identify therapeutic pathways forward.
Similar content being viewed by others
Abbreviations
- DC:
-
Dendritic cell
- TME:
-
Tumor microenvironment
- CAR:
-
Chimeric antigen receptor
- ACT:
-
Adoptive cell therapy
- MDSC:
-
Myeloid derived suppressor cell
- PTEN:
-
Phosphatase and tensin homolog
- NFκB:
-
Nuclear factor kappa-light-chain enhancer of activated B cells
- LIF:
-
Leukemia inhibitory factor
References
Holmes, W.E., J. Lee, W.J. Kuang, G.C. Rice, and W.I. Wood. 1991. Structure and functional expression of a human interleukin-8 receptor. Science 253 (5025): 1278–1280. https://doi.org/10.1126/science.1840701.
Murphy, P.M., and H.L. Tiffany. 1991. Cloning of complementary DNA encoding a functional human interleukin-8 receptor. Science 253 (5025): 1280–1283. https://doi.org/10.1126/science.1891716.
Rollins, B.J. 2009. Where the confusion began: cloning the first chemokine receptors. Journal of Immunology 183 (5): 2893–2894. https://doi.org/10.4049/jimmunol.0990065.
Strazza, M., and A. Mor. 2017. Consider the chemokines: a review of the interplay between chemokines and T cell subset function. Discovery Medicine 24 (130): 31–39.
Balkwill, F. 2004. Cancer and the chemokine network. Nature Reviews: Cancer 4 (7): 540–550. https://doi.org/10.1038/nrc1388.
Charo, I.F., and R.M. Ransohoff. 2006. The many roles of chemokines and chemokine receptors in inflammation. New England Journal of Medicine 354 (6): 610–621. https://doi.org/10.1056/NEJMra052723.
Chow, M.T., and A.D. Luster. 2014. Chemokines in cancer. Cancer Immunology Research 2 (12): 1125–1131. https://doi.org/10.1158/2326-6066.CIR-14-0160.
Strazza, M., I. Azoulay-Alfaguter, G.J. Silverman, and A. Mor. 2015. T cell chemokine receptor patterns as pathogenic signatures in autoimmunity. Discovery Medicine 19 (103): 117–125.
Chow, M.T., A.J. Ozga, R.L. Servis, D.T. Frederick, J.A. Lo, D.E. Fisher, G.J. Freeman, G.M. Boland, and A.D. Luster. 2019. Intratumoral activity of the CXCR3 chemokine system is required for the efficacy of anti-PD-1 therapy. Immunity 50 (6): 1498–1512 e1495. https://doi.org/10.1016/j.immuni.2019.04.010.
Ascierto, P.A., K.D. Lewis, A.M. Di Giacomo, L. Demidov, M. Mandala, I. Bondarenko, C. Herbert, et al. 2020. Prognostic impact of baseline tumour immune infiltrate on disease-free survival in patients with completely resected, BRAF(v600) mutation-positive melanoma receiving adjuvant vemurafenib. Annals of Oncology 31 (1): 153–159. https://doi.org/10.1016/j.annonc.2019.10.002.
Herbst, R.S., J.C. Soria, M. Kowanetz, G.D. Fine, O. Hamid, M.S. Gordon, J.A. Sosman, D. McDermott, J.D. Powderly, S.N. Gettinger, H.E. Kohrt, L. Horn, D.P. Lawrence, S. Rost, M. Leabman, Y. Xiao, A. Mokatrin, H. Koeppen, P.S. Hegde, I. Mellman, D.S. Chen, and F.S. Hodi. 2014. Predictive correlates of response to the anti-PD-L1 antibody MPDL3280A in cancer patients. Nature 515 (7528): 563–567. https://doi.org/10.1038/nature14011.
Jessurun, C.A.C., J.A.M. Vos, J. Limpens, and R.M. Luiten. 2017. Biomarkers for response of melanoma patients to immune checkpoint inhibitors: a systematic review. Frontiers in Oncology 7: 233. https://doi.org/10.3389/fonc.2017.00233.
Hegde, P.S., V. Karanikas, and S. Evers. 2016. The where, the when, and the how of immune monitoring for cancer immunotherapies in the era of checkpoint inhibition. Clinical Cancer Research 22 (8): 1865–1874. https://doi.org/10.1158/1078-0432.CCR-15-1507.
Chen, D.S., and I. Mellman. 2017. Elements of cancer immunity and the cancer-immune set point. Nature 541 (7637): 321–330. https://doi.org/10.1038/nature21349.
Ribas, A., and J.D. Wolchok. 2018. Cancer immunotherapy using checkpoint blockade. Science 359 (6382): 1350–1355. https://doi.org/10.1126/science.aar4060.
Ben-Baruch, A. 2006. The multifaceted roles of chemokines in malignancy. Cancer and Metastasis Reviews 25 (3): 357–371. https://doi.org/10.1007/s10555-006-9003-5.
Zlotnik, A., A.M. Burkhardt, and B. Homey. 2011. Homeostatic chemokine receptors and organ-specific metastasis. Nature Reviews: Immunology 11 (9): 597–606. https://doi.org/10.1038/nri3049.
Idorn, M., and P. Thor Straten. 2018. Chemokine receptors and exercise to tackle the inadequacy of T cell homing to the tumor site. Cells 7 (8). https://doi.org/10.3390/cells7080108.
Bilusic, M., C.R. Heery, J.M. Collins, R.N. Donahue, C. Palena, R.A. Madan, F. Karzai, J.L. Marté, J. Strauss, M.E. Gatti-Mays, J. Schlom, and J.L. Gulley. 2019. Phase I trial of HuMax-IL8 (BMS-986253), an anti-IL-8 monoclonal antibody, in patients with metastatic or unresectable solid tumors. Journal for Immunotherapy of Cancer 7 (1): 240. https://doi.org/10.1186/s40425-019-0706-x.
Liu, C., S. Zheng, R. Jin, X. Wang, F. Wang, R. Zang, H. Xu, et al. 2019. The superior efficacy of anti-PD-1/PD-L1 immunotherapy in KRAS-mutant non-small cell lung cancer that correlates with an inflammatory phenotype and increased immunogenicity. Cancer Letters. https://doi.org/10.1016/j.canlet.2019.10.027.
Spranger, S., R. Bao, and T.F. Gajewski. 2015. Melanoma-intrinsic beta-catenin signalling prevents anti-tumour immunity. Nature 523 (7559): 231–235. https://doi.org/10.1038/nature14404.
Li, F., S. Kitajima, S. Kohno, A. Yoshida, S. Tange, S. Sasaki, N. Okada, Y. Nishimoto, H. Muranaka, N. Nagatani, M. Suzuki, S. Masuda, T.C. Thai, T. Nishiuchi, T. Tanaka, D.A. Barbie, N. Mukaida, and C. Takahashi. 2019. Retinoblastoma inactivation induces a protumoral microenvironment via enhanced CCL2 secretion. Cancer Research 79 (15): 3903–3915. https://doi.org/10.1158/0008-5472.CAN-18-3604.
Peng, W., J.Q. Chen, C. Liu, S. Malu, C. Creasy, M.T. Tetzlaff, C. Xu, J. McKenzie, C. Zhang, X. Liang, L.J. Williams, W. Deng, G. Chen, R. Mbofung, A.J. Lazar, C.A. Torres-Cabala, Z.A. Cooper, P.L. Chen, T.N. Tieu, S. Spranger, X. Yu, C. Bernatchez, M.A. Forget, C. Haymaker, R. Amaria, J. McQuade, I.C. Glitza, T. Cascone, H.S. Li, L.N. Kwong, T.P. Heffernan, J. Hu, Bassett RL Jr, M.W. Bosenberg, S.E. Woodman, W.W. Overwijk, G. Lizée, J. Roszik, T.F. Gajewski, J.A. Wargo, J.E. Gershenwald, L. Radvanyi, M.A. Davies, and P. Hwu. 2016. Loss of PTEN promotes resistance to T cell-mediated immunotherapy. Cancer Discovery 6 (2): 202–216. https://doi.org/10.1158/2159-8290.CD-15-0283.
Huang, H., E. Langenkamp, M. Georganaki, A. Loskog, P.F. Fuchs, L.C. Dieterich, J. Kreuger, and A. Dimberg. 2015. VEGF suppresses T-lymphocyte infiltration in the tumor microenvironment through inhibition of NF-kappaB-induced endothelial activation. FASEB Journal 29 (1): 227–238. https://doi.org/10.1096/fj.14-250985.
Viola, A., A. Sarukhan, V. Bronte, and B. Molon. 2012. The pros and cons of chemokines in tumor immunology. Trends in Immunology 33 (10): 496–504. https://doi.org/10.1016/j.it.2012.05.007.
Zsiros, E., P. Duttagupta, D. Dangaj, H. Li, R. Frank, T. Garrabrant, I.S. Hagemann, B.L. Levine, C.H. June, L. Zhang, E. Wang, F.M. Marincola, D. Bedognetti, Powell DJ Jr, J. Tanyi, M.D. Feldman, L.E. Kandalaft, and G. Coukos. 2015. The ovarian cancer chemokine landscape is conducive to homing of vaccine-primed and CD3/CD28-costimulated T cells prepared for adoptive therapy. Clinical Cancer Research 21 (12): 2840–2850. https://doi.org/10.1158/1078-0432.CCR-14-2777.
Harlin, H., Y. Meng, A.C. Peterson, Y. Zha, M. Tretiakova, C. Slingluff, M. McKee, and T.F. Gajewski. 2009. Chemokine expression in melanoma metastases associated with CD8+ T-cell recruitment. Cancer Research 69 (7): 3077–3085. https://doi.org/10.1158/0008-5472.CAN-08-2281.
Sackstein, R., T. Schatton, and S.R. Barthel. 2017. T-lymphocyte homing: an underappreciated yet critical hurdle for successful cancer immunotherapy. Laboratory Investigation 97 (6): 669–697. https://doi.org/10.1038/labinvest.2017.25.
Dangaj, D., M. Bruand, A.J. Grimm, C. Ronet, D. Barras, P.A. Duttagupta, E. Lanitis, J. Duraiswamy, J.L. Tanyi, F. Benencia, J. Conejo-Garcia, H.R. Ramay, K.T. Montone, Powell DJ Jr, P.A. Gimotty, A. Facciabene, D.G. Jackson, J.S. Weber, S.J. Rodig, S.F. Hodi, L.E. Kandalaft, M. Irving, L. Zhang, P. Foukas, S. Rusakiewicz, M. Delorenzi, and G. Coukos. 2019. Cooperation between constitutive and inducible chemokines enables T cell engraftment and immune attack in solid tumors. Cancer Cell 35 (6): 885–900 e810. https://doi.org/10.1016/j.ccell.2019.05.004.
Mikucki, M.E., D.T. Fisher, J. Matsuzaki, J.J. Skitzki, N.B. Gaulin, J.B. Muhitch, A.W. Ku, J.G. Frelinger, K. Odunsi, T.F. Gajewski, A.D. Luster, and S.S. Evans. 2015. Non-redundant requirement for CXCR3 signalling during tumoricidal T-cell trafficking across tumour vascular checkpoints. Nature Communications 6: 7458. https://doi.org/10.1038/ncomms8458.
Triozzi, P.L., L. Schoenfield, T. Plesec, Y. Saunthararajah, R.R. Tubbs, and A.D. Singh. 2019. Molecular profiling of primary uveal melanomas with tumor-infiltrating lymphocytes. Oncoimmunology 8 (10): e947169. https://doi.org/10.4161/21624011.2014.947169.
Strazza, M., K. Adam, A.V. Smrcka, S. Lerrer, and A. Mor. 2020. PLCepsilon1 suppresses tumor growth by regulating murine T cell mobilization. Clinical and Experimental Immunology 200 (1): 53–60. https://doi.org/10.1111/cei.13409.
Strazza, M., I. Azoulay-Alfaguter, M. Peled, A.V. Smrcka, E.Y. Skolnik, S. Srivastava, and A. Mor. 2017. PLCepsilon1 regulates SDF-1alpha-induced lymphocyte adhesion and migration to sites of inflammation. Proceedings of the National Academy of Sciences of the United States of America 114 (10): 2693–2698. https://doi.org/10.1073/pnas.1612900114.
Jin, L., H. Tao, A. Karachi, Y. Long, A.Y. Hou, M. Na, K.A. Dyson, A.J. Grippin, L.P. Deleyrolle, W. Zhang, D.A. Rajon, Q.J. Wang, J.C. Yang, J.L. Kresak, E.J. Sayour, M. Rahman, F.J. Bova, Z. Lin, D.A. Mitchell, and J. Huang. 2019. CXCR1- or CXCR2-modified CAR T cells co-opt IL-8 for maximal antitumor efficacy in solid tumors. Nature Communications 10 (1): 4016. https://doi.org/10.1038/s41467-019-11869-4.
Whilding, L.M., L. Halim, B. Draper, A.C. Parente-Pereira, T. Zabinski, D.M. Davies, and J. Maher. 2019. CAR T-cells targeting the integrin alphavbeta6 and co-expressing the chemokine receptor CXCR2 demonstrate enhanced homing and efficacy against several solid malignancies. Cancers 11 (5). https://doi.org/10.3390/cancers11050674.
Donia, M., N. Junker, E. Ellebaek, M.H. Andersen, P.T. Straten, and I.M. Svane. 2012. Characterization and comparison of ‘standard’ and ‘young’ tumour-infiltrating lymphocytes for adoptive cell therapy at a Danish translational research institution. Scandinavian Journal of Immunology 75 (2): 157–167. https://doi.org/10.1111/j.1365-3083.2011.02640.x.
Rosenberg, S.A., J.C. Yang, R.M. Sherry, U.S. Kammula, M.S. Hughes, G.Q. Phan, D.E. Citrin, N.P. Restifo, P.F. Robbins, J.R. Wunderlich, K.E. Morton, C.M. Laurencot, S.M. Steinberg, D.E. White, and M.E. Dudley. 2011. Durable complete responses in heavily pretreated patients with metastatic melanoma using T-cell transfer immunotherapy. Clinical Cancer Research 17 (13): 4550–4557. https://doi.org/10.1158/1078-0432.CCR-11-0116.
Dudley, M.E., J.R. Wunderlich, T.E. Shelton, J. Even, and S.A. Rosenberg. 2003. Generation of tumor-infiltrating lymphocyte cultures for use in adoptive transfer therapy for melanoma patients. Journal of Immunotherapy 26 (4): 332–342. https://doi.org/10.1097/00002371-200307000-00005.
Sapoznik, S., R. Ortenberg, G. Galore-Haskel, S. Kozlovski, D. Levy, C. Avivi, I. Barshack, C.J. Cohen, M.J. Besser, J. Schachter, and G. Markel. 2012. CXCR1 as a novel target for directing reactive T cells toward melanoma: implications for adoptive cell transfer immunotherapy. Cancer Immunology, Immunotherapy 61 (10): 1833–1847. https://doi.org/10.1007/s00262-012-1245-1.
Idorn, M., P. Thor Straten, I.M. Svane, and O. Met. 2016. Transfection of tumor-infiltrating T cells with mRNA encoding CXCR2. Methods in Molecular Biology 1428: 261–276. https://doi.org/10.1007/978-1-4939-3625-0_17.
Peng, W., Y. Ye, B.A. Rabinovich, C. Liu, Y. Lou, M. Zhang, M. Whittington, Y. Yang, W.W. Overwijk, G. Lizée, and P. Hwu. 2010. Transduction of tumor-specific T cells with CXCR2 chemokine receptor improves migration to tumor and antitumor immune responses. Clinical Cancer Research 16 (22): 5458–5468. https://doi.org/10.1158/1078-0432.CCR-10-0712.
Kershaw, M.H., G. Wang, J.A. Westwood, R.K. Pachynski, H.L. Tiffany, F.M. Marincola, E. Wang, H.A. Young, P.M. Murphy, and P. Hwu. 2002. Redirecting migration of T cells to chemokine secreted from tumors by genetic modification with CXCR2. Human Gene Therapy 13 (16): 1971–1980. https://doi.org/10.1089/10430340260355374.
Murata, K., T. Tsukahara, M. Emori, Y. Shibayama, E. Mizushima, H. Matsumiya, K. Yamashita, M. Kaya, Y. Hirohashi, T. Kanaseki, T. Kubo, T. Himi, S. Ichimiya, T. Yamashita, N. Sato, and T. Torigoe. 2016. Identification of a novel human memory T-cell population with the characteristics of stem-like chemo-resistance. Oncoimmunology 5 (6): e1165376. https://doi.org/10.1080/2162402X.2016.1165376.
Gattinoni, L., C.A. Klebanoff, and N.P. Restifo. 2012. Paths to stemness: building the ultimate antitumour T cell. Nature Reviews: Cancer 12 (10): 671–684. https://doi.org/10.1038/nrc3322.
Gattinoni, L., E. Lugli, Y. Ji, Z. Pos, C.M. Paulos, M.F. Quigley, J.R. Almeida, E. Gostick, Z. Yu, C. Carpenito, E. Wang, D.C. Douek, D.A. Price, C.H. June, F.M. Marincola, M. Roederer, and N.P. Restifo. 2011. A human memory T cell subset with stem cell-like properties. Nature Medicine 17 (10): 1290–1297. https://doi.org/10.1038/nm.2446.
Di Stasi, A., B. De Angelis, C.M. Rooney, L. Zhang, A. Mahendravada, A.E. Foster, H.E. Heslop, M.K. Brenner, G. Dotti, and B. Savoldo. 2009. T lymphocytes coexpressing CCR4 and a chimeric antigen receptor targeting CD30 have improved homing and antitumor activity in a Hodgkin tumor model. Blood 113 (25): 6392–6402. https://doi.org/10.1182/blood-2009-03-209650.
Gowrishankar, K., L. Birtwistle, and K. Micklethwaite. 2018. Manipulating the tumor microenvironment by adoptive cell transfer of CAR T-cells. Mammalian Genome 29 (11–12): 739–756. https://doi.org/10.1007/s00335-018-9756-5.
Craddock, J.A., A. Lu, A. Bear, M. Pule, M.K. Brenner, C.M. Rooney, and A.E. Foster. 2010. Enhanced tumor trafficking of GD2 chimeric antigen receptor T cells by expression of the chemokine receptor CCR2b. Journal of Immunotherapy 33 (8): 780–788. https://doi.org/10.1097/CJI.0b013e3181ee6675.
Lesokhin, A.M., T.M. Hohl, S. Kitano, C. Cortez, D. Hirschhorn-Cymerman, F. Avogadri, G.A. Rizzuto, J.J. Lazarus, E.G. Pamer, A.N. Houghton, T. Merghoub, and J.D. Wolchok. 2012. Monocytic CCR2(+) myeloid-derived suppressor cells promote immune escape by limiting activated CD8 T-cell infiltration into the tumor microenvironment. Cancer Research 72 (4): 876–886. https://doi.org/10.1158/0008-5472.CAN-11-1792.
Mollica Poeta, V., M. Massara, A. Capucetti, and R. Bonecchi. 2019. Chemokines and chemokine receptors: new targets for cancer immunotherapy. Frontiers in Immunology 10: 379. https://doi.org/10.3389/fimmu.2019.00379.
Luster, A.D., and P. Leder. 1993. IP-10, a -C-X-C- chemokine, elicits a potent thymus-dependent antitumor response in vivo. Journal of Experimental Medicine 178 (3): 1057–1065. https://doi.org/10.1084/jem.178.3.1057.
House, I.G., P. Savas, J. Lai, A.X.Y. Chen, A.J. Oliver, Z.L. Teo, K.L. Todd, et al. 2019. Macrophage derived CXCL9 and CXCL10 are required for anti-tumor immune responses following immune checkpoint blockade. Clinical Cancer Research. https://doi.org/10.1158/1078-0432.CCR-19-1868.
Pascual-Garcia, M., E. Bonfill-Teixidor, E. Planas-Rigol, C. Rubio-Perez, R. Iurlaro, A. Arias, I. Cuartas, et al. 2019. LIF regulates CXCL9 in tumor-associated macrophages and prevents CD8(+) T cell tumor-infiltration impairing anti-PD1 therapy. Nature Communications 10 (1): 2416. https://doi.org/10.1038/s41467-019-10369-9.
Yan, M., N. Jene, D. Byrne, E.K. Millar, S.A. O'Toole, C.M. McNeil, G.J. Bates, et al. 2011. Recruitment of regulatory T cells is correlated with hypoxia-induced CXCR4 expression, and is associated with poor prognosis in basal-like breast cancers. Breast Cancer Research 13 (2): R47. https://doi.org/10.1186/bcr2869.
Zeng, Y., B. Li, Y. Liang, P.M. Reeves, X. Qu, C. Ran, Q. Liu, M.V. Callahan, A.E. Sluder, J.A. Gelfand, H. Chen, and M.C. Poznansky. 2019. Dual blockade of CXCL12-CXCR4 and PD-1-PD-L1 pathways prolongs survival of ovarian tumor-bearing mice by prevention of immunosuppression in the tumor microenvironment. FASEB Journal 33 (5): 6596–6608. https://doi.org/10.1096/fj.201802067RR.
Saxena, R., Y. Wang, and J.W. Mier. 2019. CXCR4 inhibition modulates the tumor microenvironment and retards the growth of B16-OVA melanoma and Renca tumors. Melanoma Research. https://doi.org/10.1097/CMR.0000000000000639.
Wu, A., R. Maxwell, Y. Xia, P. Cardarelli, M. Oyasu, Z. Belcaid, E. Kim, A. Hung, A.S. Luksik, T. Garzon-Muvdi, C.M. Jackson, D. Mathios, D. Theodros, J. Cogswell, H. Brem, D.M. Pardoll, and M. Lim. 2019. Combination anti-CXCR4 and anti-PD-1 immunotherapy provides survival benefit in glioblastoma through immune cell modulation of tumor microenvironment. Journal of Neuro-Oncology 143 (2): 241–249. https://doi.org/10.1007/s11060-019-03172-5.
Medicine, U.S. National Library of. 2017. Olaptesed (NOX-A12) alone and in combination with pembrolizumab in colorectal and pancreatic cancer (Keynote-559). https://clinicaltrials.gov/ct2/show/NCT03168139. Accessed Nov 18, 2019.
Funding
This work was supported by grants from the NIH (AI25640 and CA231277) and from the Cancer Research Institute.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Strazza, M., Mor, A. The Complexity of Targeting Chemokines to Promote a Tumor Immune Response. Inflammation 43, 1201–1208 (2020). https://doi.org/10.1007/s10753-020-01235-8
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-020-01235-8