Abstract
Purpose
Pelvic fractures are known to be one of the most difficult injuries to treat. The objective of this study is to introduce a novel technique for virtual unilateral pelvic fracture reconstruction. Since the pelvis exhibits remarkable left–right symmetry, the contralateral hemipelvis can be used as a template for rebuilding the fractured hemipelvis.
Methods
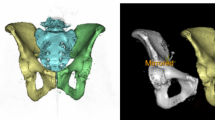
CT scan data of the pelvic region of eight subjects with acute unilateral pelvic fractures were involved in this study. Computer-aided design software was used to create 3D models of these pelvises. The contralateral hemipelvis of each subject was then reflected across the sagittal plane, and the fractured hemipelvis was rebuilt by aligning the bone fragments with their equivalent location on the reflected side. To evaluate the quality of this reduction process, a 3D deviation analysis was conducted to calculate the differences between the reflected intact hemipelvis and the reconstructed hemipelvis.
Results
Results showed that the average root mean square (RMS) of deviations and average percentage of points within a ± 2 mm predefined threshold was 1.32 ± 0.22 mm and 88.4 ± 3.78%, respectively. The deviation color maps obtained indicated that the largest differences were along the fracture lines and on the non-articular surfaces of the pelvises.
Conclusion
These results allowed us to conclude the validity of this procedure, since the average RMS difference was below 2 mm and the average percentage of points within ± 2 mm was high. The proposed technique will allow surgeons to provide their patients with more accurate reconstruction procedures which can potentially improve surgical outcomes.














Similar content being viewed by others
References
Hernandez D, Garimella R, Eltorai AEM, Daniels AH (2017) Computer-assisted orthopaedic surgery. Orthop Surg 9:152–158. https://doi.org/10.1111/os.12323
Schendel S, Hazan-Molina H, Rachmiel A, Aizenbud D (2012) The future in craniofacial surgery: computer-assisted planning. Rambam Maimonides Med J 3:e0012. https://doi.org/10.5041/rmmj.10079
Perlick L, Bäthis H, Perlick C, Lüring C, Tingart M, Grifka J (2005) Revision total knee arthroplasty: a comparison of postoperative leg alignment after computer-assisted implantation versus the conventional technique. Knee Surg Sport Traumatol Arthrosc 13:167–173. https://doi.org/10.1007/s00167-004-0507-7
Verstreken K, Van Cleynenbreugel J, Marchal G, Van Steenberghe D, Suetens P (1996) Computer-assisted planning of oral implant surgery: an approach using virtual reality. Stud Health Technol Inform 29:423–434. https://doi.org/10.3233/978-1-60750-873-1-423
Boudissa M, Courvoisier A, Chabanas M, Tonetti J (2018) Computer assisted surgery in preoperative planning of acetabular fracture surgery: state of the art. Exp Rev Med Devices 15:81–89. https://doi.org/10.1080/17434440.2017.1413347
Fornaro J, Keel M, Harders M, Marincek B, Székely G, Frauenfelder T (2010) An interactive surgical planning tool for acetabular fractures: initial results. J Orthop Surg Res 5:1–9. https://doi.org/10.1186/1749-799X-5-50
Pahuta MA, Schemitsch EH, Backstein D, Papp S, Gofton W (2012) Virtual fracture carving improves understanding of a complex fracture: a randomized controlled study. J Bone Jt Surg Ser A 94:1–7. https://doi.org/10.2106/JBJS.K.00996
Zeng C, Xing W, Wu Z, Huang H, Huang W (2016) A combination of three-dimensional printing and computer-assisted virtual surgical procedure for preoperative planning of acetabular fracture reduction. Injury 47:2223–2227. https://doi.org/10.1016/j.injury.2016.03.015
Oliveri H, Boudissa M, Tonetti J, Chabanas M (2017) Planning acetabular fracture reduction using patient-specific multibody simulation of the hip. Med Imaging 2017 Image Guid Proced Robot Interv Model 10135:101352P. https://doi.org/10.1117/12.2250380
Wang GY, Huang WJ, Song Q, Qin YT, Liang JF (2016) Computer-assisted virtual preoperative planning in orthopedic surgery for acetabular fractures based on actual computed tomography data. Comput Assist Surg 21:160–165. https://doi.org/10.1080/24699322.2016.1240235
Cimerman M, Kristan A (2007) Preoperative planning in pelvic and acetabular surgery: the value of advanced computerised planning modules. Injury 38:442–449. https://doi.org/10.1016/j.injury.2007.01.033
Hu Y, Li H, Qiao G, Liu H, Ji A, Ye F (2011) Computer-assisted virtual surgical procedure for acetabular fractures based on real CT data. Injury 42:1121–1124. https://doi.org/10.1016/j.injury.2011.01.014
Lee P, Lai J, Hu Y, Huang C, Tsai Y, Ueng W (2012) Virtual 3D planning of pelvic fracture. Biomed Eng Appl Basis Commun 24:245–262. https://doi.org/10.1142/S101623721250007X
Boudissa M, Chabanas M, Oliveri H, Tonetti J (2015) Virtual fracture reduction of the acetabulum using a rigid body biomechanical model. Rev Chir Orthop Traumatol 101:S187. https://doi.org/10.1016/j.rcot.2015.09.119
Wang D, Wang Y, Wu S, Lin H, Yang Y, Fan S, Gu C, Wang J, Song C (2017) Customized a Ti6Al4V bone plate for complex pelvic fracture by selective laser melting. Materials (Basel). https://doi.org/10.3390/ma10010035
Upex P, Jouffroy P, Riouallon G (2017) Application of 3D printing for treating fractures of both columns of the acetabulum: benefit of pre-contouring plates on the mirrored healthy pelvis. Orthop Traumatol Surg Res 103:331–334. https://doi.org/10.1016/j.otsr.2016.11.021
Shen F, Chen B, Guo Q, Qi Y, Shen Y (2013) Augmented reality patient-specific reconstruction plate design for pelvic and acetabular fracture surgery. Int J Comput Assist Radiol Surg 8:169–179. https://doi.org/10.1007/s11548-012-0775-5
Dreizen S, Snodgrasse RM, Webb Peploe H, Parker GS, Spies TD (1957) Bilateral symmetry of skeletal maturation in the human hand and wrist. AMA J Dis Child 93:122–127. https://doi.org/10.1001/archpedi.1957.02060040124004
Grammer K, Thornhill R (1994) Human (Homo sapiens) facial attractiveness and sexual selection: the role of symmetry and averageness. J Comp Psychol 108:233–242. https://doi.org/10.1037/0735-7036.108.3.233
Jansen J, Dubois L, Schreurs R, Gooris PJJ, Maal TJJ, Beenen LF, Becking AG (2018) Should virtual mirroring be used in the preoperative planning of an orbital reconstruction? J Oral Maxillofac Surg 76:380–387. https://doi.org/10.1016/j.joms.2017.09.018
Islam K, Dobbe A, Komeili A, Duke K, El-Rich M, Dhillon S, Adeeb S, Jomha NM (2014) Symmetry analysis of talus bone. Bone Jt Res 3:139–145. https://doi.org/10.1302/2046-3758.35.2000264
Ead MS, Duke KK, Jaremko JL, Westover L (2020) Investigation of pelvic symmetry using CAD software. Med Biol Eng Comput 58:75–82. https://doi.org/10.1007/s11517-019-02068-w
Boulay C, Tardieu C, Bénaim C, Hecquet J, Marty C, Prat-Pradal D, Legaye J, Duval-Beaupère G, Pélissier J (2006) Three-dimensional study of pelvic asymmetry on anatomical specimens and its clinical perspectives. J Anat 208:21–33. https://doi.org/10.1111/j.1469-7580.2006.00513.x
Osterhoff G, Petersik A, Sprengel K, Pape HC (2019) Symmetry matching of the medial acetabular surface-a quantitative analysis in view of patient-specific implants. J Orthop Trauma 33:e79–e83. https://doi.org/10.1097/BOT.0000000000001373
Letournel E, Judet R (1993) Fractures of the acetabulum. Springer, Berlin
Acknowledgements
The authors would like to acknowledge the support of the Natural Sciences and Engineering Research Council of Canada (NSERC) for funding this work. We also thank Irina Ilic for her assistance in the pelvis digitization process.
Funding
This work was funded by the Natural Sciences and Engineering Research Council of Canada (NSERC).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethics approval
Approval from the Health Research Ethics Board at the University of Alberta was obtained with a waiver of consent to use the data anonymously.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ead, M.S., Westover, L., Polege, S. et al. Virtual reconstruction of unilateral pelvic fractures by using pelvic symmetry. Int J CARS 15, 1267–1277 (2020). https://doi.org/10.1007/s11548-020-02140-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11548-020-02140-z