Abstract
Purpose
To evaluate if there was a correlation between in vivo kinematics of a medial-stabilized (MS) total knee arthroplasty (TKA) and post-operative clinical scores. We hypothesized that (1) a MS-TKA would produce a medial pivot movement and that (2) this specific pattern would be correlated with higher clinical scores.
Methods
18 patients were evaluated through clinical and functional scores evaluation (Knee Society Score clinical and functional, Womac, Oxford), and kinematically through dynamic radiostereometric analysis (RSA) at 9 months after MS-TKA, during the execution of a sit-to-stand and a lunge motor task. The anteroposterior (AP) Low Point translation of medial and lateral femoral compartments was compared through Student’s t test (p < 0.05). A correlation analysis between scores and kinematics was performed through the Pearson’s correlation coefficient r.
Results
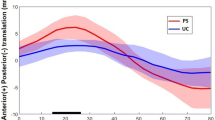
A significantly greater (p < 0.0001) anterior translation of the lateral compartment with respect to the medial one was found in both sit-to-stand (medial 2.9 mm ± 0.7 mm, lateral 7.1 mm ± 0.6 mm) and lunge (medial 5.3 mm ± 0.9 mm, lateral 10.9 mm ± 0.7 mm) motor tasks, thus resulting in a medial pivot pattern in about 70% of patients. Significant positive correlation in sit-to-stand was found between the peak of AP translation in the lateral compartment and clinical scores (r = 0.59 for Knee Society Score clinical and r = 0.61 for Oxford). Moreover, we found that the higher peak of AP translation of the medial compartment correlated with lower clinical scores (r = − 0.55 for Knee Society Score clinical, r = − 0.61 for Womac and r = − 0.53 for Oxford) in the lunge. A negative correlation was found between Knee Society Score clinical and VV laxity during sit-to-stand (r = − 0.56) and peak of external rotation in the lunge motor task (r = − 0.66).
Conclusions
The MS-TKA investigated produced in vivo a medial pivot movement in about 70% of patients in both examined motor tasks. There was a correlation between the presence of medial pivot and higher post-operative scores.
Level of evidence
IV.


Similar content being viewed by others
References
Banks SA, Hodge WA (2004) 2003 Hap Paul Award paper of the international society for technology in arthroplasty. Design and activity dependence of kinematics in fixed and mobile-bearing knee arthroplasties. J Arthroplasty 19:809–816
Behrend H, Giesinger K, Giesinger JM, Kuster MS (2012) The “forgotten joint” as the ultimate goal in joint arthroplasty: validation of a new patient-reported outcome measure. J Arthroplasty 27:430–436.e1
Bontempi M, Roberti di Sarsina T, Marcheggiani Muccioli GM, Pizza N, Cardinale U, Bragonzoni L, Zaffagnini S (2019) J-curve design total knee arthroplasty: the posterior stabilized shows wider medial pivot compared to the cruciate retaining during chair raising. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-019-05645-6
Bragonzoni L, Marcheggiani Muccioli GM, Bontempi M, Roberti di Sarsina T, Cardinale U, Alesi D, Iacono F, Neri MP, Zaffagnini S (2018) New design total knee arthroplasty shows medial pivoting movement under weight-bearing conditions. Knee Surg Sports Traumatol Arthrosc 27(4):1049–1056
Brinkman J-M, Bubra PS, Walker P, Walsh WR, Bruce WJM (2014) Midterm results using a medial pivot total knee replacement compared with the Australian national joint replacement registry data. ANZ J Surg 84:172–176
Cardinale U, Bragonzoni L, Bontempi M, Alesi D, Roberti di Sarsina T, Lo Presti M, Zaffagnini S, Marcheggiani Muccioli GM, Iacono F (2019) Knee kinematics after cruciate retaining highly congruent mobile bearing total knee arthroplasty: an in vivo dynamic RSA study. Knee pii S0968–0160(19):30258–30263. https://doi.org/10.1016/j.knee.2019.11.003
Dennis DA, Mahfouz MR, Komistek RD, Hoff W (2005) In vivo determination of normal and anterior cruciate ligament-deficient knee kinematics. J Biomech 38:241–253
Fan C-Y, Hsieh JT-S, Hsieh M-S, Shih Y-C, Lee C-H (2010) Primitive results after medial-pivot knee arthroplasties: a minimum 5-year follow-up study. J Arthroplasty 25:492–496
Freeman MAR, Pinskerova V (2005) The movement of the normal tibio-femoral joint. J Biomech 38:197–208
Freeman MAR, Pinskerova V (2003) The movement of the knee studied by magnetic resonance imaging. Clin Orthop Relat Res 410:35–43
Gunaratne R, Pratt DN, Banda J, Fick DP, Khan RJK, Robertson BW (2017) Patient dissatisfaction following total knee arthroplasty: a systematic review of the literature. J Arthroplasty 32:3854–3860
Hossain F, Patel S, Rhee S-J, Haddad FS (2011) Knee arthroplasty with a medially conforming ball-and-socket tibiofemoral articulation provides better function. Clin Orthop Relat Res 469:55–63
Johal P, Williams A, Wragg P, Hunt D, Gedroyc W (2005) Tibio-femoral movement in the living knee. A study of weight bearing and non-weight bearing knee kinematics using ‘interventional’ MRI. J Biomech 38:269–276
Karachalios T, Roidis N, Giotikas D, Bargiotas K, Varitimidis S, Malizos KN (2009) A mid-term clinical outcome study of the Advance Medial Pivot knee arthroplasty. Knee 16:484–488
Marcheggiani Muccioli GM, Pizza N, Di Paolo S, Zinno R, Alesi D, Roberti Di Sarsina T, Bontempi M, Zaffagnini S, Bragonzoni L (2020) Multi-radius posterior-stabilized mobile-bearing total knee arthroplasty partially produces in-vivo medial pivot during activity of daily living and high demanding motor task. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-05846-4
Nakagawa S, Kadoya Y, Todo S, Kobayashi A, Sakamoto H, Freeman MA, Yamano Y (2000) Tibiofemoral movement 3: full flexion in the living knee studied by MRI. J Bone Joint Surg Br 82:1199–1200
Scott G, Imam MA, Eifert A, Freeman MAR, Pinskerova V, Field RE, Skinner J, Banks SA (2016) Can a total knee arthroplasty be both rotationally unconstrained and anteroposteriorly stabilised? A pulsed fluoroscopic investigation. Bone Joint Res 5:80–86
Steinbrück A, Schröder C, Woiczinski M, Fottner A, Pinskerova V, Müller PE, Jansson V (2016) Femorotibial kinematics and load patterns after total knee arthroplasty: An in vitro comparison of posterior-stabilized versus medial-stabilized design. Clin Biomech (Bristol, Avon) 33:42–48
Van Onsem S, Verstraete M, Van Eenoo W, Van Der Straeten C, Victor J (2019) Are TKA kinematics during closed kinetic chain exercises associated with patient-reported outcomes? a preliminary analysis. Clin Orthop Relat Res 478(2):255–263
Van Overschelde P, Pinskerova V, Koch PP, Fornasieri C, Fucentese S (2017) Redefining knee balance in a medially stabilized prosthesis: an in-vitro study. Open Orthop J 11:1165–1172
Vanlommel L, Vanlommel J, Claes S, Bellemans J (2013) Slight undercorrection following total knee arthroplasty results in superior clinical outcomes in varus knees. Knee Surg Sports Traumatol Arthrosc 21:2325–2330
Watanabe T, Koga H, Katagiri H, Otabe K, Nakagawa Y, Muneta T, Sekiya I, Jinno T (2019) Coronal and sagittal laxity affects clinical outcomes in posterior-stabilized total knee arthroplasty: assessment of well-functioning knees. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-019-05500-8
Funding
This research received no specific grant from any funding agency in the public, commercial or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors declare that they have no conflict of interest.
Ethical approval
This study obtained the approval from IRB of the IRCCS Rizzoli Orthopaedic Institute (ID: 003603 February 16th, 2016).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Alesi, D., Marcheggiani Muccioli, G., Roberti di Sarsina, T. et al. In vivo femorotibial kinematics of medial-stabilized total knee arthroplasty correlates to post-operative clinical outcomes. Knee Surg Sports Traumatol Arthrosc 29, 491–497 (2021). https://doi.org/10.1007/s00167-020-05975-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-020-05975-w