Abstract
Background
This study was designed to investigate whether 3D laparoscopic common bile duct (LCBDE) could improve surgical outcomes in choledocholithiasis patients compared with 2D LCBDE.
Method
Propensity score-matched analysis was performed to balance the bias in baseline characteristic between two groups.
Results
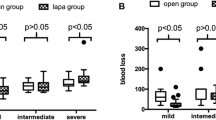
213 patients underwent 3D LCBDE and 212 patients receiving 2D LCBDE were enrolled in this study. The operation time and blood loss in 3D group were significantly less than that in 2D group. After propensity score matching, a total of 114 paired cases were selected from the two groups. The operation time and blood loss in 3D group remain significantly lower than in 2D group. In the end, the subgroup analysis based on abdominal adhesion level was performed and it was observed that for patients with adhesion level 1 and level 2, 3D surgery could obviously decrease the operation time and intraoperative blood loss.
Conclusions
3D LCBDE would significantly reduce operation time, blood loss, and conversion rate to laparotomy in choledocholithiasis patients versus 2D LCBDE. For patients with abdominal adhesions level 1 and level 2, 3D LCBDE could provide better surgical outcomes than 2D LCBDE.


Similar content being viewed by others
References
Chan DS, Jain PA, Khalifa A et al (2014) Laparoscopic common bile duct exploration. Br J Surg 101:1448–1452
Tan J, Tan Y, Chen F et al (2015) Endoscopic or laparoscopic approach for hepatolithiasis in the era of endoscopy in China. Surg Endosc 29:154–162
Baucom RB, Feurer ID, Shelton JS et al (2016) Surgeons, ERCP, and laparoscopic common bile duct exploration: do we need a standard approach for common bile duct stones? Surg Endosc 30:414–423
Tzovaras G, Baloyiannis I, Zachari E et al (2012) Laparoendoscopic rendezvous versus preoperative ERCP and laparoscopic cholecystectomy for the management of cholecysto-choledocholithiasis: interim analysis of a controlled randomized trial. Ann Surg 255:435–439
Zheng C, Huang Y, Xie E et al (2017) Laparoscopic common bile duct exploration: a safe and definitive treatment for elderly patients. Surg Endosc 31:2541–2547
Velayutham V, Fuks D, Nomi T et al (2016) 3D visualization reduces operating time when compared to high-definition 2D in laparoscopic liver resection: a case-matched study. Surg Endosc 30:147–153
Wagner OJ, Hagen M, Kurmann A et al (2012) Three-dimensional vision enhances task performance independently of the surgical method. Surg Endosc 26:2961–2968
Bilgen K, Ustun M, Karakahya M et al (2013) Comparison of 3D imaging and 2D imaging for performance time of laparoscopic cholecystectomy. Surg Laparosc Endosc Percutan Tech 23:180–183
Cologne KG, Zehetner J, Liwanag L et al (2015) Three-dimensional laparoscopy: does improved visualization decrease the learning curve among trainees in advanced procedures? Surg Laparosc Endosc Percutan Tech 25:321–323
Sakata S, Grove PM, Stevenson AR (2016) Effect of 3-dimensional vision on surgeons using the da Vinci robot for laparoscopy: more than meets the eye. JAMA Surg 151:793–794
Dowson HM, Bong JJ, Lovell DP et al (2008) Reduced adhesion formation following laparoscopic versus open colorectal surgery. Br J Surg 95:909–914
Pan L, Chen M, Ji L et al (2018) The Safety and efficacy of laparoscopic common bile duct exploration combined with cholecystectomy for the management of cholecysto-choledocholithiasis: an up-to-date meta-analysis. Ann Surg 268(2):247–253
Zhou Y, Wu XD, Fan RG et al (2014) Laparoscopic common bile duct exploration and primary closure of choledochotomy after failed endoscopic sphincterotomy. Int J Surg 12:645–648
Vidagany NE, Del Domingo CD, Tomas NP et al (2016) Eleven years of primary closure of common bile duct after choledochotomy for choledocholithiasis. Surg Endosc 30:1975–1982
Feng X, Morandi A, Boehne M et al (2015) 3-Dimensional (3D) laparoscopy improves operating time in small spaces without impact on hemodynamics and psychomental stress parameters of the surgeon. Surg Endosc 29:1231–1239
Kunert W, Storz P, Kirschniak A (2013) For 3D laparoscopy: a step toward advanced surgical navigation: how to get maximum benefit from 3D vision. Surg Endosc 27:696–699
Mutter D, Dallemagne B, Bailey C et al (2009) 3D virtual reality and selective vascular control for laparoscopic left hepatic lobectomy. Surg Endosc 23:432–435
Sorensen SM, Savran MM, Konge L et al (2016) Three-dimensional versus two-dimensional vision in laparoscopy: a systematic review. Surg Endosc 30:11–23
Wang Y, Bo X, Wang Y et al (2017) Laparoscopic surgery for choledocholithiasis concomitant with calculus of the left intrahepatic duct or abdominal adhesions. Surg Endosc 31:4780–4789
Zhu J, Sun G, Hong L et al (2018) Laparoscopic common bile duct exploration in patients with previous upper abdominal surgery. Surg Endosc 32(12):4893–4899
Srinivas GN (2006) Conversion rate for laparoscopic cholecystectomy after endoscopic retrograde cholangiography in the treatment of choledocholithiasis: does the time interval matter? Surg Endosc 20:1932
Cakir M, Kucukkartallar T, Tekin A et al (2015) Does endoscopic retrograde cholangiopancreatography have a negative effect on laparoscopic cholecystectomy? Ulus Cerrahi Derg 31:128–131
Schiphorst AH, Besselink MG, Boerma D et al (2008) Timing of cholecystectomy after endoscopic sphincterotomy for common bile duct stones. Surg Endosc 22:2046–2050
Behman R, Nathens AB, Byrne JP et al (2017) Laparoscopic surgery for adhesive small bowel obstruction is associated with a higher risk of bowel injury: a population-based analysis of 8584 patients. Ann Surg 266:489–498
Acknowledgements
This study was supported by Grants from the National Natural Science Foundation of China (No. 81872352) and the Foundation of Shanghai Science and Technology Committee (16411952000) and JianFeng project of XuHui Provincial Commission of Health and Family Planning (SHXH201703) and the Shanghai Medical Discipline of Key Programs for General Surgery (2017ZZ02007) and Clinical Study of Zhongshan Hospital (2018ZSLC24).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Disclosures
Xiaobo Bo, Jie Wang, Yanlei Xin, Lingxi Nan, Zhihui Gao, Changcheng Wang, Min Li, Sheng Shen, Han Liu, Xiaoling Ni, Tao Suo, Dexiang Zhang, Yueqi Wang, Houbao Liu have no conflict of interest or financial ties to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Bo, X., Wang, J., Nan, L. et al. 3D laparoscopic common bile duct exploration versus 2D in choledocholithiasis patients: a propensity score analysis. Surg Endosc 35, 819–825 (2021). https://doi.org/10.1007/s00464-020-07453-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-020-07453-3