Abstract
Purpose
To evaluate the outcomes of emergency endovascular treatments for delayed bleeding after pancreaticobiliary surgery.
Methods
We retrospectively evaluated 21 patients (M:F = 13:8, median age = 64 years) undergoing 23 endovascular treatments, performed from 2010 to 2017 in a single center. Data collected were patient characteristics; surgery; pathology; incidence of postoperative pancreatic fistulas (POPF); bleeding signs on CT and angiography; damaged artery; endovascular tools used; technical and clinical success; intervals between surgery, endovascular treatment, and discharge; survival rates.
Results
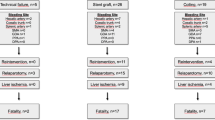
Sixteen patients had pancreatoduodenectomy, three hepaticojejunostomy, two distal pancreatectomy. Indications for surgery were mainly biliary (33%), pancreatic (19%), or duodenal (10%) malignancies. Seventeen patients had “grade C” POPF, three suffered a biliary leak, one had no POPF. Active bleeding was present in 17/23 CTs and in 22/23 angiographies, mostly from hepatic (43%), gastroduodenal (22%), and splenic (13%) arteries. The endovascular treatments were performed with coils (26%), glue (22%), stent-graft (22%), and their combinations (30%). Sixteen patients had a single endovascular treatment, one underwent a second embolization, three had subsequent surgery, one had repeat embolization followed by surgery. Relaparotomy rate was 19%. Median hospital stay was 37 days (range 12–75); median intervals among pancreaticobiliary surgery, endovascular treatment, and discharge were 21 (2–36) and 12 (8–47) days, respectively.
We observed 4/21 intrahospital deaths (median: 31 days from endovascular treatment, 4–53); 1-year survival rate of discharged patients was 71%.
Conclusions
Endovascular treatment using embolization and/or stent-graft placement is a useful first-line intervention to halt postoperative hemorrhage after pancreaticobiliary surgery and decreases the need for urgent relaparotomy.




Similar content being viewed by others
Change history
09 September 2020
The original version of this article has an error in the affiliations of all the authors. The authors affiliations are corrected.
References
Andrén-Sandberg A (2011) Complications of pancreatic surgery. N Am J Med Sci 3:531–535. https://doi.org/10.4297/najms.2011.3531
Yekebas EF, Wolfram L, Cataldegirmen G et al (2007) Postpancreatectomy hemorrhage: diagnosis and treatment: an analysis in 1669 consecutive pancreatic resections. Ann Surg 246:269–280. https://doi.org/10.1097/01.sla.0000262953.77735.db
van Berge Henegouwen MI, Allema JH, van Gulik TM et al (1995) Delayed massive haemorrhage after pancreatic and biliary surgery. Br J Surg 82:1527–1531
Wente MN, Veit JA, Bassi C et al (2007) Postpancreatectomy hemorrhage (PPH): an International Study Group of Pancreatic Surgery (ISGPS) definition. Surgery 142:20–25. https://doi.org/10.1016/j.surg.2007.02.001
Phillip V, Rasch S, Gaa J et al (2013) Spontaneous bleeding in pancreatitis treated by transcatheter arterial coil embolization: a retrospective study. PLoS ONE 8:e72903. https://doi.org/10.1371/journal.pone.0072903
Mauri G, Mattiuz C, Sconfienza LM et al (2015) Role of interventional radiology in the management of complications after pancreatic surgery: a pictorial review. Insights Imaging 6:231–239. https://doi.org/10.1007/s13244-014-0372-y
Rajarathinam G, Kannan DG, Vimalraj V et al (2008) Post pancreaticoduodenectomy haemorrhage: outcome prediction based on new ISGPS Clinical severity grading. HPB (Oxford) 10:363–370. https://doi.org/10.1080/13651820802247086
Lessing Y, Pencovich N, Nevo N et al (2019) Early reoperation following pancreaticoduodenectomy: impact on morbidity, mortality, and long-term survival. World J Surg Oncol 17:26. https://doi.org/10.1186/s12957-019-1569-9
Chatani S, Inoue A, Ohta S et al (2018) Transcatheter arterial embolization for postoperative bleeding following abdominal surgery. Cardiovasc Intervent Radiol 41:1346–1355. https://doi.org/10.1007/s00270-018-2019-8
Bassi C, Marchegiani G, Dervenis C et al (2017) The 2016 update of the International Study Group (ISGPS) definition and grading of postoperative pancreatic fistula: 11 Years After. Surgery 161:584–591. https://doi.org/10.1016/j.surg.2016.11.014
Tejedor L, Serrablo A (2013) Postoperative Pancreatic Biliary Surgical Complications. Journal of Gastroenterology and Hepatology Research
Fuks D, Piessen G, Huet E et al (2009) Life-threatening postoperative pancreatic fistula (grade C) after pancreaticoduodenectomy: incidence, prognosis, and risk factors. Am J Surg 197:702–709. https://doi.org/10.1016/j.amjsurg.2008.03.004
Schäfer M, Heinrich S, Pfammatter T, Clavien P-A (2011) Management of delayed major visceral arterial bleeding after pancreatic surgery. HPB 13:132–138. https://doi.org/10.1111/j.1477-2574.2010.00260.x
Shander A, Javidroozi M, Naqvi S, et al. (2014) An update on mortality and morbidity in patients with very low postoperative hemoglobin levels who decline blood transfusion (CME). Transfusion 54:2688–95; quiz 2687. https://doi.org/10.1111/trf.12565
Sevransky J (2009) Clinical assessment of hemodynamically unstable patients. Curr Opin Crit Care 15:234–238. https://doi.org/10.1097/MCC.0b013e32832b70e5
Ho C-K, Kleeff J, Friess H, Büchler MW (2005) Complications of pancreatic surgery. HPB (Oxford) 7:99–108. https://doi.org/10.1080/13651820510028936
Pedrazzoli S, Liessi G, Pasquali C et al (2009) Postoperative pancreatic fistulas: preventing severe complications and reducing reoperation and mortality rate. Ann Surg 249:97–104. https://doi.org/10.1097/SLA.0b013e31819274fe
Iswanto S, Nussbaum ML (2014) Hepatic artery pseudoaneurysm after surgical treatment for pancreatic cancer: minimally invasive angiographic techniques as the preferred treatment. N Am J Med Sci 6:287–290. https://doi.org/10.4103/1947-2714.134377
Huan L, Fei Q, Lin H et al (2017) Is peritoneal drainage essential after pancreatic surgery?: A meta-analysis and systematic review. Medicine (Baltimore) 96:e9245. https://doi.org/10.1097/MD.0000000000009245
Yamauchi FI, Ortega CD, Blasbalg R et al (2012) Multidetector CT evaluation of the postoperative pancreas. Radiographics 32:743–764. https://doi.org/10.1148/rg.323105121
Lanza E, Muglia R, Solbiati LA, et al. (218) Emergency transarterial embolization in postoperative hip bleeding: indications, techniques, and results in a retrospective cohort. J Arthroplasty 33:2273–2278. https://doi.org/10.1016/j.arth.2018.02.005
Roulin D, Cerantola Y, Demartines N, Schäfer M (2011) Systematic review of delayed postoperative hemorrhage after pancreatic resection. J Gastrointest Surg 15:1055–1062. https://doi.org/10.1007/s11605-011-1427-8
Andersson E, Ansari D, Andersson R (2010) Major haemorrhagic complications of acute pancreatitis. Br J Surg 97:1379–1384. https://doi.org/10.1002/bjs.7113
Roberts KJ, Blanco G, Webber J et al (2014) How severe is diabetes after total pancreatectomy? A case-matched analysis. HPB (Oxford) 16:814–821. https://doi.org/10.1111/hpb.12203
Nykänen T, Udd M, Peltola EK et al (2017) Bleeding pancreatic pseudoaneurysms: management by angioembolization combined with therapeutic endoscopy. Surg Endosc 31:692–703. https://doi.org/10.1007/s00464-016-5023-6
Zhang C, Li A, Luo T et al (2019) Strategy and management of severe hemorrhage complicating pancreatitis and post-pancreatectomy. Diagn Interv Radiol 25:81–89. https://doi.org/10.5152/dir.2018.18283
Limongelli P, Khorsandi SE, Pai M, et al. (2008) Management of delayed postoperative hemorrhage after pancreaticoduodenectomy: a meta-analysis. Arch Surg 143:1001–7; discussion 1007. https://doi.org/10.1001/archsurg.143.10.1001
Vaidya S, Tozer KR, Chen J (2008) An overview of embolic agents. Semin Intervent Radiol 25:204–215. https://doi.org/10.1055/s-0028-1085930
Loya MF, Mangat S, Santoro GC et al (2018) Prophylactic absorbable gelatin sponge embolization for angiographically occult splenic hemorrhage. Radiol Case Rep 13:753–758. https://doi.org/10.1016/j.radcr.2018.01.005
Won Y, Lee SL, Kim Y, Ku YM (2015) Clinical efficacy of transcatheter embolization of visceral artery pseudoaneurysms using N-butyl cyanoacrylate (NBCA). Diagn Interv Imaging 96:563–569. https://doi.org/10.1016/j.diii.2015.01.003
Saad NEA, Saad WEA, Davies MG et al (2005) Pseudoaneurysms and the role of minimally invasive techniques in their management. Radiographics 25 Suppl 1:S173–S189. https://doi.org/10.1148/rg.25si055503
Anil G, Tan AGS, Cheong HW et al (2012) Emergency gastroduodenal artery embolization by sandwich technique for angiographically obvious and oblivious, endotherapy failed bleeding duodenal ulcers. Clin Radiol 67:468–475. https://doi.org/10.1016/j.crad.2011.10.026
Wang BH, Boulton M, Lee DH et al (2018) A systematic characterization of the factors influencing polymerization and dynamic behavior of n-butyl cyanoacrylate. J Neurointerv Surg 10:150–155. https://doi.org/10.1136/neurintsurg-2017-013009
Lanza E, Poretti D, Tramarin M et al (2014) Colonic ischemia, perforation, and colectomy after a complicated endovascular embolization for type II endoleak with the use of cyanoacrylate glue. J Vasc Interv Radiol 25:1482–1484. https://doi.org/10.1016/j.jvir.2014.05.018
Hill H, Chick JFB, Hage A, Srinivasa RN (2018) N-butyl cyanoacrylate embolotherapy: techniques, complications, and management. Diagn Interv Radiol 24:98–103. https://doi.org/10.5152/dir.2018.17432
Nemes B, Járányi Z, Bérczi V et al (2005) Stent-graft Treatment of Carotid Pseudoaneurysms: Case Report and Review of the Literature. EJVES Extra 10:45–50. https://doi.org/10.1016/j.ejvsextra.2005.05.004
Cappucci M, Zarco F, Orgera G et al (2017) Endovascular treatment of visceral artery aneurysms and pseudoaneurysms with stent-graft: Analysis of immediate and long-term results. Cir Esp 95:283–292. https://doi.org/10.1016/j.ciresp.2017.04.011
Venturini M, Marra P, Colombo M et al (2018) Endovascular Repair of 40 Visceral Artery Aneurysms and Pseudoaneurysms with the Viabahn Stent-Graft: Technical Aspects, Clinical Outcome and Mid-Term Patency. Cardiovasc Intervent Radiol 41:385–397. https://doi.org/10.1007/s00270-017-1844-5
Ching KC, Santos E, McCluskey KM et al (2016) Covered stents and coil embolization for treatment of postpancreatectomy arterial hemorrhage. J Vasc Interv Radiol 27:73–79. https://doi.org/10.1016/j.jvir.2015.09.024
Dabbs DN, Stein DM, Scalea TM (2009) Major hepatic necrosis: a common complication after angioembolization for treatment of high-grade liver injuries. J Trauma 66:621–7; discussion 627. https://doi.org/10.1097/TA.0b013e31819919f2
Huang X-Q, Huang Z-Q, Duan W-D et al (2002) Severe biliary complications after hepatic artery embolization. World J Gastroenterol 8:119–123
Halloran CM, Ghaneh P, Bosonnet L et al (2002) Complications of pancreatic cancer resection. Dig Surg 19:138–146. https://doi.org/10.1159/000052029
de Castro SMM, Kuhlmann KFD, Busch ORC et al (2005) Delayed massive hemorrhage after pancreatic and biliary surgery: embolization or surgery? Ann Surg 241:85–91.
Funding
No financial help was obtained for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Muglia, R., Lanza, E., Poretti, D. et al. Emergency endovascular treatments for delayed hemorrhage after pancreaticobiliary surgery: indications, outcomes, and follow-up of a retrospective cohort. Abdom Radiol 45, 2593–2602 (2020). https://doi.org/10.1007/s00261-020-02480-z
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-020-02480-z