Abstract
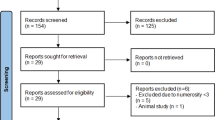
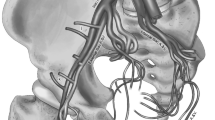
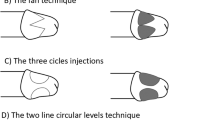
Reconstructive surgery of the penis holds many unique challenges due to the unique physiological properties of the tissues. Much of the effort involved therefore goes to preserving as much of the native tissue as possible whilst novel and creative methods have been adopted to repair defects and in creation of neophallus. A search of the PubMed database was carried out using the following keywords: ‘penile trauma’, ‘penile cancer’, ‘lichen sclerosus’, ‘glansectomy’, ‘glans resurfacing’, ‘penile-sparing surgery’, ‘micropenis’, ‘aphallia’, ‘female-to-male sex reassignment surgery’, ‘scrotal flap’ and ‘genital lymphoedema’. Results for glans resurfacing in treating cancer showed low local recurrence rates at 0–10% whilst 90% of lichen sclerosus patients reported complete resolutions of pain and pruritis. For repairs of penile shaft skin defects the literature supports the use of full-thickness skin graft and pedicled scrotal flaps. The radial artery-based forearm free flap remains the best option for neophallus creation in terms of function, sensation and cosmesis but unfortunately leaves a disfiguring scar and involves multiple stages. Some novel techniques have been developed to circumvent these issues and are discussed. This article presents an update on the important developments in the field of penile reconstructive surgery.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 8 print issues and online access
$259.00 per year
only $32.38 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A. Cancer statistics, 2016. CA Cancer J Clin 2016;66:7–30.
Pizzocaro G, Algaba F, Horenblas S, Solsona E, Tana S, Van Der Poel H, et al. EAU penile cancer guidelines 2009. Eur Urol. 2010;57:1002–12.
Brown CT, Minhas S, Ralph DJ. Conservative surgery for penile cancer: subtotal glans excision without grafting. BJU Int. 2005;96:911–2.
Depasquale I, Park AJ, Bracka A. The treatment of balanitis xerotica obliterans: the treatment of Bxo. BJU Int. 2000;86:459–65.
Hadway P, Corbishley CM, Watkin NA. Total glans resurfacing for premalignant lesions of the penis: initial outcome data. BJU Int. 2006;98:532–6.
O’Kelly F, Lonergan P, Lundon D, Nason G, Sweeney P, Cullen I, et al. A prospective study of total glans resurfacing for localized penile cancer to maximize oncologic and functional outcomes in a tertiary referral network. J Urol. 2017;197:1258–63.
Shabbir M, Muneer A, Kalsi J, Shukla CJ, Zacharakis E, Garaffa G, et al. Glans resurfacing for the treatment of carcinoma in situ of the penis: surgical technique and outcomes. Eur Urol. 2011;59:142–7.
Philippou P, Shabbir M, Malone P, Nigam R, Muneer A, Ralph DJ, et al. Conservative surgery for squamous cell carcinoma of the penis: resection margins and long-term oncological control. J Urol. 2012;188:803–8.
Pietrzak P, Corbishley C, Watkin N. Organ-sparing surgery for invasive penile cancer: early follow-up data. BJU Int. 2004;94:1253–7.
Morelli G, Pagni R, Mariani C, Campo G, Menchini-Fabris F, Minervini R, et al. Glansectomy with split-thickness skin graft for the treatment of penile carcinoma. Int J Impot Res. 2009;21:311–4.
Malone PR, Thomas JS, Blick C. A tie-over dressing for graft application in distal penectomy and glans resurfacing: the TODGA technique. BJU Int. 2011;107:836–40.
Sedigh O, Falcone M, Ceruti C, Timpano M, Preto M, Oderda M, et al. Sexual function after surgical treatment for penile cancer: Which organ-sparing approach gives the best results? Can Urol Assoc J. 2015;9:423.
Gulino G, Sasso F, Falabella R, Bassi PF. Distal urethral reconstruction of the glans for penile carcinoma: results of a novel technique at 1-year of followup. J Urol. 2007;178:941–4.
Algaba F, Arce Y, López-Beltrán A, Montironi R, Mikuz G, Bono AV. Intraoperative frozen section diagnosis in urological oncology. Eur Urol. 2005;47:129–36.
Kamel MH, Bissada N, Warford R, Farias J, Davis R. Organ sparing surgery for penile cancer: a systematic review. J Urol. 2017;198:770–9.
Hegarty PK, Shabbir M, Hughes B, Minhas S, Perry M, Watkin N, et al. Penile preserving surgery and surgical strategies to maximize penile form and function in penile cancer: recommendations from the United Kingdom experience. World J Urol. 2009;27:179–87.
Baumgarten AS, Fisher JS, Lawindy SM, Pavlinec JG, Carrion RE, Spiess PE. Penile sparing surgical approaches for primary penile tumors: preserving function and appearance. Transl Androl Urol. 2017 ;6:809–19.
Djajadiningrat RS, van Werkhoven E, Meinhardt W, van Rhijn BWG, Bex A, van der Poel HG, et al. Penile sparing surgery for penile cancer—does it affect survival? J Urol. 2014;192:120–6.
Garaffa G, Christopher N, Ralph DJ. The management of genital lymphoedema. BJU Int. 2008;102:480–4.
Shim TN, Doiron PR, Francis N, Minhas S, Muneer A, Hawkins D, et al. Penile lymphoedema: approach to investigation and management. Clin Exp Dermatol. 2019;44:20–31.
Garaffa G, Raheem AA, Ralph DJ. An update on penile reconstruction. Asian J Androl. 2011;13:391–4.
Jeong JH, Shin HJ, Woo SH, Seul JH. A new repair technique for penile paraffinoma: bilateral scrotal flaps. Ann Plast Surg. 1996;37:386–93.
Fakin R, Zimmermann S, Jindarak S, Lindenblatt N, Giovanoli P, Suwajo P. Reconstruction of penile shaft defects following silicone injection by bipedicled anterior scrotal flap. J Urol. 2017;197:1166–70.
Li C-Y, Kayes O, Kell PD, Christopher N, Minhas S, Ralph DJ. Penile suspensory ligament division for penile augmentation: indications and results. Eur Urol. 2006;49:729–33.
Morrison SD, Shakir A, Vyas KS, Kirby J, Crane CN, Lee GK. Phalloplasty: a review of techniques and outcomes. Plast Reconstr Surg. 2016;138:594–615.
Wierckx K, Van Caenegem E, Elaut E, Dedecker D, Van de Peer F, Toye K, et al. Quality of life and sexual health after sex reassignment surgery in transsexual men. J Sex Med. 2011;8:3379–88.
Bogoraz NA. On complete plastic reconstruction of a penis sufficient for coitus. Sov Surg. 1936;8:303–9.
Nair R, Sriprasad S. 1129 Sir Harold Gillies: pioneer of phalloplasty and the birth of uroplastic surgery. J Urol. 2010;183(4S). https://doi.org/10.1016/j.juro.2010.02.2326.
Chang T-S, Hwang W-Y. Forearm flap in one-stage reconstruction of the penis. Plast Reconstr Surg. 1984 ;74:251–8.
Song R, Gao Y, Song Y, Yu Y, Song Y. The forearm flap. Clin Plast Surg. 1982;9:21–6.
Garaffa G, Christopher NA, Ralph DJ. Total phallic reconstruction in female-to-male transsexuals. Eur Urol. 2010;57:715–22.
Ascha M, Massie JP, Morrison SD, Crane CN, Chen ML. Outcomes of single stage phalloplasty by pedicled anterolateral thigh flap versus radial forearm free flap in gender confirming surgery. J Urol. 2018 ;199:206–14.
Monstrey S, Hoebeke P, Dhont M, Selvaggi G, Hamdi M, Van Landuyt K, et al. Radial forearm phalloplasty: a review of 81 cases. Eur J Plast Surg. 2005;28:206–12.
Baumeister S, Sohn M, Domke C, Exner K. Phallusbildung beim Frau-zu-Mann Transsexuellen: Erfahrung in 259 Fällen. Handchir Mikrochir Plast Chir. 2011;43:215–21.
Heston AL, Esmonde NO, Dugi III DD, Berli JU. Phalloplasty: techniques and outcomes. Transl Androl Urol. 2019;8(Jun):254–65.
Garaffa G, Ralph DJ, Christopher N. Total urethral construction with the radial artery-based forearm free flap in the transsexual: creation of a sensate neourethra in female-to-male transsexuals. BJU Int. 2010;106:1206–10.
Selvaggi G, Monstrey S, Hoebeke P, Ceulemans P, Van Landuyt K, Hamdi M, et al. Donor-site morbidity of the radial forearm free flap after 125 phalloplasties in gender identity disorder. Plast Reconstr Surg. 2006;118:1171–7.
Felici N, Felici A. A new phalloplasty technique: the free anterolateral thigh flap phalloplasty. J Plast Reconstr Aesthet Surg. 2006;59:153–7.
D’Arpa S, Claes K, Lumen N, Oieni S, Hoebeke P, Monstrey S. Urethral reconstruction in anterolateral thigh flap phalloplasty: a 93-case experience. Plast Reconstr Surg. 2019;143:382e–92e.
Bettocchi C, Ralph DJ, Pryor JP. Pedicled pubic phalloplasty in females with gender dysphoria. BJU Int. 2005;95:120–4.
Kocjancic E, Jaunarena JH, Schechter L, Acar Ö. Inflatable penile prosthesis implantation after gender affirming phalloplasty with radial forearm free flap. Int J Impot Res. 2019; http://www.nature.com/articles/s41443-019-0153-8.
Falcone M, Garaffa G, Gillo A, Dente D, Christopher AN, Ralph DJ. Outcomes of inflatable penile prosthesis insertion in 247 patients completing female to male gender reassignment surgery. BJU Int. 2018;121:139–44.
Neuville P, Morel-Journel N, Maucourt-Boulch D, Ruffion A, Paparel P, Terrier J-E. Surgical outcomes of erectile implants after phalloplasty: retrospective analysis of 95 procedures. J Sex Med. 2016;13:1758–64.
Hoebeke PB, Decaestecker K, Beysens M, Opdenakker Y, Lumen N, Monstrey SM. Erectile implants in female-to-male transsexuals: our experience in 129 patients. Eur Urol. 2010;57:334–41.
Schlenker B, Tilki D, Gratzke C, Seitz M, Reich O, Schneede P, et al. Intermediate-differentiated invasive (pT1 G2) penile cancer—oncological outcome and follow-up. Urol Oncol Semin Orig Investig. 2011;29:782–7.
Ayres BE, Lam W, Al-Najjar HM, Corbishley CM, Perry MJA, Watkin NA. 1106 glans resurfacing—a new penile preserving option for superficially invasive penile cancer. Eur Urol. 2011;10(Suppl 2):340.
Garaffa G, Shabbir M, Christopher N, Minhas S, Ralph DJ. The surgical management of Lichen Sclerosus of the glans penis: our experience and review of the literature. J Sex Med. 2011;8:1246–53.
Håkansson U, Kirrander P, Uvelius B, Baseckas G, Torbrand C. Organ-sparing reconstructive surgery in penile cancer: initial experiences at two Swedish referral centres. Scand J Urol. 2015;49:149–54.
Chipollini J, Yan S, Ottenhof SR, Zhu Y, Draeger D, Baumgarten AS, et al. Surgical management of penile carcinoma in situ: results from an international collaborative study and review of the literature. BJU Int. 2018 ;121:393–8.
O’Kane HF, Pahuja A, Ho KJ, Thwaini A, Nambirajan T, Keane P. Outcome of glansectomy and skin grafting in the management of penile cancer. Adv Urol. 2011;2011:1–4.
Palminteri E, Berdondini E, Lazzeri M, Mirri F, Barbagli G. Resurfacing and reconstruction of the glans penis. Eur Urol. 2007;52:893–900.
Smith Y, Hadway P, Biedrzycki O, Perry MJA, Corbishley C, Watkin NA. Reconstructive surgery for invasive squamous carcinoma of the glans penis. Eur Urol. 2007;52:1179–85.
Veeratterapillay R, Sahadevan K, Aluru P, Asterling S, Rao GS, Greene D. Organ-preserving surgery for penile cancer: description of techniques and surgical outcomes: organ-preserving surgery for penile cancer. BJU Int. 2012;110:1792–5.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflicts of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kristinsson, S., Johnson, M. & Ralph, D. Review of penile reconstructive techniques. Int J Impot Res 33, 243–250 (2021). https://doi.org/10.1038/s41443-020-0246-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41443-020-0246-4
This article is cited by
-
Case report. Resurfacing van de glans penis bij therapieresistente lichen sclerosus: een weinig bekende therapeutische optie
Tijdschrift voor Urologie (2023)
-
Reconstruction of penile skin loss using a combined therapy of negative pressure wound therapy, dermal regeneration template, and split-thickness skin graft application
International Journal of Impotence Research (2021)
-
Imaging in Gender Affirmation Surgery
Current Urology Reports (2021)