Abstract
Objectives
This randomized controlled trial compares for the first time effects of Alvogyl versus absorbable gelatin sponge as palatal wound dressings on postoperative pain, amount of analgesic consumption, post-surgical bleeding, and wound re-epithelization.
Materials and methods
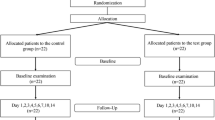
Following sample size calculation, 36 systemically healthy patients requiring palatal mucosal graft harvesting were randomized to receive Alvogyl (intervention group, 18 patients) or absorbable gelatin sponge (control group, 18 patients) palatal dressings. Patient-reported VAS pain scores over 2 weeks were defined as primary outcome. Post-surgical bleeding, number of analgesics consumed, and complete re-epithelialization of the palatal wound for up to 5 weeks were defined as secondary outcomes.
Results
Although significantly higher VAS pain scores were reported in the control as compared with the intervention group up to 12 days post-surgically (from (median [range]) 8.5 [2–10] to 1 [0–2] and from 6 [0–10] to 0 [0–2] respectively), with higher analgesics consumption (from 2 [1–3] to 1 [0–3] and from 1 [0–3] to 0 [0–2] tablets respectively), a multivariate regression analysis considering age, gender, graft width/length, tissue thickness, analgesics intake, and dressing type demonstrated no statistically significant effect of any factor, including dressing type on VAS pain scores. At 4 weeks, 22.2% of patients in the intervention group versus 11.1% in the control group demonstrated complete re-epithelization of their palatal engraftment site, before complete re-epithelization in both groups at 5 weeks. No post-surgical bleeding was reported with both dressings.
Conclusions
Within the study’s limitations, results suggest Alvogyl as a practical palatal surgical dressing, comparable with absorbable gelatin sponge in cost, pain reduction, hemostasis, and re-epithelization properties.
Trial registration
www.ClinicalTrials.gov Identifier: NCT03402321
Clinical relevance
Alvogyl could present a novel palatal wound dressing material, comparable with gelatin sponge.


Similar content being viewed by others
References
Sculean A, Gruber R, Bosshardt DD (2014) Soft tissue wound healing around teeth and dental implants. J Clin Periodontol 41(Suppl 15):S6–S22. https://doi.org/10.1111/jcpe.12206
Cho MI, Garant PR (2000) Development and general structure of the periodontium. Periodontol 2000 24:9–27. https://doi.org/10.1034/j.1600-0757.2000.2240102.x
Harris RJ (2003) Histologic evaluation of connective tissue grafts in humans. Int J Periodontics Restorative Dent 23(6):575–583
Müller HP, Schaller N, Eger T, Heinecke A (2000) Thickness of masticatory mucosa. J Clin Periodontol 27(6):431–436
Bhatia G, Kumar A, Khatri M, Bansal M, Saxena S (2015) Assessment of the width of attached gingiva using different methods in various age groups: a clinical study. J Indian Soc Periodontol 19(2):199–202. https://doi.org/10.4103/0972-124X.152106
Zucchelli G, Mele M, Stefanini M, Mazzotti C, Marzadori M, Montebugnoli L, de Sanctis M (2010) Patient morbidity and root coverage outcome after subepithelial connective tissue and de-epithelialized grafts: a comparative randomized-controlled clinical trial. J Clin Periodontol 37(8):728–738. https://doi.org/10.1111/j.1600-051X.2010.01550.x
Kim DM, Neiva R (2015) Periodontal soft tissue non-root coverage procedures: a systematic review from the AAP Regeneration Workshop. J Periodontol 86(2 Suppl):S56–S72. https://doi.org/10.1902/jop.2015.130684
Wang HL, Bunyaratavej P, Labadie M, Shyr Y, MacNeil RL (2001) Comparison of 2 clinical techniques for treatment of gingival recession. J Periodontol 72(10):1301–1311. https://doi.org/10.1902/jop.2001.72.10.1301
Yen CA, Griffin TJ, Cheung WS, Chen J (2007) Effects of platelet concentrate on palatal wound healing after connective tissue graft harvesting. J Periodontol 78(4):601–610. https://doi.org/10.1902/jop.2007.060275
Griffin TJ, Cheung WS, Zavras AI, Damoulis PD (2006) Postoperative complications following gingival augmentation procedures. J Periodontol 77(12):2070–2079. https://doi.org/10.1902/jop.2006.050296
Wessel JR, Tatakis DN (2008) Patient outcomes following subepithelial connective tissue graft and free gingival graft procedures. J Periodontol 79(3):425–430. https://doi.org/10.1902/jop.2008.070325
Ayvazyan A, Morimoto N, Kanda N, Takemoto S, Kawai K, Sakamoto Y, Taira T, Suzuki S (2011) Collagen-gelatin scaffold impregnated with bFGF accelerates palatal wound healing of palatal mucosa in dogs. J Surg Res 171(2):e247–e257. https://doi.org/10.1016/j.jss.2011.06.059
Rossmann JA, Rees TD (1999) A comparative evaluation of hemostatic agents in the management of soft tissue graft donor site bleeding. J Periodontol 70(11):1369–1375. https://doi.org/10.1902/jop.1999.70.11.1369
Femminella B, Iaconi MC, Di Tullio M, Romano L, Sinjari B, D’Arcangelo C, De Ninis P, Paolantonio M (2016) Clinical comparison of platelet-rich fibrin and a gelatin sponge in the management of palatal wounds after epithelialized free gingival graft harvest: a randomized clinical trial. J Periodontol 87(2):103–113. https://doi.org/10.1902/jop.2015.150198
Keceli HG, Aylikci BU, Koseoglu S, Dolgun A (2015) Evaluation of palatal donor site haemostasis and wound healing after free gingival graft surgery. J Clin Periodontol 42(6):582–589. https://doi.org/10.1111/jcpe.12404
Taberner-Vallverdú M, Nazir M, Sánchez-Garcés M, Gay-Escoda C (2015) Efficacy of different methods used for dry socket management: a systematic review. Med Oral Patol Oral Cir Bucal 20(5):e633–e639
Pal US, Singh BP, Verma V (2013) Comparative evaluation of zinc oxide eugenol versus gelatin sponge soaked in plasma rich in growth factor in the treatment of dry socket: an initial study. In: Contemp Clin Dent, vol 4. vol 1. pp 37-41. https://doi.org/10.4103/0976-237x.111592
Zhang EX, Zhang KH, Geng WQ, Zhang GX (1983) Experimental “dry socket” and evaluation of common clinical treatments. Chin Med J 96(7):539–546
Björn H (1963) Free transplantation of gingiva propria. Sveriges Tandläkarforbunds Tidning 22:684
Price DD, McGrath PA, Rafii A, Buckingham B (1983) The validation of visual analogue scales as ratio scale measures for chronic and experimental pain. Pain 17(1):45–56
Burkhardt R, Hämmerle CH, Lang NP, Healing RGoOSTBW (2015) Self-reported pain perception of patients after mucosal graft harvesting in the palatal area. J Clin Periodontol 42(3):281–287. https://doi.org/10.1111/jcpe.12357
Marucha PT, Kiecolt-Glaser JK, Favagehi M (1998) Mucosal wound healing is impaired by examination stress. Psychosom Med 60(3):362–365
Shetty V, Schwartz HC (2006) Wound healing and perioperative care. Oral Maxillofac Surg Clin North Am 18(1):107–113, vii. https://doi.org/10.1016/j.coms.2005.09.004
Rani A, Mohanty S, Sharma P, Dabas J (2016) Comparative evaluation of Er:Cr:YSGG, diode laser and Alvogyl in the management of alveolar osteitis: a prospective randomized clinical study. J Maxillofac Oral Surg 15(3):349–354. https://doi.org/10.1007/s12663-015-0848-4
Supe NB, Choudhary SH, Yamyar SM, Patil KS, Choudhary AK, Kadam VD (2018) Efficacy of Alvogyl (combination of iodoform + butylparaminobenzoate) and zinc oxide eugenol for dry socket. Ann Maxillofac Surg 8(2):193–199. https://doi.org/10.4103/ams.ams_167_18
Amiri A, Dugas R, Pichot AL, Bompeix G (2008) In vitro and in vivo [corrected] activity of eugenol oil (Eugenia caryophylata) against four important postharvest apple pathogens. Int J Food Microbiol 126(1–2):13–19. https://doi.org/10.1016/j.ijfoodmicro.2008.04.022
Syrjänen SM, Syrjänen KJ (1979) Influence of Alvogyl on the healing of extraction wound in man. Int J Oral Surg 8(1):22–30. https://doi.org/10.1016/s0300-9785(79)80035-6
Steinmetz EF (1969) Penawar Djambe. Quarterly Journal of Crude Drug Research 9(1):1326–1327. https://doi.org/10.3109/13880206909066272
AbdullGaffar B, Awadhi F (2019) Be aware of a potential pitfall in oral and dental specimens: Alvogyl fibers. Int J Surg Pathol. https://doi.org/10.1177/1066896919884647
Blum IR (2002) Contemporary views on dry socket (alveolar osteitis): a clinical appraisal of standardization, aetiopathogenesis and management: a critical review. Int J Oral Maxillofac Surg 31(3):309–317. https://doi.org/10.1054/ijom.2002.0263
Faizel S, Thomas S, Yuvaraj V, Prabhu S, Tripathi G (2015) Comparision between neocone, alvogyl and zinc oxide eugenol packing for the treatment of dry socket: a double blind randomised control trial. J Maxillofac Oral Surg 14(2):312–320. https://doi.org/10.1007/s12663-014-0667-z
Djagny VB, Wang Z, Xu S (2001) Gelatin: a valuable protein for food and pharmaceutical industries: review. Crit Rev Food Sci Nutr 41(6):481–492. https://doi.org/10.1080/20014091091904
Jang HJ, Kim YM, Yoo BY, Seo YK (2018) Wound-healing effects of human dermal components with gelatin dressing. J Biomater Appl 32(6):716–724. https://doi.org/10.1177/0885328217741758
Tomizawa Y (2005) Clinical benefits and risk analysis of topical hemostats: a review. J Artif Organs 8(3):137–142. https://doi.org/10.1007/s10047-005-0296-x
Rohanizadeh R, Swain MV, Mason RS (2008) Gelatin sponges (Gelfoam) as a scaffold for osteoblasts. J Mater Sci Mater Med 19(3):1173–1182. https://doi.org/10.1007/s10856-007-3154-y
Finn MD, Schow SR, Schneiderman ED (1992) Osseous regeneration in the presence of four common hemostatic agents. J Oral Maxillofac Surg 50(6):608–612. https://doi.org/10.1016/0278-2391(92)90443-4
Ponticiello MS, Schinagl RM, Kadiyala S, Barry FP (2000) Gelatin-based resorbable sponge as a carrier matrix for human mesenchymal stem cells in cartilage regeneration therapy. J Biomed Mater Res 52(2):246–255. https://doi.org/10.1002/1097-4636(200011)52:2<246::aid-jbm2>3.0.co;2-w
Fawzy El-Sayed KM, Dorfer CE (2016) Gingival mesenchymal stem/progenitor cells: a unique tissue engineering gem. Stem Cells Int 2016:7154327. https://doi.org/10.1155/2016/7154327
Tavelli L, Asa’ad F, Acunzo R, Pagni G, Consonni D, Rasperini G (2018) Minimizing patient morbidity following palatal gingival harvesting: a randomized controlled clinical study. Int J Periodontics Restorative Dent 38(6):e127–e134. https://doi.org/10.11607/prd.3581
Sharma V, Kumar A, Puri K, Bansal M, Khatri M (2019) Application of platelet-rich fibrin membrane and collagen dressing as palatal bandage for wound healing: a randomized clinical control trial. Indian J Dent Res 30(6):881–888. https://doi.org/10.4103/ijdr.IJDR_370_17
Tavelli L, Ravida A, Saleh MHA, Maska B, Del Amo FS, Rasperini G, Wang HL (2019) Pain perception following epithelialized gingival graft harvesting: a randomized clinical trial. Clin Oral Investig 23(1):459–468. https://doi.org/10.1007/s00784-018-2455-5
Yildirim S, Ozener HO, Dogan B, Kuru B (2018) Effect of topically applied hyaluronic acid on pain and palatal epithelial wound healing: an examiner-masked, randomized, controlled clinical trial. J Periodontol 89(1):36–45. https://doi.org/10.1902/jop.2017.170105
Kulkarni MR, Thomas BS, Varghese JM, Bhat GS (2014) Platelet-rich fibrin as an adjunct to palatal wound healing after harvesting a free gingival graft: a case series. J Indian Soc Periodontol 18(3):399–402. https://doi.org/10.4103/0972-124X.134591
Thoma DS, Hilbe M, Bienz SP, Sancho-Puchades M, Hammerle CH, Jung RE (2016) Palatal wound healing using a xenogeneic collagen matrix - histological outcomes of a randomized controlled clinical trial. J Clin Periodontol 43(12):1124–1131. https://doi.org/10.1111/jcpe.12624
Shanmugam M, Kumar TS, Arun KV, Arun R, Karthik SJ (2010) Clinical and histological evaluation of two dressing materials in the healing of palatal wounds. J Indian Soc Periodontol 14(4):241–244. https://doi.org/10.4103/0972-124X.76929
Bahammam MA (2018) Effect of platelet-rich fibrin palatal bandage on pain scores and wound healing after free gingival graft: a randomized controlled clinical trial. Clin Oral Investig 22(9):3179–3188. https://doi.org/10.1007/s00784-018-2397-y
Belkhede SG, Salaria SK, Aggarwal R (2019) Comparative evaluation of the platelet-rich fibrin bandage versus gelatin sponge-assisted palatal wound healing of free gingival graft donor site: a case series. J Indian Soc Periodontol 23(6):589–592. https://doi.org/10.4103/jisp.jisp_165_19
Acknowledgments
The authors thank Dr. Khaled Keraa for his excellent statistical analyses.
Funding
The work was supported by the Department of Oral Medicine and Periodontology, Faculty of Dentistry, Cairo University, Egypt.
Author information
Authors and Affiliations
Contributions
Priv-Doz. Dr. Karim M. Fawzy El-Sayed: conceived and designed the idea of the experiment, conducted and supervised the conduction of the experiment, interpreting the results, and drafted and revised the manuscript; Dr. Karim Ehab and Dr. Abdallah Hassan: conducted the experiment and acquired the data; Prof. Omenya Abouldahab: interpreting the results and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 19 kb)
Rights and permissions
About this article
Cite this article
Ehab, K., Abouldahab, O., Hassan, A. et al. Alvogyl and absorbable gelatin sponge as palatal wound dressings following epithelialized free gingival graft harvest: a randomized clinical trial. Clin Oral Invest 24, 1517–1525 (2020). https://doi.org/10.1007/s00784-020-03254-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-020-03254-z