Abstract
Background
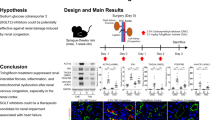
Upregulation of the sodium glucose co-transporter (SGLT2) is implicated in acute renal injury (ARI) progression and is regulated by extracellular signal-regulated kinase (ERK), hypoxia-inducible factor 1 alpha (HIF1α) or prostaglandin E2 (PGE2). This study aimed to assess the possible protective effect of nebivolol on renal ischemia/reperfusion (IR) and glycerol-induced ARI targeting SGLT2 via modulating the ERK–HIF1α pathway.
Methods
Rats were divided into control, sham, IR or nebivolol-treated group, in which rats were treated with nebivolol (10 mg/kg) for 3 days prior to the induction of IR. The rats were subjected to renal ischemia by bilateral clamping of the pedicles for 45 min, followed by 24 h reperfusion. Another group of rats received the vehicle or nebivolol (10 mg/kg) for 3 days followed by injection of 50% glycerol (8 ml/kg, IM) or saline. Kidney function tests, systolic blood pressure (SBP), oxidative stress markers [malondialdehyde (MDA) and NADPH oxidase] and kidney levels of nitric oxide (NO), inducible nitric oxide synthase (iNOS), HIF1α, ERK phosphorylation and PGE2 were determined. Additionally, renal sections were used for histological grading of renal injury and immunological expression of SGLT2.
Results
ARI rats showed significantly increased SBP, poor kidney function tests, increased oxidative stress, iNOS, NO, HIF1α levels, decreased PGE2 and ERK phosphorylation and upregulation of SGLT2 expression. Nebivolol treatment protected against the kidney damage both on the biochemical and histological levels.
Conclusion
Nebivolol has a direct renoprotective effect, at least in part, by down-regulating SGLT2 possibly via modulating HIF1α, ERK activity and PGE2 production.
Graphic abstract








Similar content being viewed by others
Abbreviations
- ANOVA:
-
One-way analysis of variance
- ARI:
-
Acute renal injury
- ERK:
-
Extracellular signal-regulated kinase
- eNOS:
-
Endothelial nitric oxide synthetase
- GFR:
-
Glomerular filtration rate
- GLY:
-
Glycerol
- HE:
-
Hematoxylin and eosin
- HIF1 α:
-
Hypoxia-inducible factor 1 alpha
- IHC:
-
Immunohistochemistry
- iNOS:
-
Inducible nitric oxide synthetase
- IR:
-
Ischemia/reperfusion
- MDA:
-
Malondialdehyde
- NADPH oxidase:
-
Nicotinamide adenine dinucleotide phosphate oxidase
- NO:
-
Nitric oxide
- PGE2:
-
Prostaglandin E2
- ROS:
-
Reactive oxygen species
- SBP:
-
Systolic blood pressure
- SEM:
-
Standard error of the mean
- SGLT2:
-
Sodium glucose co-transporter 2
References
Singh AP, Junemann A, Muthuraman A, Jaggi AS, Singh N, Grover K, et al. Animal models of acute renal failure. Pharmacol Rep. 2012;64:31–44.
Helmy MM, El-Gowelli HM. Montelukast abrogates rhabdomyolysis-induced acute renal failure via rectifying detrimental changes in antioxidant profile and systemic cytokines and apoptotic factors production. Eur J Pharmacol. 2012;683:294–300.
Panizo N, Rubio-Navarro A, Amaro-Villalobos JM, Egido J, Moreno JA. Molecular mechanisms and novel therapeutic approaches to rhabdomyolysis-induced acute kidney injury. Kidney Blood Press Res. 2015;40:520–32.
Gueler F, Gwinner W, Schwarz A, Haller H. Long-term effects of acute ischemia and reperfusion injury. Kidney Int. 2004;66:523–7.
Williams P, Lopez H, Britt D, Chan C, Ezrin A, Hottendorf R. Characterization of renal ischemia-reperfusion injury in rats. J Pharmacol Toxicol Methods. 1997;37:1–7.
Granger DN, Kvietys PR. Reperfusion injury and reactive oxygen species: the evolution of a concept. Redox Biol. 2015;6:524–51.
Villanueva S, Céspedes C, González AA, Vio CP, Velarde V. Effect of ischemic acute renal damage on the expression of COX-2 and oxidative stress-related elements in rat kidney. Am J Physiol Renal Physiol. 2007;292:F1364–71.
Weidemann A, Bernhardt WM, Klanke B, Daniel C, Buchholz B, Câmpean V, et al. HIF activation protects from acute kidney injury. J Am Soc Nephrol. 2008;19:486–94.
Minet E, Arnould T, Michel G, Roland I, Mottet D, Raes M, et al. ERK activation upon hypoxia: involvement in HIF-1 activation. FEBS Lett. 2000;468:53–8.
Hari Kishore A, Li XH, Word RA. Hypoxia and PGE(2) regulate MiTF-CX during cervical ripening. Mol Endocrinol. 2012;26:2031–45.
Haase VH. Hypoxia-inducible factors in the kidney. Am J Physiol Renal Physiol. 2006;291:F271–81.
Nasrallah R, Zimpelmann J, Eckert D, Ghossein J, Geddes S, Beique J-C, et al. PGE 2 EP 1 receptor inhibits vasopressin-dependent water reabsorption and sodium transport in mouse collecting duct. Lab Invest. 2018;98:360.
Layton AT, Vallon V, Edwards A. Predicted consequences of diabetes and SGLT inhibition on transport and oxygen consumption along a rat nephron. Am J Physiol Renal Physiol. 2016;310:F1269–83.
Panchapakesan U, Pegg K, Gross S, Komala MG, Mudaliar H, Forbes J, et al. Effects of SGLT2 inhibition in human kidney proximal tubular cells—renoprotection in diabetic nephropathy? PLoS One. 2013;8:e54442.
Maffei A, Lembo G. Nitric oxide mechanisms of nebivolol. Ther Adv Cardiovasc Dis. 2009;3:317–27.
Münzel T, Gori T. Nebivolol: the somewhat-different β-adrenergic receptor blocker. J Am Coll Cardiol. 2009;54:1491–9.
Hu T, Beattie WS, Mazer CD, Leong-Poi H, Fujii H, Wilson DF, et al. Treatment with a highly selective β1 antagonist causes dose-dependent impairment of cerebral perfusion after hemodilution in rats. Anesth Analg. 2013;116:649–62.
Zapata-Morales JR, Galicia-Cruz OG, Franco M, y Morales FM. Hypoxia-inducible factor-1α (HIF-1α) protein diminishes sodium glucose transport 1 (SGLT1) and SGLT2 protein expression in renal epithelial tubular cells (LLC-PK1) under hypoxia. J Biol Chem. 2014;289:346–57.
Georgescu A, Pluteanu F, Flonta M-L, Badila E, Dorobantu M, Popov D. The cellular mechanisms involved in the vasodilator effect of nebivolol on the renal artery. Eur J Pharmacol. 2005;508:159–66.
Chang Y-K, Choi H, Jeong JY, Na K-R, Lee KW, Lim BJ, et al. Dapagliflozin, SGLT2 inhibitor, attenuates renal ischemia-reperfusion injury. PLoS One. 2016;11:e0158810.
Wang Y, Zhang MS, Liu Y. Nebivolol treatment improves resistant arterial function and reduces ventricular hypertrophy and angiotensin II in spontaneously hypertension rats. J Renin Angiotensin Aldosterone Syst. 2013;14:146–55.
Singh D, Chander V, Chopra K. Protective effect of naringin, a bioflavonoid on glycerol-induced acute renal failure in rat kidney. Toxicology. 2004;201:143–51.
Paller MS, Hoidal J, Ferris TF. Oxygen free radicals in ischemic acute renal failure in the rat. J Clin Invest. 1984;74:1156–64.
Wei Q, Dong Z. Mouse model of ischemic acute kidney injury: technical notes and tricks. Am J Physiol Renal Physiol. 2012;303:F1487–94.
Sayhan MB, Kanter M, Oguz S, Erboga M. Protective effect of Urtica dioica L. on renal ischemia/reperfusion injury in rat. J Mol Histol. 2012;43:691–8.
Chander V, Singh D, Chopra K. Catechin, a natural antioxidant protects against rhabdomyolysis-induced myoglobinuric acute renal failure. Pharmacol Res. 2003;48:503–9.
Sorg DA, Buckner B. A simple method of obtaining venous blood from small laboratory animals. Proc Soc Exp Biol Med. 1964;115:1131–2.
Varghese F, Bukhari AB, Malhotra R, De A. IHC Profiler: an open source plugin for the quantitative evaluation and automated scoring of immunohistochemistry images of human tissue samples. PLoS One. 2014;9:e96801.
Hao Q, Xiao X, Zhen J, Feng J, Song C, Jiang B, et al. Resveratrol attenuates acute kidney injury by inhibiting death receptor-mediated apoptotic pathways in a cisplatin-induced rat model. Mol Med Rep. 2016;14:3683–9.
Kinsey GR, Sharma R, Huang L, Li L, Vergis AL, Ye H, et al. Regulatory T cells suppress innate immunity in kidney ischemia-reperfusion injury. J Am Soc Nephrol. 2009;20:1744–53.
Chatzizisis YS, Misirli G, Hatzitolios AI, Giannoglou GD. The syndrome of rhabdomyolysis: complications and treatment. Eur J Intern Med. 2008;19:568–74.
Oken D, Arce M, Wilson DR. Glycerol-induced hemoglobinuric acute renal failure in the rat. I. Micropuncture study of the development of oliguria. J Clin Invest. 1966;45:724–35.
Kobori H, Nangaku M, Navar LG, Nishiyama A. The intrarenal renin–angiotensin system: from physiology to the pathobiology of hypertension and kidney disease. Pharmacol Rev. 2007;59:251–87.
Greven J, Gabriëls G. Effect of nebivolol, a novel β1-selective adrenoceptor antagonist with vasodilating properties, on kidney function. Arzneimittelforschung. 2000;50:973–9.
Atwa A, Hegazy R, Shaffie N, Yassin N, Kenawy S. Protective effects of vasodilatory βeta-blockers carvedilol and nebivolol against glycerol model of rhabdomyolysis-induced acute renal failure in rats. Open Access Maced J Med Sci. 2016;4:329.
Youssef MI, Mahmoud AA, Abdelghany RH. A new combination of sitagliptin and furosemide protects against remote myocardial injury induced by renal ischemia/reperfusion in rats. Biochem Pharmacol. 2015;96:20–9.
Yu L, Gengaro PE, Niederberger M, Burke TJ, Schrier RW. Nitric oxide: a mediator in rat tubular hypoxia/reoxygenation injury. Proc Natl Acad Sci USA. 1994;91:1691–5.
Valdivielso J, Lopez-Novoa J, Eleno N, Barriocanal FP. Role of glomerular nitric oxide in glycerol-induced acute renal failure. Can J Physiol Pharmacol. 2000;78:476–82.
Beckman JS, Koppenol WH. Nitric oxide, superoxide, and peroxynitrite: the good, the bad, and ugly. Am J Physiol Cell Physiol. 1996;271:C1424–37.
Noiri E, Peresleni T, Miller F, Goligorsky MS. In vivo targeting of inducible NO synthase with oligodeoxynucleotides protects rat kidney against ischemia. J Clin Invest. 1996;97:2377–83.
Whaley-Connell A, Habibi J, Johnson M, Tilmon R, Rehmer N, Rehmer J, et al. Nebivolol reduces proteinuria and renal NADPH oxidase-generated reactive oxygen species in the transgenic Ren2 rat. Am J Nephrol. 2009;30:354–60.
Morsy MA, Heeba GH. Nebivolol ameliorates cisplatin-induced nephrotoxicity in rats. Basic Clin Pharmacol Toxicol. 2016;118:449–55.
Cominacini L, Pasini AF, Garbin U, Nava C, Davoli A, Criscuoli M, et al. Nebivolol and its 4-keto derivative increase nitric oxide in endothelial cells by reducing its oxidative inactivation. J Am Coll Cardiol. 2003;42:1838–44.
Yang C-C, Lin L-C, Wu M-S, Chien C-T, Lai M-K. Repetitive hypoxic preconditioning attenuates renal ischemia/reperfusion induced oxidative injury via upregulating HIF-1α-dependent bcl-2 signaling. Transplantation. 2009;88:1251–60.
Villanueva S, Céspedes C, Gonzalez A, Vio CP, Velarde V. Effect of ischemic acute renal damage on the expression of COX-2 and oxidative stress related elements in rat kidney. Am J Physiol Renal Physiol. 2007;292:F1364–71.
Pippin JW, Durvasula R, Petermann A, Hiromura K, Couser WG, Shankland SJ. DNA damage is a novel response to sublytic complement C5b-9-induced injury in podocytes. J Clin Invest. 2003;111:877–85.
Jang H-S, Han SJ, Kim JI, Lee S, Lipschutz JH, Park KM. Activation of ERK accelerates repair of renal tubular epithelial cells, whereas it inhibits progression of fibrosis following ischemia/reperfusion injury. Biochim Biophys Acta. 2013;1832:1998–2008.
El-Ashmawy NE, Khedr EG, El-Bahrawy HA, Selim HM. Nebivolol prevents indomethacin-induced gastric ulcer in rats. J Immunotoxicol. 2016;13:580–9.
Erickson CE, Gul R, Blessing CP, Nguyen J, Liu T, Pulakat L, et al. The β-blocker nebivolol is a GRK/β-arrestin biased agonist. PLoS One. 2013;8:e71980.
Nakamura N, Matsui T, Ishibashi Y, Yamagishi S-i. Insulin stimulates SGLT2-mediated tubular glucose absorption via oxidative stress generation. Diabetol Metab Syndr. 2015;7:48.
Kalra S, Singh V, Nagrale D. Sodium-glucose cotransporter-2 inhibition and the glomerulus: a review. Adv Ther. 2016;33:1502–18.
Funding
This work did not receive any funding from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest concerning this article.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Nasr, A.M., Rezq, S., Shaheen, A. et al. Renal protective effect of nebivolol in rat models of acute renal injury: role of sodium glucose co-transporter 2. Pharmacol. Rep 72, 956–968 (2020). https://doi.org/10.1007/s43440-020-00059-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s43440-020-00059-5