Abstract
Background
Patients with fibromyalgia syndrome (FMS) usually display a decrease in health-related quality of life (HRQoL). This decrease in HRQoL is related to clinical pain, anxiety, and depression. This cross-sectional study analyzes the mediating role of pain-coping strategies (especially catastrophizing) in the negative relationships of pain, anxiety, depression, and HRQoL in FMS.
Methods
One hundred and thirteen women with FMS and 63 healthy women were assessed using the Short-Form Health Survey (SF-36). Participants completed self-report questionnaires to evaluate clinical pain, anxiety, depression, and pain-coping strategies.
Results
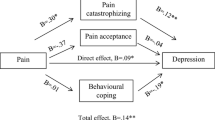
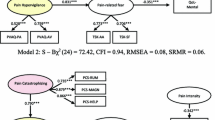
Pain catastrophizing was inversely associated with the physical function, general health perception, vitality, emotional role, mental health, the physical and mental general components, and the global index of HRQoL, with percentages of variance explained ranging between 9 and 18%. Cognitive distraction showed a positive association with the physical function, general health perception, vitality, emotional role, mental health, physical component, and global index of HRQoL, with percentages of variance explained ranging between 4 and 7%. Mediation analysis showed that catastrophizing mediates the negative influence of clinical pain and trait-anxiety on the physical function, general health perception, vitality, mental health, and global index of HRQoL. No mediating effect of pain catastrophizing on the relation between depression and HRQoL was observed.
Conclusions
Patients with FMS exhibited markedly lower HRQoL than healthy individuals. While pain catastrophizing was inversely related to several domains of HRQL, associations were positive for cognitive distraction. Catastrophizing mediates the negative influence of clinical pain and trait-anxiety on HRQoL. Therefore, cognitive behavioral treatments focused on adaptive management and control of catastrophizing and negative emotional states may be helpful.

Similar content being viewed by others
References
Wolfe, F., Smythe, H. A., Yunus, M. B., Bennett, R. M., Bombardier, C., Goldenberg, D. L., et al. (1990). The American College of Rheumatology 1990 Criteria for the Classification of Fibromyalgia. Arthritis & Rheumatism,33, 160–172. https://doi.org/10.1002/art.1780330203.
Galvez-Sánchez, C. M., Montoro, C. I., Duschek, S., & Reyes del Paso, G. A. (2019). Depression and trait-anxiety mediate the influence of clinical pain on health-related quality of life in fibromyalgia. Journal of Affective Disorders. https://doi.org/10.1016/j.jad.2020.01.129.
Jeong-Won, L., Kyung-Eun, L., Dong-Jin, P., Seong-Ho, K., Seong-Su, N., Ji-Hyun, L., et al. (2017). Determinants of quality of life in patients with fibromyalgia: A structural equation modeling approach. PLoS ONE,12, 1186–1199. https://doi.org/10.1371/journal.pone.0171186.
Perrot, S., Vicaut, E., Servant, D., & Ravaud, P. (2011). Prevalence of fibromyalgia in France: A multi-step study research combining national screening and clinical confirmation: The DEFI study (determination of epidemiology of fibromyalgia). BMC Musculoskeletal Disorder,12, 224–233. https://doi.org/10.1186/1471-2474-12-224.
Guyatt, G. H., Feeny, D. H., & Patrick, D. (1993). Measuring health-related quality of life. Annals of International Medicine,118, 622–629.
Jensen, M., Turner, J., Romano, J., & Karoly, P. (1991). Coping with chronic pain: A critical review of the literature. Pain,47, 249–283. https://doi.org/10.1016/0304-3959(91)90216-K.
Aparicio, A. V., Ortega, F. B., Carbonell-Baeza, A., Camiletti, D., Ruiz, J. R., & Delgado-Fernández, M. (2011). Relationship of weight status with mental and physical health in female fibromyalgia patients. Obesity Facts,6, 443–448. https://doi.org/10.1159/000335293.
Buskila, D., Neumann, L., Alhoashle, A., & Bu-Shakra, M. (2000). Fibromyalgia syndrome in men. Seminars in Arthritis and Rheumatism,30, 47–51. https://doi.org/10.1053/sarh.2000.8363.
Wolfe, F., Hawley, D. J., Goldenberg, D. L., Russell, I. J., Buskila, D., & Neumann, L. (2000). The assessment of functional impairment in fibromyalgia (FM): Rasch analyses of 5 functional scales and the development of the FM Health Assessment Questionnaire. Journal of Rheumatology,27, 1989–1999.
Andréll, P., Schultz, T., Mannerkorpi, K., Nordeman, L., Börjesson, M., & Mannheimer, C. (2014). Health-related quality of life in fibromyalgia and refractory angina pectoris: A comparison between two non-malignant pain disorders. Journal of Rehabilitation Medicine,46, 341–347. https://doi.org/10.2340/16501977-1279.
Cardona-Arias, J., León-Mira, V., & Cardona-Tapias, A. A. (2012). Calidad de vida relacionada con la salud en adultos con fibromialgia. Revista Colombiana de Reumatología,20, 19–29.
Branco, J. C., Rodrigues, A. M., Gouveia, N., Eusébio, M., Ramiro, S., Machado, P. M., et al. (2016). Prevalence of rheumatic and musculoskeletal diseases and their impact on health-related quality of life, physical function and mental health in Portugal: Results from EpiReumaPt—A national health survey. RMD Open,19, 166–176. https://doi.org/10.1136/rmdopen-2015-000166.
Brikman, S., Furer, V., Wollman, J., Borok, S., Matz, H., Polachek, A., et al. (2016). The effect of the presence of fibromyalgia on common clinical disease activity indices in patients with psoriatic arthritis: A cross-sectional study. Journal of Rheumatology,43, 49–54. https://doi.org/10.3899/jrheum.151491.
Turkyilmaz, A., Kurt, E. E., Karkucak, M., & Capkin, E. (2012). Sociodemographic characteristics, clinical signs and quality of life in patients with fibromyalgia. Eurasian Journal of Medicine,44, 88–93. https://doi.org/10.5152/eajm.2012.21.
Elli, A. (1962). Reason and emotion in psychotherapy. New York: Lyle Stuar.
Beck, A. T. (1987). Cognitive models of depression. Journal of Cognitive Psychotherapy,1, 5–37.
Sullivan, M. J., Thorn, B., Haythornthwaite, J. A., Keefe, F., Martin, M., Bradley, L. A., et al. (2001). Theoretical perspectives on the relation between catastrophizing and pain. Clinical Journal of Pain,17, 52–64.
Severeijns, R., Van den Hout, M. A., Vlaeyen, J. W. S., & Picavet, S. J. (2002). Pain catastrophizing and general health status in a large Dutch community sample. Pain,99, 367–376.
Sullivan, M. J. L., Bishop, S., & Pivik, J. (1995). The Pain Catastrophizing Scale: Development and validation. Psychological Assessment,7, 524–532.
Börsbo, B., Gerdle, B., & Peolsson, M. (2010). Impact of the interaction between self-efficacy, symptoms and catastrophizing on disability, quality of life and health in chronic pain patients. Disability and Rehabilitation,32, 1387–1396. https://doi.org/10.3109/09638280903419269.
Edwards, R. R., Haythornthwaite, J. A., Sullivan, M. J., & Fillingim, R. B. (2004). Catastrophizing as a mediator of sex differences in pain: Differential effects for daily pain versus laboratory-induced pain. Pain,111, 335–341.
García-Campayo, J., Rodero, B., Alda, M., Sobradiel, N., Montero, J., & Moreno, S. (2008). Validación de la versión española de la escala de la catastrofización ante el dolor en la fibromialgia. Medicina Clínica,131, 487–492.
Rodero, B., García-Campayo, J., Casanueva, B., & Buriel, Y. (2009). Tratamientos no farmacológicos en fibromialgia: Una revisión actual. Revista de Psicopatología Psicología Clínica,14, 137–151. https://doi.org/10.5944/rppc.vol.14.num.3.2009.4074.
Ovayolu, N., Ovayolu, O., & Karadag, G. (2011). Health-related quality of life in ankylosing spondylitis, fibromyalgia syndrome and rheumatoid arthritis: a comparison with a selected simple of healthy individuals. Clinical Rheumatology,30, 655–664. https://doi.org/10.1007/s10067-010-1604-2.
Keefe, F. J., Rumble, M. E., Scipio, C. D., Giordano, L. A., & Perri, L. M. (2004). Psychological aspects of persistent pain: Current state of the science. Journal of Pain,5, 195–211.
Peters, M. L., Vlaeyen, J. W., & van Drunen, C. (2000). Do fibromyalgia patients display hypervigilance for innocuous somatosensory stimuli? Application of a body scanning reaction time paradigm. Pain,86, 283–292.
Gracely, R. H., Petzke, F., Wolf, J. M., & Clauw, D. J. (2002). Functional magnetic resonance imaging evidence of augmented pain processing in fibromyalgia. Arthritis & Rheumatism,46, 1333–1343. https://doi.org/10.1002/art.10225.
Gracely, R. H., Geisser, M. E., Giesecke, T., Grant, M. A. B., Petzke, F., Williams, D. A., et al. (2004). Pain catastrophizing and neural responses to pain among persons with fibromyalgia. Brain,127, 835–843. https://doi.org/10.1093/brain/awh098.
Montoro Aguilar, C. I., Duschek, S., & Reyes del Paso, G. A. (2018). An exploratory analysis of the influence of personality and emotional factors on cerebral blood flow responses during painful stimulation in fibromyalgia. Scandinavian Journal of Psychology,59, 301–310. https://doi.org/10.1111/sjop.12434.
Edwards, R. R., Bingham, C. O., Bathon, J., & Haythornthwaite, J. A. (2006). Catastrophizing and pain in arthritis, fibromyalgia, and other rheumatic diseases. Arthritis & Rheumatism,55, 325–332.
Toth, C., Brady, S., & Hatfield, M. (2014). The importance of catastrophizing for successful pharmacological treatment of peripheral neuropathic pain. Journal of Pain Research,7, 327–338. https://doi.org/10.2147/JPR.S56883.
Van Wilgen, C. P., van Ittersum, M. W., Kaptein, A. A., & van Wijhe, M. (2008). Illness perceptions in patients with fibromyalgia and their relationship to quality of life and catastrophizing. Arthritis & Rheumatism,58, 3618–3626. https://doi.org/10.1002/art.23959.
Martin, M. Y., Bradley, L. A., Alexander, R. W., Alarcón, G. S., Triana-Alexander, M., Aaron, L. A., et al. (1996). Coping strategies predict disability in patients with primary fibromyalgia. Pain,68, 45–53. https://doi.org/10.1016/S0304-3959(96)03179-X.
Almansa, M. P., Sánchez, A. I., Miró, E., Medina, A., & Lami, M. J. (2011). The relationship between the fear-avoidance model of pain and personality traits in fibromyalgia patients. Journal of Clinical Psychology in Medical Settings,18, 380–391. https://doi.org/10.1007/s10880-011-9263-2.
Quartana, P. J., Campbell, C. M., & Edwards, R. R. (2009). Pain catastrophizing: A critical review. Expert Review of Neurotherapeutics,9, 745–758. https://doi.org/10.1586/ERN.09.34.
Burckhardt, C. S., Clark, S. R., O’Reilly, C. A., & Bennett, R. A. (1997). Pain-coping strategies of women with fibromyalgia: Relationship to pain, fatigue, and quality of life. Journal of Musculoskeletal Pain,5, 21–41. https://doi.org/10.1300/J094v05n03_02.
Radat, F., & Koleck, M. (2011). Pain and depression: Cognitive and behavioural mediators of a frequent association. Encephale,37, 172–179. https://doi.org/10.1016/j.encep.2010.08.013.
Raak, R., Hurtig, I., & Wahren, L. K. (2003). Coping strategies and life satisfaction in subgrouped fibromyalgia patients. Biological Research for Nursing,4, 93–202. https://doi.org/10.1177/1099800402239622.
Herken, H., Gursoy, S., Yetkin, O., Virit, O., & Esgi, K. (2001). Personality characteristics and depression levels in female patients with fibromyalgia syndrome. Journal of International Medicine,8, 41–44.
Houdenhove, B. V., & Luyten, P. (2006). Stress, depression and fibromyalgia. Acta Neurológica Bélgica,106, 149–156.
Montoro, C. I., & Reyes del Paso, G. A. (2015). Personality and fibromyalgia: Relationships with clinical, emotional, and functional variables. Personality and Individual Differences,85, 236–244. https://doi.org/10.1016/j.paid.2015.05.017.
Galvez-Sánchez, C. M., Reyes Del Paso, G. A., & Duschek, S. (2018). Cognitive impairments in fibromyalgia syndrome: Associations with positive and negative affect, alexithymia, pain catastrophizing and self-esteem. Frontiers in Psychology,22, 377. https://doi.org/10.3389/fpsyg.2018.00377.
Barsky, A. J., Wyshak, G., & Klerman, G. L. (1990). The somatosensory amplification scale and its relationship to hypochondriasis. Journal of Psychiatric Research,24, 323–334.
Taylor, S. S., Davis, M. C., Yeung, E. W., Zautra, A. J., & Tennen, H. A. (2017). Relations between adaptive and maladaptive pain cognitions and within-day pain exacerbations in individuals with fibromyalgia. Journal of Behavioral Medicine,40, 458–467.
Wolfe, F., Clauw, D. J., Fitzcharles, M. A., Goldenberg, D., Katz, R. S., Mease, P., et al. (2010). The American College of Rheumatology preliminary diagnostic criteria for fibromyalgia and measurement of symptom severity. Arthritis Care & Research,62, 600–610. https://doi.org/10.1002/acr.20140.
First, M., Spitzer, R. L., Gibbon, M., & Williams, J. B. W. (1999). Entrevista clínica estructurada para los trastornos del eje I del DSM-IV: SCIDI versión clínica. Barcelona: Madsson.
Ware, J. E., & Sherbourne, C. D. (1992). The MOS 36-item short-form health survey (SF-36). I. Conceptual framework and item selection. Medical Care,30, 473–483.
Alonso, J., Prieto, L., & Antó, J. M. (1995). La versión española del SF-36 Health Survey (Cuestionario de Salud SF-36): Un instrumento para la medida de los resultados clínicos. Medicina Clínica,104, 771–776.
Spielberger, C. D., Gorsuch, R., & Lushene, R. (1970). Manual for the State-Trait Anxiety Inventory. Palo Alto: Consulting Psychologist.
Spielberger, C. D., Gorsuch, R. L., & Lushene, R. E. (1982). Manual del Cuestionario de Ansiedad Estado/Rasgo (STAI). Madrid: TEA Ediciones.
Beck, A. T., Ward, C. H., & Mendelson, M. (1961). Inventory for measuring depression. Archives of General Psychiatry,4, 561–571. https://doi.org/10.1001/archpsyc.1961.01710120031004.
Vázquez, C., & Sanz, J. (1999). Fiabilidad y validez de la versión española del Inventario para la Depresión de Beck de 1978 en pacientes con trastornos psicológicos. Clínica y Salud,1, 59–81.
Melzack, R. (1975). The McGill pain questionnaire: Major properties and scoring methods. Pain,1, 277–299. https://doi.org/10.1016/0304-3959(75)90044-5.
Lázaro, C., Bosch, F., Torrubia, R., & Baños, J. E. (1994). The development of a Spanish questionnaire for assessing pain: Preliminary data concerning reliability and validity. European Journal of Psychological Assessment,10, 145–151.
Rosenstiel, A. K., & Keefe, F. J. (1983). The use of coping strategies in chronic low back pain patients: Relationship to patient characteristics and current adjustment. Pain,17, 33–44.
Rodriguez, L., Cano, E. J., & Blanco, A. (2004). Evaluación de las estrategias de afrontamiento de dolor crónico. Actas Españolas de Psiquiatría,32, 82–91.
Hair, J., Anderson, R., Tatham, R., & Black, W. (2000). Análisis multivariante. Madrid: Prentice Hall.
Preacher, K. J., & Hayes, A. F. (2004). SPSS and SAS procedures for estimating indirect effects in simple mediation models. Behavior Research Methods, Instruments, & Computers,36, 717–731.
Preacher, K. J., & Hayes, A. F. (2008). Asymptotic and resampling strategies for assessing and comparing indirect effects in multiple mediator models. Behavior Research Methods, Instruments, & Computers,40, 879–891.
Malin, K., & Littlejohn, G. (2012). Neuroticism in young women with fibromyalgia links to key clinical features. Pain Research and Treatment. https://doi.org/10.1155/2012/730741.
Geisser, M. E., & Roth, R. S. (1998). Knowledge of and agreement with pain diagnosis: Relation to pain beliefs, pain severity, disability, and psychological distress. Journal Occupational Rehabilitation,8, 73–88. https://doi.org/10.1023/A:1023060616201.
Geisser, M. E., Casey, K. L., Brucksch, C. B., Ribbens, C. M., Appleton, B. B., & Crofford, L. J. (2003). Perception of noxious and innocuous heat stimulation among healthy women and women with fibromyalgia: Association with mood, somatic focus, and catastrophizing. Pain,102, 243–250.
Watson, D., & Pennebaker, J. W. (1989). Health complaints, stress, and distress: Exploring the central role of negative affectivity. Psychological Review,96, 234–254.
Duschek, S., Mannhart, T., Winkelmann, A., Merzoug, K., Werner, N. S., Schuepbach, D., et al. (2012). Cerebral blood flow dynamics during pain processing in patients with fibromyalgia syndrome. Psychosomatic Medicine,74, 802–809. https://doi.org/10.1097/PSY.0b013e3182676d08.
Montoya, P., Pauli, P., Batra, A., & Wiedemann, G. (2005). Altered processing of pain-related information in patients with fibromyalgia. European Journal of Pain,9, 293–303.
Hassett, A. L., Cone, J. D., Patella, S. J., & Sigal, L. H. (2000). The role of catastrophizing in the pain and depression of women with fibromyalgia syndrome. Arthritis & Rheumatism,43, 2493–2500.
Rusu, A. C., & Hülsebusch, J. (2018). Cognitive bias research and depression in chronic pain. Schmerz,32, 236–242. https://doi.org/10.1007/s00482-018-0289-3.
Tellegen, A. (1985). Structures of mood and personality and their relevance to assessing anxiety, with an emphasis on self-report. In A. H. Turna & D. Maser (Eds.), Anxiety and the anxiety disorders (pp. 681–706). Hillsdale: ErIbaum.
Eysenck, M. W. (2013). Anxiety: The cognitive perspective. London: Psychology Press.
Michael, E. S., & Burns, J. W. (2004). Catastrophizing and pain sensitivity among chronic pain patients: Moderating effects of sensory and affect focus. Annals of Behavioral Medicine,27, 185–194. https://doi.org/10.1207/s15324796abm2703_6.
Kelley, G., Kelley, K., Hootman, J., & Jones, D. (2010). Exercise and global well-being in community-dwelling adults with fibromyalgia: A systematic review with meta-analysis. BMC Public Health,10, 198.
Alok, R., Das, S. K., Agarwal, G. G., Tiwari, S Ch, Salwahan, L., & Srivastava, R. (2014). Problem-focused coping and self-efficacy as correlates of quality of life and severity of fibromyalgia in primary fibromyalgia patients. Journal of Clinical Rheumatology,20, 314–316. https://doi.org/10.1371/journal.pone.0171186.
Biccheri, E., Roussiau, N., & Mambet-Doué, C. (2016). Fibromyalgia, spirituality, coping and quality of life. Journal of Religion & Health,55, 1189–1197.
Bernardy, K., Klose, P., Welsch, P., & Häuser, W. (2018). Efficacy, acceptability and safety of cognitive behavioral therapies in fibromyalgia syndrome: A systematic review and meta-analysis of randomized controlled trials. European Journal of Pain,22, 242–260. https://doi.org/10.1002/ejp.112.1.
Lazaridou, A., Kim, J., Cahalan, C. M., Loggia, M. L., Franceschelli, O., Berna, C., et al. (2017). Effects of cognitive-behavioral therapy (CBT) on brain connectivity supporting catastrophizing in fibromyalgia. Clinical Journal of Pain,33, 215–221. https://doi.org/10.1097/AJP.0000000000000422.
Luciano, J. V., D'Amico, F., Feliu-Soler, A., McCracken, L. M., Aguado, J., Peñarrubia-María, M. T., et al. (2017). Cost-utility of group acceptance and commitment therapy for fibromyalgia versus recommended drugs: an economic analysis alongside a 6-month randomized controlled trial conducted in Spain (EFFIGACT Study). Journal of Pain,18, 868–880. https://doi.org/10.1016/j.jpain.2017.03.001.
Simister, H. D., Tkachuk, G. A., Shay, B. L., Vincent, N., Pear, J. J., & Skrabek, R. Q. (2018). Randomized controlled trial of online acceptance and commitment therapy for fibromyalgia. Journal of Pain,S1526–5900, 30084–30091. https://doi.org/10.1016/j.jpain.2018.02.004.
Nelson, P. J., & Tucker, S. (2006). Developing an intervention to alter catastrophizing in persons with fibromyalgia. Journal of Orthopedic Nursing,25, 205–214.
Hernández-Petro, A., & Cardona-Arias, J. (2014). Sistematización de las investigaciones sobre calidad de vida relacionada con la salud en fibromialgia, 2004-2014. Archivos de Medicina,10, 22–34. https://doi.org/10.3823/1233.
Bernard, A. L., Prince, A., & Edsall, P. (2000). Quality of life issues for fibromyalgia patients. Arthritis Care & Research,13, 42–50.
Funding
This research was supported by a grant from the Spanish Ministry of Science and Innovation co-financed by FEDER funds (Project RTI2018-095830-B-I00) and a FPU pre-doctoral contract (ref: FPU2014-02808) from a grant from the Spanish Ministry of Education, Culture and Sport. The funding sources had no participate in the preparation of the article, the collection, analysis and interpretation of data; the writing of the article; nor in the decision to submit it for publication.
Author information
Authors and Affiliations
Contributions
CMGS conceived the original idea with GARP, contributed with the design of the experiments, carried out the experiment, analyzed the data and wrote the manuscript with support from GARP and SD. CIM contributed with the design of the experiments and analyzed the data. SD supervised the project, analyzed the data and contributed to the final version of the manuscript. GARP conceived the original idea with CMGS, designed the experiments, supervised the project, analyzed the data and contributed to the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
All the authors declare that they have no conflict of interest derived from the outcomes of this study.
Ethical approval
The study protocol was approved by the Ethics Committee for Human Research of the University of Jaén
Informed consent
All participants provided written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Galvez-Sánchez, C.M., Montoro, C.I., Duschek, S. et al. Pain catastrophizing mediates the negative influence of pain and trait-anxiety on health-related quality of life in fibromyalgia. Qual Life Res 29, 1871–1881 (2020). https://doi.org/10.1007/s11136-020-02457-x
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11136-020-02457-x