Abstract
This study examines the link between peripheral immune changes in perpetuation of the Alzheimer’s disease (AD) neuropathology and cognitive deficits. Our research design using human AD patients and rodent model is supported by past evidence from genomic studies. We observed an active immune response against Aβ as indicated by the increased Aβ specific IgG antibody in the serum of AD and patients with mild cognitive impairments as compared to healthy controls. A similar increase in IgG and decrease in IgM antibody against Aβ was also confirmed in the 5xFAD mouse model of AD. More importantly, we observed a negative correlation between reduced IgM levels and cognitive dysfunction that manifested as impaired memory consolidation. Strong peripheral immune activation was supported by increased activation of microglia in the brain and macrophages in the spleen of AD mice compared to wild type control littermates. Furthermore, inflammatory cytokine IL-21 that is involved in antibody class switching was elevated in the plasma of AD patients and correlated positively with the IgG antibody levels. Concurrently, an increase in IL-21 and IL-17 was observed in spleen cells from AD mice. Further investigation revealed that proportions of T follicular helper (Tfh) cells that secrete IL-21 are increased in the spleen of AD mice. In contrast to Tfh, the frequency of B1 cells that produce IgM antibodies was reduced in AD mice. Altogether, these data indicate that in AD the immune tolerance to Aβ is compromised leading to chronic immune/inflammatory responses against Aβ that are detrimental and cause neuropathology.

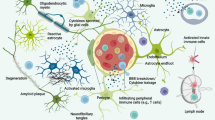
Healthy subjects are tolerant to Aβ and usually react weakly to it resulting the in the production of IgM class of antibodies that are efficient at clearing up self-antigens such as Aβ without causing inflammation. In contrast, Alzheimer’s disease patients mount a strong immune response against Aβ probably in an effort to clear up excessive Aβ. There is enhanced production of inflammatory cytokines such as IL-21 as well as an increase in Tfh cells that cause antibody class switching form IgM to IgG. The strong immune response is inefficient at clearing up Aβ and instead exacerbates inflammation that causes AD neuropathology and cognitive dysfunction.





Similar content being viewed by others
Data Availability
All relevant raw datasets analyzed during the current study are freely available from the corresponding author on reasonable request.
Abbreviations
- AD:
-
Alzheimer’s disease
- MCI:
-
Mild Cognitive Impairment
- HC:
-
Healthy Controls
- Aβ:
-
Amyloid beta
- APC:
-
Antigen presenting cells
- Tfh:
-
T follicular helper cells
- ADRC:
-
Alzheimer’s disease research center
- FE:
-
Fear Extinction
- CS:
-
conditioned stimulus
- PMA:
-
phorbol 12-myristate 13-acetate
- WT:
-
Wild type control mice
- CSF:
-
cerebrospinal fluid
- NMSOD:
-
Neuromyelitis Optica Spectrum Disorders
References
Acharya MM, Green KN, Allen BD, Najafi AR, Syage A, Minasyan H, le MT, Kawashita T, Giedzinski E, Parihar VK, West BL, Baulch JE, Limoli CL (2016) Elimination of microglia improves cognitive function following cranial irradiation. Sci Rep 6:31545. https://doi.org/10.1038/srep31545
Acharya MM et al. (2019) New concerns for neurocognitive function during deep space exposures to chronic, Low Dose-Rate, Neutron Radiation eNeuro 6 doi:https://doi.org/10.1523/ENEURO.0094-19.2019
Agrawal S, Abud EM, Snigdha S, Agrawal A (2018) IgM response against amyloid-beta in aging: a potential peripheral protective mechanism. Alzheimers Res Ther 10:81. https://doi.org/10.1186/s13195-018-0412-9
Banchereau J, Steinman RM (1998) Dendritic cells and the control of immunity. Nature 392:245–252. https://doi.org/10.1038/32588
Blanco P, Ueno H, Schmitt N (2016) T follicular helper (Tfh) cells in lupus: Activation and involvement in SLE pathogenesis. Eur J Immunol 46:281–290. https://doi.org/10.1002/eji.201545760
Cao W, Zheng H (2018) Peripheral immune system in aging and Alzheimer's disease. Mol Neurodegener 13:51. https://doi.org/10.1186/s13024-018-0284-2
Chang CH, Knapska E, Orsini CA, Rabinak CA, Zimmerman JM, Maren S (2009) Fear extinction in rodents Curr Protoc Neurosci chapter 8:Unit8 23 doi:https://doi.org/10.1002/0471142301.ns0823s47
Chen Y, Park YB, Patel E, Silverman GJ (2009) IgM antibodies to apoptosis-associated determinants recruit C1q and enhance dendritic cell phagocytosis of apoptotic cells. J Immunol 182:6031–6043. https://doi.org/10.4049/jimmunol.0804191
Clarkson BD, Ling C, Shi Y, Harris MG, Rayasam A, Sun D, Salamat MS, Kuchroo V, Lambris JD, Sandor M, Fabry Z (2014) T cell-derived interleukin (IL)-21 promotes brain injury following stroke in mice. J Exp Med 211:595–604. https://doi.org/10.1084/jem.20131377
Crotty S (2014) T follicular helper cell differentiation, function, and roles in disease. Immunity 41:529–542. https://doi.org/10.1016/j.immuni.2014.10.004
Elahi A, Sabui S, Narasappa NN, Agrawal S, Lambrecht NW, Agrawal A, Said HM (2018) Biotin deficiency induces Th1- and Th17-mediated Proinflammatory responses in human CD4(+) T lymphocytes via activation of the mTOR signaling pathway. J Immunol 200:2563–2570. https://doi.org/10.4049/jimmunol.1701200
Fan X, Jin T, Zhao S, Liu C, Han J, Jiang X, Jiang Y (2015) Circulating CCR7+ICOS+ memory T follicular helper cells in patients with multiple sclerosis. PLoS One 10:e0134523. https://doi.org/10.1371/journal.pone.0134523
Gaskin F, Finley J, Fang Q, Xu S, Fu SM (1993) Human antibodies reactive with beta-amyloid protein in Alzheimer's disease. J Exp Med 177:1181–1186. https://doi.org/10.1084/jem.177.4.1181
Gronwall C, Vas J, Silverman GJ (2012) Protective Roles of Natural IgM Antibodies. Front Immunol 3:66. https://doi.org/10.3389/fimmu.2012.00066
Heneka MT et al (2015a) Neuroinflammation in Alzheimer's disease. Lancet Neurol 14:388–405. https://doi.org/10.1016/S1474-4422(15)70016-5
Heneka MT, Golenbock DT, Latz E (2015b) Innate immunity in Alzheimer's disease. Nat Immunol 16:229–236. https://doi.org/10.1038/ni.3102
Heppner FL, Ransohoff RM, Becher B (2015) Immune attack: the role of inflammation in Alzheimer disease. Nat Rev Neurosci 16:358–372. https://doi.org/10.1038/nrn3880
King C, Tangye SG, Mackay CR (2008) T follicular helper (TFH) cells in normal and dysregulated immune responses. Annu Rev Immunol 26:741–766. https://doi.org/10.1146/annurev.immunol.26.021607.090344
Kishida T et al (2007) IL-21 induces inhibitor of differentiation 2 and leads to complete abrogation of anaphylaxis in mice. J Immunol 179:8554–8561
Li YJ et al (2015) Association of circulating follicular helper T cells with disease course of NMO spectrum disorders. J Neuroimmunol 278:239–246. https://doi.org/10.1016/j.jneuroim.2014.11.011
Mittal K et al (2019) CD4 T cells induce a subset of MHCII-expressing microglia that attenuates Alzheimer pathology. iScience 16:298–311. https://doi.org/10.1016/j.isci.2019.05.039
Monsonego A et al (2003) Increased T cell reactivity to amyloid beta protein in older humans and patients with Alzheimer disease. J Clin Invest 112:415–422. https://doi.org/10.1172/JCI18104
Montecino-Rodriguez E, Dorshkind K (2012) B-1 B cell development in the fetus and adult. Immunity 36:13–21. https://doi.org/10.1016/j.immuni.2011.11.017
Okada H, Khoury SJ (2012) Type17 T-cells in central nervous system autoimmunity and tumors. J Clin Immunol 32:802–808. https://doi.org/10.1007/s10875-012-9686-z
Prieto JMB, Felippe MJB (2017) Development, phenotype, and function of non-conventional B cells. Comp Immunol Microbiol Infect Dis 54:38–44. https://doi.org/10.1016/j.cimid.2017.08.002
Puli L, Tanila H, Relkin N (2014) Intravenous immunoglobulins for Alzheimer's disease. Curr Alzheimer Res 11:626–636
Puthenparampil M et al (2019) Peripheral imbalanced TFH/TFR ratio correlates with intrathecal IgG synthesis in multiple sclerosis at clinical onset. Mult Scler 25:918–926. https://doi.org/10.1177/1352458518779951
Qu BX et al (2014) Beta-amyloid auto-antibodies are reduced in Alzheimer's disease. J Neuroimmunol 274:168–173. https://doi.org/10.1016/j.jneuroim.2014.06.017
Recher M et al (2011) IL-21 is the primary common gamma chain-binding cytokine required for human B-cell differentiation in vivo. Blood 118:6824–6835. https://doi.org/10.1182/blood-2011-06-362533
Rothstein TL, Griffin DO, Holodick NE, Quach TD, Kaku H (2013) Human B-1 cells take the stage. Ann N Y Acad Sci 1285:97–114. https://doi.org/10.1111/nyas.12137
Sarra M, Pallone F, Macdonald TT, Monteleone G (2010) Targeting interleukin-21 in immune-mediated pathologies. Curr Drug Targets 11:645–649
Silverman GJ, Cary SP, Dwyer DC, Luo L, Wagenknecht R, Curtiss VE (2000) A B cell superantigen-induced persistent "hole" in the B-1 repertoire. J Exp Med 192:87–98
Sollvander S et al (2015) Increased number of plasma B cells producing autoantibodies against Abeta42 Protofibrils in Alzheimer's disease. J Alzheimers Dis 48:63–72. https://doi.org/10.3233/JAD-150236
Spolski R, Leonard WJ (2014) Interleukin-21: a double-edged sword with therapeutic potential. Nat Rev Drug Discov 13:379–395. https://doi.org/10.1038/nrd4296
Steinman RM (2012) Decisions about dendritic cells: past, present, and future. Annu Rev Immunol 30:1–22. https://doi.org/10.1146/annurev-immunol-100311-102839
Tangye SG (2015) Advances in IL-21 biology - enhancing our understanding of human disease. Curr Opin Immunol 34:107–115. https://doi.org/10.1016/j.coi.2015.02.010
Ueno H, Banchereau J, Vinuesa CG (2015) Pathophysiology of T follicular helper cells in humans and mice. Nat Immunol 16:142–152. https://doi.org/10.1038/ni.3054
Yang J et al. (2016) Critical roles of mTOR complex 1 and 2 for T follicular helper cell differentiation and germinal center responses Elife 5 doi:https://doi.org/10.7554/eLife.17936
Zhang J, Ke KF, Liu Z, Qiu YH, Peng YP (2013) Th17 cell-mediated neuroinflammation is involved in neurodegeneration of abeta1-42-induced Alzheimer's disease model rats. PLoS One 8:e75786. https://doi.org/10.1371/journal.pone.0075786
Acknowledgements
We are grateful to UCI-ADRC for providing the serum samples from AD, MCI patients and controls.
Funding
The project described was supported by AG045216, AG064709 to A.A. and the California Institute for Regenerative Medicine DISC1–10079 to J.E.B. The UCI-ADRC is funded by NIH/NIA Grant P50 AG16573. The content is solely the responsibility of the authors and does not necessarily represent the official views of the NIH.
Author information
Authors and Affiliations
Contributions
J.E.B. maintained the 5xFAD mouse colony and performed molecular analyses and analyzed data. M.A.A. performed mice behavior experiments, analyzed data and prepared Figs. L.A.A. performed mouse behavior experiments. C.M. helped with processing of mouse tissues for staining. S.A. performed the human serum experiments and flow cytometry of mice cells. A.A. designed the study, analyzed the data, prepared the figures and wrote the manuscript. All authors were involved in discussions and writing of manuscript.
Corresponding author
Ethics declarations
Conflict of Interests
The authors declare that they have no competing interests.
Ethics Approval and Consent to Participate
All procedures performed in studies involving human participants were in accordance with the ethical standards of the University of California Irvine Institutional Research Board and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards. Since deidentified human serum samples were obtained from ADRC, the research was considered non-human subjects by UCI-IRB. Informed consent from subjects was obtained by ADRC.
Mice
All animal experimentation procedures were performed in accordance with the guidelines provided by NIH and approved by the University of California Irvine Institutional Animal Care and Use Committee.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Supplementary figure 1
The number of dense core Aβ-plaques increase with age in 5xFAD mice. (A-C) Representative images of Thio-S staining for WT and AD mice qualitatively demonstrate early disease pathology as shown by the accumulation of plaques by 4 months of age in the basal lateral amygdala and increases at 8 months of age (BLA; 20 × confocal imaging). Dot blot of the quantitative analysis of plaque number demonstrate the advancing AD pathology reflected by gross increase in plaque number in the AD brain between 4 and 8 months of age. All data are presented as mean + SEM (n = 4 mice per group). P values are derived from Student’s t test. (PNG 662 kb)
Rights and permissions
About this article
Cite this article
Baulch, J.E., Acharya, M.M., Agrawal, S. et al. Immune and Inflammatory Determinants Underlying Alzheimer’s Disease Pathology. J Neuroimmune Pharmacol 15, 852–862 (2020). https://doi.org/10.1007/s11481-020-09908-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11481-020-09908-9