Abstract
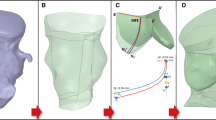
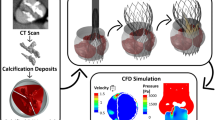
Bicuspid aortic valve (BAV) anatomy has routinely been considered an exclusion in the setting of transcatheter aortic valve implantation (TAVI) because of the large dimension of the aortic annulus having a more calcified, bulky, and irregular shape. The study aims to develop a patient-specific computational framework to virtually simulate TAVI in stenotic BAV patients using the Edwards SAPIEN 3 valve (S3) and its improved version SAPIEN 3 Ultra and quantify stent frame deformity as well as the severity of paravalvular leakage (PVL). Specifically, the aortic root anatomy of n.9 BAV patients who underwent TAVI was reconstructed from pre-operative CT imaging. Crimping and deployment of S3 frame were performed and then followed by fluid-solid interaction analysis to simulate valve leaflet dynamics throughout the entire cardiac cycle. Modeling revealed that the S3 stent frame expanded well on BAV anatomy with an elliptical shape at the aortic annulus. Comparison of predicted S3 deformity as assessed by eccentricity and expansion indices demonstrated a good agreement with the measurement obtained from CT imaging. Blood particle flow analysis demonstrated a backward blood jet during diastole, whereas the predicted PVL flows corresponded well with those determined by transesophageal echocardiography. This study represents a further step towards the use of personalized simulations to virtually plan TAVI, aiming at improving not only the efficacy of the implantation but also the exploration of “off-label” applications as the TAVI in the setting of BAV patients.

Computational frameworks of TAVI in patients with stenotic bicuspid aortic valve









Similar content being viewed by others
References
Arai T, Lefevre T, Hovasse T, Morice MC, Romano M, Benamer H, Garot P, Hayashida K, Bouvier E, Chevalier B (2017) The feasibility of transcatheter aortic valve implantation using the Edwards SAPIEN 3 for patients with severe bicuspid aortic stenosis. J Cardiol 70:220–224. https://doi.org/10.1016/j.jjcc.2016.12.009
Auricchio F, Conti M, Morganti S, Reali A (2014) Simulation of transcatheter aortic valve implantation: a patient-specific finite element approach. Comput Methods Biomech Biomed Eng 17:1347–1357. https://doi.org/10.1080/10255842.2012.746676
Bailey J, Curzen N, Bressloff NW (2016) Assessing the impact of including leaflets in the simulation of TAVI deployment into a patient-specific aortic root. Comput Methods Biomech Biomed Eng 19:733–744. https://doi.org/10.1080/10255842.2015.1058928
Bianchi M, Marom G, Ghosh RP, Rotman OM, Parikh P, Gruberg L, Bluestein D (2019) Patient-specific simulation of transcatheter aortic valve replacement: impact of deployment options on paravalvular leakage. Biomech Model Mechanobiol 18:435–451. https://doi.org/10.1007/s10237-018-1094-8
Binder RK, Rodes-Cabau J, Wood DA, Mok M, Leipsic J, De Larochelliere R, Toggweiler S, Dumont E, Freeman M, Willson AB, Webb JG (2013) Transcatheter aortic valve replacement with the SAPIEN 3: a new balloon-expandable transcatheter heart valve. JACC Cardiovasc Interven 6:293–300. https://doi.org/10.1016/j.jcin.2012.09.019
Brouwer J, Gheorghe L, Nijenhuis VJ, Ten Berg JM, Rensing B, van der Heyden JAS, Swaans MJ (2018) Insight on patient specific computer modeling of transcatheter aortic valve implantation in patients with bicuspid aortic valve disease. Catheter Cardiovasc Interv. https://doi.org/10.1002/ccd.27990
Caballero A, Mao W, Liang L, Oshinski J, Primiano C, McKay R, Kodali S, Sun W (2017) Modeling left ventricular blood flow using smoothed particle hydrodynamics. Cardiovasc Eng Technol 8:465–479. https://doi.org/10.1007/s13239-017-0324-z
D'Ancona G, Amaducci A, Rinaudo A, Pasta S, Follis F, Pilato M, Baglini R (2013) Haemodynamic predictors of a penetrating atherosclerotic ulcer rupture using fluid-structure interaction analysis. Interact Cardiovasc Thorac Surg 17:576–578. https://doi.org/10.1093/icvts/ivt245
Eker A, Sozzi FB, Civaia F, Bourlon F (2012) Aortic annulus rupture during transcatheter aortic valve implantation: safe aortic root replacement. Eur J Cardiothorac Surg 41:1205. https://doi.org/10.1093/ejcts/ezr146
Ewe SH, Ng AC, Schuijf JD, van der Kley F, Colli A, Palmen M, de Weger A, Marsan NA, Holman ER, de Roos A, Schalij MJ, Bax JJ, Delgado V (2011) Location and severity of aortic valve calcium and implications for aortic regurgitation after transcatheter aortic valve implantation. Am J Cardiol 108:1470–1477. https://doi.org/10.1016/j.amjcard.2011.07.007
Fedak PW, Verma S, David TE, Leask RL, Weisel RD, Butany J (2002) Clinical and pathophysiological implications of a bicuspid aortic valve. Circulation 106:900–904
Finotello A, Morganti S, Auricchio F (2017) Finite element analysis of TAVI: impact of native aortic root computational modeling strategies on simulation outcomes. Med Eng Phys 47:2–12. https://doi.org/10.1016/j.medengphy.2017.06.045
Rinaudo A, D'Ancona G, Lee JJ, (...), Pilato M, Pasta S Predicting Outcome of Aortic Dissection with Patent False Lumen by Computational Flow Analysis Cardiovascular Engineering and Technology, 2014, 5(2), pp. 176–188. https://doi.org/10.1007/s13239-014-0182-x
Gandolfo C, Turrisi M, Follis F, Clemenza F, Falletta C, Gentile G, Liotta R, Raffa GM, Pilato M (2018) Acute obstructive thrombosis of Sapien 3 valve after valve-in-valve transcatheter aortic valve replacement for degenerated mosaic 21 valve. JACC Cardiovasc Interven 11:215–217. https://doi.org/10.1016/j.jcin.2017.08.054
Gnyaneshwar R, Kumar RK, Balakrishnan KR (2002) Dynamic analysis of the aortic valve using a finite element model. Ann Thorac Surg 73:1122–1129
Hayashida K, Bouvier E, Lefevre T, Chevalier B, Hovasse T, Romano M, Garot P, Watanabe Y, Farge A, Donzeau-Gouge P, Cormier B, Morice MC (2013) Transcatheter aortic valve implantation for patients with severe bicuspid aortic valve stenosis. Circ-Cardiovasc Interven 6:284–291. https://doi.org/10.1161/Circinterventions.112.000084
Kappetein AP, Head SJ, Genereux P, Piazza N, van Mieghem NM, Blackstone EH, Brott TG, Cohen DJ, Cutlip DE, van Es GA, Hahn RT, Kirtane AJ, Krucoff MW, Kodali S, Mack MJ, Mehran R, Rodes-Cabau J, Vranckx P, Webb JG, Windecker S, Serruys PW, Leon MB, Valve Academic Research C (2012) Updated standardized endpoint definitions for transcatheter aortic valve implantation: the Valve Academic Research Consortium-2 consensus document. EuroIntervention 8:782–795. https://doi.org/10.4244/EIJV8I7A121
Kawamori H, Yoon SH, Chakravarty T, Maeno Y, Kashif M, Israr S, Abramowitz Y, Mangat G, Miyasaka M, Rami T, Kazuno Y, Takahashi N, Jilaihawi H, Nakamura M, Cheng W, Friedman J, Berman D, Sharma R, Makkar RR (2018) Computed tomography characteristics of the aortic valve and the geometry of SAPIEN 3 transcatheter heart valve in patients with bicuspid aortic valve disease. Eur Heart J Cardiovasc Imaging 19:1408–1418. https://doi.org/10.1093/ehjci/jex333
Kleinstreuer C, Li Z, Basciano CA, Seelecke S, Farber MA (2008) Computational mechanics of Nitinol stent grafts. J Biomech 41:2370–2378. https://doi.org/10.1016/j.jbiomech.2008.05.032
Kong WK, Delgado V, Poh KK, Regeer MV, Ng AC, McCormack L, Yeo TC, Shanks M, Parent S, Enache R, Popescu BA, Liang M, Yip JW, Ma LC, Kamperidis V, van Rosendael PJ, van der Velde ET, Ajmone Marsan N, Bax JJ (2017) Prognostic implications of raphe in bicuspid aortic valve anatomy. JAMA Cardiol 2:285–292. https://doi.org/10.1001/jamacardio.2016.5228
Lavon K, Marom G, Bianchi M, Halevi R, Hamdan A, Morany A, Raanani E, Bluestein D, Haj-Ali R (2019) Biomechanical modeling of transcatheter aortic valve replacement in a stenotic bicuspid aortic valve: deployments and paravalvular leakage. Med Biol Eng Comput 57:2129–2143. https://doi.org/10.1007/s11517-019-02012-y
Lee JJ, D'Ancona G, Amaducci A, Follis F, Pilato M, Pasta S (2014) Role of computational modeling in thoracic aortic pathology: a review. J Card Surg 29:653–662. https://doi.org/10.1111/jocs.12413
Leon MB, Smith CR, Mack M, Miller DC, Moses JW, Svensson LG, Tuzcu EM, Webb JG, Fontana GP, Makkar RR, Brown DL, Block PC, Guyton RA, Pichard AD, Bavaria JE, Herrmann HC, Douglas PS, Petersen JL, Akin JJ, Anderson WN, Wang D, Pocock S, Investigators PT (2010) Transcatheter aortic-valve implantation for aortic stenosis in patients who cannot undergo surgery. N Engl J Med 363:1597–1607. https://doi.org/10.1056/NEJMoa1008232
Luraghi G, Migliavacca F, Garcia-Gonzalez A, Chiastra C, Rossi A, Cao D, Stefanini G, Rodriguez Matas JF (2019) On the modeling of patient-specific transcatheter aortic valve replacement: a fluid-structure interaction approach. Cardiovasc Eng Technol 10:437–455. https://doi.org/10.1007/s13239-019-00427-0
Mao W, Li K, Sun W (2016) Fluid-structure interaction study of transcatheter aortic valve dynamics using smoothed particle hydrodynamics. Cardiovasc Eng Technol 7:374–388. https://doi.org/10.1007/s13239-016-0285-7
Mao W, Caballero A, McKay R, Primiano C, Sun W (2017) Fully-coupled fluid-structure interaction simulation of the aortic and mitral valves in a realistic 3D left ventricle model. PLoS One 12:e0184729. https://doi.org/10.1371/journal.pone.0184729
Mao W, Wang Q, Kodali S, Sun W (2018) Numerical parametric study of paravalvular leak following a transcatheter aortic valve deployment into a patient-specific aortic root. J Biomech Eng 140. https://doi.org/10.1115/1.4040457
Marwan M, Achenbach S, Ensminger SM, Pflederer T, Ropers D, Ludwig J, Weyand M, Daniel WG, Arnold M (2013) CT predictors of post-procedural aortic regurgitation in patients referred for transcatheter aortic valve implantation: an analysis of 105 patients. Int J Cardiovasc Imaging 29:1191–1198. https://doi.org/10.1007/s10554-013-0197-7
Monaghan J (2012) Smoothed particle hydrodynamics and its diverse applications. Annu Rev Fluid Mech 44:323–346
Morganti S, Conti M, Aiello M, Valentini A, Mazzola A, Reali A, Auricchio F (2014) Simulation of transcatheter aortic valve implantation through patient-specific finite element analysis: two clinical cases. J Biomech 47:2547–2555. https://doi.org/10.1016/j.jbiomech.2014.06.007
Morganti S, Brambilla N, Petronio AS, Reali A, Bedogni F, Auricchio F (2016) Prediction of patient-specific post-operative outcomes of TAVI procedure: the impact of the positioning strategy on valve performance. J Biomech 49:2513–2519. https://doi.org/10.1016/j.jbiomech.2015.10.048
Morlacchi S, Chiastra C, Gastaldi D, Pennati G, Dubini G, Migliavacca F (2011) Sequential structural and fluid dynamic numerical simulations of a stented bifurcated coronary artery. J Biomech Eng 133:121010. https://doi.org/10.1115/1.4005476
Mylotte D, Lefevre T, Watanabe Y, Sondergaard L, Windecker S, Bosmans J, Tchetche D, Kornowski R, Modine T, Sinning JM, O'Sullivan C, Barbanti M, Codner P, Dorfmeister M, Martucci J, Wenaweser P, Tamburino C, Grube E, Webb J, Lange R, Piazza N (2014) Transcatheter aortic valve replacement in bicuspid aortic valve disease. J Am Coll Cardiol 63:A1939–A1939
Pasta S, Phillippi JA, Tsamis A, D'Amore A, Raffa GM, Pilato M, Scardulla C, Watkins SC, Wagner WR, Gleason TG, Vorp DA (2016) Constitutive modeling of ascending thoracic aortic aneurysms using microstructural parameters. Med Eng Phys 38:121–130. https://doi.org/10.1016/j.medengphy.2015.11.001
Pasta S, Gentile G, Raffa GM, Scardulla F, Bellavia D, Luca A, Pilato M, Scardulla C (2017) Three-dimensional parametric modeling of bicuspid aortopathy and comparison with computational flow predictions. Artif Organs 41:E92–E102. https://doi.org/10.1111/aor.12866
Perlman GY, Blanke P, Dvir D, Pache G, Modine T, Barbanti M, Holy EW, Treede H, Ruile P, Neumann FJ, Gandolfo C, Saia F, Tamburino C, Mak G, Thompson C, Wood D, Leipsic J, Webb JG (2016) Bicuspid aortic valve stenosis: favorable early outcomes with a next-generation transcatheter heart valve in a multicenter study. JACC Cardiovasc Interven 9:817–824. https://doi.org/10.1016/j.jcin.2016.01.002
Roberts WC, Janning KG, Ko JM, Filardo G, Matter GJ (2012) Frequency of congenitally bicuspid aortic valves in patients >/=80 years of age undergoing aortic valve replacement for aortic stenosis (with or without aortic regurgitation) and implications for transcatheter aortic valve implantation. Am J Cardiol 109:1632–1636. https://doi.org/10.1016/j.amjcard.2012.01.390
Sannino A, Cedars A, Stoler RC, Szerlip M, Mack MJ, Grayburn PA (2017) Comparison of efficacy and safety of transcatheter aortic valve implantation in patients with bicuspid versus tricuspid aortic valves. Am J Cardiol 120:1601–1606. https://doi.org/10.1016/j.amjcard.2017.07.053
Sievers HH, Schmidtke C (2007) A classification system for the bicuspid aortic valve from 304 surgical specimens. J Thorac Cardiovasc Surg 133:1226–1233. https://doi.org/10.1016/j.jtcvs.2007.01.039
Sturla F, Ronzoni M, Vitali M, Dimasi A, Vismara R, Preston-Maher G, Burriesci G, Votta E, Redaelli A (2016) Impact of different aortic valve calcification patterns on the outcome of transcatheter aortic valve implantation: a finite element study. J Biomech 49:2520–2530. https://doi.org/10.1016/j.jbiomech.2016.03.036
Ward C (2000) Clinical significance of the bicuspid aortic valve. Heart 83:81–85
Wijesinghe N, Ye J, Rodes-Cabau J, Cheung A, Velianou JL, Natarajan MK, Dumont E, Nietlispach F, Gurvitch R, Wood DA, Tay E, Webb JG (2010) Transcatheter aortic valve implantation in patients with bicuspid aortic valve stenosis. JACC Cardiovasc Interven 3:1122–1125. https://doi.org/10.1016/j.jcin.2010.08.016
Xiong FL, Goetz WA, Chong CK, Chua YL, Pfeifer S, Wintermantel E, Yeo JH (2010) Finite element investigation of stentless pericardial aortic valves: relevance of leaflet geometry. Ann Biomed Eng 38:1908–1918. https://doi.org/10.1007/s10439-010-9940-6
Yoon SH, Bleiziffer S, De Backer O, Delgado V, Arai T, Ziegelmueller J, Barbanti M, Sharma R, Perlman GY, Khalique OK, Holy EW, Saraf S, Deuschl F, Fujita B, Ruile P, Neumann FJ, Pache G, Takahashi M, Kaneko H, Schmidt T, Ohno Y, Schofer N, Kong WKF, Tay E, Sugiyama D, Kawamori H, Maeno Y, Abramowitz Y, Chakravarty T, Nakamura M, Kuwata S, Yong G, Kao HL, Lee M, Kim HS, Modine T, Wong SC, Bedgoni F, Testa L, Teiger E, Butter C, Ensminger SM, Schaefer U, Dvir D, Blanke P, Leipsic J, Nietlispach F, Abdel-Wahab M, Chevalier B, Tamburino C, Hildick-Smith D, Whisenant BK, Park SJ, Colombo A, Latib A, Kodali SK, Bax JJ, Sondergaard L, Webb JG, Lefevre T, Leon MB, Makkar R (2017) Outcomes in transcatheter aortic valve replacement for bicuspid versus tricuspid aortic valve stenosis. J Am Coll Cardiol 69:2579–2589. https://doi.org/10.1016/j.jacc.2017.03.017
Zhao ZG, Jilaihawi H, Feng Y, Chen M (2015) Transcatheter aortic valve implantation in bicuspid anatomy. Nat Rev Cardiol 12:123–128. https://doi.org/10.1038/nrcardio.2014.161
Funding
This work was supported by a “Ricerca Finalizzata” grant from the Italian Ministry of Health (GR-2011-02348129) to Salvatore Pasta.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(AVI 5314 kb)
Rights and permissions
About this article
Cite this article
Pasta, S., Cannata, S., Gentile, G. et al. Simulation study of transcatheter heart valve implantation in patients with stenotic bicuspid aortic valve. Med Biol Eng Comput 58, 815–829 (2020). https://doi.org/10.1007/s11517-020-02138-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11517-020-02138-4