Abstract
Purpose
This study aimed to assess the reliability of rectal villous tumors staging between rectal MRI and histological examination used as the Gold Standard and to investigate causes for discrepancies.
Methods
The rectal 1.5 T MR scans of 40 patients followed for a histologically proven rectal villous adenoma were retrospectively included. Two independent experienced radiologists staged each tumor according to the TNM classification and described the occurrence of retraction of the rectal wall or spiculations within the associated mesorectum. A third radiologist collected tumor’s morphological characteristics.
Results
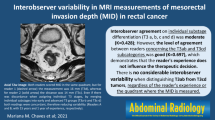
Among the 40 villous tumors studied, 25 (63%) were non-invasive and 15 (37%) were invasive. The mean volume of tumors with spiculations and retraction was significantly greater (p < 0.05) compared to tumors without these characteristics. Spiculations and retraction of the rectal wall were observed regardless of the definitive histological stage and did not represent a malignancy criterion. A weak interobserver reliability [Gwet’s AC2: 0.31 (0.04–0.57)] in T-staging was observed between the two readers. Reader 1 showed a high reliability [Gwet’s AC2: 0.90 (0.81–0.99)] in T-staging between Histopathological examination and preoperative MRI. In the opposite, reader 2 showed a weak reliability [Gwet’s AC2: 0.31 (0.03–0.58)] in T-staging. He overstaged all tumors (100%) with spiculations (p < 0.05).
Conclusion
MRI understaged rectal villous adenoma and was unable to detect degenerative criteria, along with slight Interobserver agreement. The typical worrisome signs of rectal tumor, such as retractions and spiculations, occurred in all stages and were responsible for misstaging in most cases, in particular bulky tumors.







Similar content being viewed by others
References
Haute Autorité de Santé - Dépistage et prévention du cancer colorectal, (2019). https://www.has-sante.fr/portail/jcms/c_1623732/fr/depistage-et-prevention-du-cancer-colorectal (accessed June 25, 2019).
M. Gschwantler, S. Kriwanek, E. Langner, B. Göritzer, C. Schrutka-Kölbl, E. Brownstone, H. Feichtinger, W. Weiss, High-grade dysplasia and invasive carcinoma in colorectal adenomas: a multivariate analysis of the impact of adenoma and patient characteristics, Eur. J. Gastroenterol. Hepatol. 14 (2002) 183–188.
E.R. Bresnihan, K.C. Simpkins, Villous adenoma of the large bowel; benign and malignant, Br. J. Radiol. 48 (1975) 801–806. doi: 10.1259/0007-1285-48-574-801.
P.M. Madsen, O. Braendstrup, Carcinoma recti. The predictive value of diagnostic biopsies for histologic grading, Dis. Colon Rectum. 28 (1985) 676–677.
S.C. Nahas, A.R. Imperiale, S.E. Araújo, A.A. Aisaka, C.W. Sobrado Júnior, A. Habr-Gama, H.W. Pinotti, [Villous and tubulovillous adenomas of the colon and rectum. Results in 30 patients], Rev. Hosp. Clin. 53 (1998) 162–168.
N.A. Ahmad, M.L. Kochman, G.G. Ginsberg, Endoscopic ultrasound and endoscopic mucosal resection for rectal cancers and villous adenomas, Hematol. Oncol. Clin. North Am. 16 (2002) 897–906. doi: 10.1016/S0889-8588(02)00038-2.
K. Konishi, Y. Akita, K. Kaneko, T. Kurahashi, T. Yamamoto, S. Kusayanagi, N. Yoshikawa, N. Miyasaka, H. Tajiri, K. Mitamura, Evaluation of endoscopic ultrasonography in colorectal villous lesions, Int. J. Colorectal Dis. 18 (2003) 19–24. doi: 10.1007/s00384-002-0423-6.
M. De Vargas Macciucca, A. Casale, L. Manganaro, I. Floriani, F. Fiore, L. Marchetti, G. Panzironi, Rectal villous tumours: MR features and correlation with TRUS in the preoperative evaluation, Eur. J. Radiol. 73 (2010) 329–333. https://doi.org/10.1016/j.ejrad.2008.11.026.
M. Zappa, L. Raynaud, C. Bertin, L. Maggiori, Y. Panis, V. Vilgrain, MR imaging of villous rectal tumours in the era of transanal endoscopic microsurgery, (2017). https://posterng.netkey.at/esr/viewing/index.php?module=viewing_poster&task=viewsection&pi=137807&ti=469706&si=1639&searchkey= (accessed June 24, 2019).
J.-F. Fléjou, Classification OMS 2010 des tumeurs digestives : la quatrième édition,/data/revues/02426498/v31i5sS/S0242649811001775/. (2011). https://www.em-consulte.com/en/article/675515#N1022C (accessed October 21, 2019).
R. Kikuchi, M. Takano, K. Takagi, N. Fujimoto, R. Nozaki, T. Fujiyoshi, Y. Uchida, Management of early invasive colorectal cancer. Risk of recurrence and clinical guidelines, Dis. Colon Rectum. 38 (1995) 1286–1295.
C. Klessen, P. Rogalla, M. Taupitz, Local staging of rectal cancer: the current role of MRI, Eur. Radiol. 17 (2007) 379–389. doi: 10.1007/s00330-006-0388-x.
P.J. Brown, R. Hyland, A.J. Quyn, N.P. West, D. Sebag-Montefiore, D. Jayne, P. Sagar, D.J. Tolan, Current concepts in imaging for local staging of advanced rectal cancer, Clin. Radiol. (2019). doi: 10.1016/j.crad.2019.03.023.
N. Hayashi, S. Tanaka, D.G. Hewett, T.R. Kaltenbach, Y. Sano, T. Ponchon, B.P. Saunders, D.K. Rex, R.M. Soetikno, Endoscopic prediction of deep submucosal invasive carcinoma: validation of the Narrow-Band Imaging International Colorectal Endoscopic (NICE) classification, Gastrointest. Endosc. 78 (2013) 625–632. doi: 10.1016/j.gie.2013.04.185.
The Paris endoscopic classification of superficial neoplastic lesions: esophagus, stomach, and colon: November 30 to December 1, 2002. - PubMed - NCBI, (2019). https://www.ncbi.nlm.nih.gov/pubmed/14652541 (accessed June 26, 2019).
M. Ferlitsch, A. Moss, C. Hassan, P. Bhandari, J.-M. Dumonceau, G. Paspatis, R. Jover, C. Langner, M. Bronzwaer, K. Nalankilli, P. Fockens, R. Hazzan, I.M. Gralnek, M. Gschwantler, E. Waldmann, P. Jeschek, D. Penz, D. Heresbach, L. Moons, A. Lemmers, K. Paraskeva, J. Pohl, T. Ponchon, J. Regula, A. Repici, M.D. Rutter, N.G. Burgess, M.J. Bourke, Colorectal polypectomy and endoscopic mucosal resection (EMR): European Society of Gastrointestinal Endoscopy (ESGE) Clinical Guideline, Endoscopy. 49 (2017) 270–297. doi: 10.1055/s-0043-102569.
P. Pimentel-Nunes, M. Dinis-Ribeiro, T. Ponchon, A. Repici, M. Vieth, A. De Ceglie, A. Amato, F. Berr, P. Bhandari, A. Bialek, M. Conio, J. Haringsma, C. Langner, S. Meisner, H. Messmann, M. Morino, H. Neuhaus, H. Piessevaux, M. Rugge, B. Saunders, M. Robaszkiewicz, S. Seewald, S. Kashin, J.-M. Dumonceau, C. Hassan, P. Deprez, Endoscopic submucosal dissection: European Society of Gastrointestinal Endoscopy (ESGE) Guideline, Endoscopy. 47 (2015) 829–854. doi: 10.1055/s-0034-1392882.
J. Fleshman, M. Branda, D.J. Sargent, A.M. Boller, V. George, M. Abbas, W.R. Peters, D. Maun, G. Chang, A. Herline, A. Fichera, M. Mutch, S. Wexner, M. Whiteford, J. Marks, E. Birnbaum, D. Margolin, D. Larson, P. Marcello, M. Posner, T. Read, J. Monson, S.M. Wren, P.W.T. Pisters, H. Nelson, Effect of Laparoscopic-Assisted Resection vs Open Resection of Stage II or III Rectal Cancer on Pathologic Outcomes: The ACOSOG Z6051 Randomized Clinical Trial, JAMA. 314 (2015) 1346. doi: 10.1001/jama.2015.10529.
F. Glaser, P. Schlag, C. Herfarth, Endorectal ultrasonography for the assessment of invasion of rectal tumours and lymph node involvement, Br. J. Surg. 77 (1990) 883–887. doi: 10.1002/bjs.1800770813.
M.S. Absar, N.Y. Haboubi, Colonic neoplastic polyps: biopsy is not efficient to exclude malignancy. The Trafford experience, Tech. Coloproctology. 8 Suppl 2 (2004) s257-260. https://doi.org/10.1007/s10151-004-0172-3.
A. Pikarsky, S. Wexner, P. Lebensart, J. Efron, E. Weiss, J. Nogueras, P. Reissman, The use of rectal ultrasound for the correct diagnosis and treatment of rectal villous tumors, Am. J. Surg. 179 (2000) 261–265. doi: 10.1016/s0002-9610(00)00328-7.
Histologic grade of metastatic lymph node and prognosis of rectal cancer. - PubMed - NCBI, (n.d.). https://www.ncbi.nlm.nih.gov/pubmed/11052477 (accessed October 28, 2019).
P. Videhult, K. Smedh, P. Lundin, W. Kraaz, Magnetic resonance imaging for preoperative staging of rectal cancer in clinical practice: high accuracy in predicting circumferential margin with clinical benefit, Colorectal Dis. 9 (2007) 412–419. Doi : 10.1111/j.1463-1318.2006.01167.x.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by CV, Prof VL and RT. The first draft of the manuscript was written by CV and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
The studies have been approved by the appropriate institutional and/or national research ethics committee and have been performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards. A declaration was made to the National Commission on Information Technology and Civil Liberties (CNIL) and registered under CNIL number 2019PI073.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Vogrig, C., Leclerc, J., Haghnejad, V. et al. Reliability in villous tumors staging between preoperative MRI and histopathological examination. Abdom Radiol 45, 3046–3056 (2020). https://doi.org/10.1007/s00261-020-02450-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00261-020-02450-5