Abstract
Endoscopic resection techniques, such as endoscopic mucosal resection (EMR) and endoscopic submucosal dissection (ESD), are frequently aided by injection of submucosal lifting solutions that create a plane for dissection and protect deeper mural layers. ORISE™ gel is a recently approved synthetic lifting solution that produces a localized inflammatory reaction associated with retained gel at the injection site. We describe a series of six cases of ORISE™-associated inflammatory lesions in patients who underwent endoscopic resections. Deposits comprised pale fibrillary or hyalinized eosinophilic material, depending on their age. All cases were associated with an inflammatory reaction composed of foreign-body giant cells and scattered eosinophils. ORISE™ gel extended laterally and deeply beyond residual tumors in all cases. Histochemically, the material proved to be negative for Congo Red, and mucicarmine, faint blue with Alcian blue, but positive for PAS and PAS-D. It stained blue with trichrome. Such deposits were absent in cases, wherein other widely-available lifting solutions were used. We compared ORISE™ deposits to histologically similar extracellular deposits, namely amyloid and pulse granulomata. Unlike ORISE™ material, amyloid deposits appear as waxy, more densely eosinophilic material, and stain positive with Congo Red. Amyloid demonstrated prominent intramucosal and perivascular distributions, features not seen in this series of ORISE™ deposits. Hyalinized pulse granulomata showed strong overlap with ORISE™ deposits, since they also comprise eosinophilic material associated with giant cell reaction. On the other hand, they form ribbons of glassy material in circumscribed lobules, unlike the ill-defined ORISE™ deposits. In summary, we describe the pathologic findings at injection sites in patients who underwent endoscopic procedures aided by the recently approved lifting agent, ORISE™. Pathologists should be aware of its appearance and associated reaction to avoid confusion with other common extracellular deposits seen in the gastrointestinal tract.
Similar content being viewed by others
Introduction
Endoscopic techniques are increasingly employed as alternatives to colectomy for removal of colonic adenomas and superficially invasive adenocarcinomas [1, 2]. Pedunculated adenomas, including those that harbor superficially invasive adenocarcinoma, and small (≤10–15 mm) sessile adenomas, are amenable to complete removal via snare polypectomy with or without the use of diathermy [3]. Flat or sessile polyps and laterally growing tumors that span ≥15 mm are more challenging to remove and often require the use of advanced techniques, including endoscopic mucosal resection (EMR) and endoscopic submucosal dissection (ESD) [2, 4, 5]. Complete resection with clear margins constitutes definitive therapy for non-invasive neoplasms and for adenocarcinomas with low risk of lymph node metastasis [6]. Thus, the goal of endoscopic resection is to completely remove tumors en bloc to allow for accurate diagnosis, assessment of margins, and staging of adenocarcinoma, when present. This can be achieved via EMR for most lesions <20 mm and for some larger tumors, but EMR may result in piecemeal resection of invasive or large tumors, which compromises histologic evaluation. ESD is an alternative to surgery, in these cases. It allows for the submucosa to be lifted off of the muscularis propria, producing a deeper plane for dissection and en bloc removal [7]. EMR and ESD rely on the injection of submucosal lifting solutions to expand the submucosal space and create a cushion that protects the muscularis propria [8, 9]. In general, the use of submucosal lifting solutions is recommended for polyps >1.5 cm, especially if located in the proximal colon where the wall is thinner [4].
Ideally, a fluid cushion should last for the duration of a procedure without altering tissue architecture or compromising histologic examination [1, 9, 10]. Common agents, such as saline and dextrose, are inexpensive and nontoxic, but dissipate quickly, and must be injected multiple times to complete procedures [1, 8, 9]. Need for repeated injections increases procedure time and risk of bleeding or perforation [4, 8,9,10]. Higher viscosity agents, such as glycerol, hyaluronic acid, and succinylated gelatin, have been developed to increase elevation time while decreasing total procedure time. For example, Eleview™ is a commonly used premixed, sterile, and synthetic solution designed to increase efficiency of EMR and ESD procedures [4, 5, 8, 9]. It contains water, sodium chloride, poloxamer 188 (bulking and structural agent), polyoxyl-15-hydroxystearate (emulsifier), and medium-chain triglycerides (oil component) [9].
ORISE™ gel is a newer premixed synthetic solution from Boston Scientific (MA, USA), with similar composition to Eleview™, recently approved by the Food and Drug Administration for use in submucosal injection throughout the gastrointestinal tract [9, 11]. We have recently noticed that patients who undergo ORISE™ gel injection during EMR develop localized, mass-forming inflammatory reactions associated with retained foreign material at the injection site. In this series, we describe the clinical and pathologic features of six cases of ORISETM-associated mural response in patients with incompletely resected colonic neoplasms.
Materials and methods
Case selection
Six cases from patients who underwent colonic resection after attempted EMR aided by ORISE™ injection were prospectively identified during routine signout for inclusion in the study. Resection specimens from patients who underwent prior EMR with injection of other submucosal lifting solutions were retrieved for comparison. Cases with amyloid deposits and pulse granulomata were also studied for comparison. The latter were included due to their histologic similarity to ORISE™ deposits. Clinical data were derived from the electronic medical records.
Histologic evaluation
Biopsy and resection specimens were reviewed at the originating institutions. The mural layers involved, localization and morphology of deposits, and nature of the inflammatory reaction were recorded in study and comparison cases with extracellular deposits. Tumors were classified and staged according to current World Health Organization and American Joint Committee on Cancer criteria, respectively [12, 13].
Results
Clinical and pathologic features of endoscopic submucosal resection cases
The clinical and pathologic features of study cases are summarized in Table 1. Study cases included three men and three women with a mean age of 61 years. EMRs were attempted for sessile polyps ranging from 2.5 to 10 cm. In all cases, endoscopists noted inadequate lifting in portions of the polyp when ORISE™ was injected; thus, ESD was not attempted, and the decision was made to perform piecemeal EMR to obtain diagnostic tissue with the expectation that a surgical resection would ensue. Resection specimens revealed either residual adenoma (n = 4), invasive adenocarcinoma (n = 1), or no residual tumor (n = 1). The interval between endoscopic and surgical procedures ranged from 3 to 19 weeks.
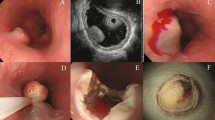
The appearance of the deposits correlated with the time interval between ORISE™ injections and resections. Cases 2, 4, and 5 (Table 1), resected after 5-, 5-, and 3-week intervals, respectively, featured pale fibrillary material resembling mucin (Fig. 1a, b), and in cases 2 and 5, the foreign-body giant cell reaction was decreased compared with other cases in the series. In contrast, cases 1, 3, and 6 (Table 1), resected between 9 and 19 weeks after ORISETM injection, featured dense eosinophilic material with exuberant foreign-body giant cells (Fig. 1c) and scattered eosinophils. ORISETM material in case 1, which was injected 19 weeks prior to resection, featured cracking artifact, similar to that typically seen in amyloid (Fig. 2a). In case 5, ORISETM deposits accounted for a majority of the grossly perceived residual tumor. In all cases, ORISETM deposits extended beyond the residual neoplasm. Resections performed after EMR for similar indications (Table 2), using other common lifting solutions (Eleview™, saline), lacked any of these features.
The material produces an ill-defined expansile submucosal mass associated with giant cell reaction at the periphery (arrow) (a). The material is faintly eosinophilic, acellular, and fibrillary in this case (b). Older deposits are more dense and eosinophilic. They contained a more prominent inflammatory reaction, comprising predominantly giant cells and eosinophils, at the periphery and within the deposits (c). ORISETM in subserosal tissue, in one case, was associated with reactive mesothelial changes in the serosa (arrow) (d).
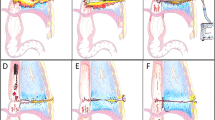
ORISETM material (a) raised concern for amyloidosis, due to its eosinophilic appearance and cracking artifact, but was negative for Congo Red (b). It stained faint blue with Alcian blue (c) and faint pink with mucicarmine (d). Trichrome stains imparted a blue appearance (e). The deposits were PAS-positive (not shown) and diastase resistant (f).
Histochemical stains were performed on cases detected earlier in the study period, in an attempt to clarify the nature of the extracellular deposits. Once the association with ORISETM injection was established, the diagnosis was made based on clinical history. Deposits were negative for Congo Red (Fig. 2b). They showed faint blue staining with Alcian blue (Fig. 2c) and a faint pink hue with mucicarmine stains (Fig. 2d). They stained blue with trichrome (Fig. 2e). They were PAS-positive and diastase resistant (Fig. 2f), possibly due to the presence of polymers with hydroxyl groups within the compound.
Clinical and pathologic features of amyloidosis cases
Two resection specimens that contained amyloid deposits were identified. One patient had renal failure and underwent resection for ischemic colitis that proved to be due to extensive vascular amyloid deposits. The other underwent resection of a gastrointestinal stromal tumor, and amyloid was found incidentally upon histologic examination (Fig. 3). Important distinctions (Table 3) from ORISETM include prominent intramucosal and perivascular distribution of amyloid. Amyloid is more densely eosinophilic and displays more prominent “cracking” artifact. Positive Congo Red stains support the diagnosis of amyloidosis.
Amyloid deposits in the colonic lamina propria appear as chunky eosinophilic material with artifactual cracks. The deposits are more hyalinized and opaque than ORISETM residue (a). Amyloid is distributed primarily in the blood vessel walls in this segment of the ischemic bowel from a patient with renal failure (b). The amyloid is Congo Red positive (c) and shows apple green birefringence when polarized (d).
Clinical and pathologic features of pulse granuloma cases
Pulse granulomata were detected in a background of diverticulitis in two cases in this series (Table 3). They appeared as ribbons of hyalinized material associated with giant cells (Fig. 4) in the immediate vicinity of diverticula. They were confined to the muscularis propria and subserosa, and were closely associated with blood vessels in one case, but unlike amyloid, they did not directly involve vessel walls.
Discussion
Herein, we describe a series of ORISE™ gel-associated mural reactions in patients who underwent EMR and surgical resection for treatment of preinvasive or superficially invasive colonic neoplasms. In our experience, the deposits and inflammatory response can form endoscopically- and surgically-apparent masses. Deposits resected within a few weeks of injection appear as pale fibrillary material that resembles mucin. Those left in situ for months are eosinophilic and associated with numerous foreign-body giant cells and eosinophils. They may extend as far as the subserosa, simulating a transmurally invasive tumor. The ORISETM material, which is PAS-D positive and Congo Red negative, shows faint mucicarmine and Alcian blue staining. It appears blue with trichrome stains.
Two other case series have described histologic features of ORISETM deposits [14, 15]. Similarly to those reports, we found that the material becomes hyalinized and more eosinophilic over time. However, since all of the cases in our series were resection specimens, we did not observe the bubbly appearance or prominent hemorrhage reported by others in specimens taken minutes after the injection. The cases in our series displayed a similar histochemical profile to that described by Westbrook et al. in cases examined 2 or more months post injection. Interestingly, in that work, ORISETM was reported to be positive for mucicarmine and negative for PAS and PAS-D immediately after injection. Since we did not review any cases resected within a similarly short interval, we did not observe this phenomenon; however, very faint mucicarmine staining was present in our cases. This implies that histologic appearance and histochemical properties of ORISETM evolve once injected into the gastrointestinal tract. Pezhouh et al. additionally found ORISETM to be nonreactive for Movat, GMS, iron, von Kossa, and colloidal iron. Similarly to Westbrook et al. and Pezhouh et al., we did not observe ORISETM in the mucosa. We also did not find ORISETM material in EMR specimens in our series. We note that one case reported by Pezhouh et al. did contain the deposits in a polypectomy specimen. We also understand that others have subsequently observed ORISETM material in EMR specimens (Dr. Ashwini Esnakula, personal communication). We observed that EleviewTM was not histologically detectable in EMR or resection specimens. This is in keeping with the observation by Pezhouh et al. that the material does not survive histologic processing. On the other hand, these authors reported that EleviewTM appears similar to ORISETM in a polypectomy specimen taken 1 day after injection. Our cases that were lifted with EleviewTM were resected between four and 10 weeks after injection. We speculate that the difference in time intervals accounts for the discrepancy in our findings and theirs.
We compared the features of ORISETM deposits to similar-appearing extracellular material, including amyloid and pulse granulomata, in order to better define its features and aid its recognition in biopsy and resection specimens. Amyloidosis of various etiologies, including plasma cell neoplasms, chronic inflammatory conditions, kidney failure, and hereditary defects in protein folding, may involve the gastrointestinal tract [16, 17]. Amyloid may deposit in any layer of the intestinal wall, and deposits are usually asymptomatic. On the other hand, substantial deposition in tissue in and around blood vessels in the colon and small intestine leads to ischemia [18]. Although amyloid deposits are usually segmental or diffuse, localized, mass-forming deposits are well described in the gastrointestinal tract [19]. All forms are morphologically identical and appear as waxy, eosinophilic extracellular material with artifactual “cracks”. The material stains positive with Congo Red and displays “apple green birefringence” when polarized. It is weakly PAS-positive. Amyloid is more densely eosinophilic than ORISETM material. It frequently shows perivascular distribution or deposition within vessel walls. Amyloid can deposit within the intestinal mucosa, a feature not seen in this series of ORISETM deposits. Moreover, ORISETM is Congo Red negative and PAS-D positive. Similarly to ORISETM deposits, amyloid may be associated with a foreign-body giant cell reaction. We also observed one case from an elderly patient who was lost to follow-up for nearly 5 months after ORISETM injection; these deposits did display artifactual “cracks”. This may be a feature of older ORISETM residue that enhances its histologic overlap with amyloid.
Pulse or hyaline ring granulomata are extracellular deposits of dense, eosinophilic hyaline material arranged in rings or ribbons and associated with multinucleated giant cells. They form in the oral mucosa, lungs, and gastrointestinal tract. They have been reported in the stomach, small intestine, colorectum, appendix, and gallbladder [20,21,22,23,24]. While their etiology is not entirely clear, some propose that they represent a granulomatous response to partially digested vegetables or legumes introduced through mucosal tears [25]. This would explain why they are frequently identified in a background of perforated diverticulitis [25]. Ultrastructural studies have also shown vegetable material within pulse granulomata. Others suggest that it is caused by hyaline degenerative changes of damaged blood vessels [25, 26]. It is possible that both of these theories are correct, since pulse granulomata display a spectrum of morphologic findings that may reflect differing etiologies. They are well-described mimickers in the gastrointestinal tract, because of their tumefactive nature and histologic overlap with amyloidosis [20, 23]. However, pulse granulomata tend to be more cellular, and their eosinophilic material is always negative for Congo Red and PAS. The hyaline material in pulse granulomata lacks internal cracks that are usually present in amyloid. ORISETM-associated deposits exhibit the strongest overlap with hyalinized pulse granulomata, and the association of both entities with giant cell reaction makes the overlap more striking.
The newly-introduced submucosal lifting agent, ORISETM, may persist at injection sites long after EMR or ESD. Indeed, deposits may distribute laterally and deeply beyond the histologic extent of residual tumor, and produce the gross impression of a more advanced lesion. Histologically, the deposits may simulate amyloid or pulse granulomata. Ancillary stains, including Congo Red and PAS-D, may help in the differential diagnosis. It is expedient for pathologists to be aware of the histologic features of ORISETM deposits and the associated reaction so that they may obtain clinical history to properly classify this finding.
References
Hwang JH, Konda V, Abu Dayyeh BK, Chauhan SS, Enestvedt BK, Fujii-Lau LL, et al. Endoscopic mucosal resection. Gastrointest Endosc 2015;82:215–26.
Kantsevoy SV, Adler DG, Conway JD, Diehl DL, Farraye FA, Kwon R, et al. Endoscopic mucosal resection and endoscopic submucosal dissection. Gastrointest Endosc 2008;68:11–18.
Ferlitsch M, Moss A, Hassan C, Bhandari P, Dumonceau JM, Paspatis G, et al. Colorectal polypectomy and endoscopic mucosal resection (EMR): European Society of Gastrointestinal Endoscopy (ESGE) clinical guideline. Endoscopy 2017;49:270–97.
Burke C, Kaul V, Pohl H. Polyp resection and removal procedures: insights from the 2017 digestive disease week. Gastroenterol Hepatol (NY). 2017;13 Suppl 2:1–24.
Wallace MB. New strategies to improve polypectomy during colonoscopy. Gastroenterol Hepatol (NY). 2017;13(10 Suppl 3):1–12.
Vogel JD, Eskicioglu C, Weiser MR, Feingold DL, Steele SR. The American Society of colon and rectal surgeons clinical practice guidelines for the treatment of colon cancer. Dis Colon Rectum. 2017;60:999–1017.
Holmes I, Friedland S. Endoscopic mucosal resection versus endoscopic submucosal dissection for large polyps: a western colonoscopist’s view. Clin Endosc 2016;49:454–6.
Johnson DA, Wallace MB, Kaul V, Kaltenbach T. Incomplete resection rates in polyps smaller than 2 centimeters. Proceedings from a live clinical roundtable held during digestive disease week. Gastroenterol Hepatol (NY). 2018;14 Suppl 5:1–19.
Castro R, Libânio D, Pita I, Dinis-Ribeiro M. Solutions for submucosal injection: what to choose and how to do it. World J Gastroenterol. 2019;25:777–88.
Ferreira AO, Moleiro J, Torres J, Dinis-Ribeiro M. Solutions for submucosal injection in endoscopic resection: a systematic review and meta-analysis. Endosc Int Open. 2016;4:E1–E16.
ORISE™. ORISE™ Gel. Gel Submucosal Lifting Agent. Boston Scientific Corporation. 2019 https://www.bostonscientific.com/content/gwc/en-US/products/lifting-agents/orise-gel.html.
World Health Organization (WHO). Classification of tumours editorial board. Digestive system tumours. 5th ed. Lyon, France: International Agency for Research on Cancer; 2019. p. 635.
Amin MB, Edge S, Greene F, Byrd DR, Brookland RK, Washington MK, et al. AJCC cancer staging manual. 8th ed. New York: Springer International Publishing; 2017.
Westbrook LM, Henn PA, Cornish TC. Lifting agent granuloma. Am J Clin Pathol. 2019. pii: aqz204. https://doi.org/10.1093/ajcp/aqz204. [Epub ahead of print].
Pezhouh MK, Burgart LJ, Chiu K, Cohen DA, Hutchings DA, Sanderson SO, et al. Characterization of novel injectable lifting agents used in colonic polyp removal: an emerging amyloid mimic. Am J Surg Pathol. 2020. https://doi.org/10.1097/PAS.0000000000001435. [Epub ahead of print].
Iida T, Yamano H, Nakase H. Systemic amyloidosis with gastrointestinal involvement: diagnosis from endoscopic and histological views. J Gastroenterol Hepatol. 2018;33:583–90.
Sipe JD, Benson MD, Buxbaum JN, Ikeda S, Merlini G, Saraiva MJ, et al. Nomenclature 2014: amyloid fibril proteins and clinical classification of the amyloidosis. Amyloid. 2014;21:221–4.
Freudenthaler S, Hegenbart U, Schönland S, Behrens HM, Krüger S, Röcken C. Amyloid in biopsies of the gastrointestinal tract-a retrospective observational study on 542 patients. Virchows Arch. 2016;468:569–77.
Oyasiji T, Yood S. Jejunal amyloidoma—a rare cause of gastrointestinal bleeding. Cases J 2009;2:9100.
Nowacki NB, Arnold MA, Frankel WL, Harzman A, Limketkai BN, Yearsley MM, et al. Gastrointestinal tract-derived pulse granulomata: clues to an underrecognized pseudotumor. Am J Surg Pathol. 2015;39:84–92.
Gonzalez RS. Incidence of pulse granuloma in the small and large intestines. Am J Surg Pathol. 2016;40:137–40.
Ban S, Fujii A, Takimoto T, Kikuchi K, Kang W, Namiki Y, et al. Pulse granulomas in interval appendectomy specimens: histochemical identification of cellulose matter. Case Rep Gastroenterol. 2018;12:765–72.
Deroche TC, Gates GA, Huber AR. Pulse granulomas of the gastrointestinal tract and gallbladder: report of five cases. Case Rep Pathol. 2017;2017:2497945.
Gupta A, Lyapichev K, Rojas CP. Pulse granuloma of the rectum: an unusual entity. Histopathology. 2016;68:938–9.
Philipsen HP, Reichart PA. Pulse or hyaline ring granuloma. Review of the literature on etiopathogenesis of oral and extraoral lesions. Clin Oral Investig. 2010;14:121–8.
Kotrashetti VS, Angadi PV, Mane DR, Hallikerimath SR. Oral pulse granuloma associated with keratocystic odontogenic tumor: report of a case and review on etiopathogenesis. Ann Maxillofac Surg. 2011;1:83–6.
Acknowledgements
The authors wish to thank Katherine E. Tanaka, MD for her critical review of the revised manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Castrodad-Rodríguez, C.A., Panarelli, N.C., Gersten, A.J. et al. Features of endoscopic procedure site reaction associated with a recently approved submucosal lifting agent. Mod Pathol 33, 1581–1588 (2020). https://doi.org/10.1038/s41379-020-0509-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41379-020-0509-0
This article is cited by
-
Submucosal lifting agent ORISE gel causes extensive foreign body granuloma post endoscopic resection
International Journal of Colorectal Disease (2021)