Abstract
Purpose
The aim of this study is to determine whether there is a relationship between radiographic slip progression and symptomatic worsening after decompression without fusion for low-grade degenerative lumbar spondylolisthesis (DLS).
Methods
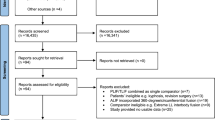
A retrospective review of 1–2-level minimally invasive surgical decompression for grade I–II DLS was performed. Included subjects had a minimum of 1-year follow-up with prospectively collected baseline and follow-up Oswestry Disability Index (ODI) scores.
Results
Fifty-six patients (33 females, 58.9%), having a mean age 65.6 years (SD 10.0), met inclusion criteria. Spondylolisthesis slip percentage increased in 55.4% (31/56) of patients. Slip percentage increased significantly (p = 0.002) from baseline (mean 17.2; SD 8.0) to follow-up (mean 20.1; SD 9.6). A logistic regression model identified that females were more likely to have progressive slips compared to males (odd ratio 6.09, 95% CI 1.77–21.01; p = 0.004). ODI scores and spondylolisthesis slip percentage did not correlate at baseline (r = 0.0170; p = 0.90) nor follow-up (r = 0.094; p = 0.49). There was no correlation between the change in ODI scores and change in slip percentage from baseline to final follow-up (r = 0.0474; p = 0.73). Of the 31 patients with slip progression, there was no difference in mean ODI score changes (p = 0.91) for those with 1–5% progression (13/31 [41.9%]; − 18.0 [SD 19.7]) compared to those with > 5% slip progression (18/31 [58.1%]; − 18.7 [SD 16.4]).
Conclusions
Despite a small degree of slip progression in the majority of patients, there was no correlation with symptom worsening, as measured by the ODI.
Graphic abstract
These slides can be retrieved under Electronic Supplementary Material.


Similar content being viewed by others
References
Herkowitz HN, Kurz LT (1991) Degenerative lumbar spondylolisthesis with spinal stenosis. A prospective study comparing decompression with decompression and intertransverse process arthrodesis. J Bone Joint Surg Am 73:802–808
Bridwell KH, Sedgewick TA, O’Brien MF et al (1993) The role of fusion and instrumentation in the treatment of degenerative spondylolisthesis with spinal stenosis. J Spinal Disord 6:461–472
Försth P, Ólafsson G, Carlsson T et al (2016) A randomized, controlled trial of fusion surgery for lumbar spinal stenosis. N Engl J Med 374:1413–1423. https://doi.org/10.1056/NEJMoa1513721
Ghogawala Z, Dziura J, Butler WE et al (2016) Laminectomy plus fusion versus laminectomy alone for lumbar spondylolisthesis. N Engl J Med 374:1424–1434. https://doi.org/10.1056/NEJMoa1508788
Chang HS, Fujisawa N, Tsuchiya T et al (2014) Degenerative spondylolisthesis does not affect the outcome of unilateral laminotomy with bilateral decompression in patients with lumbar stenosis. Spine 39:400–408. https://doi.org/10.1097/BRS.0000000000000161
Rampersaud YR, Fisher C, Yee A et al (2014) Health-related quality of life following decompression compared to decompression and fusion for degenerative lumbar spondylolisthesis: a Canadian multicentre study. Can J Surg J Can Chir 57:E126–E133
Kelleher MO, Timlin M, Persaud O, Rampersaud YR (2010) Success and failure of minimally invasive decompression for focal lumbar spinal stenosis in patients with and without deformity. Spine 35:E981–E987. https://doi.org/10.1097/BRS.0b013e3181c46fb4
Müslüman AM, Cansever T, Yılmaz A et al (2012) Midterm outcome after a microsurgical unilateral approach for bilateral decompression of lumbar degenerative spondylolisthesis. J Neurosurg Spine 16:68–76. https://doi.org/10.3171/2011.7.SPINE11222
Kim S, Mortaz Hedjri S, Coyte PC, Rampersaud YR (2012) Cost-utility of lumbar decompression with or without fusion for patients with symptomatic degenerative lumbar spondylolisthesis. Spine J Off J N Am Spine Soc 12:44–54. https://doi.org/10.1016/j.spinee.2011.10.004
Alvin MD, Lubelski D, Abdullah KG et al (2016) Cost-utility analysis of instrumented fusion versus decompression alone for grade I L4-L5 spondylolisthesis at 1-year follow-up: a pilot study. Clin Spine Surg 29:E80–E86. https://doi.org/10.1097/BSD.0000000000000103
Gerling MC, Leven D, Passias PG et al (2017) Risk factors for reoperation in patients treated surgically for degenerative spondylolisthesis: a subanalysis of the 8-year data from the SPORT trial. Spine 42:1559–1569. https://doi.org/10.1097/BRS.0000000000002196
Meyerding HW (1932) Spondylolisthesis. Surg Gynecol Obstet 54:371–377
Alimi M, Hofstetter CP, Pyo SY et al (2015) Minimally invasive laminectomy for lumbar spinal stenosis in patients with and without preoperative spondylolisthesis: clinical outcome and reoperation rates. J Neurosurg Spine 22:339–352. https://doi.org/10.3171/2014.11.SPINE13597
Moayeri N, Pahuta M, Rampersaud Y (2017) Revision rates following minimally invasive decompression for lumbar spinal stenosis in patients with and without preoperative degenerative lumbar spondylolisthesis with a minimum of 5-year follow-up. Can J Surg 60(3 Suppl 4):S66
Mori G, Mikami Y, Arai Y et al (2016) Outcomes in cases of lumbar degenerative spondylolisthesis more than 5 years after treatment with minimally invasive decompression: examination of pre- and postoperative slippage, intervertebral disc changes, and clinical results. J Neurosurg Spine 24:367–374. https://doi.org/10.3171/2015.6.SPINE141298
Sudhir G, Acharya S, Kalra KL, Chahal R (2016) Radiographic analysis of the sacropelvic parameters of the spine and their correlation in normal asymptomatic subjects. Glob Spine J 6:169–175. https://doi.org/10.1055/s-0035-1558652
Wilkerson RD, Mason MA (2000) Differences in men’s and women’s mean ankle ligamentous laxity. Iowa Orthop J 20:46–48
Noojin FK, Barrett GR, Hartzog CW, Nash CR (2000) Clinical comparison of intraarticular anterior cruciate ligament reconstruction using autogenous semitendinosus and gracilis tendons in men versus women. Am J Sports Med 28:783–789. https://doi.org/10.1177/03635465000280060301
Kirkaldy-Willis WH, Farfan HF (1982) Instability of the lumbar spine. Clin Orthop 165:110–123
Enyo Y, Yoshimura N, Yamada H et al (2015) Radiographic natural course of lumbar degenerative spondylolisthesis and its risk factors related to the progression and onset in a 15-year community-based cohort study: the Miyama study. J Orthop Sci Off J Jpn Orthop Assoc 20:978–984. https://doi.org/10.1007/s00776-015-0759-8
Kalichman L, Kim DH, Li L et al (2009) Spondylolysis and spondylolisthesis: prevalence and association with low back pain in the adult community-based population. Spine 34:199–205. https://doi.org/10.1097/BRS.0b013e31818edcfd
Jacobsen S, Sonne-Holm S, Rovsing H et al (2007) Degenerative lumbar spondylolisthesis: an epidemiological perspective: the Copenhagen Osteoarthritis Study. Spine 32:120–125. https://doi.org/10.1097/01.brs.0000250979.12398.96
Coleman RR, Cremata EJ, Lopes MA et al (2014) Exploratory evaluation of the effect of axial rotation, focal film distance and measurement methods on the magnitude of projected lumbar retrolisthesis on plain film radiographs. J Chiropr Med 13:247–259. https://doi.org/10.1016/j.jcm.2014.09.001
Blumenthal C, Curran J, Benzel EC et al (2013) Radiographic predictors of delayed instability following decompression without fusion for degenerative grade I lumbar spondylolisthesis. J Neurosurg Spine 18:340–346. https://doi.org/10.3171/2013.1.SPINE12537
Simmonds AM, Rampersaud YR, Dvorak MF et al (2015) Defining the inherent stability of degenerative spondylolisthesis: a systematic review. J Neurosurg Spine 23:178–189. https://doi.org/10.3171/2014.11.SPINE1426
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethical approval
The project received research ethics board approval at the Toronto Western Hospital, University Health Network (Toronto, Canada), which is where the work originated.
Conflict of interest
The authors declare that they have no direct conflict of interest. Y.R. Rampersaud is a consultant for and has roylaties from Medtronic.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ravinsky, R.A., Crawford, E.J., Reda, L.A. et al. Slip progression in degenerative lumbar spondylolisthesis following minimally invasive decompression surgery is not associated with increased functional disability. Eur Spine J 29, 896–903 (2020). https://doi.org/10.1007/s00586-020-06336-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-020-06336-4