Abstract
Background
Although ureteral catheters and ureteral fluorescence methods have been investigated to avoid ureteral injury, they have not been standardized for procedural complexity and safety to the living body. A near-infrared (NIR) fluorescence ureteral catheter made of fluorescent resin was jointly developed for non-invasive detection of ureters. The aims of this study were to (1) evaluate its bench-top performance and (2) assert its safety and potential usefulness in a series of animal models.
Methods
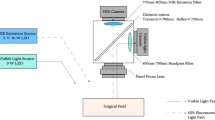
[Bench-top study]: Confirmed stimulation of NIR fluorescence catheter by NIR light was investigated with the use of a laparoscopic fluorescence imaging system. Additionally, the influence of imaging distance and shielding objects, such as 1.5-mm sliced pig loin with multiple sheets, was also evaluated. [Performance study]: The safety and potential usefulness of fluorescence catheter was evaluated in five pigs. Non-fluorescence and fluorescence ureteral catheters were alternatively placed in the animals’ left and right ureters. The ImageJ software was used in all experiments to quantify fluorescence signal and the signal-to-background ratio.
Results
[Bench-top study]: The fluorescence ureteral catheter was successfully identified at all distances. Its fluorescence decreased in inverse proportion to distance and to the intervening shield thickness (p < 0.01). When shields were present, catheter position could not be recognized with non-fluorescence catheters, but with fluorescence catheters they could be recognized. [Performance study]: Fluorescence catheter’s ability to fluoresce at all distances was confirmed (p < 0.01). No individual differences (p = 0.21) or left/right ureter differences (p = 0.79) were observed. The fluorescence of the fluorescence catheter decreased in inverse proportion to distance (p < 0.01).
Conclusions
The new fluorescence ureter catheter investigated shows promising performance in providing ureteral identification with high specificity during laparoscopic surgery.









Similar content being viewed by others
References
Harkki-Siren P, Sjoberg J, Makinen J, Heinonen PK, Kauko M, Tomas E, Laatikainen T (1997) Finnish national register of laparoscopic hysterectomies: a review and complications of 1165 operations. Am J Obstet Gynecol 176:118–122
Datta S, Wheatstone S, Challacombe B (2013) The acute management of iatrogenic urological injuries; strategies and mind-set for the urologist attending an unfamiliar operating theatre. BJU Int 112:540–542
Halabi WJ, Jafari MD, Nguyen VQ, Carmichael JC, Mills S, Pigazzi A, Stamos MJ (2014) Ureteral injuries in colorectal surgery: an analysis of trends, outcomes, and risk factors over a 10-year period in the United States. Dis Colon Rectum 57:179–186
Brandes S, Coburn M, Armenakas N, McAninch J (2004) Diagnosis and management of ureteric injury: an evidence-based analysis. BJU Int 94:277–289
Summerton DJ, Kitrey ND, Lumen N, Serafetinidis E, Djakovic N (2012) EAU guidelines on iatrogenic trauma. Eur Urol 62:628–639
Palaniappa NC, Telem DA, Ranasinghe NE, Divino CM (2012) Incidence of iatrogenic ureteral injury after laparoscopic colectomy. Arch Surg 147:267–271
Andersen P, Andersen LM, Iversen LH (2015) Iatrogenic ureteral injury in colorectal cancer surgery: a nationwide study comparing laparoscopic and open approaches. Surg Endosc 29:1406–1412
Kiran A, Hilton P, Cromwell D (2016) The risk of ureteric injury associated with hysterectomy: a 10-year retrospective cohort study. BJOG 123(7):1184–1191
Hairston JC, Ghoniem G (2003) Urinary tract injuries: recognition And management. Clin Colon Rectal Surg 16(1):027–038
Senagore AJ, Luchtefeld M (1994) An initial experience with lighted ureteral catheters during laparoscopic colectomy. J Laparoendosc Surg 4:399–403
Blackwell RH, Kirshenbaum EJ, Shah AS, Kuo PC, Gupta GN, Turk TMT (2018) Complications of recognized and unrecognized Iatrogenic ureteral injury at time of hysterectomy: a population based analysis. J Urol 199:1540–1545
Coakley KM, Kasten KR, Sims SM, Prasad T, Heniford BT, Davis BR (2018) Prophylactic ureteral catheters for colectomy: a National surgical quality improvement program-based analysis. Dis Colon Rectum 61:84–88
da Silva G, Boutros M, Wexner SD (2012) Role of prophylactic ureteric stents in colorectal surgery. Asian J Endosc Surg 5:105–110
Chahin F, Dwivedi AJ, Paramesh A, Chau W, Agrawal S, Chahin C, Kumar A, Tootla A, Tootla F, Silva YJ (2002) The implications of lighted ureteral stenting in laparoscopic colectomy. JSLS 6:49–52
Kaku S, Shimizu Y, Wakinoue S, Takebayashi A, Takashima A, Tarumoto Y, Nakagawa T, Kita N, Takahashi K, Murakami T (2010) Prevention of ureteral damage by using ureteral illuminating catheter during laparoscopic surgery. Jpn J Gynecol Obstet Endosc 26:541–544
Ushimaru Y, Omori T, Fujiwara Y, Yanagimoto Y, Sugimura K, Yamamoto K, Moon JH, Miyata H, Ohue M, Yano M (2018) The feasibility and safety of preoperative fluorescence marking with indocyanine green (ICG) in laparoscopic gastrectomy for gastric cancer. J Gastrointest Surg 23(3):468–476
Matsui A, Tanaka E, Choi HS, Kianzad V, Gioux S, Lomnes SJ, Frangioni JV (2010) Real-time, near-infrared, fluorescence-guided identification of the ureters using methylene blue. Surgery 148:78–86
Schols RM, Lodewick TM, Bouvy ND, van Dam GM, Dejong CH, Stassen LP (2014) Application of a new dye for near-infrared fluorescence laparoscopy of the ureters: demonstration in a pig model. Dis Colon Rectum 57:407–411
Al-Taher M, van den Bos J, Schols RM, Bouvy ND, Stassen LP (2016) Fluorescence ureteral visualization in human laparoscopic colorectal surgery using methylene blue. J Laparoendosc Adv Surg Tech A 26:870–875
Schols RM, Connell NJ, Stassen LP (2015) Near-infrared fluorescence imaging for real-time intraoperative anatomical guidance in minimally invasive surgery: a systematic review of the literature. World J Surg 39:1069–1079
Kono Y, Ishizawa T, Tani K, Harada N, Kaneko J, Saiura A, Bandai Y, Kokudo N (2015) Techniques of fluorescence cholangiography during laparoscopic cholecystectomy for better delineation of the bile duct anatomy. Medicine 94:e1005
Schneider CA, Rasband WS, Eliceiri KW (2012) NIH image to ImageJ: 25 years of image analysis. Nat Methods 9:671–675
Parpala-Sparman T, Paananen I, Santala M, Ohtonen P, Hellstrom P (2008) Increasing numbers of ureteric injuries after the introduction of laparoscopic surgery. Scand J Urol Nephrol 42:422–427
McKinley SK, Brunt LM, Schwaitzberg SD (2014) Prevention of bile duct injury: the case for incorporating educational theories of expertise. Surg Endosc 28:3385–3391
Shallaly GEI, Cuschieri A (2000) Nature, aetiology and outcome of bile duct injuries after laparoscopic cholecystectomy. HPB 2:3–12
Strasberg SM, Hertl M, Soper NJ (1995) An analysis of the problem of biliary injury during laparoscopic cholecystectomy. J Am Coll Surg 180:101–125
Way LW, Stewart L, Gantert W, Liu K, Lee CM, Whang K, Hunter JG (2003) Causes and prevention of laparoscopic bile duct injuries: analysis of 252 cases from a human factors and cognitive psychology perspective. Ann Surg 237:460–469
Merola J, Arnold B, Luks V, Ibarra C, Resio B, Davis KA, Pei KY (2018) Prophylactic ureteral stent placement vs no ureteral stent placement during open colectomy. JAMA Surg 153:87–90
Chu W, Chennamsetty A, Toroussian R, Lau C (2017) Anaphylactic shock after intravenous administration of indocyanine green during robotic partial nephrectomy. Urol Case Rep 12:37–38
Ginimuge PR, Jyothi SD (2010) Methylene blue: revisited. J Anaesthesiol Clin Pharmacol 26:517–520
Acknowledgments
This work was presented and prized at the Gerhard Buess Technology Award session during the 27th International EAES Congress, Sevilla, Spain, held on June 13 and 14, 2019.
Funding
No funding was received for this research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Disclosures
Dr. Yuki Ushimaru, Mr. Atsushi Ohigawa, Dr. Kotaro Yamashita, Dr. Takuro Saito, Dr. Koji Tanaka, Dr. Tomoki Makino, Dr. Tsuyoshi Takahashi, Dr. Yukinori Kurokawa, Dr. Makoto Yamasaki, Dr. Masaki Mori, Dr. Yuichiro Doki, and Dr. Kiyokazu Nakajima have no conflicts of interest or financial ties to disclose.
Ethical approval
All procedures in this study were performed in accordance with the ethical standards of the responsible committee on institutional human experimentation and with the Helsinki Declaration of 1964 and its later versions.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ushimaru, Y., Ohigawa, A., Yamashita, K. et al. Real-time ureteral identification with novel, versatile, and inexpensive catheter. Surg Endosc 34, 3669–3678 (2020). https://doi.org/10.1007/s00464-019-07261-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00464-019-07261-4