Abstract
Introduction
Although the advantages of total hip arthroplasty (THA) using the direct anterior approach (DAA) have been well documented, DAA in the supine position is limited by the difficulty in exposing the acetabulum and femur, which may result in implant malpositioning and intra-operative complications. Recent studies have reported that DAA-THA in the lateral position can achieve satisfactory clinical and radiographic outcomes. The aim of this study was to investigate the difference in implant alignment between two patient cohorts that underwent primary THA by DAA and the traditional posterolateral approach (PLA) in the lateral position.
Methods
A total of 208 THAs (110 using DAA and 98 using PLA) were retrospectively analyzed.
Results
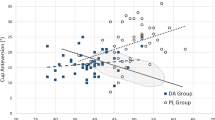
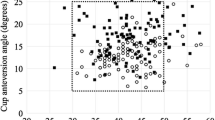
The cup anteversion angle was closer to the target anteversion angle, and the accuracy of cup orientation was superior in the DAA group. A total of 82 (74.5%) DAA-THA and 56 (57.1%) PLA-THA cases showed successful inclination and anteversion angles (p = 0.008) of the implant. In addition, 90 (81.8%) DAA-THA and 67 (68.4%) PLA-THA cases had successful anteversion angle (p = 0.024). There was no significant difference between the two groups in terms of successful inclination angle (98 vs. 81, p = 0.181), as well as in the stem alignment in both coronal and sagittal planes.
Conclusion
THA using DAA in the lateral position can achieve superior cup orientation compared to PLA while maintaining the stem alignment.





Similar content being viewed by others
References
Nakata K, Nishikawa M, Yamamoto K, Hirota S, Yoshikawa H (2009) A clinical comparative study of the direct anterior with mini-posterior approach: two consecutive series. J Arthroplast 24:698–704. https://doi.org/10.1016/j.arth.2008.04.012
Jia F, Guo B, Xu F, Hou Y, Tang X, Huang L (2018) A comparison of clinical, radiographic and surgical outcomes of total hip arthroplasty between direct anterior and posterior approaches: a systematic review and meta-analysis. Hip Int 31:1120700018820652. https://doi.org/10.1177/1120700018820652
Wang Z, Hou JZ, Wu CH, Zhou YJ, Gu XM, Wang HH, Feng W, Cheng YX, Sheng X, Bao HW (2018) A systematic review and meta-analysis of direct anterior approach versus posterior approach in total hip arthroplasty. J Orthop Surg Res 13:229. https://doi.org/10.1186/s13018-018-0929-4
Barrett WP, Turner SE, Leopold JP (2013) Prospective randomized study of direct anterior vs postero-lateral approach for total hip arthroplasty. J Arthroplast 28:1634. https://doi.org/10.1016/j.arth.2013.01.034
Brismar BH, Hallert O, Tedhamre A, Lindgren JU (2018) Early gain in pain reduction and hip function, but more complications following the direct anterior minimally invasive approach for total hip arthroplasty: a randomized trial of 100 patients with 5 years of follow up. Acta Orthop 89:484–489. https://doi.org/10.1080/17453674.2018.1504505
Ahmed MM, Otto TJ, Moed BR (2016) Anterior total hip arthroplasty using a metaphyseal bone-sparing stem: component alignment and early complications. J Orthop Surg Res 22:46. https://doi.org/10.1186/s13018-016-0383-0
Kawarai Y, Iida S, Nakamura J, Shinada Y, Suzuki C, Ohtori S (2017) Does the surgical approach influence the implant alignment in total hip arthroplasty? Comparative study between the direct anterior and the anterolateral approaches in the supine position. Int Orthop 41:2487–2493. https://doi.org/10.1007/s00264-017-3521-3
Kobayashi H, Homma Y, Baba T, Ochi H, Matsumoto M, Yuasa T, Kaneko K (2016) Surgeons changing the approach for total hip arthroplasty from posterior to direct anterior with fluoroscopy should consider potential excessive cup anteversion and flexion implantation of the stem in their early experience. Int Orthop 40:1813–1819. https://doi.org/10.1007/s00264-015-3059-1
Abe H, Sakai T, Takao M, Nishii T, Nakamura N, Sugano N (2015) Difference in stem alignment between the direct anterior approach and the posterolateral approach in total hip arthroplasty. J Arthroplast 30:1761–1766.https://doi.org/10.1016/j.arth.2015.04.026
Jolles BM, Zangger P, Leyvraz PF (2002) Factors predisposing to dislocation after primary total hip arthroplasty: a multivariate analysis. J Arthroplast 17:282–288. https://doi.org/10.1054/arth.2002.30286
Melman WP, Mollen BP, Kollen BJ, Verheyen CC (2015) First experiences with the direct anterior approach in lateral decubitus position: learning curve and 1 year complication rate. Hip Int 25:251–257. https://doi.org/10.5301/hipint.5000221
Chen M, Luo Z, Ji X, Cheng P, Tang G, Shang X (2017) Direct anterior approach for total hip arthroplasty in the lateral decubitus position: our experiences and early results. J Arthroplast 32:131–138. https://doi.org/10.1016/j.arth.2016.05.066
Lewinnek GE, Lewis JL, Tarr R, Compere CL, Zimmerman JR (1978) Dislocations after total hip re-placement arthroplasties. J Bone Joint Surg Am 60:217–220
Widmer KH (2004) A simplified method to determine acetabular cup anteversion from plain radiographs. J Arthroplast 19:387–390
Dorr LD, Faugere MC, Mackel AM, Gruen TA, Bognar B, Malluche HH (1993) Structural and cellular assessment of bone quality of proximal femur. Bone 14:231–242
Noble PC, Alexander JW, Lindahl LJ, Yew DT, Granberry WM, Tullos HS (1988) The anatomic basis of femoral component design. Clin Orthop Relat Res 235:148–165
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This retrospective study was conducted in compliance with the Helsinki Declaration and was approved by Anhui Provincial Hospital review board.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 49 kb)
Rights and permissions
About this article
Cite this article
Hu, F., Shang, X., Zhang, X. et al. Direct anterior approach in lateral position achieves superior cup orientation in total hip arthroplasty: a radiological comparative study of two consecutive series. International Orthopaedics (SICOT) 44, 453–459 (2020). https://doi.org/10.1007/s00264-019-04461-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-019-04461-4