Abstract
Aim of the study
To identify the most reliable anatomical landmarks and imaging techniques for assessing the rotation of the tibial component in total knee arthroplasty (TKA).
Methods
An extensive literature review (from January 2016 to March 2019) was performed. We included studies about primary TKA with details concerning the anatomical landmarks used for implanting the tibial component and also imaging studies assessing tibial component rotation. The final selection comprises only thirty-five articles consistent with the inclusion criteria.
Results
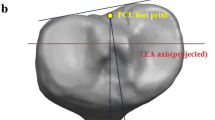
Extra-articular landmarks are not always reliable (even though the tibial tubercle is one of the most popular extra-articular landmarks used to assess the rotation of the tibial component), mainly because they vary and can lead to malrotation of the tibial component. Akagi’s line (an intra-articular landmark) is considered to be the most reliable and easy to find during surgery and likewise is not affected by articular deformities. The anterior tibial cortex (intra-articular landmark) also proved to be accurate and reliable with the main advantage being that is palpable after tibial resection.
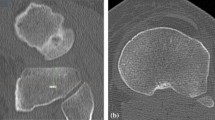
Radiography provides a good and inexpensive option for imaging, but it is insufficient. Magnetic resonance imaging (MRI) is used in some cases but not routinely for assessing TKA components or their orientation. Computed tomography (CT), used together with a well-defined protocol (Berger’s method being the preferred choice), remains the “gold standard” for evaluating the rotation of the tibial component after TKA.
Conclusion
Currently, the most accurate and reliable anatomical landmarks are represented by Akagi’s line and the anterior cortex of the tibia. Post-operatively, through CT and well-established protocols, the rotation of the tibial component can be accurately determined.



Similar content being viewed by others
References
Gaillard R, Cerciello S, Lustig S et al (2017) Risk factors for tibial implant malpositioning in total knee arthroplasty – consecutive series of one thousand, four hundred and seventeen cases. Int Orthop (SICOT) 41(4):749–756. https://doi.org/10.1007/s00264-016-3307-z
Pedraza W, Beckmann J, Mayer C et al (2016) Partially loaded plain radiographic measurement to evaluate rotational alignment in total knee arthroplasty. Int Orthop (SICOT) 40(12):2519–2526. https://doi.org/10.1007/s00264-016-3247-7
Drexler M, Backstein D, Studler U et al (2017) The medial border of the tibial tuberosity as an auxiliary tool for tibial component rotational alignment during total knee arthroplasty (TKA). Knee Surg Sports Traumatol Arthrosc 25(6):1736–1742. https://doi.org/10.1007/s00167-016-4072-7
Hirakawa M, Miyazaki M, Ikeda S, Matsumoto Y, Kondo M, Tsumura H (2017) Evaluation of the rotational alignment of tibial component in total knee arthroplasty: position prioritizing maximum coverage. Eur J Orthop Surg Traumatol 27(1):119–124. https://doi.org/10.1007/s00590-016-1850-3
Kim JI, Jang J, Lee KW, Han HS, Lee S, Lee MC (2017) Anterior tibial curved cortex is a reliable landmark for tibial rotational alignment in total knee arthroplasty. BMC Musculoskelet Disord 18:252. https://doi.org/10.1186/s12891-017-1609-y
Mitshuhashi S, Akamatsu Y, Kobayashi H et al (2018) Combined CT-based and image free-navigation systems in TKA reduces postoperative outliers of rotational alignment of the tibial component. Arch Orthop Trauma Surg 138(2):259–266. https://doi.org/10.1007/s00402-017-2837-1
Cerquiglini A, Henckel J, Hothi H et al (2018) 3D patient imaging and retrieval analysis help understand the clinical importance of rotation in knee replacements. Knee Surg Sports Traumatol Arthrosc 26(11):3351–3361. https://doi.org/10.1007/s00167-018-4891-9
Singh AK, Nedopil AJ, Howell SM et al (2018) Does alignment of the limb and tibial width determine relative narrowing between compartments when planning mechanically aligned TKA? Arch Orthop Trauma Surg 138(1):91–97. https://doi.org/10.1007/s00402-017-2824-6
Slevin O, Hirschmann A, Schiapparelli FF, Amsler F et al (2018) Neutral alignment leads to higher knee society scores after total knee arthroplasty in preoperatively non-varus patients: a prospective clinical study using 3D-CT. Knee Surg Sports Traumatol Arthrosc 26(6):1602–1609. https://doi.org/10.1007/s00167-017-4744-y
Sailhan F, Jacob L, Hamadouche M (2017) Differences in limb alignment and femoral mechanical-anatomical angles using two dimensions versus three dimension radiograph imaging. Int Orthop 41(10):2009–2016. https://doi.org/10.1007/s00264-017-3428-z
Schiapparelli FF, Amsler F, Hirschmann MT (2018) Medial parapatellar approach leads to internal rotation of tibial component in total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 26(5):1564–1570. https://doi.org/10.1007/s00167-017-4586-7
Hanada M, Furuhashi H, Matsuyama Y (2019) Investigation of the control of rotational alignment in tibial component during total knee arthroplasty. Eur J Orthop Surg Traumatol 29(6):1313–1317. https://doi.org/10.1007/s00590-019-02427-1
Saffarini M, Nover L, Tandogan R et al (2019) The original Akagi line is the most reliable: a systematic review of landmarks for rotational alignment of the tibial component in TKA. Knee Surg Sports Traumatol Arthrosc 27(4):1018–1027. https://doi.org/10.1007/s00167-018-5131-z
Benazzo F, Rossi SMP, Danesino G et al (2019) Computed tomography evaluation of total knee arthroplasty implants position after two different surgical methods of implantation. Int Orthop 43(1):139–149. https://doi.org/10.1007/s00264-018-4180-8
Benazzo F, Ghiara M, Rossi SMP et al (2019) Clinical and radiological analysis of a personalized total knee arthroplasty system design. Int Orthop (SICOT) 43(5):1113–1121. https://doi.org/10.1007/s00264-018-4095-4
Mahmood FF, Holloway NJ, Deakin AH, Clarke JV, Picard F (2019) A new landmark for measuring tibial component rotation after total knee arthroplasty. Knee 26(3):779–786. https://doi.org/10.1016/j.knee.2018.09.002
Ohmori T, Kabata T, Kajino Y, Inoue D, Taga T, Yamamoto T, Takagi T, Yoshitani J, Ueno T, Ueoka K, Tsuchiya H (2018) A proposed new rotating reference axis for the tibial component after proximal tibial resection in total knee arthroplasty. PLoS One. https://doi.org/10.1371/journal.pone.0209317
Tiftikçi U, Serbest S, Burulday V (2017) Can Achilles tendon be used as a new distal landmark for coronal tibial component alignment in total knee replacement surgery? An observational MRI study. Ther Clin Risk Manag 13:81–86. https://doi.org/10.2147/TCRM.S125551
Ma Y, Mizu-uchi H, Ushio T et al (2018) Bony landmarks with tibial cutting surface are useful to avoid rotational mismatch in the total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 27(5):1570–1579. https://doi.org/10.1007/s00167-018-5052-x
Wernecke GC, Harris IA, Seeto BG et al (2016) Normal femorotibial rotational alignment and implications for total knee arthroplasty: an MRI analysis. HSS J 12(3):223–223. https://doi.org/10.1007/s11420-016-9503-y
Sina Babazadeh PD, Dowsey MM, Vasimalla MG, Stoney JD, Choong PFM (2019) Knee arthroplasty component malrotation does not affect function or quality of life in the short to medium term. J Arthroplast 34(7):1382–1386. https://doi.org/10.1016/j.arth.2019.02.056
Feckzo PZ, Pijls BG, van Steijn MJ, van Rhijn LW, Arts JJ, Emans PJ (2016) Tibial component rotation in total knee arthroplasty. BMC Musculoskelet Disord 17:87. https://doi.org/10.1186/s12891-016-0940-z
Niki Y, Nagura T, Nagai K et al (2018) Kinematically aligned total knee arthroplasty reduces knee adduction moment more than mechanically aligned total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 26(6):1629–1635. https://doi.org/10.1007/s00167-017-4788-z
Chanalithichai N, Tammachote N, Jitapunkul C et al (2019) Rotational component alignment in patient-specific total knee arthroplasty compared with conventional cutting instrument. Eur J Orthop Surg Traumatol 29(6):1297–1304. https://doi.org/10.1007/s00590-019-02423-5
Saffi M, Young SW, Spangehl MJ, Clarke HD (2019) Measuring tibial component rotation following total knee arthroplasty: what is the best method? J Arthroplast 34(7):S355–S360. https://doi.org/10.1016/j.arth.2018.10.022
Fritz J, Lurie B, Potter HG (2015) MR imaging of knee arthroplasty implants. Radiographics 35(5):1483–1501. https://doi.org/10.1148/rg.2015140216
Haaker RG, Stockheim M, Kamp M, Proff G, Breitenfelder J, Ottersbach A (2005) Computer-assisted navigation increases precision of component placement in total knee arthroplasty. Clin Orthop Relat Res 433:152–159. https://doi.org/10.1097/01.blo.0000150564.31880.c4
Cheng T, Zhao S, Peng X et al (2012) Does computer-assisted surgery improve postoperative leg alignment and implant positioning following total knee arthroplasty? A meta-analysis of randomized controlled trials. Knee Surg Sports Traumatol Arthrosc 20(7):1307–1322. https://doi.org/10.1007/s00167-011-1588-8
Murakami AM, Hash TW, Hepinstall MS, Lyman S, Nestor BJ, Potter HG (2012) MRI evaluation of rotational alignment and synovitis in patients with pain after total knee replacement. J Bone Joint Surg Br 94-B(9):1209–1215. https://doi.org/10.1302/0301-620X.94B9.28489
Slevin O, Amsler F, Hirschmann MT (2017) No correlation between coronal alignment of total knee arthroplasty and clinical outcomes: a prospective clinical study using 3D-CT. Knee Surg Sports Traumatol Arthrosc 25(12):3892–3900. https://doi.org/10.1007/s00167-016-4400-y
Amantullah DF, Ollivier MP, Pallante GD, Abdel MP, Clarke HD, Mabry TM, Taunton MJ (2017) Reproducibility and precision of CT scans to evaluate tibial component rotation. J Arthroplast 32:2552–2555. https://doi.org/10.1016/j.arth.2017.01.040
van Houten AH, Kosse NM, Wessels M, Wymenga AB (2018) Measurement techniques to determine tibial rotation after total knee arthroplasty are less accurate than we think. Knee 25(4):663–668. https://doi.org/10.1016/j.knee.2018.05.006
Stolarczyk A, Nagraba L, Mitek T, Stolarczyk M, Deszczyński JM, Jakucinski M (2018) Does patient-specific instrumentation improve femoral and tibial component alignment in total knee arthroplasty? A prospective randomized study. Adv Exp Med Biol 1096:11–17. https://doi.org/10.1007/5584_2018_193
Hochreiter B, Hirschmann MT, Amsler F et al (2019) Highly variable tibial tubercle-trochlear groove distance (TT-TG) in osteoarthritic knees should be considered when performing TKA. Knee Surg Sports Traumatol Arthrosc 27(5):1403–1409. https://doi.org/10.1007/s00167-018-5141-x
Song EK, Agrawal PR, Kim SK et al (2016) A randomized controlled clinical and radiological trial about outcomes of navigation- assisted TKA compared to conventional TKA: long-term follow-up. Knee Surg Sports Traumatol Arthrosc 24(11):3381–3386. https://doi.org/10.1007/s00167-016-3996-2
Teeter MG, Naudie DD, McCalden RW, Yuan X et al (2018) Varus tibial alignment is associated with greater tibial baseplate migration at 10 years following total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 26(6):1610–1617. https://doi.org/10.1007/s00167-017-4765-6
Loures FB, Correia W, Reis JH et al. (2018) Outcomes after knee arthroplasty in extra-articular deformity. Int Orthop (SICOT) 1–6. https://doi.org/10.1007/s00264-018-4147-9
Puliero B, Favreau H, Eichler D et al (2019) Total knee arthroplasty in patients with varus deformities greater than 10 degrees: survival analysis at a mean ten year follow-up. Int Orthop (SICOT) 43(2):333–341. https://doi.org/10.1007/s00264-018-4019-3
Mugnai R, Zambianchi F, Digennaro V, Marcovigi A, Tarallo L, del Giovane C, Catani F (2016) Clinical outcome is not affected by total knee arthroplasty alignment. Knee Surg Sports Traumatol Arthrosc 24(10):3339–3345. https://doi.org/10.1007/s00167-016-4094-1
Sardana V, Burzynski JM, Khan M et al (2016) Long-term functional outcomes and knee alignment of computer-assisted navigated total knee arthroplasty. Musculoskelet Surg 101(1):37–43. https://doi.org/10.1007/s12306-016-0442-z
Sasanuma H, Sekiya H, Takatoku K, Ajiki T, Hagiwara H (2014) Accuracy of a proximal tibial cutting method using the anterior tibial border in TKA. Eur J Orthop Surg Traumatol 24(8):1525–1530. https://doi.org/10.1007/s00590-014-1415-2
Nishikawa K, Mizuuchi H, Okazaki K, Matsuda S, Tashiro Y, Iwamoto Y (2015) Accuracy of proximal tibial bone cut using anterior border of tibia as bony landmark in total knee arthroplasty. J Arthroplasty 30(12):2121–2124. https://doi.org/10.1016/j.arth.2015.06.055
Lützner J, Krummenauer F, Günther KP, Kirschner S (2010) Rotational alignment of the tibial component in total knee arthroplasty is better at the medial third of the tuberosity than at the medial border. BMC Musculoskelet Disord 11:57. https://doi.org/10.1186/1471-2474-11-57
Cobb JP, Dixon H, Dandachli W, Iranpour F (2008) The anatomical tibial axis: reliable rotational orientation in knee replacement. J Bone Joint Surg Br 90(8):1032–1038. https://doi.org/10.1302/0301-620X.90B8.19905
Berger RA, Runash HE (2001) Rotational instability and malrotation after total knee arthroplasty. Orthop Clin N Am 32(4):639–647. https://doi.org/10.1016/S0030-5898(05)70233-9
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflicts of interest.
Permissions
The authors have obtained permission from the Springer Nature and Copyright Clearance Centre to use Table 3 and Fig. 2 from this text, which are taken from the article written by Mo Saffarini, Luca Nover, Reha Tandogan et al., “The original Akagi line is the most reliable: a systematic review of landmarks for rotational alignment of the tibial component in TKA,” published in Knee Surgery, Sports Traumatology, Arthroscopy (2018). Permission attached.
Ethical approval
Ethical approval was not required for this study.
Informed consent and patient details
Informed consent was not applicable to this study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Popescu, R., Haritinian, E.G. & Cristea, S. Methods of intra- and post-operative determination of the position of the tibial component during total knee replacement. International Orthopaedics (SICOT) 44, 119–128 (2020). https://doi.org/10.1007/s00264-019-04424-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00264-019-04424-9