Abstract
Objectives
To identify the relationship between human epidermal growth factor receptor 2 (HER2) status and cone-beam breast CT (CBBCT) characteristics in surgically resected breast cancer.
Methods
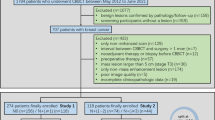
Preoperative CBBCT of patients with BI-RADS 4 or 5 lesions identified on mammography or ultrasound and dense or very dense breast tissue were retrospectively evaluated in 181 surgically resected breast cancer (triple-negative excluded) between May 2012 and November 2014. A set of CBBCT descriptors was semiquantitatively assessed by consensus double reading. Reader reproducibility was analyzed. Multivariable logistic regression analysis using backward elimination (BEA) with the Wald criterion was performed to identify independent predictive factors of harboring HER2/neu. Principle component analysis (PCA) was used to determine characteristics that might differentiate HER2 status. Receiver operating characteristic (ROC) curve analyses were conducted to determine the predictive capability.
Results
HER2 positive was found in 101 (55.8%) of 181 patients. Inter-observer agreement was high for characteristics’ assessment. Based on BEA, pathologic grade, maximum dimension, lobulation, ΔCT, and calcification morphology were confirmed as independent predictive factors of HER2/neu overexpression. PCA showed that calcification- and border-related characteristics were the most important for differentiation. ROC curve analyses showed that CBBCT features (AUC = 0.853) were superior to clinicopathologic features (AUC = 0.613, p < 0.001) and comparable with combination (AUC = 0.856, p = 0.866).
Conclusions
CBBCT features could be used to prognosticate HER2 status independently, which are potentially complementary to histopathologic result and helpful in guiding biopsy.
Key Points
• Dmax, lobulation, ΔCT, and calcification morphology are independent predictors of HER2 status.
• CBBCT features are superior to clinicopathologic features in HER2+/− discrimination.
• CBBCT features are comparable with combination with clinicopathologic features in HER2+/− discrimination.



Similar content being viewed by others
Change history
17 February 2020
The original version of this article, published on 03 January 2020, unfortunately contained two mistakes.
Abbreviations
- AUC:
-
Area under the ROC curve
- BEA:
-
Backward elimination analysis
- BI-RADS:
-
Breast Imaging Reporting and Data System
- CBBCT:
-
Cone-beam breast computed tomography
- FISH:
-
Fluorescent in situ hybridization
- HER2:
-
Human epidermal growth factor receptor 2
- IHC:
-
Immunohistochemical
- NME:
-
Non-mass enhancement
- PCA:
-
Principle component analysis
- ROC:
-
Receiver operating characteristic
References
Harbeck N, Gnant M (2017) Breast cancer. Lancet 389:1134–1150
Leung HWC, Leung JH, Chan ALF (2018) Efficacy and safety of a combination of HER2-targeted agents as first-line treatment for metastatic HER2-positive breast cancer: a network meta-analysis. Expert Opin Drug Saf 17:1–7
Rye IH, Trinh A, Saetersdal AB et al (2018) Intratumor heterogeneity defines treatment-resistant HER2+ breast tumors. Mol Oncol 12:1838–1855
Gillies RJ, Kinahan PE, Hricak H (2016) Radiomics: images are more than pictures, they are data. Radiology 278:563–577
O’Connell AM, Karellas A, Vedantham S, Kawakyu-O’Connor DT (2018) Newer technologies in breast cancer imaging: dedicated cone-beam breast computed tomography. Semin Ultrasound CT MR 39:106–113
Wienbeck S, Fischer U, Perske C et al (2017) Cone-beam breast computed tomography: CT density does not reflect proliferation potential and receptor expression of breast carcinoma. Transl Oncol 10:599–603
Uhlig J, Fischer U, von Fintel E et al (2017) Contrast enhancement on cone-beam breast-CT for discrimination of breast cancer immunohistochemical subtypes. Transl Oncol 10:904–910
Meattini I, Bicchierai G, Saieva C et al (2017) Impact of molecular subtypes classification concordance between preoperative core needle biopsy and surgical specimen on early breast cancer management: single-institution experience and review of published literature. Eur J Surg Oncol 43:642–648
Yoshida A, Hayashi N, Suzuki K, Takimoto M, Nakamura S, Yamauchi H (2017) Change in HER2 status after neoadjuvant chemotherapy and the prognostic impact in patients with primary breast cancer. J Surg Oncol 116:1021–1028
Elias SG, Adams A, Wisner DJ et al (2014) Imaging features of HER2 overexpression in breast cancer: a systematic review and meta-analysis. Cancer Epidemiol Biomarkers Prev 23:1464–1483
American College of Radiology (ACR) (2018) ACR practice parameter for the performance of screening and diagnostic mammography. Available via https://www.acr.org/-/media/ACR/Files/Practice-Parameters/screen-diag-mammo.pdf. Accessed 16 Sept 2019
European Reference Organisation for Quality Assured Breast Screening and Diagnostic Services (EUREF) (2006) European guidelines for quality assurance in breast cancer screening and diagnosis. Available via https://www.euref.org/downloads?download=24:european-guidelines-for-quality-assurance-in-breast-cancer-screening-and-diagnosis-pdf. Accessed 16 Sept 2019
D’Orsi CJ, Sickles EA, Mendelson EB et al (2013) ACR BI-RADS Atlas, breast imaging reporting and data system. American College of Radiology, Reston, VA
Wang H, Schabath MB, Liu Y et al (2015) Semiquantitative computed tomography characteristics for lung adenocarcinoma and their association with lung cancer survival. Clin Lung Cancer 16:e141–e163
Liu Y, Kim J, Qu F et al (2016) CT features associated with epidermal growth factor receptor mutation status in patients with lung adenocarcinoma. Radiology 280:271–280
Prionas ND, Lindfors KK, Ray S et al (2010) Contrast-enhanced dedicated breast CT: initial clinical experience. Radiology 256:714–723
Sardanelli F, Iozzelli A, Fausto A, Carriero A, Kirchin MA (2005) Gadobenate dimeglumine–enhanced MR imaging breast vascular maps: association between invasive cancer and ipsilateral increased vascularity. Radiology 235:791–797
Wolff AC, Hammond ME, Hicks DG et al (2013) Recommendations for human epidermal growth factor receptor 2 testing in breast cancer: American Society of Clinical Oncology/College of American Pathologists clinical practice guideline update. J Clin Oncol 31:3997–4013
Bae MS, Moon WK, Chang JM et al (2013) Mammographic features of calcifications in DCIS: correlation with oestrogen receptor and human epidermal growth factor receptor 2 status. Eur Radiol 23:2072–2078
Cen D, Xu L, Li N et al (2017) BI-RADS 3-5 microcalcifications can preoperatively predict breast cancer HER2 and luminal a molecular subtype. Oncotarget 8:13855–13862
Nie Z, Wang J, Ji XC (2018) Microcalcification-associated breast cancer: HER2-enriched molecular subtype is associated with mammographic features. Br J Radiol 21:20170942
Nasir A, Holzer TR, Chen M, Man MZ, Schade AE (2017) Differential expression of VEGFR2 protein in HER2 positive primary human breast cancer: potential relevance to anti-angiogenic therapies. Cancer Cell Int 17:56
Bae MS, Seo M, Kim KG, Park IA, Moon WK (2015) Quantitative MRI morphology of invasive breast cancer: correlation with immunohistochemical biomarkers and subtypes. Acta Radiol 56:269–275
Jiang S, Hong YJ, Zhang F, Li YK (2017) Computer-aided evaluation of the correlation between MRI morphology and immunohistochemical biomarkers or molecular subtypes in breast cancer. Sci Rep 7:13818
Ma Y, Cao Y, Liu A et al (2019) A reliability comparison of cone-beam breast computed tomography and mammography: breast density assessment referring to the fifth edition of the BI-RADS atlas. Acad Radiol 26:752–759
Wienbeck S, Uhlig J, Luftner-Nagel S et al (2017) The role of cone-beam breast-CT for breast cancer detection relative to breast density. Eur Radiol 27:5185–5195
Wienbeck S, Fischer U, Luftner-Nagel S, Lotz J, Uhlig J (2018) Contrast-enhanced cone-beam breast-CT (CBBCT): clinical performance compared to mammography and MRI. Eur Radiol 28:3731–3741
O’Connell A, Conover DL, Zhang Y et al (2010) Cone-beam CT for breast imaging: radiation dose, breast coverage, and image quality. AJR Am J Roentgenol 195:496–509
Uhlig J, Fischer U, Biggemann L, Lotz J, Wienbeck S (2019) Pre- and post-contrast versus post-contrast cone-beam breast CT: can we reduce radiation exposure while maintaining diagnostic accuracy? Eur Radiol 29:3141–3148
Ding H, Ducote JL, Molloi S (2013) Measurement of breast tissue composition with dual energy cone-beam computed tomography: a postmortem study. Med Phys 40:061902
Bian J, Yang K, Boone JM, Han X, Sidky EY, Pan X (2014) Investigation of iterative image reconstruction in low-dose breast CT. Phys Med Biol 59:2659–2685
Kalender WA, Kolditz D, Steiding C et al (2017) Technical feasibility proof for high-resolution low-dose photon-counting CT of the breast. Eur Radiol 27:1081–1086
Funding
This study has received funding by the National Key R&D Program of China (No. 2017YFC0112600 and 2017YFC0112601), National Natural Science Foundation of China (No. 81571671), Tianjin Science and Technology Major Project (No. 19ZXDBSY00080), and Key Project of Tianjin Medical Industry (No. 16KG130).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Prof. Dr. Zhaoxiang Ye.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
One of the authors (Yuwei Zhang) has significant statistical expertise.
Informed consent
Written informed consent was obtained from all patients in this study.
Ethical approval
Institutional Review Board approval was obtained (E2012036).
Study subjects or cohorts overlap
This study included the population of a clinical trial (NCT01792999) of which subgroup analyses had been published previously regarding diagnostic performance analysis, visual and quantitative breast density assessment, breast tissue coverage and comfort comparison, and tumor size evaluation. In comparison, here we investigated molecular subtype prediction that had not been evaluated previously.
① Li H, Yin L, Ye Z, et al (2015) Comparative study of breast tissue coverage in cone-beam breast CT versus digital mammography. Chin J Radiol 49:488–490 in Chinese
② Liu A, Ma Y, Yin L, Han P, Li H, Ye Z (2018) Comparison of the diagnostic efficiency in breast malignancy between cone beam breast CT and mammography in dense breast. Chin J Oncol 40:604–609 in Chinese
③ Liu A, Ma Y, Yin L, Han P, Li H, Ye Z (2018) Diagnostic value of contrast-enhanced cone beam breast CT in dense breast lesions. China Oncology 28:807–812 in Chinese
④ Liu A, Ye Z, Ma Y, Cao Y (2018) Reliability of breast density estimation based on cone beam breast CT. Chin J Clin Oncol 45:246–250 in Chinese
⑤ Ma Y, Ye Z, Liu A, Yin L, Han P, Li H (2019) The accuracy of tumor size evaluation on invasive breast cancer based on cone beam breast CT. Chin J Radiol 53:286–291 in Chinese
⑥ Ma Y, Cao Y, Liu A, et al (2019) A reliability comparison of cone-beam breast computed tomography and mammography: breast density assessment referring to the Fifth Edition of the BI-RADS Atlas. Acad Radiol 26:752–759
⑦ Li H, Yin L, He N, et al (2019) Comparison of comfort between cone beam breast computed tomography and digital mammography. Eur J Radiol 120:108674
Methodology
• retrospective
• diagnostic or prognostic study
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Firstly, in the third paragraph of section “Introduction”, the second sentence was worded incorrectly. The correct wording is: “Advantages of CBBCT include patient comfort improvement due to lack of breast compression and lesion conspicuity increasing with avoiding tissue overlap owing to true 3D display compared with mammography and tomosynthesis, elimination of operator subjectivity in contrast to ultrasound, rapid acquisition and less cost in comparison with magnetic resonance imaging (MRI), and available simultaneous assessment of calcification and contrast enhancement [5].” Secondly, the presentation of Figure 2b was incorrect. The Δ in ΔCT was missing.
Electronic supplementary material
ESM 1
(DOC 186 kb)
Rights and permissions
About this article
Cite this article
Zhu, Y., Zhang, Y., Ma, Y. et al. Cone-beam breast CT features associated with HER2/neu overexpression in patients with primary breast cancer. Eur Radiol 30, 2731–2739 (2020). https://doi.org/10.1007/s00330-019-06587-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-019-06587-w