Abstract
Objectives
To assess a disease-specific structured report (dsSR) for CT staging of ovarian malignancy compared to a simple structured report (sSR).
Methods
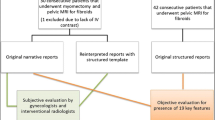
This is a HIPAA-compliant, IRB-approved study with waiver of informed consent. An adnexal mass-specific structured reporting CT template was developed in collaboration between gynecologic oncologists and diagnostic radiologists. The study population included 24 consecutive women who had a staging CT prior to undergoing debulking surgery for a primary ovarian malignancy. Objective evaluation by radiologists for the presence of 19 key features and subjective evaluation by gynecologic oncologists were performed to assess the clarity and usefulness for procedural planning of dsSR and sSR. Accuracy, sensitivity, and specificity were assessed using operating room notes and pathology reports as the reference standard.
Results
Fewer key features were missing from dsSR than sSR: 0.2 ± 0.8 (range 0–2) vs.10.2 ± 1.7 (range 7–14), respectively (p < 0.0001). Compared to sSR, gynecologic oncologists deemed dsSR more helpful (4.3 ± 0.7 vs. 3.7 ± 0.8, p < 0.0001) and easier to understand (4.3 ± 0.6 vs. 3.9 ± 0.7, p = 0.0057) (on a scale 0–5, 0 not helpful/very difficult to understand; 5 extremely helpful/very clear to understand). Gynecologic oncologists reported a higher rate of potential to modify their surgical approach based on dsSR (33–42%) compared to sSR (13–17%), p = 0.004.
Conclusions
Disease-specific structured reports were more reliable than simple structured reports in describing key features essential for procedural planning. dsSR was described as more helpful and easier to understand and more likely to lead to modification of the surgical approach by gynecologic oncologists compared to sSR.
Key Points
• Disease-specific structured report is easier to understand and more helpful for planning gynecological surgery as compared with simple structured report.
• Disease-specific structured report for pre-operative evaluation of ovarian cancer provides better documentation of essential features required for surgical planning as compared with simple structured report.
• Disease-specific structured report has the potential to modify the surgical approach as assessed by gynecologic oncologists.



Similar content being viewed by others
Abbreviations
- dsSR:
-
Disease-specific structured reports
- sSR:
-
Simple structured reports
References
Radiology Reporting Templates | RadReport.org. http://www.radreport.org/. Accessed 9 Feb 2017
Morgan TA, Helibrun ME, Kahn CE Jr (2014) Reporting initiative of the Radiological Society of North America: progress and new directions. Radiology 273(3):642–645
Kahn CE Jr, Langlotz CP, Burnside ES et al (2009) Toward best practices in radiology reporting. Radiology 252(3):852–856
Noumeir R (2006) Benefits of the DICOM structured report. J Digit Imaging 19(4):295–306
Kahn CE Jr, Heilbrun ME, Applegate KE (2013) From guidelines to practice: how reporting templates promote the use of radiology practice guidelines. J Am Coll Radiol 10(4):268–273
Travis AR, Sevenster M, Ganesh R, Peters JF, Chang PJ (2014) Preferences for structured reporting of measurement data: an institutional survey of medical oncologists, oncology registrars, and radiologists. Acad Radiol 21(6):785–796
Schwartz LH, Panicek DM, Berk AR, Li Y, Hricak H (2011) Improving communication of diagnostic radiology findings through structured reporting. Radiology 260(1):174–181
Brook OR, Brook A, Vollmer CM, Kent TS, Sanchez N, Pedrosa I (2015) Structured reporting of multiphasic CT for pancreatic cancer: potential effect on staging and surgical planning. Radiology 274(2):464–472
Franconeri A, Fang J, Carney B et al (2018) Structured vs narrative reporting of pelvic MRI for fibroids: clarity and impact on treatment planning. Eur Radiol 28(7):3009–3017
Faggioni L, Coppola F, Ferrari R, Neri E, Regge D (2017) Usage of structured reporting in radiological practice: results from an Italian online survey. Eur Radiol 27(5):1934–1943
Johnson AJ, Chen MY, Swan JS, Applegate KE, Littenberg B (2009) Cohort study of structured reporting compared with conventional dictation. Radiology 253(1):74–80
Langlotz CP (2009) Structured radiology reporting: are we there yet? Radiology 253(1):23–25
Anderson TJT, Lu N, Brook OR (2017) Disease-specific report templates for your practice. J Am Coll Radiol 14(8):1055–1057
Wright AA, Bohlke K, Armstrong DK et al (2016) Neoadjuvant chemotherapy for newly diagnosed, advanced ovarian cancer: Society of Gynecologic Oncology and American Society of Clinical Oncology Clinical Practice Guideline. J Clin Oncol 34(28):3460–3473
Vergote I, Tropé CG, Amant F et al (2010) Neoadjuvant chemotherapy or primary surgery in stage IIIC or IV ovarian cancer. N Engl J Med 363(10):943–953
Kehoe S, Hook J, Nankivell M et al (2015) Primary chemotherapy versus primary surgery for newly diagnosed advanced ovarian cancer (CHORUS): an open-label, randomised, controlled, non-inferiority trial. Lancet 386(9990):249–257
Flusberg M, Ganeles J, Ekinci T et al (2017) Impact of a structured report template on the quality of CT and MRI reports for hepatocellular carcinoma diagnosis. J Am Coll Radiol 14(9):1206–1211
Sverzellati N, Odone A, Silva M et al (2018) Structured reporting for fibrosing lung disease: a model shared by radiologist and pulmonologist. Radiol Med 123(4):245–253
Wildman-Tobriner B, Allen BC, Bashir MR et al (2017) Structured reporting of CT enterography for inflammatory bowel disease: effect on key feature reporting, accuracy across training levels, and subjective assessment of disease by referring physicians. Abdom Radiol (NY) 42(9):2243–2250
Sahdev A (2016) CT in ovarian cancer staging: how to review and report with emphasis on abdominal and pelvic disease for surgical planning. Cancer Imaging 16(1):19
Benedet JL, Bender H, Jones H 3rd, Ngan HY, Pecorelli S (2000) FIGO staging classifications and clinical practice guidelines in the management of gynecologic cancers. FIGO Committee on Gynecologic Oncology. Int J Gynaecol Obstet 70(2):209–262
Nörenberg D, Sommer WH, Thasler W et al (2016) Structured reporting of rectal magnetic resonance imaging in suspected primary rectal cancer: potential benefits for surgical planning and interdisciplinary communication. Invest Radiol 52(4):232–239
Ghoshhajra BB, Lee AM, Ferencik M et al (2013) Interpreting the interpretations: the use of structured reporting improves referring clinicians’ comprehension of coronary CT angiography reports. J Am Coll Radiol 10(6):432–438
Marcovici PA, Taylor GA (2014) Journal Club: structured radiology reports are more complete and more effective than unstructured reports. AJR Am J Roentgenol 203(6):1265–1271
Sistrom CL, Langlotz CP (2005) A framework for improving radiology reporting. J Am Coll Radiol 2(2):159–167
Reiner BI, Knight N, Siegel EL (2007) Radiology reporting, past, present, and future: the radiologist’s perspective. J Am Coll Radiol 4(5):313–319
Timmerman D, Valentin L, Bourne TH et al (2000) Terms, definitions and measurements to describe the sonographic features of adnexal tumors: a consensus opinion from the International Ovarian Tumor Analysis (IOTA) Group. Ultrasound Obstet Gynecol 16(5):500–505
Ellenbogen PH (2013) Imaging 3.0: what is it? J Am Coll Radiol 10(4):229
Bell DS, Greenes RA (1994) Evaluation of UltraSTAR: performance of a collaborative structured data entry system. Proc Annu Symp Comput Appl Med Care:216–222
Amor F, Alcázar JL, Vaccaro H, León M, Iturra A (2011) GI-RADS reporting system for ultrasound evaluation of adnexal masses in clinical practice: a prospective multicenter study. Ultrasound Obstet Gynecol 38(4):450–455
Funding
The authors state that this work has not received any funding.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Guarantor
The scientific guarantor of this publication is Olga Rachel Brook.
Conflict of interest
The authors of this manuscript declare no relationships with any companies, whose products or services may be related to the subject matter of the article.
Statistics and biometry
No complex statistical methods were necessary for this paper.
Informed consent
Written informed consent was waived by the Institutional Review Board.
Ethical approval
Institutional Review Board approval was obtained.
Methodology
• retrospective
• observational
• performed at one institution
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendices
Appendix 1: Sample of a simple structured report at our Institution
EXAMINATION: CT abdomen pelvis with contrast
INDICATION: 38 year old woman with bilateral ovarian masses, elevated CA125. Patient with bilateral ovarian masses worrisome for ovarian carcinoma seen on pelvic ultrasound dated 7/24/2015, elevated CA125 of 388, please evaluate formets.
COMPARISON: None.
FINDINGS:
LOWER CHEST: Visualized lung fields are within normal limits. There is no evidence of pleural or pericardial effusion.
ABDOMEN:
HEPATOBILIARY: The liver demonstrates homogenous attenuation throughout. There is no evidence of focal lesionsThere is no evidence of intrahepatic or extrahepatic biliary dilatation. The gallbladder is within normal limits, without stones or gallbladder wall thickening.
PANCREAS: The pancreas has normal attenuation throughout, without evidence of focal lesions or pancreatic ductal dilatation. There is no peripancreatic stranding.
SPLEEN: The spleen shows normal size and attenuation throughout, without evidence of focal lesions.
ADRENALS: The right and left adrenal glands are normal in size and shape.
URINARY: The kidneys are of normal and symmetric size with normal nephrogram.
There is no evidence of stones, focal renal lesions, or hydronephrosis. There are no urothelial lesions in the kidneys or ureters. There is no perinephric abnormality.
GASTROINTESTINAL: Small bowel loops demonstrate normal caliber, wall thickness and enhancement throughout. The colon and rectum are within normal limits. The appendix is not visualized. There is no evidence of mesenteric lymphadenopathy.
RETROPERITONEUM: There is no evidence of retroperitoneal lymphadenopathy.
VASCULAR: There is no abdominal aortic aneurysm. There is no calcium burden in the abdominal aorta and great abdominal arteries.
PELVIS: The urinary bladder and distal ureters are unremarkable. There is no evidence of pelvic or inguinal lymphadenopathy. There is no free fluid in the pelvis.
REPRODUCTIVE ORGANS: A heterogeneously enhancing soft tissue mass measuring7.7 × 3.9 × 9.5 cm arises from the left adnexa (series 6, image 101, and series 9, image 20). On the right, heterogeneous soft tissue mass measures 3.5 × 2.4 × 3.8 cm (series 6, image 101, and series 9, image 21). Endometrial stripe measures 6 mm.
BONES AND SOFT TISSUES: There is no evidence of worrisome osseous lesions. The abdominal and pelvic wall is within normal limits.
IMPRESSION: 1. No evidence of metastatic disease.
2.Heterogeneously enhancing masses arising from bilateral adnexa measures 7.7× 3.9 × 9.5cm on the left and on the right, 3.5 × 2.4 × 3.8 cm.
Appendix 2: Questionnaire to Gyncecologic oncologists
-
1.
Does this report provide sufficient information for pre-operative staging purposes?

-
2.
Does this report provide sufficient information to make next clinical management decision?

-
3.
Based on this report, if you decide to operate, would you modify your surgical approach?

-
4.
How helpful is this report for surgical planning (1- not helpful, 5 - extremely helpful)?

-
5.
How easy to understand is this report (1 - very difficult, 5 - very clear)?

Rights and permissions
About this article
Cite this article
Franconeri, A., Boos, J., Fang, J. et al. Adnexal mass staging CT with a disease-specific structured report compared to simple structured report. Eur Radiol 29, 4851–4860 (2019). https://doi.org/10.1007/s00330-019-06037-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00330-019-06037-7