Abstract
Background
This study was to develop an algorithm capable of predicting the survival of patients with NSCLC spinal metastasis for individualized therapy.
Methods
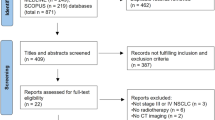
We identified 176 consecutive patients with NSCLC spinal metastasis between 2006 and 2017. Twenty-four features, including age, gender, smoking, KPS, paralysis, histological subtype, tumor stage, surgery, EGFR status, CEA, CA125, CA19-9, NSE, SCC, CYFRA21-1, calcium, AKP, albumin, the number of spinal, extra-spinal bone and visceral metastasis, time to metastasis, pathological fracture, and primary or secondary metastasis, were retrospectively analyzed. Features associated with survival in the multivariate analyses were included in a scoring model, which was prospectively validated in another 63 patients (NCT03363685).
Results
The median follow-up period was 12.00 months (interquartile range 6.00–23.40 months). One hundred forty-seven patients died during follow-up, with a median survival of 13.6 months being observed. Multivariate analysis revealed that the following features were associated with survival: age, smoking, CA125, SCC, KPS, and EGFR status. A scoring system based on these features was created to stratify patients into low-risk (0–3), intermediate-risk (4–6) and high-risk (7–10) groups, whose estimated median survival times 29.10, 10.40 and 3.90 months, respectively. The Harrell’s c-index was 0.72. Model validation supported this model’s validity and reproducibility.
Conclusions
In patients with NSCLC spinal metastasis, survival was associated with age, smoking, CA125, SCC, KPS, and EGFR status. A validated scoring system based on these features was devised that can predict the survival times of those patients. This scoring system provides a basis for applying the NOMS framework and for facilitating individual treatment.



Similar content being viewed by others
References
Siegel RL, Miller KD, Jemal A (2017) Cancer statistics. CA Cancer J Clin 67(1):7–30. https://doi.org/10.3322/caac.21387
Utzschneider S, Wicherek E, Weber P et al (2011) Surgical treatment of bone metastases in patients with lung cancer. Int Orthop 35(5):731–736. https://doi.org/10.1007/s00264-010-1074-9
Dohzono S, Sasaoka R, Takamatsu K et al (2017) Overall survival and prognostic factors in patients with spinal metastases from lung cancer treated with and without epidermal growth factor receptor tyrosine kinase inhibitors. Int J Clin Oncol 22(4):698–705. https://doi.org/10.1007/s10147-017-1116-z
Hessler C, Vettorazzi E, Madert J et al (2011) Actual and predicted survival time of patients with spinal metastases of lung cancer: evaluation of the robustness of the Tokuhashi score. Spine (Phila Pa 1976) 36(12):983–989. https://doi.org/10.1097/brs.0b013e3181e8f7f8
Tokuhashi Y, Matsuzaki H, Toriyama S et al (1990) Scoring system for the preoperative evaluation of metastatic spine tumor prognosis. Spine (Phila Pa 1976) 15(11):1110–1113
Tomita K, Kawahara N, Kobayashi T et al (2001) Surgical strategy for spinal metastases. Spine (Phila Pa 1976) 26(3):298–306
Bauer HC, Wedin R (1995) Survival after surgery for spinal and extremity metastases. Prognostication in 241 patients. Acta Orthop Scand 66(2):143–146
van der Linden YM, Dijkstra SP, Vonk EJ et al (2005) Prediction of survival in patients with metastases in the spinal column: results based on a randomized trial of radiotherapy. Cancer 103(2):320–328. https://doi.org/10.1002/cncr.20756
Rades D, Dunst J, Schild SE (2008) The first score predicting overall survival in patients with metastatic spinal cord compression. Cancer 112(1):157–161. https://doi.org/10.1002/cncr.23150
Katagiri H, Takahashi M, Wakai K et al (2005) Prognostic factors and a scoring system for patients with skeletal metastasis. J Bone Jt Surg Br 87(5):698–703. https://doi.org/10.1302/0301-620x.87b5.15185
Tokuhashi Y, Matsuzaki H, Oda H et al (2005) A revised scoring system for preoperative evaluation of metastatic spine tumor prognosis. Spine (Phila Pa 1976) 30(19):2186–2191
Zoccali C, Skoch J, Walter CM et al (2016) The Tokuhashi score: effectiveness and pitfalls. Eur Spine J 25(3):673–678. https://doi.org/10.1007/s00586-015-4339-6
Crnalic S, Lofvenberg R, Bergh A et al (2012) Predicting survival for surgery of metastatic spinal cord compression in prostate cancer: a new score. Spine (Phila Pa 1976) 37(26):2168–2176. https://doi.org/10.1097/brs.0b013e31826011bc
Rades D (2012) A validated survival score for patients with metastatic spinal cord compression from non-small cell lung cancer. BMC Cancer 12(1):302
Lei M, Liu Y, Liu S et al (2016) Individual strategy for lung cancer patients with metastatic spinal cord compression. Eur J Surg Oncol 42(5):728–734
Wong DA, Fornasier VL, Macnab I et al (1990) Spinal metastases: the obvious, the occult, and the impostors. Spine (Phila Pa 1976) 15(1):1–4
Laufer I, Rubin DG, Lis E et al (2013) The NOMS framework: approach to the treatment of spinal metastatic tumors. Oncologist 18(6):744–751. https://doi.org/10.1634/theoncologist.2012-0293
Warren GW, Sobus S, Gritz ER (2014) The biological and clinical effects of smoking by patients with cancer and strategies to implement evidence-based tobacco cessation support. Lancet Oncol 15(12):e568–580. https://doi.org/10.1016/s1470-2045(14)70266-9
Dearden S, Stevens J, Wu YL et al (2013) Mutation incidence and coincidence in non small-cell lung cancer: meta-analyses by ethnicity and histology (mutMap). Ann Oncol 24(9):2371–2376. https://doi.org/10.1093/annonc/mdt205
Cedres S, Nunez I, Longo M et al (2011) Serum tumor markers CEA, CYFRA21-1, and CA-125 are associated with worse prognosis in advanced non-small-cell lung cancer (NSCLC). Clin Lung Cancer 12(3):172–179. https://doi.org/10.1016/j.cllc.2011.03.019
Ogihara S, Seichi A, Hozumi T et al (2006) Prognostic factors for patients with spinal metastases from lung cancer. Spine 31(14):1585
Harrell FE, Califf RM, Pryor DB et al (1982) Evaluating the yield of medical tests. JAMA 247(18):2543–2546
Wessler BS, Ruthazer R, Udelson JE et al (2017) Regional validation and recalibration of clinical predictive models for patients with acute heart failure. J Am Heart Assoc Cardiovasc Cerebrovasc Dis 6(11):e006121
Lee A, Mu JL, Joynt GM et al (2017) Risk prediction models for delirium in the intensive care unit after cardiac surgery: a systematic review and independent external validation. Br J Anaesth 118(3):391–399
Siontis GCM, Tzoulaki I, Castaldi PJ et al (2015) External validation of new risk prediction models is infrequent and reveals worse prognostic discrimination. J Clin Epidemiol 68(1):25–34
O’Brien RM (2007) A caution regarding rules of thumb for variance inflation factors. Qual Quant 41(5):673–690
Molina JR, Yang P, Cassivi SD et al (2008) Non-small cell lung cancer: epidemiology, risk factors, treatment, and survivorship. Mayo Clin Proc 83(5):584–594. https://doi.org/10.4065/83.5.584
Ettinger DS, Wood DE, Aisner DL et al (2017) Non-small cell lung cancer, Version 5.2017, NCCN clinical practice guidelines in oncology. J Nat Compr Cancer Netw JNCCN 15(4):504–535
Reck M, Rabe KF (2017) Precision diagnosis and treatment for advanced non-small-cell lung cancer. N Engl J Med 377(9):849–861. https://doi.org/10.1056/NEJMra1703413
Spratt DE, Beeler WH, de Moraes FY (2017) An integrated multidisciplinary algorithm for the management of spinal metastases: an International Spine Oncology Consortium report. Lancet Oncol 18(12):e720
Tokuhashi Y, Uei H, Oshima M (2014) Scoring system for prediction of metastatic spine tumor prognosis. World J Orthop 5(3):262–271. https://doi.org/10.5312/wjo.v5.i3.262
Fisher CG, Dipaola CP, Ryken TC (2010) A novel classification system for spinal instability in neoplastic disease: an evidence-based approach and expert consensus from the Spine Oncology Study Group. Spine 35(22):1221–1229
Bilsky MH, Laufer I, Fourney DR et al (2010) Reliability analysis of the epidural spinal cord compression scale. J Neurosurg Spine 13(3):324
Cataldo VD, Gibbons DL, Perez-Soler R, Quintas-Cardama A (2011) Treatment of non-small-cell lung cancer with erlotinib or gefitinib. N Engl J Med 364(10):947–955. https://doi.org/10.1056/NEJMct0807960
Dohzono S, Sasaoka R, Takamatsu K et al (2017) Overall survival and prognostic factors in patients with spinal metastases from lung cancer treated with and without epidermal growth factor receptor tyrosine kinase inhibitors. Int J Clin Oncol 22(2):1–8
Shepherd FA, Pereira J, Ciuleanu TE et al (2004) A randomized placebo-controlled trial of erlotinib in patients with advanced non-small cell lung cancer (NSCLC) following failure on 1st line or 2nd line chemotherapy: a National Cancer Institute of Canada Clinical Trials Group (NCIC CTG) trial [abstract 7022]. J Clin Oncol 22(14s):622s
National Center for Chronic Disease P, Health Promotion Office on S, Health (2014) Reports of the surgeon general. In: The health consequences of smoking-50 years of progress: a report of the surgeon general. Centers for Disease Control and Prevention (US), Atlanta (GA)
Nakamura H, Nishimura T (2017) History, molecular features, and clinical importance of conventional serum biomarkers in lung cancer. Surg Today 47(9):1037–1059. https://doi.org/10.1007/s00595-017-1477-y
Owonikoko TK, Ragin CC, Belani CP, Oton AB, Gooding WE, Taioli E, Ramalingam SS (2007) Lung cancer in elderly patients: an analysis of the surveillance, epidemiology, and end results database. J Clin Oncol 25(35):5570
Acknowledgements
This research was supported by the Shanghai Science and Technology Committee (Grant No. 17411950300, 17411950303).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
About this article
Cite this article
Zang, S., He, Q., Bao, Q. et al. Establishment and validation of a novel survival prediction scoring algorithm for patients with non-small-cell lung cancer spinal metastasis. Int J Clin Oncol 24, 1049–1060 (2019). https://doi.org/10.1007/s10147-019-01452-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10147-019-01452-8