Abstract
Background
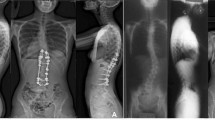
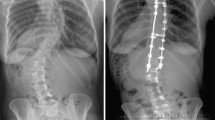
The current classifications of adolescent idiopathic scoliosis (AIS) aim to guide surgical decision making. However, variance exists within treatment recommendations and suboptimal outcomes have been observed while following these guidelines based on two-dimensional images. We used previously developed 3D classification for right thoracic AIS patients and aimed to determine the variation in surgical decision making and the risk of suboptimal outcomes in each subtype according to our classification.
Methods
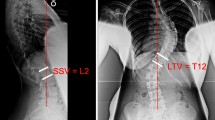
Seventy-six right thoracic AIS patients with 2-year follow-up were included retrospectively. Five 3D preoperative subgroups were determined based on a previous classification system. The upper and lower instrumented vertebrae (UIV and LIV) and the radiographic surgical outcomes at 2-year [frontal balance (FB), proximal junctional kyphosis (PJK), and adding on] were compared between the subtypes.
Results
The fusion length and the rate of radiographic suboptimal outcomes were statistically different between the five groups. LIV at T12 in Type 1 and UIV at T2 in Type 2 were associated with improved FB and lower PJK, respectively. Type 3 had the highest rate of suboptimal FB and developing PJK. Type 4 had the longest fusion, and suboptimal FB was observed in 42% of the patients independent from the LIV level. Type 5 had the lowest rate of unsatisfactory radiographic outcomes at 2 years.
Conclusion
Following the preoperative 3D classification of the AIS patients, we showed that the UIV and LIV selection has a different impact on the surgical outcomes in each of the five subtypes. The proposed 3D classification has the potential for risk stratification following a posterior spinal surgery in right thoracic AIS.
Graphic abstract
These slides can be retrieved under Electronic Supplementary Material.







Similar content being viewed by others
References
Pasha S, Flynn J (2018) Data-driven classification of the 3D spinal curve in adolescent idiopathic scoliosis with an applications in surgical outcome prediction. Sci Rep 8:16296. https://doi.org/10.1038/s41598-018-34261-6
Lenke LG, Betz RR, Harms J, Bridwell KH, Clements DH, Lowe TG, Blanke K (2001) Adolescent idiopathic scoliosis: a new classification to determine extent of spinal arthrodesis. J Bone Joint Surg Am 83-A:1169–1181
Kadoury S, Labelle H (2012) Classification of three-dimensional thoracic deformities in adolescent idiopathic scoliosis from a multivariate analysis. Eur Spine J 21:40–49. https://doi.org/10.1007/s00586-011-2004-2
Abelin-Genevois K, Sassi D, Verdun S, Roussouly P (2018) Sagittal classification in adolescent idiopathic scoliosis: original description and therapeutic implications. Eur Spine J. https://doi.org/10.1007/s00586-018-5613-1
King HA, Moe JH, Bradford DS, Winter RB (1983) The selection of fusion levels in thoracic idiopathic scoliosis. J Bone Joint Surg Am 65:1302–1313
Chang KW, Leng X, Zhao W, Chen YY, Chen TC, Chang KI (2011) Broader curve criteria for selective thoracic fusion. Spine (Phila Pa 1976) 36:1658 1664. https://doi.org/10.1097/BRS.0b013e318215fa73
Pasha S, Flynn JM, Sankar WN (2018) Outcomes of selective thoracic fusion for Lenke 1 adolescent idiopathic scoliosis: predictors of success from the sagittal plane. Eur Spine J. https://doi.org/10.1007/s00586-018-5553-9
Stokes IA, Sangole AP, Aubin CE (2009) Classification of scoliosis deformity three-dimensional spinal shape by cluster analysis. Spine (Phila Pa 1976) 34:584–590. https://doi.org/10.1097/BRS.0b013e318190b914
Pasha S, Hassanzadeh P, Ecker M, Ho V (2019) A hierarchical classification of adolescent idiopathic scoliosis: Identifying the distinguishing features in 3D spinal deformities. PLoS ONE 14:e0213406. https://doi.org/10.1371/journal.pone.0213406
Pasha S, Cahill PJ, Dormans JP, Flynn JM (2016) Characterizing the differences between the 2D and 3D measurements of spine in adolescent idiopathic scoliosis. Eur Spine J 25:3137–3145. https://doi.org/10.1007/s00586-016-4582-5
Pasha S, Ecker M, Deeney V (2018) Considerations in sagittal evaluation of the scoliotic spine. Eur J Orthop Surg Traumatol 28:1039–1045. https://doi.org/10.1007/s00590-018-2175-1
DeFrancesco CJ, Pasha S, Miller DJ, Betz RR, Clements DH, Fletcher ND, Glotzbecker MG, Hwang SW, Kelly MP, Lehman RA, Lonner BS, Newton PO, Roye BD, Sponseller PD, Upasani VV, Harms Study G, Cahill PJ (2018) Agreement between manual and computerized designation of neutral vertebra in idiopathic scoliosis. Spine Deform 6:644–650. https://doi.org/10.1016/j.jspd.2018.03.001
Rose PS, Lenke LG (2007) Classification of operative adolescent idiopathic scoliosis: treatment guidelines. Orthop Clin North Am 38(521–529):vi. https://doi.org/10.1016/j.ocl.2007.06.001
Pasha S, Baldwin K (2018) Are we simplifying balance evaluation in adolescent idiopathic scoliosis? Clin Biomech (Bristol, Avon) 51:91–98. https://doi.org/10.1016/j.clinbiomech.2017.11.011
Kim YJ, Lenke LG, Bridwell KH, Kim J, Cho SK, Cheh G, Yoon J (2007) Proximal junctional kyphosis in adolescent idiopathic scoliosis after 3 different types of posterior segmental spinal instrumentation and fusions: incidence and risk factor analysis of 410 cases. Spine (Phila Pa 1976) 32:2731–2738. https://doi.org/10.1097/BRS.0b013e31815a7ead
Helgeson MD, Shah SA, Newton PO, Clements DH 3rd, Betz RR, Marks MC, Bastrom T, Harms Study G (2010) Evaluation of proximal junctional kyphosis in adolescent idiopathic scoliosis following pedicle screw, hook, or hybrid instrumentation. Spine (Phila Pa 1976) 35:177–181. https://doi.org/10.1097/BRS.0b013e3181c77f8c
Wang Y, Hansen ES, Hoy K, Wu C, Bunger CE (2011) Distal adding-on phenomenon in Lenke 1A scoliosis: risk factor identification and treatment strategy comparison. Spine (Phila Pa 1976) 36:1113–1122. https://doi.org/10.1097/BRS.0b013e3181f51e95
Lakhal W, Loret JE, de Bodman C, Fournier J, Bergerault F, de Courtivron B, Bonnard C (2014) The progression of lumbar curves in adolescent Lenke 1 scoliosis and the distal adding-on phenomenon. Orthop Traumatol Surg Res 100:S249–254. https://doi.org/10.1016/j.otsr.2014.03.012
Pasha S, Baldwin K (2019) Preoperative sagittal spinal profile of adolescent idiopathic scoliosis lenke types and non-scoliotic adolescents: a systematic review and meta-analysis. Spine (Phila Pa 1976) 44:134–142. https://doi.org/10.1097/BRS.0000000000002748
Cammarata M, Aubin CE, Wang X, Mac-Thiong JM (2014) Biomechanical risk factors for proximal junctional kyphosis: a detailed numerical analysis of surgical instrumentation variables. Spine (Phila Pa 1976) 39:E500–E507. https://doi.org/10.1097/BRS.0000000000000222
Ilharreborde B (2018) Sagittal balance and idiopathic scoliosis: does final sagittal alignment influence outcomes, degeneration rate or failure rate? Eur Spine J 27:48–58. https://doi.org/10.1007/s00586-018-5472-9
Pasha S, Ilharreborde B, Baldwin K (2019) Sagittal spinopelvic alignment after posterior spinal fusion in adolescent idiopathic scoliosis: a systematic review and meta-analysis. Spine (Phila Pa 1976) 44:41–52. https://doi.org/10.1097/BRS.0000000000002736
Pasha S, Aubin CE, Labelle H, Parent S, Mac-Thiong JM (2015) The biomechanical effects of spinal fusion on the sacral loading in adolescent idiopathic scoliosis. Clin Biomech (Bristol, Avon) 30:981–987. https://doi.org/10.1016/j.clinbiomech.2015.06.019
Pasha S, Smith L, Sankar WN (2019) Bone remodeling and disc morphology in the distal unfused spine after spinal fusion in adolescent idiopathic scoliosis. Spine Deform 7(5):746–753
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Pasha, S., Baldwin, K. Surgical outcome differences between the 3D subtypes of right thoracic adolescent idiopathic scoliosis. Eur Spine J 28, 3076–3084 (2019). https://doi.org/10.1007/s00586-019-06145-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-019-06145-4