Abstract
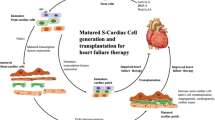
Stem cells provide a new strategy for the treatment of cardiac diseases; however, their effectiveness in dilated cardiomyopathy (DCM) has not been investigated. In this study, cardiosphere-derived cells (CDCs) were isolated from infants (≤ 24 months) and identified by the cell surface markers CD105, CD90, CD117 and CD45, which is consistent with a previous report, although increased CD34 expression was observed. The molecular expression profile of CDCs from infants was determined by RNA sequencing and compared with adult CDCs, showing that infant CDCs have almost completely altered gene expression patterns compared with adult CDCs. The upregulated genes in infant CDCs are mainly related to the biological processes of cell morphogenesis and differentiation. The molecular profile of infant CDCs was characterized by lower expression of inflammatory cytokines and higher expression of stem cell markers and growth factors compared to adult CDCs. After intramyocardial administration of infant CDCs in the heart of DCM rats, we found that infant CDCs remained in the heart of DCM rats for at least 7 days, improved DCM-induced cardiac function impairment and protected the myocardium by elevating the left ventricular ejection fraction and fraction shortening. However, the effectiveness of transplanted CDCs was reversed later, as increased fibrosis formation instead of angiogenesis was observed. We concluded that infant CDCs, with higher expression of stem cell markers and growth factors, exhibit non-durable heart protection due to limited residence time in the heart of DCM animals, suggesting that multiple administrations of the CDCs or post-regulation after transplantation may be the key for cell therapy in the future.


Similar content being viewed by others
Abbreviations
- CDCs:
-
Cardiosphere-derived cells
- DCM:
-
Dilated cardiomyopathy
- GEO:
-
Gene expression omnibus
- CSps:
-
Explant-derived cardiospheres
- LVEF:
-
Left ventricular ejection fraction
- LVFS:
-
Left ventricular fractional shortening
- LVEDD:
-
Left ventricular end-diastolic diameter
- LVESD:
-
Left ventricular end-systolic diameter
- LVEDV:
-
Left ventricular end-diastolic volume
- LVESV:
-
Left ventricular end-systolic volume
- TOF:
-
Tetralogy of Fallot
- PA:
-
Pulmonary atresia
- PS:
-
Pulmonary stenosis
References
Aminzadeh MA, Tseliou E, Sun B, Cheng K, Malliaras K, Makkar RR, Marban E (2015) Therapeutic efficacy of cardiosphere-derived cells in a transgenic mouse model of non-ischaemic dilated cardiomyopathy. Eur Heart J 36:751–762. https://doi.org/10.1093/eurheartj/ehu196
Cambier L, Giani JF, Liu W, Ijichi T, Echavez AK, Valle J, Marban E (2018) Angiotensin ii-induced end-organ damage in mice is attenuated by human exosomes and by an exosomal Y RNA fragment. Hypertension 72:370–380. https://doi.org/10.1161/hypertensionaha.118.11239
de Couto G, Liu W, Tseliou E, Sun B, Makkar N, Kanazawa H, Arditi M, Marban E (2015) Macrophages mediate cardioprotective cellular postconditioning in acute myocardial infarction. J Clin Invest 125:3147–3162. https://doi.org/10.1172/jci81321
Frangogiannis NG (2015) Emerging roles for macrophages in cardiac injury: cytoprotection, repair, and regeneration. J Clin Invest 125:2927–2930. https://doi.org/10.1172/jci83191
Gallet R, de Couto G, Simsolo E, Valle J, Sun B, Liu W, Tseliou E, Zile MR, Marban E (2016) Cardiosphere-derived cells reverse heart failure with preserved ejection fraction (hfpef) in rats by decreasing fibrosis and inflammation. JACC Basic Transl Sci 1:14–28. https://doi.org/10.1016/j.jacbts.2016.01.003
Harvey E, Zhang H, Sepulveda P, Garcia SP, Sweeney D, Choudry FA, Castellano D, Thomas GN, Kattach H, Petersen R, Blake DJ, Taggart DP, Frontini M, Watt SM, Martin-Rendon E (2017) Potency of human cardiosphere-derived cells from patients with ischemic heart disease is associated with robust vascular supportive ability. Stem Cells Transl Med 6:1399–1411. https://doi.org/10.1002/sctm.16-0229
Hensley MT, Tang J, Woodruff K, Defrancesco T, Tou S, Williams CM, Breen M, Meurs K, Keene B, Cheng K (2017) Intracoronary allogeneic cardiosphere-derived stem cells are safe for use in dogs with dilated cardiomyopathy. J Cell Mol Med 21:1503–1512. https://doi.org/10.1111/jcmm.13077
Ishigami S, Ohtsuki S, Eitoku T, Ousaka D, Kondo M, Kurita Y, Hirai K, Fukushima Y, Baba K, Goto T, Horio N, Kobayashi J, Kuroko Y, Kotani Y, Arai S, Iwasaki T, Sato S, Kasahara S, Sano S, Oh H (2017) Intracoronary cardiac progenitor cells in single ventricle physiology: The perseus (cardiac progenitor cell infusion to treat univentricular heart disease) randomized phase 2 trial. Circ Res 120:1162–1173. https://doi.org/10.1161/circresaha.116.310253
Kasai-Brunswick TH, Costa AR, Barbosa RA, Farjun B, Mesquita FC, Silva Dos Santos D, Ramos IP, Suhett G, Brasil GV, Cunha ST, Brito JO, Passipieri JD, Carvalho AB, Campos de Carvalho AC (2017) Cardiosphere-derived cells do not improve cardiac function in rats with cardiac failure. Stem Cell Res Ther 8:36. https://doi.org/10.1186/s13287-017-0481-x
Kopecky SL, Gersh BJ (1987) Dilated cardiomyopathy and myocarditis: natural history, etiology, clinical manifestations, and management. Curr Probl Cardiol 12:569–647
Lapchak PA, Boitano PD, de Couto G, Marban E (2018) Intravenous xenogeneic human cardiosphere-derived cell extracellular vesicles (exosomes) improves behavioral function in small-clot embolized rabbits. Exp Neurol 307:109–117. https://doi.org/10.1016/j.expneurol.2018.06.007
Lo CY, Weil BR, Palka BA, Momeni A, Canty JM Jr, Neelamegham S (2016) Cell surface glycoengineering improves selectin-mediated adhesion of mesenchymal stem cells (mscs) and cardiosphere-derived cells (cdcs): pilot validation in porcine ischemia-reperfusion model. Biomaterials 74:19–30. https://doi.org/10.1016/j.biomaterials.2015.09.026
Makkar RR, Smith RR, Cheng K, Malliaras K, Thomson LE, Berman D, Czer LS, Marban L, Mendizabal A, Johnston PV, Russell SD, Schuleri KH, Lardo AC, Gerstenblith G, Marban E (2012) Intracoronary cardiosphere-derived cells for heart regeneration after myocardial infarction (caduceus): a prospective, randomised phase 1 trial. Lancet 379:895–904. https://doi.org/10.1016/s0140-6736(12)60195-0
Middleton RC, Fournier M, Xu X, Marban E, Lewis MI (2017) Therapeutic benefits of intravenous cardiosphere-derived cell therapy in rats with pulmonary hypertension. PLoS ONE 12:e0183557. https://doi.org/10.1371/journal.pone.0183557
Mishra R, Vijayan K, Colletti EJ, Harrington DA, Matthiesen TS, Simpson D, Goh SK, Walker BL, Almeida-Porada G, Wang D, Backer CL, Dudley SC Jr, Wold LE, Kaushal S (2011) Characterization and functionality of cardiac progenitor cells in congenital heart patients. Circulation 123:364–373. https://doi.org/10.1161/circulationaha.110.971622
Nana-Leventaki E, Nana M, Poulianitis N, Sampaziotis D, Perrea D, Sanoudou D, Rontogianni D, Malliaras K (2019) Cardiosphere-derived cells attenuate inflammation, preserve systolic function, and prevent adverse remodeling in rat hearts with experimental autoimmune myocarditis. J Cardiovasc Pharmacol Ther 24:70–77. https://doi.org/10.1177/1074248418784287
Silva JN, Canter CE (2010) Current management of pediatric dilated cardiomyopathy. Curr Opin Cardiol 25:80–87. https://doi.org/10.1097/HCO.0b013e328335b220
Simpson DL, Mishra R, Sharma S, Goh SK, Deshmukh S, Kaushal S (2012) A strong regenerative ability of cardiac stem cells derived from neonatal hearts. Circulation 126:S46–53. https://doi.org/10.1161/circulationaha.111.084699
Smith RR, Barile L, Cho HC, Leppo MK, Hare JM, Messina E, Giacomello A, Abraham MR, Marban E (2007) Regenerative potential of cardiosphere-derived cells expanded from percutaneous endomyocardial biopsy specimens. Circulation 115:896–908. https://doi.org/10.1161/circulationaha.106.655209
Suzuki G, Weil BR, Leiker MM, Ribbeck AE, Young RF, Cimato TR, Canty JM Jr (2014) Global intracoronary infusion of allogeneic cardiosphere-derived cells improves ventricular function and stimulates endogenous myocyte regeneration throughout the heart in swine with hibernating myocardium. PLoS ONE 9:e113009. https://doi.org/10.1371/journal.pone.0113009
Tavazzi L (1997) Epidemiology of dilated cardiomyopathy: a still undetermined entity. Eur Heart J 18:4–6. https://doi.org/10.1093/oxfordjournals.eurheartj.a015116
Towbin JA, Lowe AM, Colan SD, Sleeper LA, Orav EJ, Clunie S, Messere J, Cox GF, Lurie PR, Hsu D, Canter C, Wilkinson JD, Lipshultz SE (2006) Incidence, causes, and outcomes of dilated cardiomyopathy in children. JAMA 296:1867–1876. https://doi.org/10.1001/jama.296.15.1867
Walravens AS, Vanhaverbeke M, Ottaviani L, Gillijns H, Trenson S, Driessche NV, Luttun A, Meyns B, Herijgers P, Rega F, Heying R, Sampaolesi M, Janssens S (2018) Molecular signature of progenitor cells isolated from young and adult human hearts. Sci Rep 8:9266. https://doi.org/10.1038/s41598-018-26969-2
Acknowledgements
We sincerely thank the Heart Center, Guangzhou Women and Children’s Medical Center for the surgical assistance. We also thank the Nature Science Foundation of China (No. 81670262), the Guangzhou Lingnan Yingjie Project and start-up funding from Guangzhou Women and Children’s Medical Center.
Funding
This work was funded by the Nature Science Foundation of China (No. 81670262), the Guangzhou Lingnan Yingjie Project and the start-up funding from Guangzhou Women and Children’s Medical Center.
Author information
Authors and Affiliations
Contributions
SW, WC, LM and MZ performed this experiment. XC and JD designed the study and wrote the main manuscript. WD and HY collected the data and analysed the results. LS reviewed the data and prepared the pictures. All authors read and approved the final manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare.
Ethical approval
The study was approved by the Animal Ethics Committee of Guangzhou Medical University (G2017-080).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Supplement Table 1
Detailed clinical information of the infant donors for CDCs isolation (data from the Heart Center of Guangzhou Women and Children Medical Center). (PDF 575 kb)
Supplement Table 2
Reported expression of cell surface markers on CDCs isolated from patients of different ages and the effect of CDCs in vivo after transplantation. References are listed in the last column. (PDF 196 kb)
Supplement Figure 3
(a-b) Expression of cell surface markers of infant CDCs by flow cytometry (a) after multiple generation culture and (b) after cryopreservation. (All graphs show the mean±S.E.M. *p<0.05, n=3). (PDF 164 kb)
Rights and permissions
About this article
Cite this article
Wang, S., Chen, W., Ma, L. et al. Infant cardiosphere-derived cells exhibit non-durable heart protection in dilated cardiomyopathy rats. Cytotechnology 71, 1043–1052 (2019). https://doi.org/10.1007/s10616-019-00328-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10616-019-00328-z