Abstract
Objectives
This study evaluated the cytotoxicity of resin-based luting cements on fibroblast cells using different polymerization protocols.
Materials and methods
Two conventional dual-polymerized (RelyX ARC, VariolinkN) and two self-adhesive resin cements (RelyX Unicem, Multilink Speed) specimens were polymerized using four different polymerization protocols: (a) photo-polymerization with direct light application, (b) photo-polymerization over ceramic and (c) resin nano-ceramic discs and (d) auto-polymerization. The specimens were then assigned to four groups to test cytotoxicity at 0, 1, 2 and 7 preincubation days (n = 5). MTT test was performed using NIH/3T3 fibroblast cells. Data were analysed using three- and one-way ANOVA. Multiple comparisons were made using Bonferroni post hoc test (p < 0.05).
Results
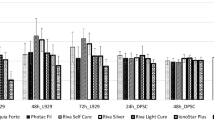
The highest cytotoxic values were recorded at day 2 for conventional resin cements and at day 0 for self-adhesive resin cements. Self-adhesive resin cements showed the most cytotoxic effect at the second day, while conventional resin cements presented immediate cytotoxicity. Auto-polymerized resin specimens and especially Multilink Speed demonstrated the most cytotoxic effect regardless of the preincubation time. Cytotoxicity of cements tested reached the lowest level at day 7. Interposition of ceramic or nano-ceramic restorative material did not significantly affect the cytotoxicity of tested luting cements (p > 0.05).
Conclusions
Cytotoxicity of dual-polymerized resin cements was material-dependent and decreased gradually up to 7 days. Photo-polymerization plays an important role in reducing the cytotoxic effects.
Clinical relevance
When luting ceramic or resin nano-ceramic restorations of which thickness does not exceed 2 mm, the level of cytotoxicity with the tested materials is not significant. Luting of restorative materials that do not allow for light transmission such as metal-fused porcelain, clinicians should be cautious in the use of dual-polymerized conventional resin cements as only auto-polymerization of resin cements takes place under such materials.



Similar content being viewed by others
References
Costa CA, Hebling J, Randall RC (2006) Human pulp response to resin cements used to bond inlay restorations. Dent Mater 22:954–962
Ulker HE, Sengun A (2009) Cytotoxicity evaluation of self-adhesive composite resin cements by dentin barrier test on 3D pulp cells. Eur J Dent 3:120–126
da Fonseca Roberti Garcia L, Pontes EC, Basso FG, Hebling J, Souza Costa CA, Soares DG (2016) Transdentinal cytotoxicity of resin-based luting cements to pulp cells. Clin Oral Investig 20:1559–1566
Trumpaite-Vanagiene R, Bukelskiene V, Aleksejuniene J, Puriene A, Baltriukiene D, Rutkunas V (2015) Cytotoxicity of commonly used luting cements —an in vitro study. Dent Mater J 34:294–301
Bakopoulou A, Papadopoulos T, Garefis P (2009) Molecular toxicology of substances released from resin-based dental restorative materials. Int J Mol Sci 10:3861–3899
Schmid-Schwap M, Franz A, König F, Bristela M, Lucas T, Piehslinger E, Watts DC, Schedle A (2009) Cytotoxicity of four categories of dental cements. Dent Mater 25:360–368
Pontes EC, Soares DG, Hebling J, Costa CA (2014) Cytotoxicity of resin-based luting cements to pulp cells. Am J Dent 27:237–244
D'Alpino PHP, Moura GEDD, Barbosa SCA, Marques LA, Eberlin MN, Nascimento FD, Tersariol ILDS (2017) Differential cytotoxic effects on odontoblastic cells induced by self-adhesive resin cements as a function of the activation protocol. Dent Mater 33:1402–1415
Moraes RR, Boscato N, Jardim PS, Schneider LF (2011) Dual and self-curing potential of self-adhesive resin cements as thin films. Oper Dent 36:635–642
Acquaviva PA, Cerutti F, Adami G, Gagliani M, Ferrari M, Gherlone E, Cerutti A (2009) Degree of conversion of three composite materials employed in the adhesive cementation of indirect restorations: a micro-Raman analysis. J Dent 37:610–615
Aguiar TR, Francescantonio MD, Arrais CAG, Ambrosano GMB, Davanzo C, Giannin M (2010) Influence of curing mode and time on degree of conversion of one composite and two self-adhesive resin cements. Oper Dent 35:295–299
Ayres AP, Andre CB, Pacheco RR, Carvalho AO, Bacelar-Sá RC, Rueggeberg FA, Giannini M (2015) Indirect restoration thickness and time after light-activation effects on degree of conversion of resin cement. Braz Dent J 26:363–367
Vrochari AD, Eliades G, Hellwig E, Wrbas KT (2009) Curing efficiency of four self-etching, self-adhesive resin cements. Dent Mater 25:1104–1108
Monteiro GQ, Souza FB, Pedrosa RF, Sales GC, Castro CM, Fraga SN, Galvão BH, Braz R (2010) In vitro biological respons to a self-adhesive resin cement under different curing strategies. J Biomed Mater Res B Appl Biomater 92:317–321
Monticelli F, Osorio R, Mazzitelli C, Ferrari M, Toledano M (2008) Limited decalcification/diffusion of self-adhesive cements into dentin. J Dent Res 87:974–979
Hitz T, Stawarczyk B, Fischer J, Hämmerle CH, Sailer I (2012) Are self-adhesive resin cements a valid alternative to conventional resin cements? A laboratory study of the long-term bond strength. Dent Mater 28:1183–1190
Lisboa DS, Santos SV, Griza S, Rodrigues JL, Faria-E-Silva AL (2013) Dentin deproteinization effect on bond strength of self-adhesive resin cements. Braz Oral Res 27:73–75
Dos Santos VH, Griza S, de Moraes RR, Faria-E-Silva AL (2014) Bond strength of self-adhesive resin cements to composite submitted to different surface pretreatments. Restor Dent Endod 39:12–16
Almeida CM, Meereis CTW, Leal FB, Ogliari AO, Piva E, Ogliari FA (2018) Evaluation of long-term bond strength and selected properties of self-adhesive resin cements. Braz Oral Res 1(32):e15
Ergun G, Egilmez F, Yilmaz S (2011) Effect of reduced exposure times on the cytotoxicity of resin luting cements cured by high-power led. J Appl Oral Sci 19:286–292
Rai Y, Pathak R, Kumari N, Sah DK, Pandey S, Kalra N, Soni R, Dwarakanath BS, Bhatt AN (2018) Mitochondrial biogenesis and metabolic hyperactivation limits the application of MTT assay in the estimation of radiation induced growth inhibition. Sci Rep 24(8):1531
Stockert JC, Horobin RW, Colombo LL, Blázquez-Castro A (2018) Tetrazolium salts and formazan products in cell biology: viability assessment, fluorescence imaging, and labeling perspectives. Acta Histochem 120:159–167
Moharamzadeh K, Brook IM, Van Noort R (2009) Biocompatibility of resin-based dental materials. Materials (Basel) 2:514–548
Toz T, Kiremitçi A, Çakmak AS, Ünsal Tan O, Palaska E, Gümüşderelioğlu M, Özcan M (2017) A comparative study on monomer elution and cytotoxicity of different adhesive restoration. J Adhes Sci Technol 31:414–429
Fontes ST, Fernández MR, Ogliari FA, de Carvalho RV, de Moraes RR, Pinto MB, Piva E (2013) Tetrahydrofuran as solvent in dental adhesives: cytotoxicity and dentin bond stability. Clin Oral Investig 17:237–242
Klein-Júnior CA, Zimmer R, Hentschke GS, Machado DC, Dos Santos RB, Reston EG (2018) Effect of heat treatment on cytotoxicity of self-adhesive resin cements: cell viability analysis. Eur J Dent 12:281–286
Kurt A, Altintas SH, Kiziltas MV, Tekkeli SE, Guler EM, Kocyigit A, Usumez A (2018) Evaluation of residual monomer release and toxicity of self-adhesive resin cements. Dent Mater J 37:40–48
Soares DG, Brito CA, Tavares da Silva RH, Ribeiro AP, Hebling J, Costa CA (2016) Cytocompatibility of HEMA-free resin-based luting cements according to application protocols on dentine surfaces. Int Endod J 49:551–560
International Organization for Standardization (2009) ISO 10993-5 biological evaluation of medical devices-part 5: test for in vitro cytotoxicity. Geneva, Switzerland
Jiang RD, Lin H, Zheng G, Zhang XM, Du Q, Yang M (2017) In vitro dentin barrier cytotoxicity testing of some dental restorative materials. J Dent 58:28–33
Pereira SG, Fulgêncio R, Nunes TG, Toledano M, Osorio R, Carvalho RM (2010) Effect of curing protocol on the polymerization of dual-cured resin cements. Dent Mater 26:710–718
Mendonça AA, Souza PP, Hebling J, Costa CA (2007) Cytotoxic effects of hard-setting cements applied on the odontoblast cell line MDPC-23. Oral Surg Oral Med Oral Pathol Oral Radiol Endod 104:102–108
Altintas SH, Usumez A (2008) Evaluation of monomer leaching from a dual cured resin cement. J Biomed Mater Res B Appl Biomater 86:523–529
Tezvergil-Mutluay A, Lassila LV, Vallittu PK (2007) Degree of conversion of dual-cure luting resins light-polymerized through various materials. Acta Odontol Scand 65:201–205
Nocca G, Iori A, Rossini C, Martorana GE, Ciasca G, Arcovito A, Cordaro M, Lupi A, Marigo L (2015) Effects of barriers on chemical and biological properties of two dual resin cements. Eur J Oral Sci 123:208–214
De Souza G, Braga RR, Cesar PF, Lopes GC (2015) Correlation between clinical performance and degree of conversion of resin cements: a literature review. J Appl Oral Sci 23:358–368
Noronha Filho JD, Brandão NL, Poskus LT, Guimarães JGA, Silva EM (2010) A critical analysis of the degree of conversion of resin-based luting cements. J Appl Oral Sci 18:442–446
Farrugia C, Cassar G, Valdramidis V, Camilleri J (2015) Effect of sterilization techniques prior to antimicrobial testing on physical properties of dental restorative materials. J Dent 43:703–714
Acknowledgements
The authors extend their gratitude to Mr. S.K. Köse, Ankara University, Department of Biostatistics, for his assistance with the statistical analysis.
Funding
This study was supported by Ankara University, Scientific Research Projects Coordination Unit (project no. 14B0234001).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
This article does not contain any studies with living human participants or animals. Institutional approval was given.
Informed consent
Not required.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Oguz, E.I., Hasanreisoglu, U., Uctasli, S. et al. Effect of various polymerization protocols on the cytotoxicity of conventional and self-adhesive resin-based luting cements. Clin Oral Invest 24, 1161–1170 (2020). https://doi.org/10.1007/s00784-019-02980-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00784-019-02980-3