Our official English website, www.x-mol.net, welcomes your feedback! (Note: you will need to create a separate account there.)
Effect of a Strategy of Comprehensive Vasodilation vs Usual Care on Mortality and Heart Failure Rehospitalization Among Patients With Acute Heart Failure
JAMA ( IF 120.7 ) Pub Date : 2019-12-17 , DOI: 10.1001/jama.2019.18598 Nikola Kozhuharov 1, 2 , Assen Goudev 3 , Dayana Flores 1, 2 , Micha T Maeder 4 , Joan Walter 1, 2, 5 , Samyut Shrestha 1, 2, 5 , Danielle Menosi Gualandro 1, 2, 6 , Mucio Tavares de Oliveira Junior 6 , Zaid Sabti 1, 2 , Beat Müller 7 , Markus Noveanu 1, 2 , Thenral Socrates 1, 2, 8 , Ronny Ziller 1, 2 , Antoni Bayés-Genís 9 , Alessandro Sionis 10 , Patrick Simon 11 , Eleni Michou 1, 2 , Samuel Gujer 12, 13 , Tommaso Gori 14 , Philip Wenzel 14 , Otmar Pfister 1, 2 , David Conen 1, 2, 15 , Ioannis Kapos 12, 16 , Richard Kobza 12 , Hans Rickli 4 , Tobias Breidthardt 1, 2, 5 , Thomas Münzel 14 , Paul Erne 12 , Christian Mueller 1, 2 , , Christian Mueller , Paul Erne , Beat Müller , Hans Rickli , Micha Maeder , Mucio Tavares de Oliveira , Thomas Münzel , Antoni Bayés-Genís , Alessandro Sionis , Assen Goudev , Bojidar Dimov , Sabine Hartwiger , Nisha Arenja , Bettina Glatz , Natascha Herr , Rahel Isenrich , Tamina Mosimann , Raphael Twerenbold , Jasper Boeddinghaus , Thomas Nestelberger , Christian Puelacher , Michael Freese , Janine Vögele , Kathrin Meissner , Jasmin Martin , Ivo Strebel , Desiree Wussler , Carmela Schumacher , Stefan Osswald , Fabian Vogt , Jonas Hilti , Sara Barata , Deborah Schneider , Jonas Schwarz , Brigitte Fitze , Sabine Hartwiger , Nisha Arenja , Bettina Glatz , Natascha Herr , Rahel Isenrich , Tamina Mosimann , Raphael Twerenbold , Jasper Boeddinghaus , Thomas Nestelberger , Christian Puelacher , Michael Freese , Janine Vögele , Kathrin Meissner , Jasmin Martin , Ivo Strebel , Desiree Wussler , Carmela Schumacher , Stefan Osswald , Fabian Vogt , Jonas Hilti , Sara Barata , Deborah Schneider , Jonas Schwarz , Brigitte Fitze , Nisha Arenja , Katharina Rentsch , Aline Bossa , Sergio Jallad , Alexandre Soeiro , Dimitar Georgiev , Thomas Jansen , Gabriele Gebel , Matthias Bossard , Michael Christ
JAMA ( IF 120.7 ) Pub Date : 2019-12-17 , DOI: 10.1001/jama.2019.18598 Nikola Kozhuharov 1, 2 , Assen Goudev 3 , Dayana Flores 1, 2 , Micha T Maeder 4 , Joan Walter 1, 2, 5 , Samyut Shrestha 1, 2, 5 , Danielle Menosi Gualandro 1, 2, 6 , Mucio Tavares de Oliveira Junior 6 , Zaid Sabti 1, 2 , Beat Müller 7 , Markus Noveanu 1, 2 , Thenral Socrates 1, 2, 8 , Ronny Ziller 1, 2 , Antoni Bayés-Genís 9 , Alessandro Sionis 10 , Patrick Simon 11 , Eleni Michou 1, 2 , Samuel Gujer 12, 13 , Tommaso Gori 14 , Philip Wenzel 14 , Otmar Pfister 1, 2 , David Conen 1, 2, 15 , Ioannis Kapos 12, 16 , Richard Kobza 12 , Hans Rickli 4 , Tobias Breidthardt 1, 2, 5 , Thomas Münzel 14 , Paul Erne 12 , Christian Mueller 1, 2 , , Christian Mueller , Paul Erne , Beat Müller , Hans Rickli , Micha Maeder , Mucio Tavares de Oliveira , Thomas Münzel , Antoni Bayés-Genís , Alessandro Sionis , Assen Goudev , Bojidar Dimov , Sabine Hartwiger , Nisha Arenja , Bettina Glatz , Natascha Herr , Rahel Isenrich , Tamina Mosimann , Raphael Twerenbold , Jasper Boeddinghaus , Thomas Nestelberger , Christian Puelacher , Michael Freese , Janine Vögele , Kathrin Meissner , Jasmin Martin , Ivo Strebel , Desiree Wussler , Carmela Schumacher , Stefan Osswald , Fabian Vogt , Jonas Hilti , Sara Barata , Deborah Schneider , Jonas Schwarz , Brigitte Fitze , Sabine Hartwiger , Nisha Arenja , Bettina Glatz , Natascha Herr , Rahel Isenrich , Tamina Mosimann , Raphael Twerenbold , Jasper Boeddinghaus , Thomas Nestelberger , Christian Puelacher , Michael Freese , Janine Vögele , Kathrin Meissner , Jasmin Martin , Ivo Strebel , Desiree Wussler , Carmela Schumacher , Stefan Osswald , Fabian Vogt , Jonas Hilti , Sara Barata , Deborah Schneider , Jonas Schwarz , Brigitte Fitze , Nisha Arenja , Katharina Rentsch , Aline Bossa , Sergio Jallad , Alexandre Soeiro , Dimitar Georgiev , Thomas Jansen , Gabriele Gebel , Matthias Bossard , Michael Christ
Affiliation
|
Importance
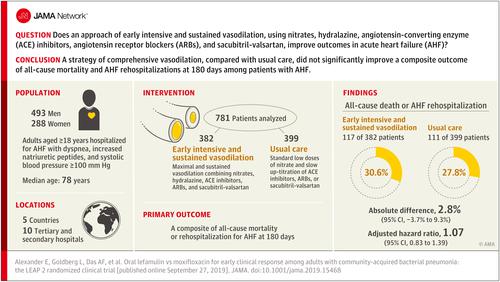
Short-term infusions of single vasodilators, usually given in a fixed dose, have not improved outcomes in patients with acute heart failure (AHF). Objective
To evaluate the effect of a strategy that emphasized early intensive and sustained vasodilation using individualized up-titrated doses of established vasodilators in patients with AHF. Design, Setting, and Participants
Randomized, open-label blinded-end-point trial enrolling 788 patients hospitalized for AHF with dyspnea, increased plasma concentrations of natriuretic peptides, systolic blood pressure of at least 100 mm Hg, and plan for treatment in a general ward in 10 tertiary and secondary hospitals in Switzerland, Bulgaria, Germany, Brazil, and Spain. Enrollment began in December 2007 and follow-up was completed in February 2019. Interventions
Patients were randomized 1:1 to a strategy of early intensive and sustained vasodilation throughout the hospitalization (n = 386) or usual care (n = 402). Early intensive and sustained vasodilation was a comprehensive pragmatic approach of maximal and sustained vasodilation combining individualized doses of sublingual and transdermal nitrates, low-dose oral hydralazine for 48 hours, and rapid up-titration of angiotensin-converting enzyme inhibitors, angiotensin receptor blockers, or sacubitril-valsartan. Main Outcomes and Measures
The primary end point was a composite of all-cause mortality or rehospitalization for AHF at 180 days. Results
Among 788 patients randomized, 781 (99.1%; median age, 78 years; 36.9% women) completed the trial and were eligible for primary end point analysis. Follow-up at 180 days was completed for 779 patients (99.7%). The primary end point, a composite of all-cause mortality or rehospitalization for AHF at 180 days, occurred in 117 patients (30.6%) in the intervention group (including 55 deaths [14.4%]) and in 111 patients (27.8%) in the usual care group (including 61 deaths [15.3%]) (absolute difference for the primary end point, 2.8% [95% CI, -3.7% to 9.3%]; adjusted hazard ratio, 1.07 [95% CI, 0.83-1.39]; P = .59). The most common clinically significant adverse events with early intensive and sustained vasodilation vs usual care were hypokalemia (23% vs 25%), worsening renal function (21% vs 20%), headache (26% vs 10%), dizziness (15% vs 10%), and hypotension (8% vs 2%). Conclusions and Relevance
Among patients with AHF, a strategy of early intensive and sustained vasodilation, compared with usual care, did not significantly improve a composite outcome of all-cause mortality and AHF rehospitalization at 180 days. Trial Registration
ClinicalTrials.gov Identifier: NCT00512759.
中文翻译:

综合血管舒张策略与常规护理对急性心力衰竭患者死亡率和心力衰竭再住院的影响
重要性 短期输注单一血管扩张剂,通常以固定剂量给药,并没有改善急性心力衰竭 (AHF) 患者的预后。目的 评估在 AHF 患者中使用个体化递增剂量的既定血管扩张剂强调早期强化和持续血管扩张的策略的效果。设计、设置和参与者 随机、开放标签盲终点试验,纳入 788 名因 AHF 住院且呼吸困难、利钠肽血浆浓度升高、收缩压至少为 100 mmHg 并计划进行一般治疗的患者在瑞士、保加利亚、德国、巴西和西班牙的 10 家三级和二级医院病房。2007 年 12 月开始入组,2019 年 2 月完成随访。 干预措施 患者被随机分配 1:1 到整个住院期间(n = 386)或常规护理(n = 402)的早期强化和持续血管舒张策略。早期强化和持续血管舒张是最大和持续血管舒张的综合实用方法,结合个体化剂量的舌下和透皮硝酸盐、低剂量口服肼苯哒嗪 48 小时,以及快速滴定血管紧张素转换酶抑制剂、血管紧张素受体阻滞剂或沙库巴曲缬沙坦。主要结果和措施 主要终点是 180 天时 AHF 的全因死亡率或再住院的复合终点。结果 在随机分配的 788 名患者中,781 名(99.1%;中位年龄为 78 岁;36.9% 为女性)完成了试验并符合主要终点分析条件。779 名患者(99.7%)完成了 180 天的随访。主要终点,干预组 117 名患者 (30.6%)(包括 55 名死亡 [14.4%])和常规护理组 111 名患者 (27.8%) 发生了 180 天 AHF 全因死亡或再住院的复合事件(包括 61 例死亡 [15.3%])(主要终点的绝对差异,2.8% [95% CI,-3.7% 至 9.3%];调整后的风险比,1.07 [95% CI,0.83-1.39];P = . 59)。与常规治疗相比,早期强化和持续血管扩张最常见的临床显着不良事件是低钾血症(23% 对 25%)、肾功能恶化(21% 对 20%)、头痛(26% 对 10%)、头晕(15%) vs 10%)和低血压(8% vs 2%)。结论和相关性 在 AHF 患者中,与常规护理相比,早期强化和持续血管扩张的策略,没有显着改善 180 天时全因死亡率和 AHF 再住院的复合结果。试验注册 ClinicalTrials.gov 标识符:NCT00512759。
更新日期:2019-12-17
中文翻译:

综合血管舒张策略与常规护理对急性心力衰竭患者死亡率和心力衰竭再住院的影响
重要性 短期输注单一血管扩张剂,通常以固定剂量给药,并没有改善急性心力衰竭 (AHF) 患者的预后。目的 评估在 AHF 患者中使用个体化递增剂量的既定血管扩张剂强调早期强化和持续血管扩张的策略的效果。设计、设置和参与者 随机、开放标签盲终点试验,纳入 788 名因 AHF 住院且呼吸困难、利钠肽血浆浓度升高、收缩压至少为 100 mmHg 并计划进行一般治疗的患者在瑞士、保加利亚、德国、巴西和西班牙的 10 家三级和二级医院病房。2007 年 12 月开始入组,2019 年 2 月完成随访。 干预措施 患者被随机分配 1:1 到整个住院期间(n = 386)或常规护理(n = 402)的早期强化和持续血管舒张策略。早期强化和持续血管舒张是最大和持续血管舒张的综合实用方法,结合个体化剂量的舌下和透皮硝酸盐、低剂量口服肼苯哒嗪 48 小时,以及快速滴定血管紧张素转换酶抑制剂、血管紧张素受体阻滞剂或沙库巴曲缬沙坦。主要结果和措施 主要终点是 180 天时 AHF 的全因死亡率或再住院的复合终点。结果 在随机分配的 788 名患者中,781 名(99.1%;中位年龄为 78 岁;36.9% 为女性)完成了试验并符合主要终点分析条件。779 名患者(99.7%)完成了 180 天的随访。主要终点,干预组 117 名患者 (30.6%)(包括 55 名死亡 [14.4%])和常规护理组 111 名患者 (27.8%) 发生了 180 天 AHF 全因死亡或再住院的复合事件(包括 61 例死亡 [15.3%])(主要终点的绝对差异,2.8% [95% CI,-3.7% 至 9.3%];调整后的风险比,1.07 [95% CI,0.83-1.39];P = . 59)。与常规治疗相比,早期强化和持续血管扩张最常见的临床显着不良事件是低钾血症(23% 对 25%)、肾功能恶化(21% 对 20%)、头痛(26% 对 10%)、头晕(15%) vs 10%)和低血压(8% vs 2%)。结论和相关性 在 AHF 患者中,与常规护理相比,早期强化和持续血管扩张的策略,没有显着改善 180 天时全因死亡率和 AHF 再住院的复合结果。试验注册 ClinicalTrials.gov 标识符:NCT00512759。

























 京公网安备 11010802027423号
京公网安备 11010802027423号