Acta Biomaterialia ( IF 9.7 ) Pub Date : 2020-05-16 , DOI: 10.1016/j.actbio.2020.04.042 Suja Shrestha 1 , Meghan J McFadden 2 , Anthony O Gramolini 3 , J Paul Santerre 4
|
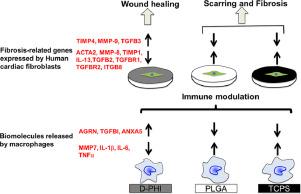
The use of exogenous biomolecules (BM) for the purpose of repairing and regenerating damaged cardiac tissue can yield serious side effects if used for prolonged periods. As well, such strategies can be cost prohibitive depending on the regiment and period of time applied. Alternatively, autologous monocytes/monocyte-derived macrophages (MDM) can provide a viable path towards generating an endogenous source of stimulatory BM. Biomaterials are often considered as delivery vehicles to generate unique profiles of such BM in tissues or to deliver autologous cells, that can influence the nature of BM produced by the cells. MDM cultured on a degradable polar hydrophobic ionic (D-PHI) polyurethane has previously demonstrated a propensity to increase select anti-inflammatory cytokines, and therefore there is good rationale to further investigate a broader spectrum of the cells’ BM in order to provide a more complete proteomic analysis of human MDM secretions induced by D-PHI. Further, it is of interest to assess the potential of such BM to influence cells involved in the reparative state of vital tissues such as those that affect cardiac cell function. Hence, this current study examines the proteomic profile of MDM secretions using mass spectrometry for the first time, along with ELISA, following their culture on D-PHI, and compares them to two important reference materials, poly(lactic-co-glycolic acid) (PLGA) and tissue culture polystyrene (TCPS). Secretions collected from D-PHI cultured MDM led to higher levels of regenerative BM, AGRN, TGFBI and ANXA5, but lower levels of pro-fibrotic BM, MMP7, IL-1β, IL-6 and TNFα, when compared to MDM secretions collected from PLGA and TCPS. In the application to cardiac cell function, the secretion collected from D-PHI cultured MDM led to more human cardiac fibroblast (HCFs) migration. A lower collagen gel contraction induced by MDM secretions collected from D-PHI was supported by gene array analysis for human fibrosis-related genes. The implication of these findings is that more tailored biomaterials such as D-PHI, may lead to a lower pro-inflammatory phenotype of macrophages when used in cardiac tissue constructs, thereby enabling the development of vehicles for the delivery of interventional therapies, or be applied as coatings for sensor implants in cardiac tissue that minimize fibrosis. The general approach of using synthetic biomaterials in order to induce MDM secretions in a manner that will guide favorable regeneration will be critical in making the choice of biomaterials for tissue regeneration work in the future.
Statement of significance
Immune modulation strategies currently applied in cardiac tissue repair are mainly based on the delivery of defined exogenous biomolecules. However, the use of such biomolecules may pose wide ranging systemic effects, thereby rendering them clinically less practical. The chemistry of biomaterials (used as a potential targeted delivery modality to circumvent the broad systemic effects of biomolecules) can not only affect acute and chronic toxicity but also alters the timeframe of the wound healing cascade. In this context, monocytes/monocyte-derive macrophages (MDM) can be harnessed as an immune modulating strategy to promote wound healing by an appropriate choice of the biomaterial. However, there are limited reports on the complete proteome analysis of MDM and their reaction of biomaterial related interventions on cardiac tissues and cells. No studies to date have demonstrated the complete proteome of MDM secretions when these cells were cultured on a non-traditional immune modulatory ionomeric polyurethane D-PHI film. This study demonstrated that MDM cultured on D-PHI expressed significantly higher levels of AGRN, TGFBI and ANXA5 but lower levels of MMP7, IL-1β, IL-6 and TNFα when compared to MDM cultured on a well-established degradable biomaterials in the medical field, e.g. PLGA and TCPS, which are often used as the relative standards for cell culture work in the biomaterials field. The implications of these findings have relevance to the repair of cardiac tissues. In another aspect of the work, human cardiac fibroblasts showed significantly lower contractility (low collagen gel contraction and low levels of ACTA2) when cultured in the presence of MDM secretions collected after culturing them on D-PHI compared to PLGA and TCPS. The findings place emphasis on the importance of making the choice of biomaterials for tissue engineering and regenerative medicine applied to their use in cardiac tissue repair.
中文翻译:

暴露于生物材料后人类单核细胞衍生的巨噬细胞分泌物的蛋白质组分析以及分泌物对心脏成纤维细胞纤维化特征的影响。
如果长时间使用外源性生物分子(BM)修复和再生受损的心脏组织,会产生严重的副作用。同样,根据所使用的方案和时间段,这些策略在成本上也可能过高。或者,自体单核细胞/单核细胞衍生的巨噬细胞(MDM)可以提供一条可行的途径,以产生刺激性BM的内源性来源。生物材料通常被认为是在组织中产生此类BM的独特特征或传递自体细胞的传递媒介,这会影响细胞产生的BM的性质。在可降解的极性疏水离子(D-PHI)聚氨酯上培养的MDM先前已证明有增加选择抗炎细胞因子的倾向,因此,有充分的理由进一步研究更广泛的细胞BM,以便对D-PHI诱导的人MDM分泌物提供更完整的蛋白质组学分析。此外,令人感兴趣的是评估这种BM影响重要组织(如影响心脏细胞功能的组织)修复状态中涉及的细胞的潜力。因此,本研究在D-PHI上培养后,首次使用质谱法和ELISA首次检测了MDM分泌的蛋白质组学特征,并将其与两种重要的参考物质(聚乳酸-乙醇酸)进行比较(PLGA)和组织培养聚苯乙烯(TCPS)。从D-PHI培养的MDM中收集的分泌物导致较高水平的再生BM,AGRN,TGFBI和ANXA5,但较低水平的促纤维化BM,MMP7,IL-1β,IL-6和TNFα,与从PLGA和TCPS收集的MDM分泌物相比。在应用于心脏细胞功能中,从D-PHI培养的MDM中收集的分泌物导致更多的人类心脏成纤维细胞(HCF)迁移。通过对人纤维化相关基因进行基因阵列分析,支持了由D-PHI收集的MDM分泌引起的胶原蛋白凝胶收缩降低。这些发现的含义是,当在心脏组织构建物中使用时,更多定制的生物材料(例如D-PHI)可能会导致较低的巨噬细胞促炎表型,从而使得能够开发用于介入治疗的载体,或者被应用作为用于心脏组织中的传感器植入物的涂层,可最大程度地减少纤维化。
重要声明
当前应用于心脏组织修复的免疫调节策略主要基于确定的外源生物分子的递送。但是,使用此类生物分子可能会产生广泛的全身效应,从而使它们在临床上不太实用。生物材料的化学作用(用作潜在的靶向传递方式,以规避生物分子的广泛系统作用)不仅会影响急性和慢性毒性,而且还会改变伤口愈合级联的时间框架。在这种情况下,单核细胞/单核细胞 - 巨噬细胞派生(MDM)可以被利用作为一种免疫调节策略由生物材料的适当选择,以促进伤口愈合。然而,关于MDM的完整蛋白质组分析及其对心脏组织和细胞的生物材料相关干预的反应,报道很少。迄今为止,尚无研究证明当将这些细胞培养在非传统免疫调节离聚物聚氨酯D-PHI膜上时,MDM分泌的完整蛋白质组。这项研究表明,与在医学上成熟的可降解生物材料上培养的MDM相比,在D-PHI上培养的MDM表达的AGRN,TGFBI和ANXA5的水平明显更高,但MMP7,IL-1β,IL-6和TNFα的水平更低。领域,例如PLGA和TCPS,它们通常用作生物材料领域中细胞培养工作的相对标准。这些发现的含义与心脏组织的修复有关。在工作的另一方面,与PLGA和TCPS相比,在D-PHI培养后收集到的MDM分泌物存在下培养时,人心脏成纤维细胞显示出显着较低的收缩力(胶原凝胶收缩低和ACTA2水平低)。研究结果强调了选择用于组织工程和再生医学的生物材料用于心脏组织修复的重要性。

























 京公网安备 11010802027423号
京公网安备 11010802027423号