Abstract
Background
Even if Meares-Stamey 4-glass (M&S) test is regarded a decisive tool for diagnosing prostatitis its use is only rarely performed in everyday clinical practice. Here, we analyze if the diagnostic yield of the M&S test could be improved by a pre-test categorization of patients due to undergo a M&S test.
Methods
All clinical and microbiological data of patients who underwent M&S test in two urological centers from January 2004 to December 2021 were analyzed in this retrospective cohort study. One center has a dedicated staff member for the study of prostatitis (Cohort I), while the other center is a general urological unit (Cohort II). All patients were divided into 3 groups on the basis of the assembled data: patients with symptoms related to prostatitis only (Group I), patients with symptoms related to both prostatitis and BPH (Group II), patients with symptoms related to BPH only (Group III). The rates of positive microbiological results in each group were compared.
Results
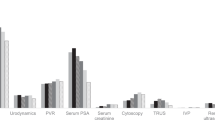
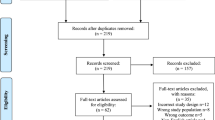
In the whole period, 9347 patients were analyzed and categorized as follows: Group I, 1884; Group II, 5151; Group III, 2312. Three-thousand and eight-hundred twenty-three patients showed positive culture results (40.9%). The most common isolated species was Escherichia coli (49.7%), followed by Enteroccus spp. (31.8%). The rates of positive M&S tests in the different symptom groups were: Group I, 1532 (81.4%); Group II, 1494 (29.0%); Group III, 797 (34.4%). The overall rate of positive M&S tests in each urology center showed that the center with a staff member who is dedicated to prostatitis studies (Cohort I) had a significantly higher rate of positive M&S tests than the general urological department (Cohort II) (64.3% vs 31.4%; p < 0.001).
Conclusions
Symptom-based patient selection and dedicated staff members will increase the diagnostic yield of the M&S test and reduce the number of unnecessary tests.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
Data availability
Data is unavailable due to privacy or ethical restrictions in accordance with Italian bylaws.
References
Cai T, Alidjanov J, Palagin I, Medina-Polo J, Nickel JC, Wagenlehner FME Chronic prostatitis/chronic pelvic pain syndrome (CP/CPPS): look to the future. Prostate Cancer Prostatic Dis. 2023. https://doi.org/10.1038/s41391-023-00645-7.
Magistro G, Wagenlehner FM, Grabe M, Weidner W, Stief CG, Nickel JC. Contemporary management of chronic prostatitis/chronic pelvic pain syndrome. Eur Urol. 2016;69:286–97.
Polackwich AS, Shoskes DA. Chronic prostatitis/chronic pelvic pain syndrome: a review of evaluation and therapy. Prostate Cancer Prostatic Dis. 2016;19:132–8.
EAU. European Association of Urology guidelines on urological infections, update 2023. http://uroweb.org/guideline/urological-infections/. Access on June 27th, 2023.
Mazzoli S, Cai T, Addonisio P, Bechi A, Mondaini N, Bartoletti R. Chlamydia trachomatis infection is related to poor semen quality in young prostatitis patients. Eur Urol. 2010;57:708–14.
Lam JC, Lang R, Stokes W. How I manage bacterial prostatitis. Clin Microbiol Infect. 2023;29:32–37.
Magri V, Boltri M, Cai T, Colombo R, Cuzzocrea S, De Visschere P, et al. Multidisciplinary approach to prostatitis. Arch Ital Urol Androl. 2019;90:227–48.
Nickel JC, Shoskes D, Wang Y, Alexander RB, Fowler JE Jr, et al. How does the pre-massage and post-massage 2-glass test compare to the Meares-Stamey 4-glass test in men with chronic prostatitis/chronic pelvic pain syndrome? J Urol. 2006;176:119–24.
Cai T, Pisano F, Nesi G, Magri V, Verze P, Perletti G, et al. Chlamydia trachomatis versus common uropathogens as a cause of chronic bacterial prostatitis: is there any difference? Results of a prospective parallel-cohort study. Investig Clin Urol. 2017;58:460–7.
Cai T, Gallelli L, Cione E, Perletti G, Ciarleglio F, Malossini G, et al. The use of Lactobacillus casei DG® prevents symptomatic episodes and reduces the antibiotic use in patients affected by chronic bacterial prostatitis: results from a phase IV study. World J Urol 2021. 2021;39:3433–40.
Cai T, Tamanini I, Mattevi D, Verze P, Palmieri A, Malossini G, et al. Fosfomycin trometamol and N-acetyl-L-cysteine as combined oral therapy of difficult-to-treat chronic bacterial prostatitis: results of a pilot study. Int J Antimicrob Agents. 2020;56:105935.
Mazzoli S, Cai T, Rupealta V, Gavazzi A, Castricchi Pagliai R, Mondaini N, et al. Interleukin 8 and anti-chlamydia trachomatis mucosal IgA as urogenital immunologic markers in patients with C. trachomatis prostatic infection. Eur Urol. 2007;51:1385–93.
Meares EM Jr, Stamey TA. The diagnosis and management of bacterial prostatitis. Br J Urol. 1972;44:175–9.
Giubilei G, Mondaini N, Crisci A, Raugei A, Lombardi G, Travaglini F, et al. The Italian version of the National Institutes of Health Chronic Prostatitis Symptom Index. Eur Urol. 2005;47:805–11.
Badia X, Garcia-Losa M, Dal-Re R. Ten-language translation and harmonization of the International Prostate Symptom Score: developing a methodology for multinational clinical trials. Eur Urol. 1997;31:129–40.
McNaughton Collins M, Fowler FJ Jr, Elliott DB, Albertsen PC, Barry MJ. Diagnosing and treating chronic prostatitis: do urologists use the four-glass test? Urology. 2000;55:403–7.
Nickel JC, Nigro M, Valiquette L, Anderson P, Patrick A, Mahoney J, et al. Diagnosis and treatment of prostatitis in Canada. Urology. 1998;52:797–802.
Zegarra Montes LZ, Sanchez Mejia AA, Loza Munarriz CA, Gutierrez EC. Semen and urine culture in the diagnosis of chronic bacterial prostatitis. Int Braz J Urol. 2008;34:30–40.
de la Rosette JJ, Hubregtse MR, Karthaus HF, Debruyne FM. Results of a questionnaire among Dutch urologists and general practitioners concerning diagnostics and treatment of patients with prostatitis syndromes. Eur Urol. 1992;22:14–19.
Nickel JC. Prostatitis: myths and realities. Urology. 1998;51:362–6.
Kong X, Hu W, Dong Z, Tian J, Wang Y, Jin C, et al. The efficacy and safety of low-intensity extracorporeal shock wave treatment combined with or without medications in Chronic prostatitis/chronic pelvic pain syndrome: a systematic review and meta-analysis. Prostate Cancer Prostatic Dis. 2023;26:483–94.
Mjaess G, Karam A, Roumeguère T, Diamand R, Aoun F, McVary K, et al. Urinary microbiota and prostatic diseases: the key for the lock? A systematic review. Prostate Cancer Prostatic Dis. 2023;26:451–60.
Lipsky B. Prostatitis and urinary tract infection in men: what’s new? What’s true? Am J Med. 1999;106:327–34.
McCaig L, Hughes J. Trends in antimicrobial drug prescribing among office-based physicians in the United States. JAMA. 1995;273:214–9.
Author information
Authors and Affiliations
Contributions
Conceptualization, TC and SM; methodology, TC and OM; formal analysis, TC and LG; data collection, PL, IT, KO, ML; writing, original draft preparation, TC and TEBJ; writing, review and editing, FMEW and AP; supervision CDN. All authors have read and agreed to the published version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
There are no competing interests to declare.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Cai, T., Tamanini, I., Odorizzi, K. et al. The diagnostic yield of the Meares & Stamey test can be significantly improved by symptom-based patient selection and the experience of the test performer. Prostate Cancer Prostatic Dis (2024). https://doi.org/10.1038/s41391-024-00824-0
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41391-024-00824-0