Abstract
Objective
Bronchopulmonary dysplasia (BPD) is a common complication of preterm birth and is associated with abnormal vasculature that contributes to pulmonary hypertension (PH). We evaluated how a tracheostomy may alter PH in these patients.
Methods
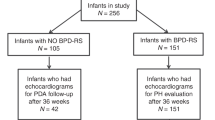
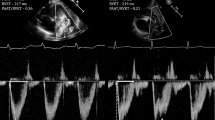
A retrospective chart review over 15-years identified 17 patients with BPD and PH who underwent tracheostomy. Each patient had four echocardiograms re-reviewed and scored for tricuspid valve regurgitation velocity (TR), tricuspid annular plane systolic excursion (TAPSE), right atrial cross-sectional area (RACA), and left ventricle eccentricity indices (EI).
Result
There was improvement in TR, TAPSE, RACA, and left ventricle EI indicating reduction in PH after tracheostomy.
Conclusion
PH improves over time though role of tracheostomy in PH needs to be further defined. The EI may be a sensitive marker to follow over time in these patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Northway WH Jr, Rosan RC, Porter DY. Pulmonary disease following respirator therapy of hyaline-membrane disease. Bronchopulmonary dysplasia. N Engl J Med. 1967;276:357–68.
Stoll BJ, Hansen NI, Bell EF, Shankaran S, Laptook AR, Walsh MC, et al. Neonatal outcomes of extremely preterm infants from the NICHD Neonatal Research Network. Pediatrics. 2010;126:443–56.
Kinsella JP, Greenough A, Abman SH. Bronchopulmonary dysplasia. Lancet. 2006;367:1421–31.
Latham GJ, Yung D. Current understanding and perioperative management of pediatric pulmonary hypertension. Paediatr Anaesth. 2019;29:441–56.
Jensen EA, Dysart K, Gantz MG, McDonald S, Bamat NA, Keszler M, et al. The diagnosis of bronchopulmonary dysplasia in very preterm infants. an evidence-based approach. Am J Respir Crit Care Med. 2019;200:751–9.
Khemani E, McElhinney DB, Rhein L, Andrade O, Lacro RV, Thomas KC, et al. Pulmonary artery hypertension in formerly premature infants with bronchopulmonary dysplasia: clinical features and outcomes in the surfactant era. Pediatrics. 2007;120:1260–9.
Al-Ghanem G, Shah P, Thomas S, Banfield L, El Helou S, Fusch C, et al. Bronchopulmonary dysplasia and pulmonary hypertension: a meta-analysis. J Perinatol. 2017;37:414–9.
Goodman G, Perkin RM, Anas NG, Sperling DR, Hicks DA, Rowen M. Pulmonary hypertension in infants with bronchopulmonary dysplasia. J Pediatr. 1988;112:67–72.
Wu KY, Jensen EA, White AM, Wang Y, Biko DM, Nilan K, et al. Characterization of disease phenotype in very preterm infants with severe bronchopulmonary dysplasia. Am J Respir Crit Care Med. 2020;201:1398–406.
Upadhyay K, Vallarino DA, Talati AJ. Outcomes of neonates with tracheostomy secondary to bronchopulmonary dysplasia. BMC Pediatr. 2020;20:414.
Ivy D. Pulmonary hypertension in children. Cardiol Clin. 2016;34:451–72.
Choi EK, Shin SH, Kim EK, Kim HS. Developmental outcomes of preterm infants with bronchopulmonary dysplasia-associated pulmonary hypertension at 18-24 months of corrected age. BMC Pediatr. 2019;19:26.
Altit G, Bhombal S, Hopper RK, Tacy TA, Feinstein J. Death or resolution: the “natural history” of pulmonary hypertension in bronchopulmonary dysplasia. J Perinatol. 2019;39:415–25.
Bhat R, Salas AA, Foster C, Carlo WA, Ambalavanan N. Prospective analysis of pulmonary hypertension in extremely low birth weight infants. Pediatrics. 2012;129:e682–9.
An HS, Bae EJ, Kim GB, Kwon BS, Beak JS, Kim EK, et al. Pulmonary hypertension in preterm infants with bronchopulmonary dysplasia. Korean Circ J. 2010;40:131–6.
Mourani PM, Abman SH. Pulmonary vascular disease in bronchopulmonary dysplasia: pulmonary hypertension and beyond. Curr Opin Pediatr. 2013;25:329–37.
Luo J, Shepard S, Nilan K, Wood A, Monk HM, Jensen EA, et al. Improved growth and developmental activity post tracheostomy in preterm infants with severe BPD. Pediatr Pulmonol. 2018;53:1237–44.
Mandy G, Malkar M, Welty SE, Brown R, Shepherd E, Gardner W, et al. Tracheostomy placement in infants with bronchopulmonary dysplasia: safety and outcomes. Pediatr Pulmonol. 2013;48:245–9.
Manimtim WM, Agarwal A, Alexiou S, Levin JC, Aoyama B, Austin ED, et al. Respiratory outcomes for ventilator-dependent children with bronchopulmonary dysplasia. Pediatrics. 2023;151:e2022060651.
Vyas-Read S, Logan JW, Cuna AC, Machry J, Leeman KT, Rose RS, et al. A comparison of newer classifications of bronchopulmonary dysplasia: findings from the Children’s Hospitals Neonatal Consortium Severe BPD Group. J Perinatol. 2022;42:58–64.
Vayalthrikkovil S, Vorhies E, Stritzke A, Bashir RA, Mohammad K, Kamaluddeen M, et al. Prospective study of pulmonary hypertension in preterm infants with bronchopulmonary dysplasia. Pediatr Pulmonol. 2019;54:171–8.
Bice T, Nelson JE, Carson SS. To trach or not to trach: uncertainty in the care of the chronically critically Ill. Semin Respir Crit Care Med. 2015;36:851–8.
Cox CE, Carson SS, Holmes GM, Howard A, Carey TS. Increase in tracheostomy for prolonged mechanical ventilation in North Carolina, 1993-2002. Crit Care Med. 2004;32:2219–26.
Unal S, Bilgin LK, Gonulal D, Akcan FA. Optimal time of tracheotomy in infants: still a dilemma. Glob Pediatr Health. 2015;2:2333794x15569300.
Knirsch W, Eiselt M, Nürnberg J, Haas NA, Berger F, Dähnert I, et al. [Pulmonary plasma catecholamine levels and pulmonary hypertension in congenital heart disease]. Z Kardiol. 2002;91:1035–43.
Matsuura H. Cardiac catheterization in children with pulmonary arterial hypertension. Pediatr Int. 2017;59:3–9.
Ciarka A, Doan V, Velez-Roa S, Naeije R, van de Borne P. Prognostic significance of sympathetic nervous system activation in pulmonary arterial hypertension. Am J Respir Crit Care Med. 2010;181:1269–75.
Nseir S, Di Pompeo C, Jozefowicz E, Cavestri B, Brisson H, Nyunga M. Relationship between tracheotomy and ventilator-associated pneumonia: a case control study. Eur Respir J. 2006;30:314–20.
Abman SH, Hansmann G, Archer SL, Ivy DD, Adatia I, Chung WK, et al. Pediatric pulmonary hypertension: guidelines From the American Heart Association and American Thoracic Society. Circulation. 2015;132:2037–99.
Burkett DA, Patel SS, Mertens L, Friedberg MK, Ivy DD. Relationship between left ventricular geometry and invasive hemodynamics in pediatric pulmonary hypertension. Circ Cardiovasc Imaging. 2020;13:e009825.
Thierry S, Steven DC. Structural measurements and adjustment for growth. In: W. W. Lai, L. L. Mertens, editors. Echocardiography in Pediatric and Congenital Heart Disease. West Sussex, UK: Wiley-Blackwell; 2009.
Colan SD. Normal echocardiographic values for cardiovascular structures. In: W. W. Lai, L. L. Mertens, editors. Echocardiography in Pediatric and Congenital Heart Disease. West Sussex, UK: Wiley-Blackwell; 2009. p. 765–85.
Team R. RStudio: Integrated Development for R. Rstudio. Boston, MA: PBC; 2020.
Sallmon H, Koestenberger M, Avian A, Reiterer F, Schwaberger B, Meinel K, et al. Extremely premature infants born at 23–25 weeks gestation are at substantial risk for pulmonary hypertension. J Perinatol. 2022;42:781–7.
Varghese N, Rios D. Pulmonary hypertension associated with bronchopulmonary dysplasia: a review. Pediatr Allergy Immunol Pulmonol. 2019;32:140–8.
Farmakis IT, Demerouti E, Karyofyllis P, Karatasakis G, Stratinaki M, Tsiapras D, et al. Echocardiography in pulmonary arterial hypertension: is it time to reconsider its prognostic utility? J Clin Med. 2021;10:2826.
Jone PN, Ivy DD. Echocardiography in pediatric pulmonary hypertension. Front Pediatr. 2014;2:124.
Liu K, Zhang C, Chen B, Li M, Zhang P. Association between right atrial area measured by echocardiography and prognosis among pulmonary arterial hypertension: a systematic review and meta-analysis. BMJ Open. 2020;10:e031316.
Mourani PM, Sontag MK, Younoszai A, Ivy DD, Abman SH. Clinical utility of echocardiography for the diagnosis and management of pulmonary vascular disease in young children with chronic lung disease. Pediatrics. 2008;121:317–25.
Mourani PM, Sontag MK, Younoszai A, Miller JI, Kinsella JP, Baker CD, et al. Early pulmonary vascular disease in preterm infants at risk for bronchopulmonary dysplasia. Am J Respir Crit Care Med. 2015;191:87–95.
Mourani PM, Abman SH. Pulmonary hypertension and vascular abnormalities in bronchopulmonary dysplasia. Clin Perinatol. 2015;42:839–55.
El-Saie A, Varghese NP, Webb MK, Villafranco N, Gandhi B, Guaman MC, et al. Bronchopulmonary dysplasia—associated pulmonary hypertension: an updated review. Semin Perinatol. 2023. https://doi.org/10.1016/j.semperi.2023.151817.
Check J, Gotteiner N, Liu X, Su E, Porta N, Steinhorn R, et al. Fetal growth restriction and pulmonary hypertension in premature infants with bronchopulmonary dysplasia. J Perinatol. 2013;33:553–7.
Valenzuela D, Moya F, Luco M, Tapia JL. The role of pulmonary hypertension on bronchopulmonary dysplasia. Rev Chil Pediatr. 2017;88:699–706.
Meau-Petit V, Thouvenin G, Guillemot-Lambert N, Champion V, Tillous-Borde I, Flamein F, et al. [Bronchopulmonary dysplasia-associated pulmonary arterial hypertension of very preterm infants]. Arch Pediatr 2013;20:44–53.
Dasgupta S, Richardson JC, Aly AM, Jain SK. Role of functional echocardiographic parameters in the diagnosis of bronchopulmonary dysplasia-associated pulmonary hypertension. J Perinatol. 2022;42:19–30.
Wang C, Ma X, Xu Y, Chen Z, Shi L, Du L. A prediction model of pulmonary hypertension in preterm infants with bronchopulmonary dysplasia. Front Pediatr. 2022;10:925312.
Author information
Authors and Affiliations
Contributions
Timothy D. Hicks: Conceptualization, methodology, formal analysis, investigation, writing – original draft preparation, writing—review and editing. Julian Cameron: Methodology, investigation. Shuo Wang: Conceptualization, writing—review and editing, Amir Ashrafi: Conceptualization, methodology, writing—review and editing, Jacqueline Szmuszkovicz: Conceptualization, methodology, writing—review and editing, Narayan Iyer: Conceptualization, methodology, formal analysis, writing—review and editing. Manvi Bansal: Supervision, Conceptualization, methodology, formal analysis, investigation, writing – review and editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Institutional Review Board
The study was approved by the CHLA IRB: Study ID Number: CHLA-21-00031.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Hicks, T.D., Cameron, J., Wang, S. et al. Assessing the role of tracheostomy placement in bronchopulmonary dysplasia with pulmonary hypertension. J Perinatol (2024). https://doi.org/10.1038/s41372-024-01881-y
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41372-024-01881-y