Abstract
Purpose
Aim of the study was to evaluate the prevalence of LUTS in taxi drivers.
Methods
Between February 24th 2021 and March 26th 2021 a web based survey was administered to Taxi drivers in the city of Florence. Taxi drivers were evaluated with baseline characteristics such as: age, BMI, smoking, career length, comorbidities, and treatment. LUTS were evaluated using the international prostate symptom score (IPSS) and the overactive bladder (OAB) score. As well sexual function was evaluated using the international index erectile function (IIEF) and female sexual function index (FSFI) questionnaires. Risk factors for LUTS were evaluated using regression analysis.
Results
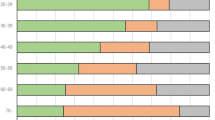
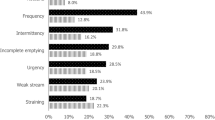
The overall response rate was 64.6% (537/830 taxi drivers filled the questionnaires). Among them, 449 (83.6%) were men and 88 (16.4%) females. Overall, median IPSS was 5 (2/9) and median OAB score was 10 (7/14). On multivariate binary regression analysis age > 50 (OR:1.60; p < 0,05), Smoking (OR:1.57; p < 0,05), chronic treatment (OR:1.57; p < 0,05), recurrent cystitis (OR: 2.66; p < 0,05) and chronic pelvic pain (OR:4.94; p < 0,05) were independent risk factors for moderate/severe LUTS. On multivariate binary logistic regression analysis, risk factors for erectile dysfunction were age older than 50 years (OR = 3.64; p < 0.05) and urinary incontinence (OR = 5.53; p = 0.005).
Conclusions
According to our web-based survey, Taxi drivers in the metropolitan city of Florence had non-negligible symptomatic LUTS and even sexual dysfunction. Our data suggest as LUTS are particular influenced by several life-style and behavioural factors as type and duration of work.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
Data and materials are available upon request.
References
Egan KB. The epidemiology of benign prostatic hyperplasia associated with lower urinary tract symptoms: prevalence and incident rates. Urol Clin North Am. 2016;43:289–97
Huang J, Chan CK, Yee S, Deng Y, Bai Y, Chan SC, et al. Global burden and temporal trends of lower urinary tract symptoms: a systematic review and meta-analysis. Prostate Cancer Prostatic Dis. 2022;26:421–28
De Nunzio C, Franco A, Lombardo R. LUTS/BPH and SARS-COV2: when a misunderstanding in the correct physiopathology results in incorrect associations. Prostate Cancer Prostatic Dis. 2021;25:5–6
Ornaghi PI, Porreca A, Sandri M, Sciarra A, Falsaperla M, Ludovico GM, et al. Features of patients referring to the outpatient office due to benign prostatic hyperplasia: analysis of a national prospective cohort of 5815 cases. Prostate Cancer Prostatic Dis. 2022;26:730–35
Sahakyan Y, Erman A, Bhojani N, Chughtai B, Zorn KC, Sander B, et al. Pharmacotherapy vs. minimally invasive therapies as initial therapy for moderate-to-severe benign prostatic hyperplasia: a cost-effectiveness study. Prostate Cancer Prostatic Dis Nat. 2022;26:113–8.
Tallman JE, Wallis CJD, Zhao Z, Huang LC, Penson DF, Koyama T, et al. Prostate volume, baseline urinary function, and their association with treatment choice and post-treatment urinary function in men treated for localized prostate cancer. Prostate Cancer Prostatic Dis. 2022;26:787–94
Del Giudice F, Huang J, Li S, Sorensen S, Enemchukwu E, Maggi M, et al. Contemporary trends in the surgical management of urinary incontinence after radical prostatectomy in the United States. Prostate Cancer Prostatic Dis Nat. 2022;26:367–73.
Welliver C, Feinstein L, Ward JB, Kirkali Z, Martinez-Miller EE, Matlaga BR, et al. Poor clinical guideline adherence and inappropriate testing for incident lower urinary tract symptoms associated with benign prostatic hyperplasia. Prostate Cancer Prostatic Dis. 2021;25:269–73.
Gratzke C, Cornu J-N, Gacci M. Guidelines on the Management of Non-Neurogenic Male Lower Urinary Tract Symptoms (LUTS), incl. Benign Prostatic Obstruction (BPO). Eur Assoc Urol. 2020;50-100
De Nunzio C, Truscelli G, Presicce F, Bellangino M, Gacci M, Gaudio C, et al. Moderate-to-high cardiovascular risk is associated with increased lower urinary tract storage symptoms in patients with benign prostatic enlargement. Minerva Urol Nefrol. 2018;70:340–6.
De Nunzio C, Presicce F, Lombardo R, Trucchi A, Bellangino M, Tubaro A, et al. Patient centred care for the medical treatment of lower urinary tract symptoms in patients with benign prostatic obstruction: A key point to improve patients’ care - A systematic review. BMC Urol. 2018;18:62
Pecoraro A, Morselli S, Raspollini MR, Sebastianelli A, Nicoletti R, Manera A, et al. The role of COVID-19 in prostate tissue inflammation: first pathological evidence. Prostate Cancer Prostatic Dis Nat. 2022;25:370–2.
De Nunzio C, Nacchia A, Cicione A, Sica A, Baldassarri V, Voglino O, et al. Night shift workers refer higher urinary symptoms with an impairment quality of life: a single cohort study. Minerva Urol Nefrol. 2020.
Higa R, Lopes MH. The impact of urinary incontinence on female nursing personnel. Rev Bras Enferm Rev Bras Enferm. 2007;60:213–6.
Brassetti A, De Nunzio C, Nacchia A, Lombardo R, Sica A, Baldassarri V, et al. Effect of vacation on urinary symptoms in health care workers: an Italian multicenter study. Eur Urol Open Sci. 2020;20:S85–6.
Mass AY, Goldfarb DS, Shah O. Taxi Cab Syndrome: A Review of the Extensive Genitourinary Pathology Experienced by Taxi Cab Drivers and What We Can Do to Help. Rev Urol MedReviews. LLC. 2014;16:99.
Eysenbach G. Improving the quality of Web surveys: the Checklist for Reporting Results of Internet E-Surveys (CHERRIES). J Med Internet Res. 2004;6:e34
Badía X, García-Losa M, Dal-Ré R. Ten-language translation and harmonization of the International Prostate Symptom Score: developing a methodology for multinational clinical trials. Eur Urol. 1997;31:129–40.
Acquadro C, Kopp Z, Coyne KS, Corcos J, Tubaro A, Choo MS. Translating overactive bladder questionnaires in 14 languages. Urology. 2006;67:536–40.
Rosen RC, Riley A, Wagner G, Osterloh IH, Kirkpatrick J, Mishra A. The international index of erectile function (IIEF): A multidimensional scale for assessment of erectile dysfunction. Urology.1997;49:822–30.
Filocamo MT, Serati M, Li Marzi V, Costantini E, Milanesi M, Pietropaolo A, et al. The Female Sexual Function Index (FSFI): linguistic validation of the Italian version. J Sex Med;. 2014;11:447–53.
Madersbacher S, Sampson N, Culig Z. Pathophysiology of Benign Prostatic Hyperplasia and Benign Prostatic Enlargement: A Mini-Review. Gerontology. 2019;65:458–64.
Malde S, Solomon E, Spilotros M, Mukhtar B, Pakzad M, Hamid R, et al. Female bladder outlet obstruction. Common Symptoms Mask uncommon causes Low Urin Trac Symptoms. 2019;11:72–7.
Irwin DE, Milsom I, Hunskaar S, Reilly K, Kopp Z, Herschorn S, et al. Population-Based Survey of Urinary Incontinence, Overactive Bladder, and Other Lower Urinary Tract Symptoms in Five Countries: Results of the EPIC Study. Eur Urol. 2006;50:1306–15.
De Nunzio C, Tema G, Lombardo R, Cicione A, Nacchia A, D’Annunzio S, et al. Metabolic syndrome and smoking are associated with persistence of nocturia after transurethral resection of the prostate. Neurourol Urodyn John Wiley Sons Inc. 2019;38:1692–9.
Hagovska M, Švihra J, Buková A, Horbacz A, Dračková D, Švihrová V. Comparison of body composition and overactive bladder symptoms in overweight female university students. Eur J Obstet Gynecol Reprod Biol. 2019;237:18–22.
Peyronnet B, Mironska E, Chapple C, Cardozo L, Oelke M, Dmochowski R, et al. A Comprehensive Review of Overactive Bladder Pathophysiology: On the Way to Tailored Treatment(Figure presented.) Eur. Urol. 2019;988–1000.
Nguyen HMT, Gabrielson AT, Hellstrom WJG. Erectile Dysfunction in Young Men-A Review of the Prevalence and Risk Factors. Sex Med Rev. 2017;5:508–20.
Geerkens MJM, Al-Itejawi HHM, Nieuwenhuijzen JA, Meuleman EJM, Lissenberg-Witte BI, van Moorselaar RJA, et al. Sexual Dysfunction and Bother Due to Erectile Dysfunction in the Healthy Elderly Male Population: Prevalence from a Systematic Review. Eur Urol Focus. 2020;6:776–90.
Imprialos KP, Koutsampasopoulos K, Katsimardou A, Bouloukou S, Theodoulidis I, Themistoklis M, et al. Female Sexual Dysfunction: A Problem Hidden in the Shadows. Curr Pharm Des. 2021;27:3762–74.
Thomas HN, Neal-Perry GS, Hess R. Female Sexual Function at Midlife and Beyond. Obstet Gynecol Clin North Am. 2018;45:709–22.
Author information
Authors and Affiliations
Consortia
Contributions
CDN: Protocol/project development, Data collection or management, Data analysis, Manuscript writing/editing. ACicione: Data collection or management, Manuscript writing/editing. SMusco: Data collection or management, Data analysis, Manuscript writing/editing. VLM: Data collection or management, Manuscript writing/editing. RL: Data collection or management, Manuscript writing/editing, Data analysis. LG: Data collection or management, Manuscript writing/editing, Data analysis. SMorselli: Data collection or management, Manuscript writing/editing, Data analysis. MLG: Data collection or management, Manuscript writing/editing. SS: Data collection or management, Manuscript writing/editing. CR: Data collection or management, Manuscript writing/editing.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
The study was approved by a local ethical committee and was conducted in accordance with the principles of the Declaration of Helsinki.
Consent to participate
A specific informed consent was signed by all the patients to participate.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Li Marzi, V., Musco, S., Lombardo, R. et al. Prevalence of lower urinary tract symptoms in taxi drivers: a cross-sectional web-based survey. Prostate Cancer Prostatic Dis (2023). https://doi.org/10.1038/s41391-023-00777-w
Received:
Revised:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41391-023-00777-w