PLOS Neglected Tropical Diseases ( IF 3.8 ) Pub Date : 2018-02-28 , DOI: 10.1371/journal.pntd.0006257 Corey M Peak 1 , Amanda L Reilly 2 , Andrew S Azman 3 , Caroline O Buckee 1
|
Background
Oral cholera vaccination is an approach to preventing outbreaks in at-risk settings and controlling cholera in endemic settings. However, vaccine-derived herd immunity may be short-lived due to interactions between human mobility and imperfect or waning vaccine efficacy. As the supply and utilization of oral cholera vaccines grows, critical questions related to herd immunity are emerging, including: who should be targeted; when should revaccination be performed; and why have cholera outbreaks occurred in recently vaccinated populations?
Methods and findings
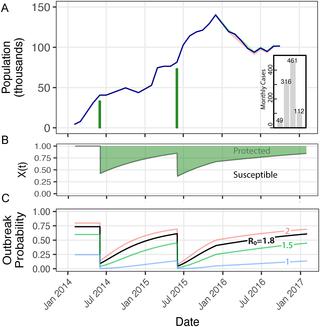
We use mathematical models to simulate routine and mass oral cholera vaccination in populations with varying degrees of migration, transmission intensity, and vaccine coverage. We show that migration and waning vaccine efficacy strongly influence the duration of herd immunity while birth and death rates have relatively minimal impacts. As compared to either periodic mass vaccination or routine vaccination alone, a community could be protected longer by a blended “Mass and Maintain” strategy. We show that vaccination may be best targeted at populations with intermediate degrees of mobility as compared to communities with very high or very low population turnover. Using a case study of an internally displaced person camp in South Sudan which underwent high-coverage mass vaccination in 2014 and 2015, we show that waning vaccine direct effects and high population turnover rendered the camp over 80% susceptible at the time of the cholera outbreak beginning in October 2016.
Conclusions
Oral cholera vaccines can be powerful tools for quickly protecting a population for a period of time that depends critically on vaccine coverage, vaccine efficacy over time, and the rate of population turnover through human mobility. Due to waning herd immunity, epidemics in vaccinated communities are possible but become less likely through complementary interventions or data-driven revaccination strategies.
中文翻译:

通过疫苗接种延长群体对霍乱的免疫力:考虑到人口流动性和疫苗效应减弱
背景
口服霍乱疫苗接种是预防高危地区疫情爆发和控制流行地区霍乱的一种方法。然而,由于人类流动性和疫苗功效不完善或减弱之间的相互作用,疫苗产生的群体免疫可能是短暂的。随着口服霍乱疫苗的供应和使用的增长,与群体免疫相关的关键问题正在出现,包括:谁应该成为目标;何时应重新接种疫苗;为什么最近接种疫苗的人群会爆发霍乱?
方法和结果
我们使用数学模型来模拟不同迁移程度、传播强度和疫苗覆盖率的人群中的常规和大规模口服霍乱疫苗接种。我们发现,迁移和疫苗效力减弱对群体免疫的持续时间有很大影响,而出生率和死亡率的影响相对较小。与定期大规模疫苗接种或单独常规疫苗接种相比,通过“大规模和维持”混合策略可以更长时间地保护社区。我们表明,与人口流动率非常高或非常低的社区相比,疫苗接种可能最适合具有中等流动性的人群。通过对南苏丹境内流离失所者营地的案例研究,该营地在 2014 年和 2015 年进行了高覆盖率的大规模疫苗接种,我们发现,在霍乱爆发时,疫苗直接效应减弱和人口流动率高,使得该营地 80% 以上的人容易受到影响从 2016 年 10 月开始。
结论
口服霍乱疫苗可以成为在一段时间内快速保护人口的强大工具,这在很大程度上取决于疫苗覆盖率、疫苗随时间的效力以及人员流动导致的人口流动率。由于群体免疫力减弱,接种疫苗的社区有可能发生流行病,但通过补充干预措施或数据驱动的重新接种策略,这种可能性会降低。

























 京公网安备 11010802027423号
京公网安备 11010802027423号